Essentials of Abnormal Psychology Eighth Edition Chapter 12

Essentials of Abnormal Psychology Eighth Edition Chapter 12 Schizophrenia Spectrum and Other Psychotic Disorders © 2019 Cengage. All rights reserved.

Outline • • Perspectives on Schizophrenia Clinical Description, Symptoms, and Subtypes Prevalence and Causes of Schizophrenia Treatment of Schizophrenia © 2019 Cengage. All rights reserved.

Focus Questions • • • How is schizophrenia defined? What are the clinical features of schizophrenia and related disorders? What are positive, negative, and disorganized symptoms? What factors contribute to the development of schizophrenia? What treatments exist for schizophrenia? © 2019 Cengage. All rights reserved.

Key Terms • Psychosis: Gross departure from reality, which may include: – Hallucinations: Sensory experiences in the absence of sensory input (e. g. , hearing voices) – Delusions: Strong, inaccurate beliefs that persist in the face of evidence to the contrary • Schizophrenia: A pervasive type of psychosis characterized by disturbed thought, emotion, behavior © 2019 Cengage. All rights reserved.

Nature of Schizophrenia and Psychosis: History and Current Thinking, Part 1 • Historical background – Emil Kraepelin – used the term dementia praecox to describe schizophrenic syndrome § Early subtypes of schizophrenia – Catatonia, hebephrenia, and paranoia – Eugen Bleuler – introduced the term schizophrenia § “Splitting of the mind” © 2019 Cengage. All rights reserved.

Nature of Schizophrenia and Psychosis: History and Current Thinking, Part 2 • Impact of early ideas on current thinking – Many of Kraeplin and Bleuler’s ideas are still with us – Understanding onset and course considered important • Psychotic behavior – May refer only to hallucinations or delusions or to the unusual behavior (e. g. , inappropriate emotionality, strange actions) accompanying them © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Schizophrenia (1 of 3) A. Two (or more) of the following, each present for a significant portion of time during a one-month period: – (1) delusions – (2) hallucinations – (3) disorganized speech (e. g. , frequent derailment or incoherence) – (4) grossly disorganized or catatonic behavior – (5) negative symptoms (i. e. , diminished emotional expression or avolition) © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Schizophrenia (2 of 3) B. For a significant portion of the time since the onset of the disturbance, level of functioning in one or more major areas, such as work, interpersonal relations, or self-care, is markedly below the level achieved prior to the onset. C. Continuous signs of the disturbance persist for at least six months. D. Schizoaffective disorder and depressive or bipolar disorder with psychotic features have been ruled out. E. The disturbance is not attributable to the physiological effects of a substance (e. g. , a drug of abuse, a medication) or another medical condition. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Schizophrenia (3 of 3) F. If there is a history of autistic spectrum disorder or a communication disorder of childhood onset, the additional diagnosis of schizophrenia is made only if prominent delusions or hallucinations, in addition to the other required symptoms of schizophrenia, are also present for at least one month (or less if successfully treated). From American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5 th ed. ). Washington, DC. © 2019 Cengage. All rights reserved.

Schizophrenia: The “Positive” Symptom Cluster, Part 1 • The positive symptoms – Active manifestations of abnormal behavior – Distortions or exaggerations of normal behavior • Delusions: The basic feature of madness – Gross misrepresentations of reality – Most common: § § Delusions of grandeur Delusions of persecution © 2019 Cengage. All rights reserved.

Schizophrenia: The “Positive” Symptom Cluster, Part 2 • Hallucinations – Experience of sensory events without environmental input – Can involve all senses (e. g. , tasting something when not eating, having skin sensations when not being touched) – Most common: Auditory – Findings from SPECT studies § Neuroimaging: Part of the brain most active during auditory hallucinations = Broca’s area, involved in speech production (not comprehension) © 2019 Cengage. All rights reserved.
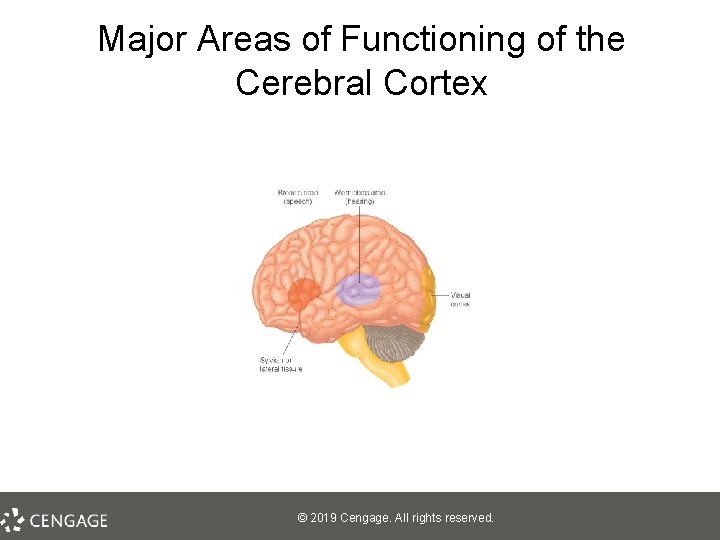
Major Areas of Functioning of the Cerebral Cortex © 2019 Cengage. All rights reserved.

Schizophrenia: The “Negative” Symptom Cluster • The negative symptoms – Absence or insufficiency of normal behavior • Spectrum of negative symptoms – – Avolition (or apathy) – lack of initiation and persistence Alogia – relative absence of speech Anhedonia – lack of pleasure, or indifference Affective flattening – little expressed emotion © 2019 Cengage. All rights reserved.

Schizophrenia: The “Disorganized” Symptom Cluster, Part 1 • The disorganized symptoms – Confused or abnormal speech, behavior, and emotion • Nature of disorganized speech – Cognitive slippage – illogical and incoherent speech – Tangentiality – “going off on a tangent” – Loose associations – conversation in unrelated directions © 2019 Cengage. All rights reserved.

Schizophrenia: The “Disorganized” Symptom Cluster, Part 2 • Nature of disorganized affect – Inappropriate emotional behavior • Nature of disorganized behavior – Includes a variety of unusual behaviors – Catatonia § May be considered a psychotic spectrum disorder in its own right or, when occurring in the presence of schizophrenia, a symptom of schizophrenia © 2019 Cengage. All rights reserved.

Subtypes of Schizophrenia: A Thing of the Past • • • Schizophrenia was previously divided in to subtypes based on content of psychosis This is no longer the case in DSM-5, but outdated terms are still in partial use Included paranoid, catatonic, residual (minor symptoms persist after past episode), disorganized (many disorganized symptoms) and undifferentiated © 2019 Cengage. All rights reserved.

Other Schizophrenia Spectrum Disorders • Schizophreniform disorder – Psychotic symptoms lasting between one and six months (less than six months = schizophrenia) • Brief psychotic disorder – Psychotic symptoms lasting less than one month • Both disorders associated with relatively good functioning – Most patients resume normal lives © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Schizophreniform Disorder (1 of 3) A. Two (or more) of the following, each present for a significant portion of time during a one-month period: – (1) delusions, (2) hallucinations, (3) disorganized speech (e. g. , frequent derailment or incoherence), (4) grossly disorganized or catatonic behavior, (5) negative symptoms. B. An episode of the disorder lasts at least one month but less than six months. C. Schizoaffective disorder and depressive or bipolar disorder with psychotic features have been ruled out. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Schizophreniform Disorder (2 of 3) D. The disturbance is not attributable to the physiological effects of a substance (e. g. , a drug of abuse) or another medical condition. – Specify if: § With good prognostic features: This specifier requires the presence of at least two of the following features: onset of prominent psychotic symptoms within four weeks of the first noticeable change in usual behavior or functioning; confusion or perplexity; good premorbid social and occupational functioning; and absence of blunted or flat affect. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Schizophreniform Disorder (3 of 3) § Without good prognostic features: This specifier is applied if two or more of the above features have not been present. From American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5 th ed. ). Washington, DC. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Brief Psychotic Disorder (1 of 2) A. Presence of one (or more) of the following symptoms. At least one of these must be (1), (2), or (3): 1. delusions 2. hallucinations 3. disorganized speech (e. g. , frequent derailment or incoherence) 4. grossly disorganized or catatonic behavior. Note: Do not include a symptom if it is a culturally sanctioned response. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Brief Psychotic Disorder (2 of 2) B. Duration of an episode of the disturbance is at least one day but less than one month, with eventual full return to premorbid level of functioning. C. The disturbance is not better explained by major depressive of bipolar disorder with psychotic features or another psychotic disorder such as schizophrenia or catatonia, and is not attributable to the physiological effects of a substance (e. g. , a drug of abuse, a medication) or another medical condition. From American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5 th ed. ). Washington, DC. © 2019 Cengage. All rights reserved.

Other Schizophrenia Spectrum Disorders: Schizoaffective Disorder • Schizoaffective disorder – Symptoms of schizophrenia + additional experience of a major mood episode (depressive or manic) – Psychotic symptoms must also occur outside the mood disturbance – Prognosis is similar for people with schizophrenia – Such persons do not tend to get better on their own © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Schizoaffective Disorder (1 of 2) A. An uninterrupted period of illness during which there is a major mood episode (major depressive or manic) concurrent with Criterion A of schizophrenia. Note: The major depressive episode must include Criterion A 1: Depressed mood. B. Delusions or hallucinations for two or more weeks in the absence of a major mood episode (depressive or manic) during the lifetime duration of the illness. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Schizoaffective Disorder (2 of 2) B. Symptoms that meet criteria for a major mood episode are present for the majority of the total duration of the active and residual portions of the illness. C. The disturbance is not attributable to the effects of a substance (e. g. , a drug of abuse, a medication) or another medical condition. From American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5 th ed. ). Washington, DC. © 2019 Cengage. All rights reserved.

Delusional Disorder • Key feature: Delusions that are contrary to reality – Lack other positive and negative symptoms – Types of delusions include: § § § Erotomanic Grandiose Jealous Persecutory Somatic – Extremely rare – Better prognosis than schizophrenia © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Delusional Disorder (1 of 4) A. The presence of one (or more) delusions with a duration of one month or longer. B. Criterion A for schizophrenia has never been met. C. Apart from the impact of the delusion(s) or its ramifications, functioning is not markedly impaired, and behavior is not obviously bizarre or odd. D. If manic or major depressive episodes have occurred, these have been brief relative to the duration of the delusional periods. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Delusional Disorder (2 of 4) E. The disturbance is not attributable to the physiological effects of a substance or another medical condition and is not better explained by another mental disorder. Specify whether: • Erotomanic type: delusion that another person is in love with the individual. • Grandiose type: delusion of having some great (but unrecognized) talent or insight or having made some important discovery. • Jealous type: delusion that the individual’s spouse or lover is unfaithful. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Delusional Disorder (3 of 4) • • • Persecutory type: delusions that the individual is being conspired against, cheated, spied on, followed, poisoned or drugged, maliciously maligned, harassed, or obstructed in the pursuit of long-term goals. Somatic type: delusions that involve bodily functions or sensations. Mixed type: no delusional theme predominates. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Delusional Disorder (4 of 4) • Unspecified type: delusional belief cannot be clearly determined or is not described in the specific types (e. g. , referential delusions without a prominent persecutory or grandiose component). From American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5 th ed. ). Washington, DC. © 2019 Cengage. All rights reserved.

Catatonia • • Unusual motor responses, particularly immobility or agitation, and odd mannerisms Tends to be severe and quite rare May be present in psychotic disorders or diagnosed alone May include: – – Stupor, mutism, or maintaining the same pose for hours Opposition or lack of response to instructions Repetitive, meaningless motor behaviors Mimicking others’ speech or movement © 2019 Cengage. All rights reserved.

Psychotic Disorders due to Other Causes • • Psychosis may occur as the result of substance use, some medications and some medical conditions Knowing these causes is important for treatment – Address underlying cause • Include: – Substance/medication-induced psychotic disorder – Psychotic disorder associated with another medical condition © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Substance/Medication. Induced Psychotic Disorder (1 of 3) A. Presence of either/both of delusions or hallucinations. B. There is evidence from the history, physical examination, or laboratory findings of both (1) and (2): – 1. The symptoms in Criterion A developed during, or soon after substance intoxication or withdrawal or after exposure to a medication. – 2. The involved substance/medication is capable of producing the symptoms in Criterion A. C. The disturbance is not better explained by a psychotic disorder that is not substance/medication-induced. Such evidence of an independent psychotic disorder could include: © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Substance/Medication. Induced Psychotic Disorder (2 of 3) – The symptoms preceded the onset of the substance/medication use; the symptoms persist for a substantial period of time after the cessation of acute withdrawal or severe intoxication; there is other evidence of an independent non-substance/medication induced psychotic disorder. D. The disturbance does not occur exclusively during the course of a delirium. E. The disturbance causes clinically significant distress or impairment in social, occupational, or other important areas of functioning. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Substance/Medication. Induced Psychotic Disorder (3 of 3) From American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5 th ed. ). Washington, DC. © 2019 Cengage. All rights reserved.

DSM-5 Criteria: Psychotic Disorder Associated with Another Condition A. Prominent hallucinations or delusions. B. There is evidence from the history, physical examination, or laboratory findings that the disturbance is the direct pathophysiological consequence of another medical condition. C. The disturbance is not better explained by another mental disorder. D. The disturbance does not occur exclusively during the course of a delirium. From American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5 th ed. ). Washington, DC. © 2019 Cengage. All rights reserved.

Schizophrenia: Statistics, Part 1 • Onset and prevalence of schizophrenia worldwide – About 0. 2% to 1. 5% (or about 1% population) – Often develops in early adulthood – Can emerge at any time; childhood cases are extremely rare but not unheard of © 2019 Cengage. All rights reserved.

Schizophrenia: Statistics, Part 2 • Schizophrenia is generally chronic – Most suffer with moderate-to-severe lifetime impairment – Life expectancy is slightly less than average § § § Increased risk for suicide Increased risk for accidents Self care may be poorer © 2019 Cengage. All rights reserved.

Schizophrenia: Statistics, Part 3 • Schizophrenia affects males and females about equally – Females tend to have a better long-term prognosis – Onset slightly earlier for males • Cultural factors – Psychotic behaviors not always pathologized – Yet schizophrenia is found at similar rates in all cultures © 2019 Cengage. All rights reserved.
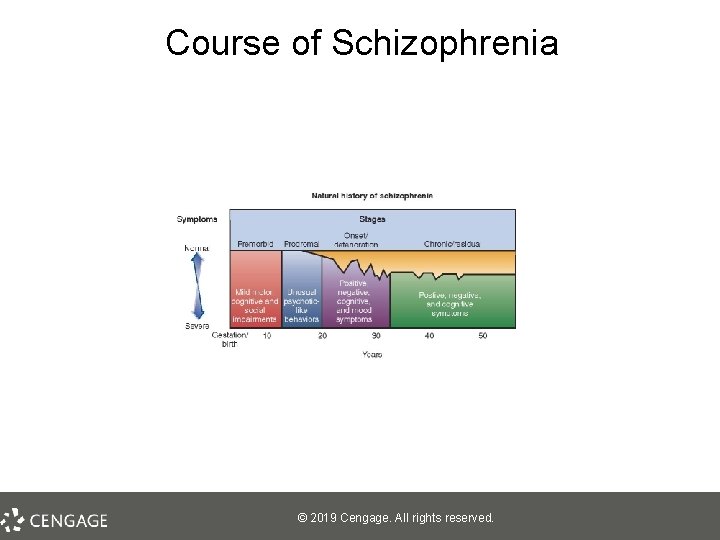
Course of Schizophrenia © 2019 Cengage. All rights reserved.

Causes of Schizophrenia: Findings From Genetic Research, Part 1 • Family studies – Inherit a tendency for schizophrenia, not specific forms of schizophrenia – Risk increases with genetic relatedness § For example, having a twin with schizophrenia incurs greater risk than having an uncle with schizophrenia © 2019 Cengage. All rights reserved.
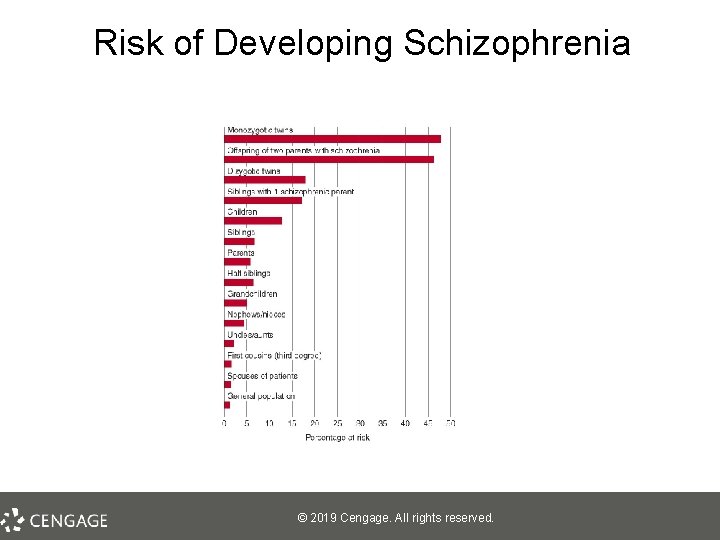
Risk of Developing Schizophrenia © 2019 Cengage. All rights reserved.

Causes of Schizophrenia: Findings From Genetic Research, Part 2 • Twin studies – Monozygotic twins versus fraternal (dizygotic) twins § At greater risk if your identical twin has schizophrenia – supports role of genes – Adoption studies § § Adoptee risk for developing schizophrenia remains high if a biological parent has schizophrenia But risk is lower than for children raised by their biological parent with schizophrenia – healthy environment is a protective factor © 2019 Cengage. All rights reserved.
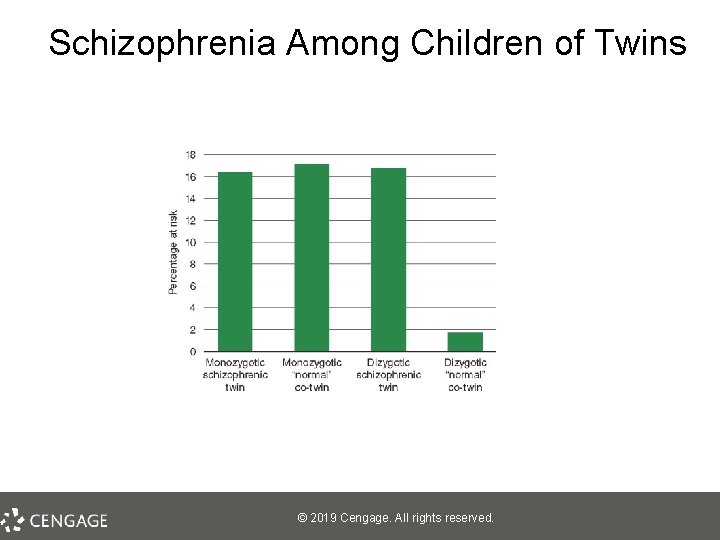
Schizophrenia Among Children of Twins © 2019 Cengage. All rights reserved.

Search for Genetic and Behavioral Markers of Schizophrenia • Genetic markers: Linkage and association studies – Endophentypes – Schizophrenia is likely to involve multiple genes • Behavioral markers: Smooth-pursuit eye movement – Schizophrenia patients show reduced ability to track a moving object with their eyes – Relatives of schizophrenic patients also have deficits in this area © 2019 Cengage. All rights reserved.

Causes of Schizophrenia: Neurobiological Influences • The dopamine hypothesis: Schizophrenia is partially caused by overactive dopamine – Drugs that increase dopamine (agonists) result in schizophrenic-like behavior – Drugs that decrease dopamine (antagonists) reduce schizophrenic-like behavior § • Examples – neuroleptics, L-dopa for Parkinson’s disease Problem: Overly simplistic – Many neurotransmitters are likely involved © 2019 Cengage. All rights reserved.
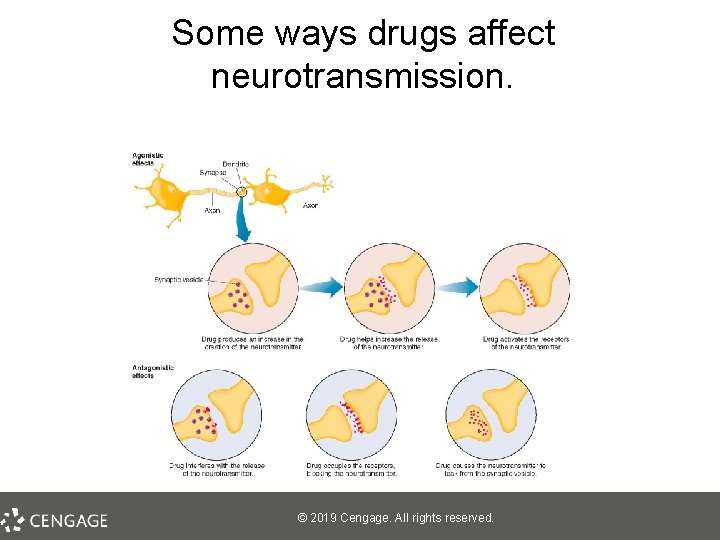
Some ways drugs affect neurotransmission. © 2019 Cengage. All rights reserved.

Causes of Schizophrenia: Other Neurobiological Influences • Structural and functional abnormalities in the brain – Enlarged ventricles and reduced tissue volume – Hypofrontality – less active frontal lobes § • A major dopamine pathway Viral infections during early prenatal development – Findings are inconclusive © 2019 Cengage. All rights reserved.
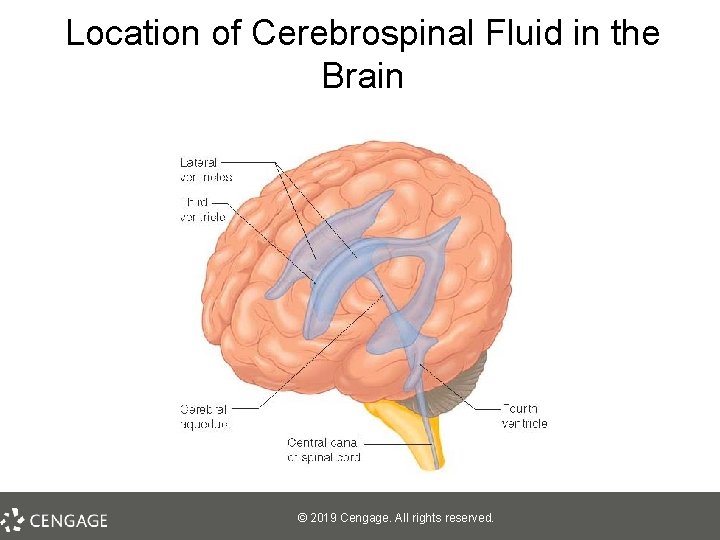
Location of Cerebrospinal Fluid in the Brain © 2019 Cengage. All rights reserved.

Other Neurobiological Influences • • Marijuana use also increases the risk for developing schizophrenia in at-risk individuals Conclusions about neurobiology and schizophrenia – Schizophrenia reflects diffuse neurobiological dysregulation – Structural and functional brain abnormalities § Not unique to schizophrenia © 2019 Cengage. All rights reserved.

Causes of Schizophrenia: Psychological and Social Influences, Part 1 • The role of stress – May activate underlying vulnerability – May also increase risk of relapse • Family interactions – Unsupported theories § § Schizophrenogenic mother Double bind communication – High expressed emotion (EE) – associated with relapse © 2019 Cengage. All rights reserved.
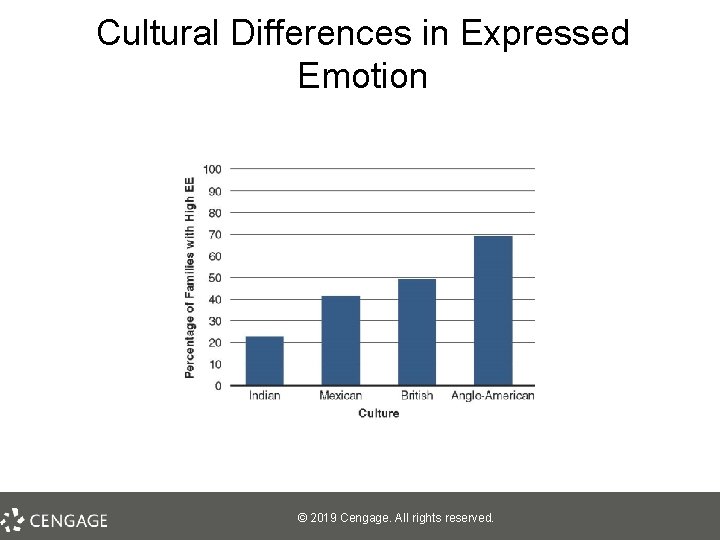
Cultural Differences in Expressed Emotion © 2019 Cengage. All rights reserved.

Causes of Schizophrenia: Psychological and Social Influences, Part 2 • The role of psychological factors – May function as the diathesis in a diathesis-stress model – Exert only a minimal effect in producing schizophrenia © 2019 Cengage. All rights reserved.

Medical Treatment of Schizophrenia • • Historical precursors Development of antipsychotic (neuroleptic) medications – – Often the first line treatment for schizophrenia Began in the 1950 s Most reduce or eliminate positive symptoms Acute and permanent side effects are common § § § Parkinson’s-like side effects Tardive dyskinesia Compliance with medication is often a problem – Noncompliance with medication © 2019 Cengage. All rights reserved.

Psychosocial Treatment of Schizophrenia, Part 1 • • Historical precursors Psychosocial approaches – Behavioral (i. e. , token economies) on inpatient units: Reward adaptive behavior – Community care programs – Social and living skills training – Behavioral family therapy – Vocational rehabilitation © 2019 Cengage. All rights reserved.

Psychosocial Treatment of Schizophrenia, Part 2 • Psychosocial approaches cont. – Illness management and recovery: Engages patient as an active participant in his/her care, focusing on goal setting and dealing with functional impairment – Cultural considerations: Important to take into account cultural factors that influence individuals’ understanding of their own illness – Prevention: Identify at-risk children and intervene (e. g. , with supportive, nurturing environments, social skills training) © 2019 Cengage. All rights reserved.

Summary of Schizophrenia and Psychotic Disorders, Part 1 • Schizophrenia – spectrum of dysfunctions – Affecting cognitive, emotional, and behavioral domains – Positive, negative, and disorganized symptom clusters © 2019 Cengage. All rights reserved.

Summary of Schizophrenia and Psychotic Disorders, Part 2 • • • DSM-5 documents a range of psychotic disorders Several bio-psycho-social variables are involved Successful treatment rarely includes complete recovery © 2019 Cengage. All rights reserved.
- Slides: 58