Eric S Rosenberg M D Associate Professor of

Eric S. Rosenberg, M. D. Associate Professor of Medicine Massachusetts General Hospital Harvard Medical School erosenberg 1@partners. org

47 year old male • Present to MGH ED with an 8 day history of : Fever to 102. 5 Headache Photophobia Myalgias and arthralgias Nausea and vomiting 3 rd visit to health care system

47 year old male Additional history: MSM Recent unprotected sex with an HIV infected partner PMH: prior hx of syphilis Exam: Fever Cervical lymphadenopathy Rash (started on torso spread to limbs and scalp)
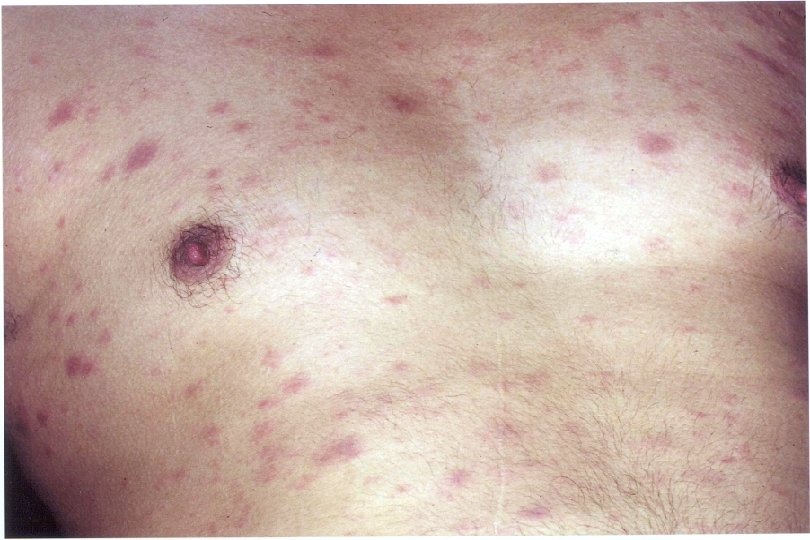

47 year old male Diagnostics: Test for EBV, CMV, influenza were negative HIV ELISA Positive Western Blot negative (no bands) HIV RNA > 750, 000 copies/ml 1: 100 dilution 47, 000 copies/ml CD 4 count = 432 cells

Diagnosis Acute HIV infection

Framing the Question MGH-NCSU collaboration Should this individual be treated with antiretroviral therapy? ?

Acute HIV infection Goals 1. To discuss the advantages and disadvantages of treating individuals with acute HIV 2. To review the early biological events of acute HIV infection 3. To review the immunologic rationale for treatment during acute infection and possible treatment interruption

Should individuals with Acute HIV-1 infection be treated with antiretroviral therapy? Advantages Preservation of HIV-specific cellular immune responses Opportunity for structured treatment interruption ? ? Lowering of HIV-1 set point Limitation of viral evolution and diversity Decreased transmission Mitigation of acute retroviral symptoms ? Disadvantages Toxicities and unknown longterm risks ? ? Short- and long-term clinical benefits are not well-defined Resistance acquisition Limitation of future antiretroviral therapy options Quality of life impact Cost Kassutto et al, CID 2006
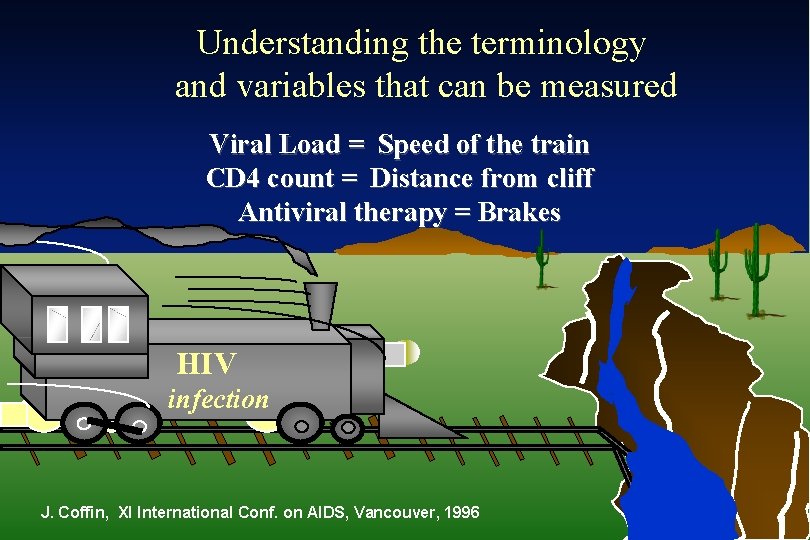
Understanding the terminology and variables that can be measured Viral Load = Speed of the train CD 4 count = Distance from cliff Antiviral therapy = Brakes HIV infection J. Coffin, XI International Conf. on AIDS, Vancouver, 1996
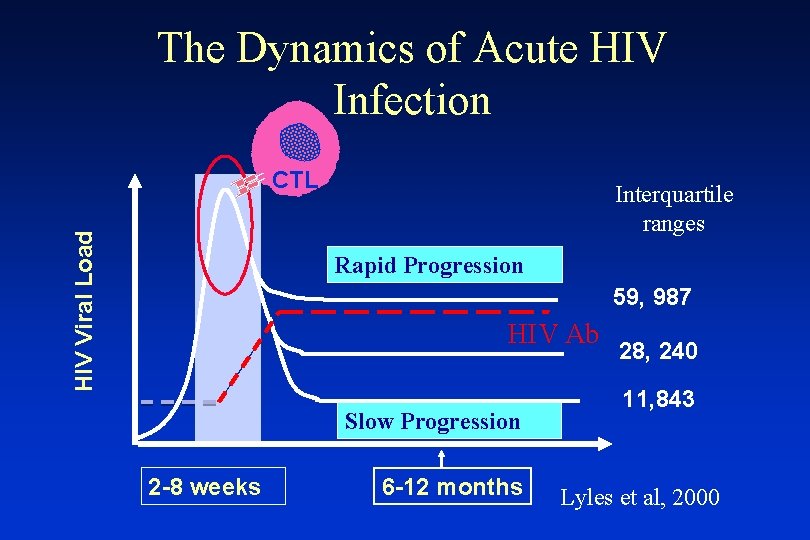
The Dynamics of Acute HIV Infection HIV Viral Load CTL Interquartile ranges Rapid Progression 59, 987 HIV Ab Slow Progression 2 -8 weeks 6 -12 months 28, 240 11, 843 Lyles et al, 2000

Since the level of HIV in the blood predicts progression, What factors influence viral replication?
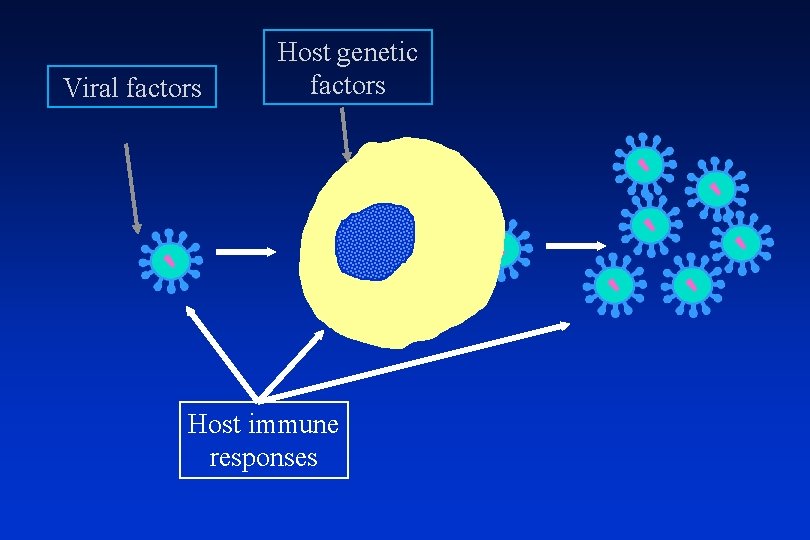
Viral factors Host genetic factors Host immune responses
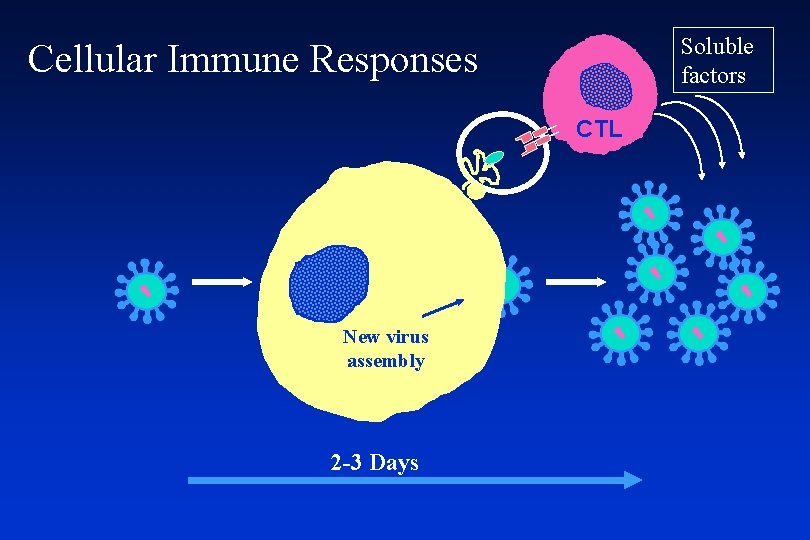
Soluble factors Cellular Immune Responses CTL New virus assembly 2 -3 Days

If CTL are present, why is the immune response not more effective in HIV infection?
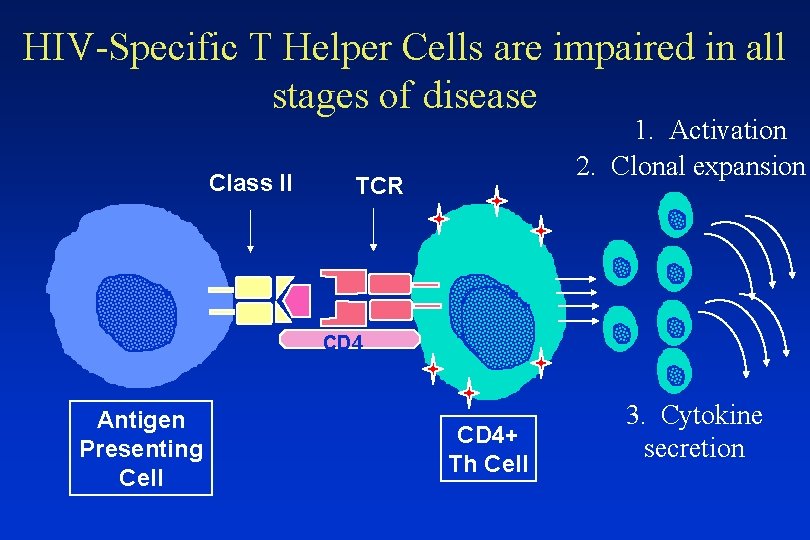
HIV-Specific T Helper Cells are impaired in all stages of disease Class II 1. Activation 2. Clonal expansion TCR CD 4 Antigen Presenting Cell CD 4+ Th Cell 3. Cytokine secretion
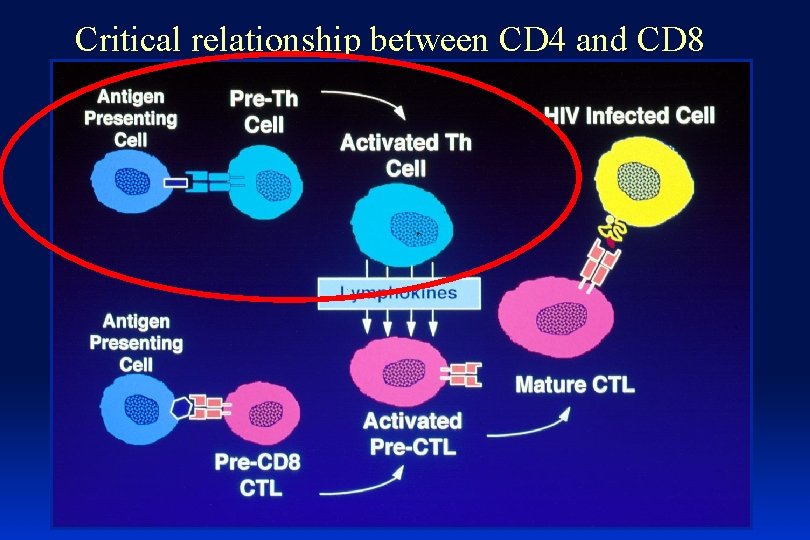
Critical relationship between CD 4 and CD 8

What happens to HIV-specific T helper cells? The acute infection hypothesis Hypothesis (pathogenesis): • HIV-specific T helper cell (CD 4) responses are impaired during acute infection Hypothesis (opportunity): • Treatment with ARV during acute infection will protect these responses from being lost
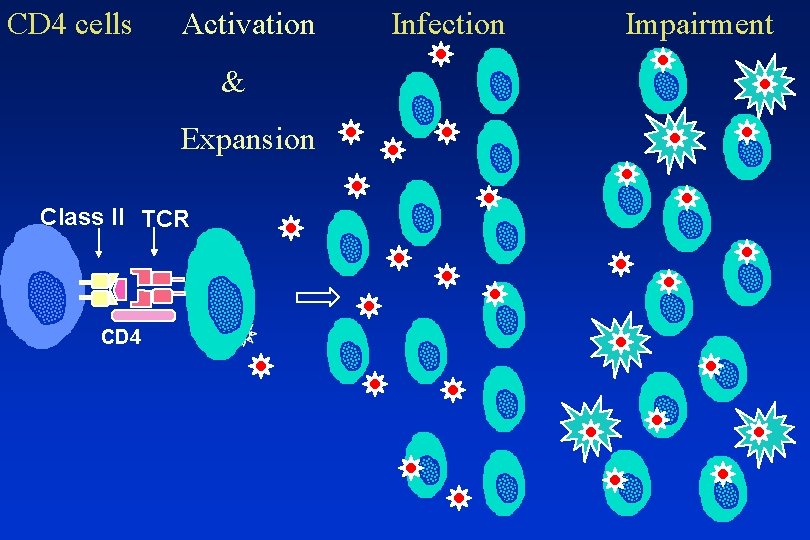
CD 4 cells Activation & Expansion Class II TCR CD 4 Infection Impairment
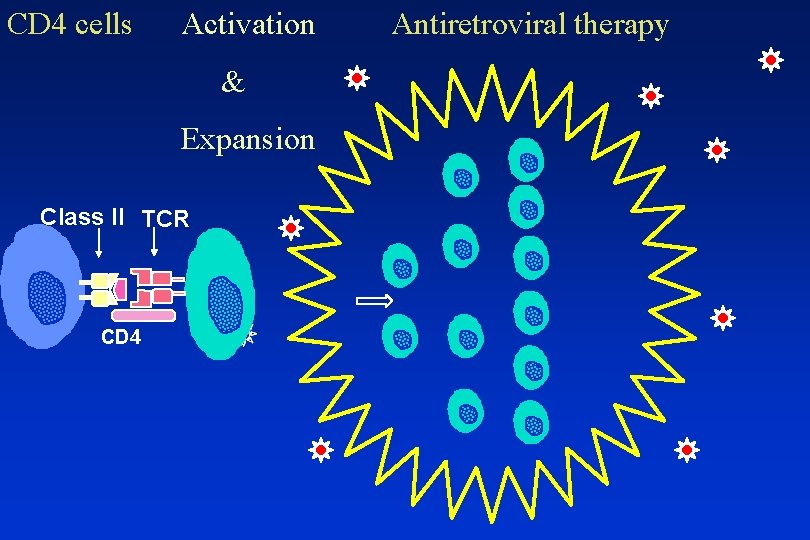
CD 4 cells Activation & Expansion Class II TCR CD 4 Antiretroviral therapy
![Acute Early total n 35 [31, 39] 37 [34, 43] 102 Male gender (%) Acute Early total n 35 [31, 39] 37 [34, 43] 102 Male gender (%)](http://slidetodoc.com/presentation_image_h/dc32a75f9d57b8a09bb057db66ede498/image-21.jpg)
Acute Early total n 35 [31, 39] 37 [34, 43] 102 Male gender (%) HIV Risk Factor MSM (%) 94 94 102 82 81 94 White race (%) 77 78 102 382, 000 (2800 -2. 95 million) 75 567 (170 -981) 100 Characteristic Median age (years) [IQR] Mean baseline VL (copies/m. L) (range) Mean baseline CD 4 (cells/mm 3) (range) 5. 61 million (11, 000 -95 million) 445 (42 -1093) Kassutto et al, CID 2006
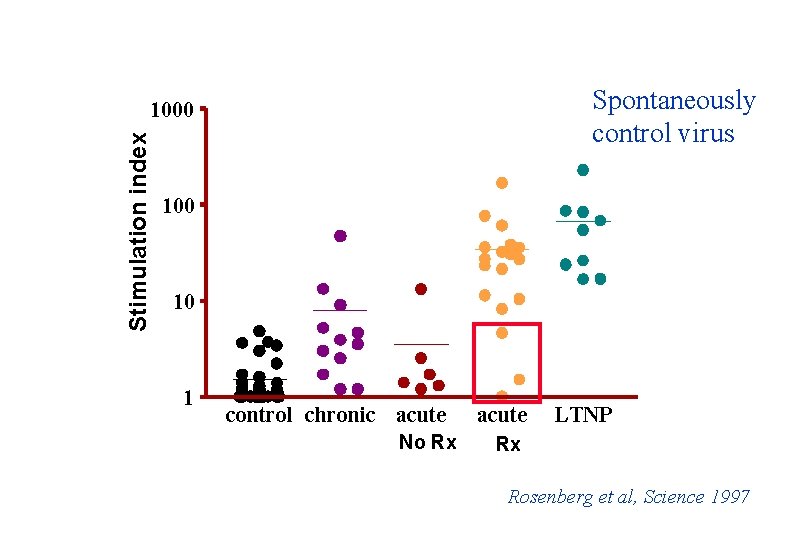
Spontaneously control virus Stimulation index 1000 10 1 control chronic acute No Rx acute LTNP Rx Rosenberg et al, Science 1997

Observation • Immune damage occurs in the earliest stages of acute HIV infection, but there appears to be a “window of opportunity” to reverse this damage with treatment

Can treatment be initiated during acute HIV infection and then discontinued?
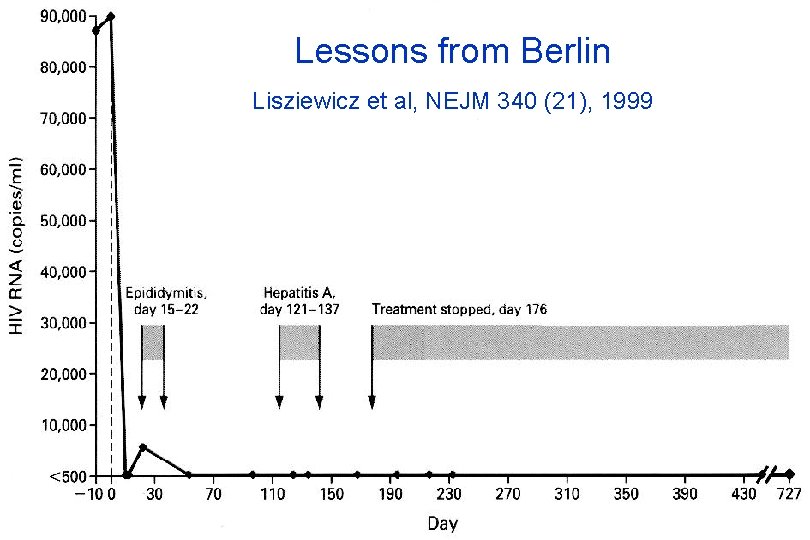
Lessons from Berlin Lisziewicz et al, NEJM 340 (21), 1999
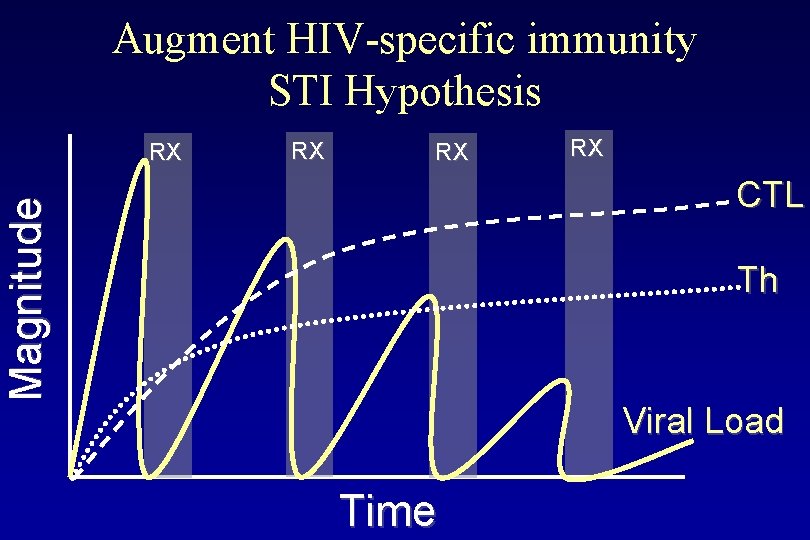
Augment HIV-specific immunity STI Hypothesis RX RX RX CTL Magnitude RX Th Viral Load Time

Can therapy be discontinued? • Will HIV-1 -specific immune responses generated and maintained during acute infection be enough to control viremia? • If virus returns once therapy is discontinued, can this “snap-shot” of autologous virus further boost the immune system?

Structured treatment interruption • Several patterns have emerged • Failure • Transient control of viremia with sudden loss of containment • Control (durability? ) Rosenberg et al, Nature 2000 Kaufmann et al, PLo. S Med 2004

Is the “possibility” of STI enough reason to treat individuals during acute HIV infection? Enough question exists regarding the use of STI as a management strategy that the most relevant question in 2008 is whether or not to treat during acute infection

Conclusions • It is not known whether treatment during acute infection is the correct thing to do • STI may have a role in management of individuals treated during acute infection but optimal approach not known. • Robust mathematical and statistical modeling (NCSU-MGH) to inform the design of the first randomized trial of treatment versus no treatment during acute HIV.
- Slides: 30