ERYTHROCYTE C 4 d A MARKER OF ANTIBODY

ERYTHROCYTE C 4 d: A MARKER OF ANTIBODY MEDIATED REJECTION T. Mohanakumar, Ph. D. Department of Surgery, Pathology & Immunology Washington University School of Medicine

ANTIBODY MEDIATED REJECTION (AMR) n n Allograft rejection caused by antibodies Directed against – Donor-specific HLA molecules – Non-HLA tissue specific antigens n n n Myosin, Vimentin, Collagen V (Heart) K-alpha-1 -tublin, Collagen V (Lung) Vimentin, Collagen IV (Kidney) – Blood group ABO isoagglutinins

ANTIBODIES IN ORGAN ALLOGRAFTS Colvin RB et al, Antibody-mediated organ-allograft rejection. Nat Rev Immunol 2005; 5(10): 807 -17
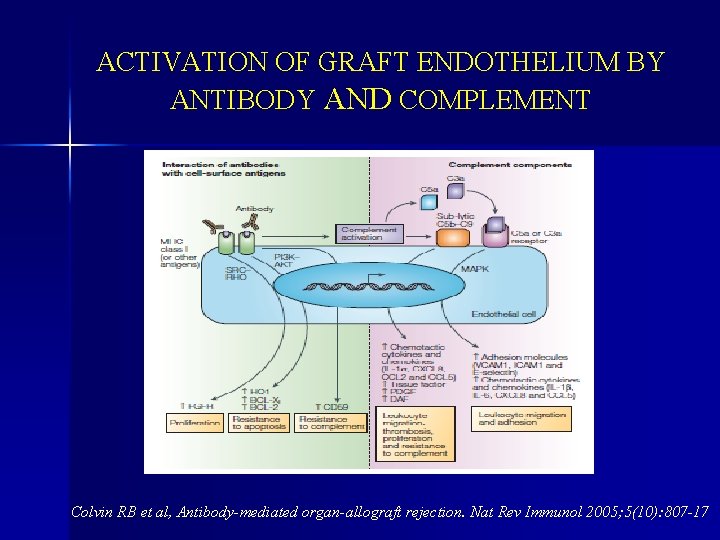
ACTIVATION OF GRAFT ENDOTHELIUM BY ANTIBODY AND COMPLEMENT Colvin RB et al, Antibody-mediated organ-allograft rejection. Nat Rev Immunol 2005; 5(10): 807 -17

INCIDENCE OF AMR n Acute _ Heart-10 -30% – Lung: unknown – Kidney: 20 -30% n Chronic AMR – Heart: 20 -40% – Lung: unknown – Kidney: 30 -40%
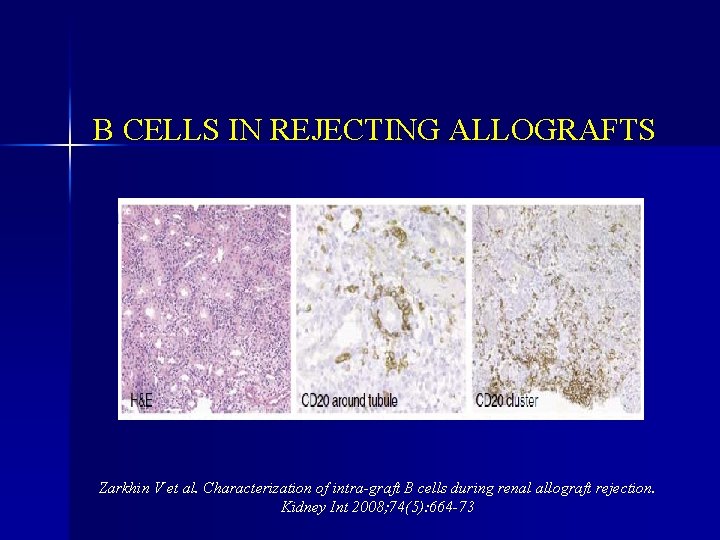
B CELLS IN REJECTING ALLOGRAFTS Zarkhin V et al. Characterization of intra-graft B cells during renal allograft rejection. Kidney Int 2008; 74(5): 664 -73

DIAGNOSTIC CRITERIA FOR AMR n n Clinical Evidence of Acute Graft Dysfunction Histological Evidence of Acute Capillary Injury – – – n Capillary endothelial swelling or denudation with congestion Macrophages or neutrophils in capillaries Interstitial edema and/or hemorrhage Immunopathologic Evidence for Antibody Mediated Injury – Ig + C 3 d and/or C 4 d or C 1 q by immunofluorescence – CD 68 positivity for capillary macrophages/C 4 d capillary staining – Fibrin in vessels n Serological Evidence for DSA or Anti-HLA antibodies Takemoto SK et al. National conference to assess antibody mediated rejection in solid organ transplantation. Am J Transplant 2004; 4: 1022 -41

MONITORING FOR AMR n Clinical Parameters – Heart: Diminished ventricular ejection fraction – Lung: Diminished FEV 1 – Kidney: Diminished GFR n Histology – Ab and/or Complement deposition (C 3 d, C 4 d) n Serum Markers – Donor specific antibody (DSA) to HLA – Antibodies to self antigens

ERYTHROCYTE BOUND C 4 d (E-C 4 d) n n Increased cell bound complement activation product, C 4 d, detected on the surface of erythrocytes. Have been shown to correlate with – Disease activity in systemic lupus erythematous (SLE) – Acute rejection after cardiac transplantation n n E-C 4 d have increased half-life compared to serum C 3 and C 4 d More reliable tool compared to serum/biopsy C 3 d or C 4 d.

METHODS OF E-C 4 d DETECTION n n Erythrocytes from 5 cc fresh EDTA blood were analyzed by indirect immunofluorescence using flow cytometry Calculation of E-C 4 d : – Surface expression E-C 4 d = MFI C 4 d/CR 1 – MFI Isotype Control SLE study: Manzi S et al, Arthritis Rheum 2004; 50: 3596 -604 – E-C 4 d/E-CR 1 ratio = (MFI E-C 4 d – MFI Isotype Control) / (MFI ECR 1 – MFI Isotype Control) Cardiac transplant study, Lee KC et al. Transplant Proc 2008; 40: 2638 -2642 – % E-C 4 d = % of total RBCs with > 2 S. D. positive mean fluorescence shift (MFIanti-C 4 d - MFIisotype control Ig. G ) compared to healthy controls.

E-C 4 d IN LUNG TRANSPLANTATION
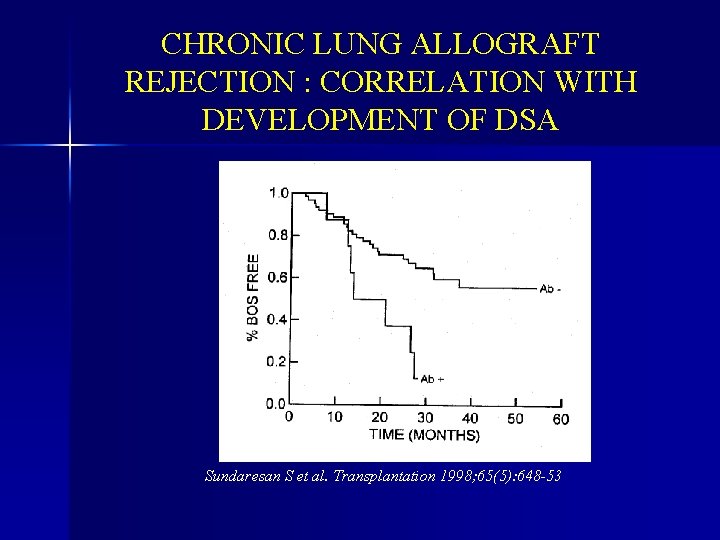
CHRONIC LUNG ALLOGRAFT REJECTION : CORRELATION WITH DEVELOPMENT OF DSA Sundaresan S et al. Transplantation 1998; 65(5): 648 -53

CHRONIC LUNG ALLOGRAFT REJECTION; CORRELATION WITH DEVELOPMENT OF ANTIBODIES TO SELF-ANTIGENS K-alpha-1 -tubulin Collagen V

E-C 4 D IN ASSESSING AMR n n n Breakdown products of complement activation which are bound to erythrocytes Have been shown to correlate with disease status in SLE, used as an adjunct to monitor SLE Erythrocyte bound form is more stable and has an increased half-life

OBJECTIVE n n Determine the E-C 4 d by flow cytometry ( a non-invasive, simple and reliable method for diagnosing AMR) Correlate % E-C 4 d with Development of DSA n Development of Antibodies to self-antigens n C 3 d staining in biopsy specimen n

MATERIALS AND METHODS n 22 post-lung transplant study patients 15 normal healthy adult volunteers n Antibodies to HLA (Luminex) n Antibodies to Self-Antigens (KA 1 T and Col V , ELISA) C 3 d deposition by Immunohistochemistry n n

MATERIALS AND METHODS n E-C 4 d: Immunofluorescence by flow cytometry 10 ul fresh anticoagulated (EDTA) blood – Murine monoclonal anti-human C 4 d or isotype control – Fluorescein isothiocyanate conjugated goat anti-mouse Ig. G n n % E-C 4 d was calculated by determining the percentage of total RBCs with a positive mean fluorescence shift (MFIanti-C 4 d - MFIisotype Ig. G 1) Two standard deviation from mean fluorescence shift obtained in the control population was used as cutoff value to calculate % E-C 4 d
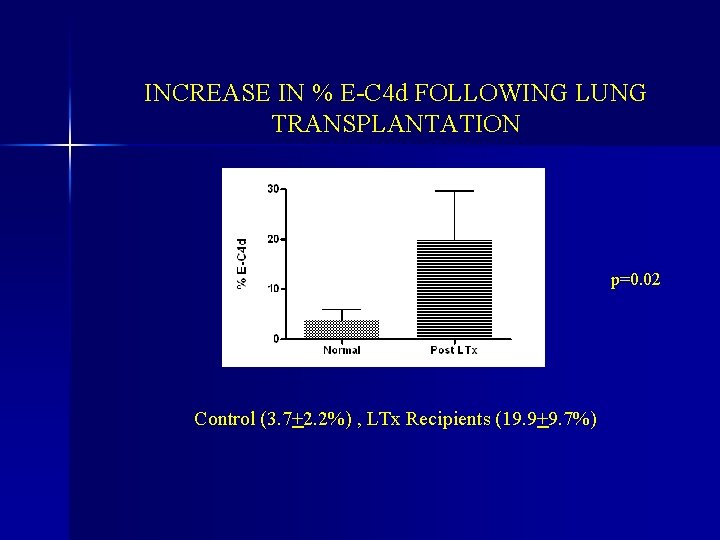
INCREASE IN % E-C 4 d FOLLOWING LUNG TRANSPLANTATION p=0. 02 Control (3. 7+2. 2%) , LTx Recipients (19. 9+9. 7%)
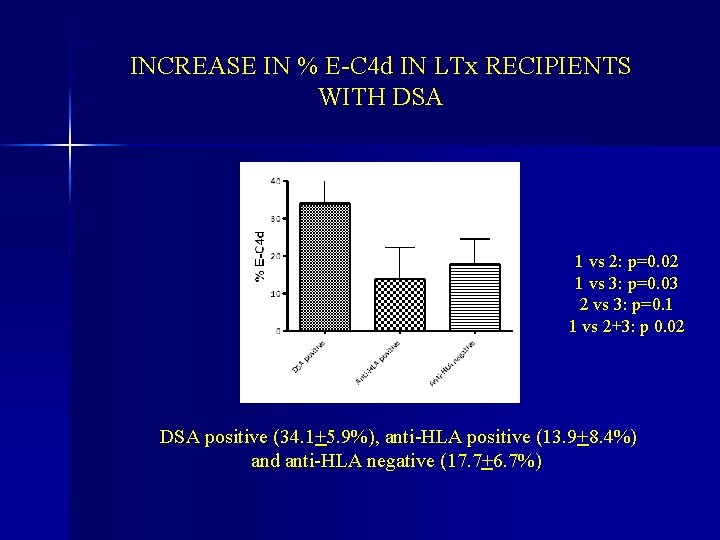
INCREASE IN % E-C 4 d IN LTx RECIPIENTS WITH DSA 1 vs 2: p=0. 02 1 vs 3: p=0. 03 2 vs 3: p=0. 1 1 vs 2+3: p 0. 02 DSA positive (34. 1+5. 9%), anti-HLA positive (13. 9+8. 4%) and anti-HLA negative (17. 7+6. 7%)
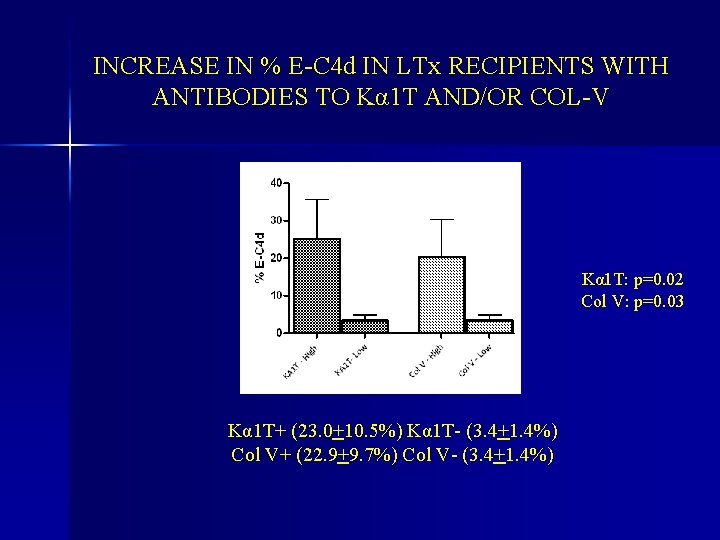
INCREASE IN % E-C 4 d IN LTx RECIPIENTS WITH ANTIBODIES TO Kα 1 T AND/OR COL-V Kα 1 T: p=0. 02 Col V: p=0. 03 Kα 1 T+ (23. 0+10. 5%) Kα 1 T- (3. 4+1. 4%) Col V+ (22. 9+9. 7%) Col V- (3. 4+1. 4%)
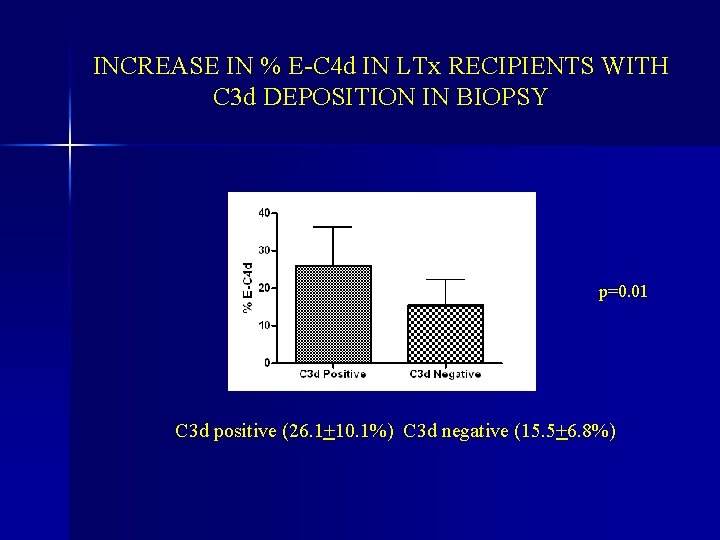
INCREASE IN % E-C 4 d IN LTx RECIPIENTS WITH C 3 d DEPOSITION IN BIOPSY p=0. 01 C 3 d positive (26. 1+10. 1%) C 3 d negative (15. 5+6. 8%)

SUMMARY AND CONCLUSION n Increase in % E-C 4 d are found in patients with – DSA – Antibodies to Kα 1 T and Col V – C 3 d deposition in biopsy n % E-C 4 d may be useful as a simple method for monitoring AMR following human lung transplantation.

LIMITATIONS n Small cohort of patients and therefore can only be viewed as encouraging preliminary results.

Acknowledgements Fellows • • • • • Sudhir Sundaresan, MD Scott I Reznik, MD Michael A Smith, MD Andres Jaramillo, Ph. D Ryan Fields, MD Trudie Goers, MD Toru Higuchi, MD Takahiro Maruyama, MD Kishore Narayanan, Ph. D Naohiko Fukami, MD, Ph. D Deepti Saini, Ph. D Ilias H. Basha, M. D Sabarinathan Ramachandran, Ph. D Ankit Bharat, MD Anguswamy Nataraju, Ph. D Swarup Trivedi, M. D, Ph. D Masashi Takenaka, M. D Lung Transplant Physicians • G Alexander Patterson, MD • Elbert P Trulock, MD • Michael J Walter , MD • Ramsey R Hachem, MD Renal Transplant physicians • Martin Jendrisak, M. D • Surendra Shenoy, M. D Lung Transplant co-ordinator • Aviva Aloush HLA Laboratory
- Slides: 24