ER Drugs and their cardiovascular effects PRE PARED






















































- Slides: 67

ER Drugs and their cardiovascular effects PRE PARED BY SH AN E BARCLAY M D

Objectives Review some of the common drugs used in the ER and review their cardiovascular effects.

Why these drugs and why the CV effects? Think of these drugs as your ‘menu’ that you are going to be able to ‘offer’ patients for various conditions. Of all their potential side effects it is the cardiovascular ones that are most important for working in the ER. Obviously this is not an exhaustive list of ER drugs, but the ones with CV effects.

The List of drugs Phenylephrine Epinephrine Norepinephrine Isoproterenol Dobutamine Dopamine Digoxin Atropine Calcium Channel Blockers Amiodarone Beta Blockers Nitroglycerin Ketamine Fentanyl Morphine Propofol Midazolam Morphine Nitroglycerin Norepinephrine Phenyleprhine Propofol Midazolam

Remember pharmacology from med school ! • Alpha 1 – Agonists cause peripheral vasoconstriction. Antagonists cause vasodilation. • Alpha 2 – CNS mediated, agonists cause hypotension, sedation… • Beta 1 – Heart effects: agonists positive, antagonists negative – inotropic (strength of contraction), chronotropic (heart rate), dromotropic (‘conduction’) • Beta 2 – Lung effects: Agonists cause bronchodilation. Antagonists cause bronchoconstriction.

Remember pharmacology from med school ! ER drug ‘pharmacology’ is mainly about alpha and beta activity. Half lives, volume of distribution etc are also important but will not be covered here.

Drug a 1 Phenylephrine +++ b 1 b 1 Inotr Chron Dromo b 2 V/C V/D

Phenylnephrine • Uses: cardiogenic shock, decompensated atrial fib, diastolic heart failure. . • Can be used as a bolus or infusion, although usually it is used in small boluses.

Drug a 1 b 1 b 1 Inotr Chron Dromo b 2 Phenylephrine +++ Epinephrine +++ ++ V/C V/D

Epinephrine Unlike phenylephrine Epi has both alpha and beta activity. Uses: - ACLS – V. Fib/V-Tach, asystole (1: 10, 000 solution IV) Anaphylaxis – (1: 1, 000 solution S. C. ) Peri intubation, septic shock while getting norepi, etc As a pressor can be given as an IV bolus or infusion.

Drug a 1 b 1 b 1 Inotr Chron Dromo b 2 Phenylephrine +++ Epinephrine +++ ++ Norepinephrine +++ + V/C V/D

Norepinephrine Has more alpha adrenergic properties than epinephrine, but less positive inotropic effect. Is used in a variety of conditions where you need both ‘pressor’ and ‘inotropic’ support. ie – sepsis, cardiovascular collapse, CHF, etc Can be given through a peripheral line, but better if via a central line.

Norepinephrine Dosage “Up to Date” Dosages Hypotension/Shock Start 0. 1 mcg/kg/min – (range 0. 1 -1. 5 mcg/kg/min) Sepsis Start 0. 01 mcg/kg/min (range 0. 01 – 3 mcg/kg/min)

Norepinephrine Dosage “One starting dose” 0. 1 mcg/kg/min then titrate.

Drug a 1 b 1 b 1 Inotr Chron Dromo b 2 Phenylephrine +++ Epinephrine +++ ++ Norepinephrine +++ + Isoproterenol ++ ++ + V/C V/D

Isoproterenol Non selective beta 1 , beta 2 agonist Structurally related to epinephrine. Uses: Bradycardia Torsades - to shorten the QT interval by increasing rate Dose: 0. 4 mg IV then 2 – 20 mcg/min

Drug a 1 b 1 b 1 Inotr Chron Dromo b 2 Phenylephrine +++ Epinephrine +++ ++ Norepinephrine +++ + Isoproterenol ++ ++ Dobutamine ++ + V/C V/D

Dobutamine The “cardiac squeeze” drug Main use is in Cardiogenic Shock Start 2 mcg/kg/min

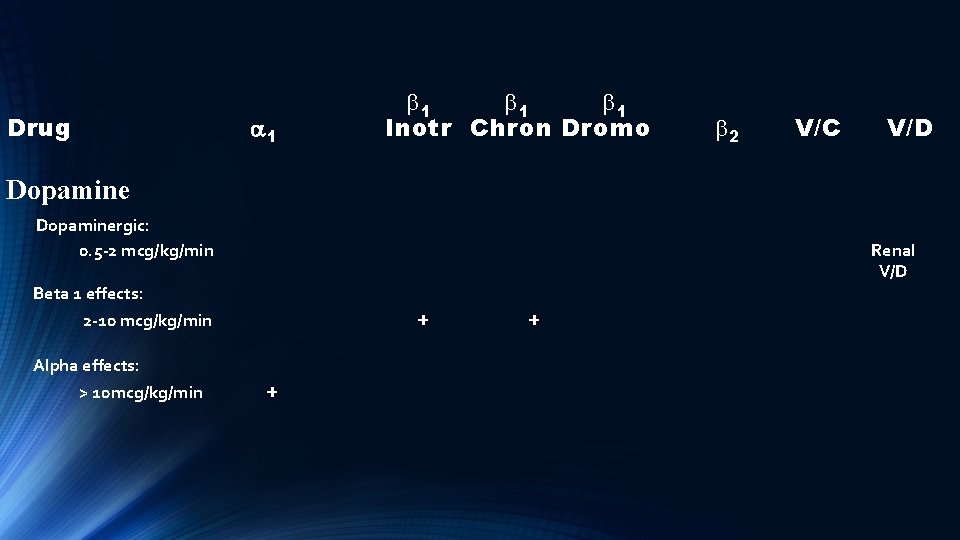
Drug a 1 b 1 b 1 Inotr Chron Dromo b 2 V/C V/D Dopaminergic: 0. 5 -2 mcg/kg/min Renal V/D Beta 1 effects: + 2 -10 mcg/kg/min Alpha effects: > 10 mcg/kg/min + +

Dopamine Although a very commonly used drug in the past, the issue of ‘dose’ effect has relegated dopamine to a ‘rarely’ used pressor now.

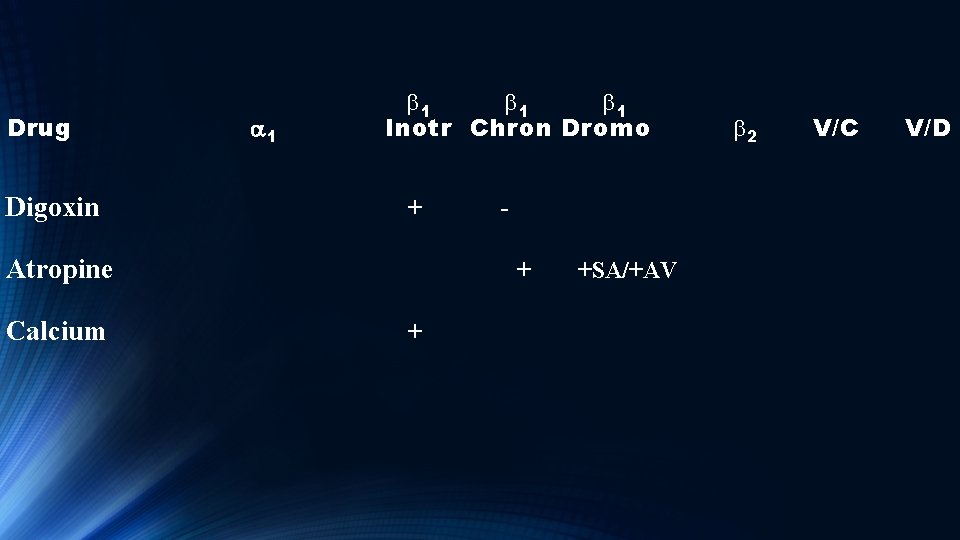
Drug a 1 b 1 b 1 Inotr Chron Dromo Digoxin + - b 2 V/C V/D

Digoxin Like Dopamine, digoxin has been used less and less in recent years. However given its primarily inotropic effect is can be of benefit for some patients in chronic congestive heart failure.

Drug a 1 b 1 b 1 Inotr Chron Dromo Digoxin + Atropine + +SA/+AV b 2 V/C V/D

Atropine Anticholinergic antimuscarinic In addition to increasing heart rate can cause dry mouth, urinary retention, blurred vision, mydriasis, reduce bowel spasm, agitation, confusion, drowsiness and amnesia. Use prior to intubation? Especially if using Ketamine for induction agent to decrease salivation.

Drug a 1 b 1 b 1 Inotr Chron Dromo Digoxin + Atropine + +SA/+AV Calcium + b 2 V/C V/D

Calcium - indications 1. Hypocalcemia 2. Calcium channel blocker overdose 3. Shock – positive inotrope 4. Hyperkalemia 5. Hypermagnesemia

Calcium – 2 Forms Calcium Chloride Quickly cleaved in the plasma to free Calcium and Chloride Usual dose is 1 -2 gm (but can be as much as 4 -5 gm) Is usually recommended to be given via a central line or a very good antecubital vein. Injection into tissue/interstitial can cause necrosis and sloughing.

Calcium – 2 Forms Calcium Gluconate Metabolized in the liver to free calcium Usual dose is 3 times that of Ca. Cl (ie 3 -6 gm) Can be given through a peripheral IV line.

Calcium – Administration Calcium Chrolide Comes in 1 gm/10 ml vial Give maximum 1 ml/minute – i. e. 10 minutes Calcium Gluconate Give 3 gm over 15 -20 minutes.

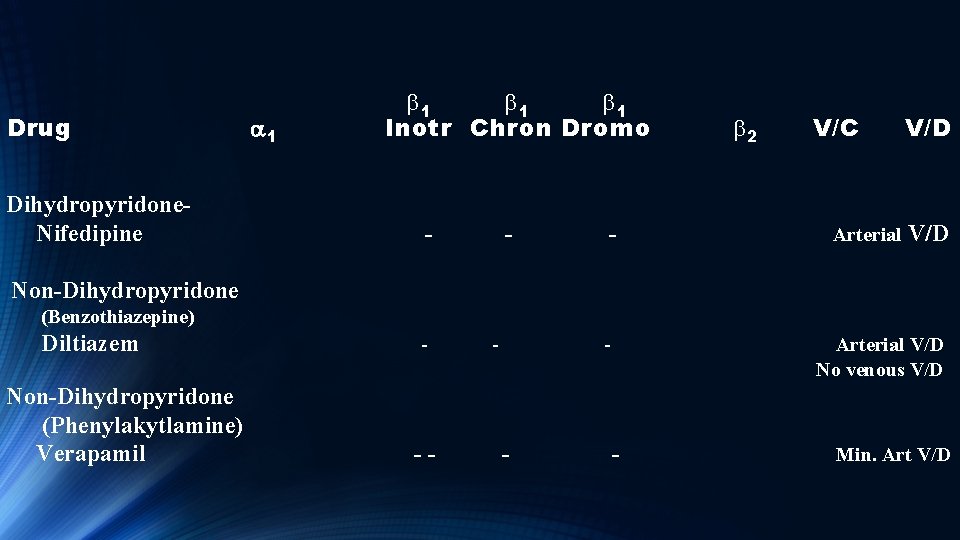
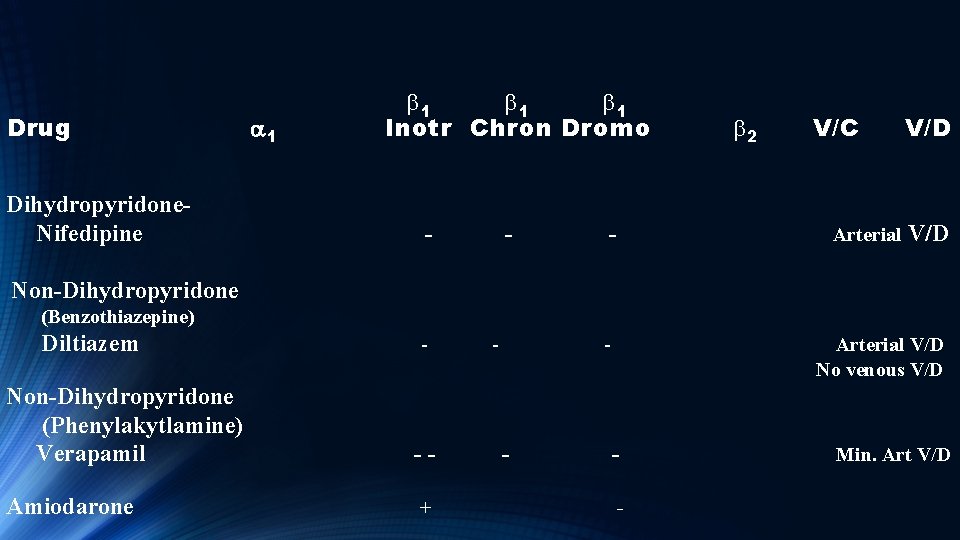
Drug a 1 b 1 b 1 Inotr Chron Dromo b 2 V/C V/D Dihydropyridone Nifedipine - - Arterial V/D Non-Dihydropyridone (Benzothiazepine) Diltiazem - Arterial V/D No venous V/D Non-Dihydropyridone (Phenylakytlamine) Verapamil - - - Min. Art V/D

Calcium Channel Blockers Nifedipine and Diltiazem have negative inotropic and chronotropic effects, and block the AV node to treat arrhythmias. Both cause arterial vasodilation. Verapamil has weak arterial vasodilation properties compared to other CCB, but is a potent AV node blocking agent.

Drug a 1 b 1 b 1 Inotr Chron Dromo b 2 V/C V/D Dihydropyridone Nifedipine - - Arterial V/D Non-Dihydropyridone (Benzothiazepine) Diltiazem - Arterial V/D No venous V/D Non-Dihydropyridone (Phenylakytlamine) Verapamil - - - Min. Art V/D Amiodarone + -

Amiodarone Nifedipine and Diltiazem have negative inotropic and chronotropic effects, and block the AV node to treat arrhythmias. Both cause arterial vasodilation. Verapamil has weak arterial vasodilation properties compared to other CCB, but is a potent AV node blocking agent. Amiodarone has positive inotropic effects along with negative dromotropic effects on both the SA and AV node.

Amiodarone The drug that “never met an arrhythmia it didn’t like” can be used for VT, VF, Wide Comples Tachy, A Fib, SVT Amiodarone has positive inotropic effects along with negative dromotropic effects on both the SA and AV node, which is its main mechanism of action. (it prolongs the action potential, thus refractory period, of all cardiac fibers)

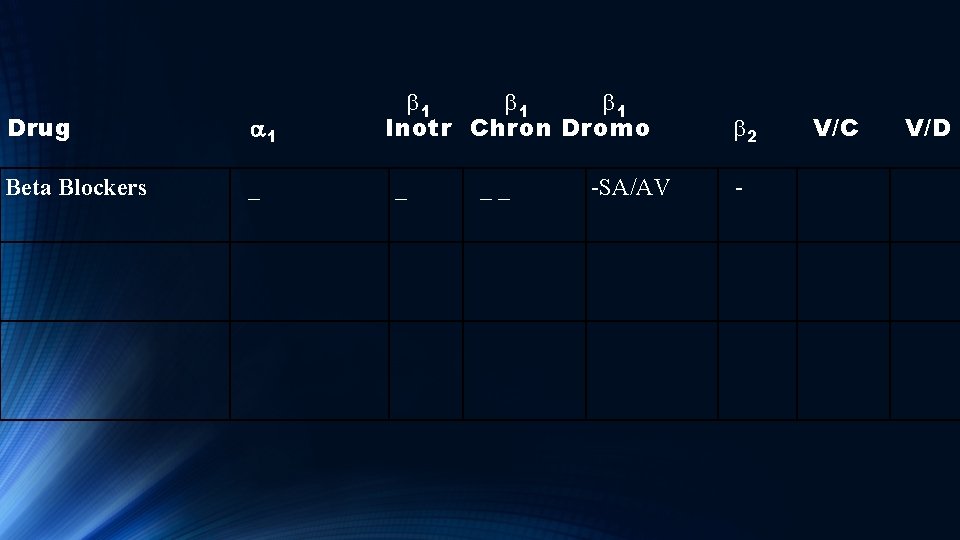
Drug Beta Blockers a 1 _ b 1 b 1 Inotr Chron Dromo _ _ _ -SA/AV V/C b 2 - V/D

Beta Blockers As the name suggests, beta blockers block all Beta adrenergic receptors – beta 1 and beta 2 ‘Selective’ beta blockers don’t block Beta 2 receptors. All Beta blockers affect heart rate (Chromotropic) as well as block the SA and AV node.

Drug a 1 Beta Blocker - b 1 b 1 Inotr Chron Dromo - -- -SA/AV b 2 - Epinephrine +++ ++ +SA/AV ++ V/C V/D

Beta Blockers and Epinephrine As the previous slide shows, beta blockers and epinephrine have virtually opposite effects. Clinically this is why patients on beta blockers who are having an anaphylactic reaction can be very difficult to treat with epinephrine.

Glucagon Promotes gluconeogenesis Promotes production of c. AMP (including in the myocardium) Therefore can ‘get around’ beta blockade. Used for impacted food bolus in the esophagus, hypoglycemia, blocker overdose or in patients on beta blockers having anaphylactic reactions Dose: 1 – 2 mg Glucagon IV

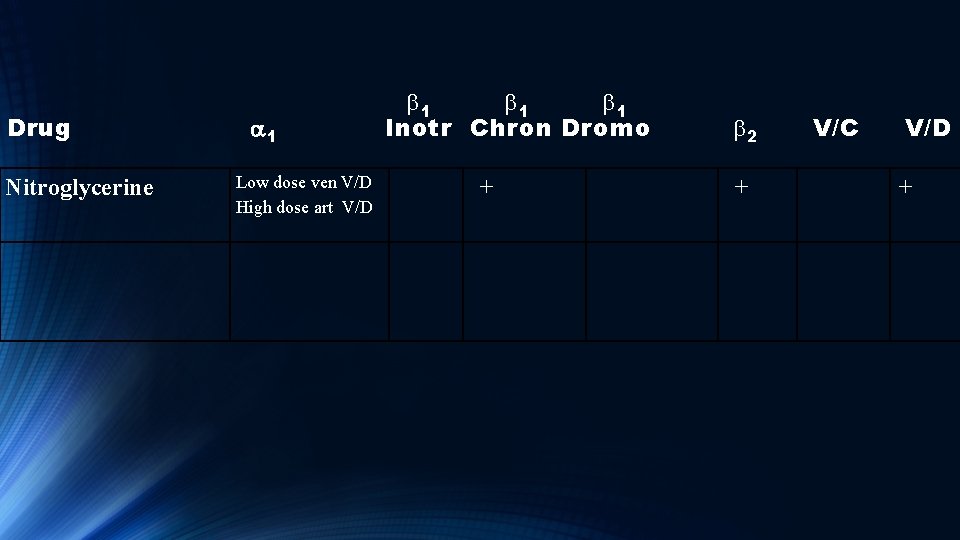
Drug Nitroglycerine a 1 Low dose ven V/D High dose art V/D b 1 b 1 Inotr Chron Dromo + V/C b 2 + V/D +

Nitroglycerin • Predominately a venodilator, but at high doses is also an arteriodilator. • Reduces preload and afterload. • Preload reduction (venous V/D) decreases myocardial O 2 demand. • Afterload reduction increases stroke volume and ejection fraction • Active metabolite is Nitric Oxide (not nitrous oxide!)

Nitroglycerin – bioavailability • Oral table Nitro - < 1% bioavailable due to liver metabolism. • SL nitro – onset 1 -2 minutes and ~ 30 -40% bioavailable. • So a 400 mcg spray dose has about 100 + mcg plasma level for 4 -5 minutes • Nitro patch – takes 15 minutes before any plasma level is detectable and peaks by 3 -4 hours. Is about 60 -70% bioavailable. • So a 400 mcg patch will have about 250 mcg plasma level but will take up to 2 hours to attain that level.

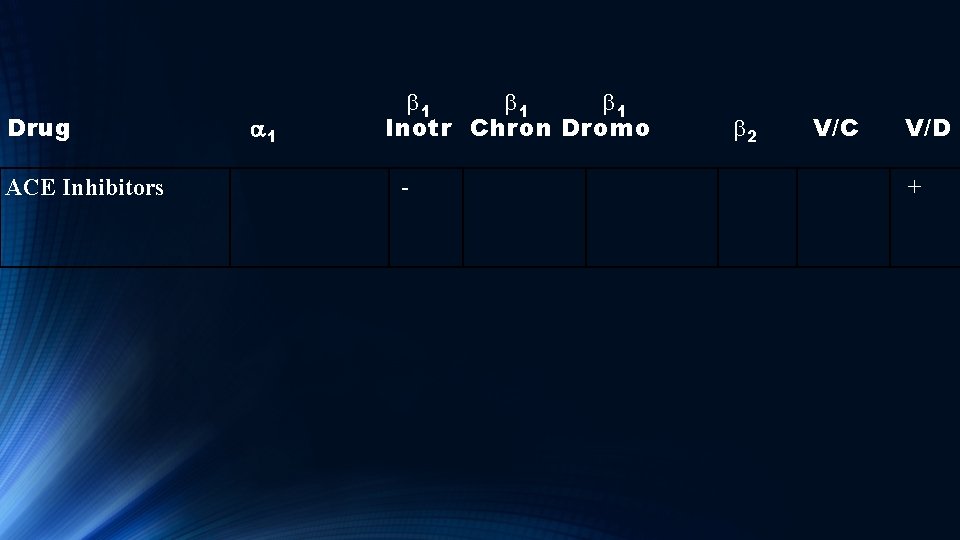
Drug ACE Inhibitors a 1 b 1 b 1 Inotr Chron Dromo - V/C b 2 V/D +

ACE Inhibitors Reduce afterload and preload via vasodilation (inhibiting angiotension II) which in turn improve oxygen to tissue.

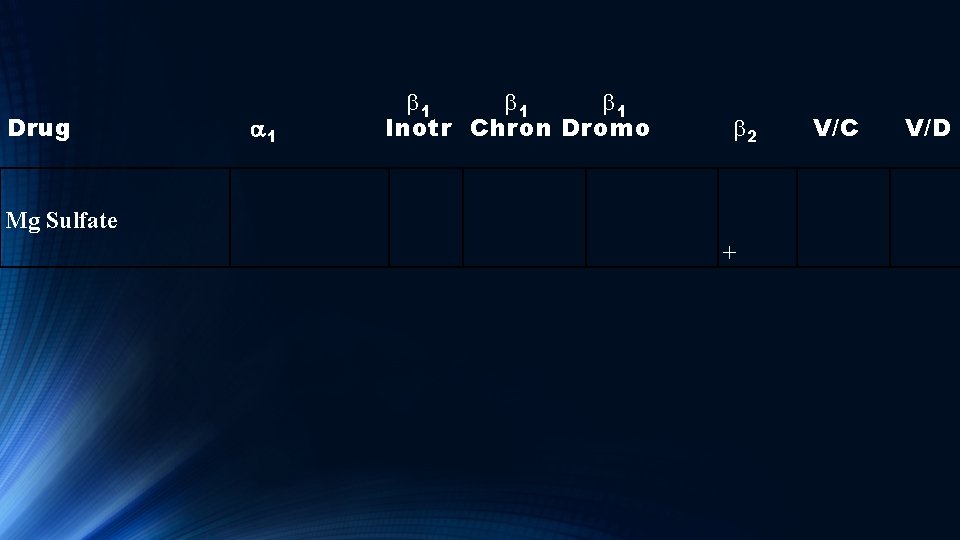
Drug a 1 b 1 b 1 Inotr Chron Dromo V/C b 2 Mg Sulfate + V/D

Magnesium Sulfate Has Beta 2 agonist properties which is why it can be used in asthmatics. It also lowers systolic blood pressure without affecting diastolic blood pressure, thus its use in eclampsia. Slows SA /AV node recovery time and slows antegrade and retrograde conduction over accessory pathways. Thus its use in WPW, AVNRT, MAT, polymorphic VT, VF

Drug a 1 b 1 b 1 Inotr Chron Dromo b 2 V/C V/D Phentolamine ++

Phentolamine Use in extravasation injuries from vasopressors (ie norepi, vasopressin, epinephrine. . ) Prevention of extravasation injuries: 1. Avoid hand wrist IVs for pressors 2. Avoid lousy IV’s generally for pressors 3. Can add 10 mg Phentolamine to each liter of IV solution containing norepinephrine. 4. Did I mention avoiding crappy peripheral IVs?

Treatment Steps: Phentolamine 1. Stop the IV but don’t remove it. 2. Start the vasopressor in another line. 3. Suck out as much as you can from the blown IV. 4. Comes in 5 mg per 1 ml vial. Place in 9 ml of N/S 5. Administer up to 0. 2 mg/kg into the catheter and S. C. around the site 6. Watch for systemic hypotension (should be on a pressor) 7. Call plastics.

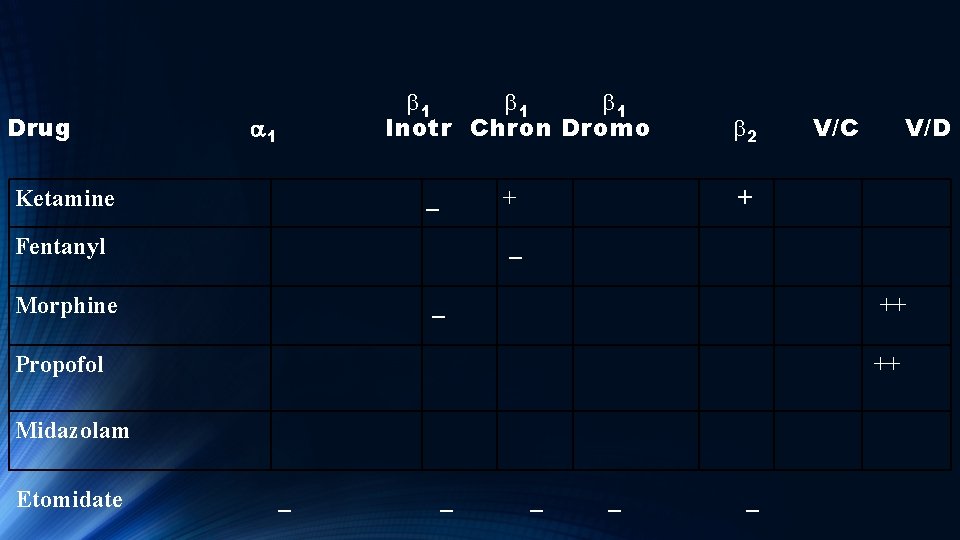
Drug Ketamine a 1 b 1 b 1 Inotr Chron Dromo _ + b 2 + V/C V/D

Ketamine - Interacts with at least 10 different receptors. - One of these are the opioid receptors - Negative inotrope but due to secondary CNS simulation causes increase in pulmonary BP, heart rate, cardiac output and myocardial O 2 demand. - Usually there will be no change in systemic vascular resistance. - Possesses bronchodilator activity (used in asthma intubations) - Does not increase ICP. (Neuro. Crit. Care Aug 2014)

Ketamine Dosing - Analgesic dosing (sub dissociative) – 0. 1 - 0. 2 mg/kg - Procedural sedation (sub dissociative) – 0. 25 – 0. 5 mg/kg. Can be associated with ‘nightmare’ like haze. - Dissociative dose (intubation) 1 – 2 mg/kg - Withdrawal agitation associated more with younger age, co-morbidity and dose. (~15 - 35%)

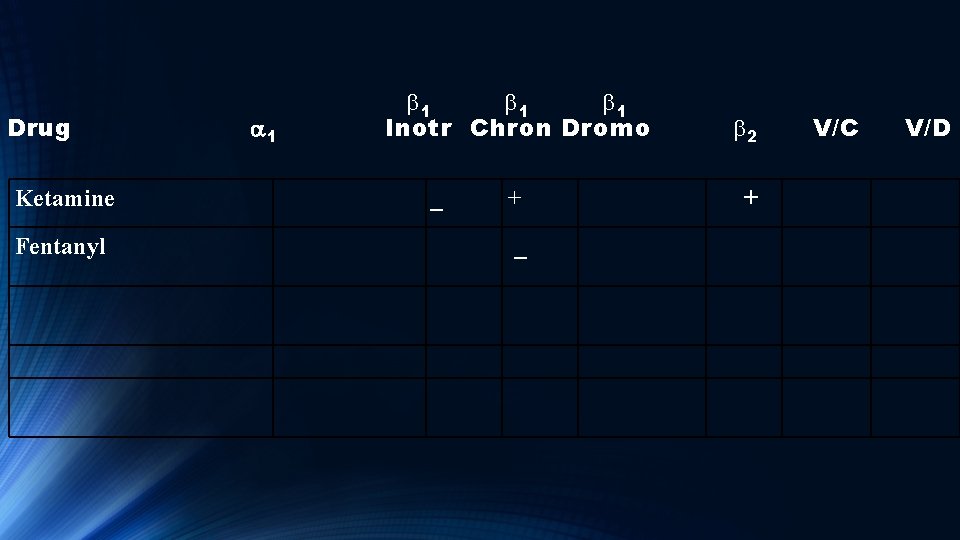
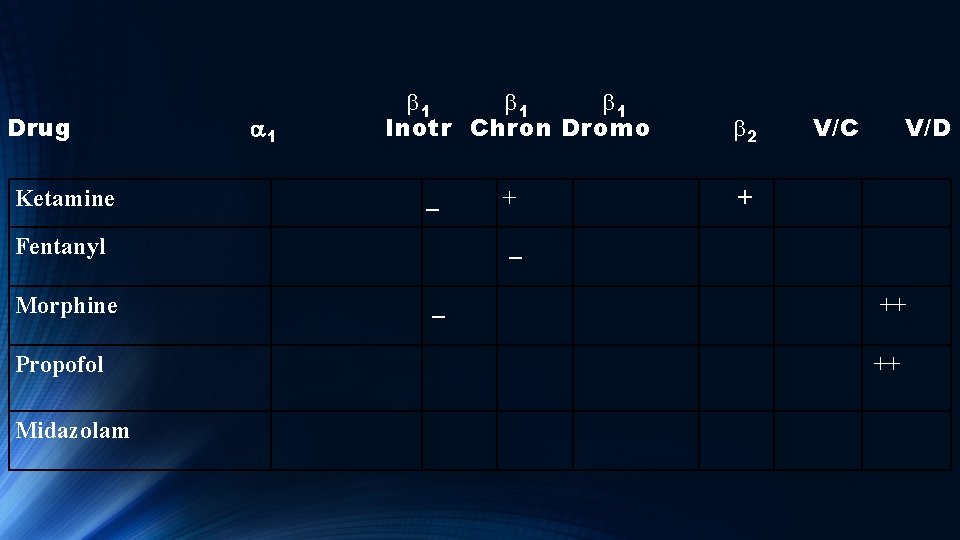
Drug b 1 b 1 Inotr Chron Dromo a 1 Ketamine Fentanyl V/C b 2 V/D + _ + _

Fentanyl Usually has minimal or no effect on BP, LV Pressure and cardiac output. Initial large boluses can decrease MAP. May have some negative Chronotropy (decrease HR) that can be treated with atropine. Addition of benzodiazepines can cause CV depression

Alfentanil Opioid analgesic 1/4 - 1/10 as potent as Fentanyl. Can be used in sublingual form for pain control Single injection can last up to 30 minutes, S. L. 10 -15 minutes. Usual dose is 8 - 40 mcg/kg IV, 0. 56 mg SL Onset of action IV is 4 times faster than Fentanyl Very few CV effects other than bradycardia Side effects can be respiratory depression, muscle rigidity

Remifentanil Opioid analgesic Approximately twice as potent as Fentanyl. Usually used as an infusion. Very short half life ~ 4 minutes (1 – 11 minutes) Causes decrease HR, BP, RR, tidal volume. Side effects can be muscle rigidity (dose and speed related), pruritus

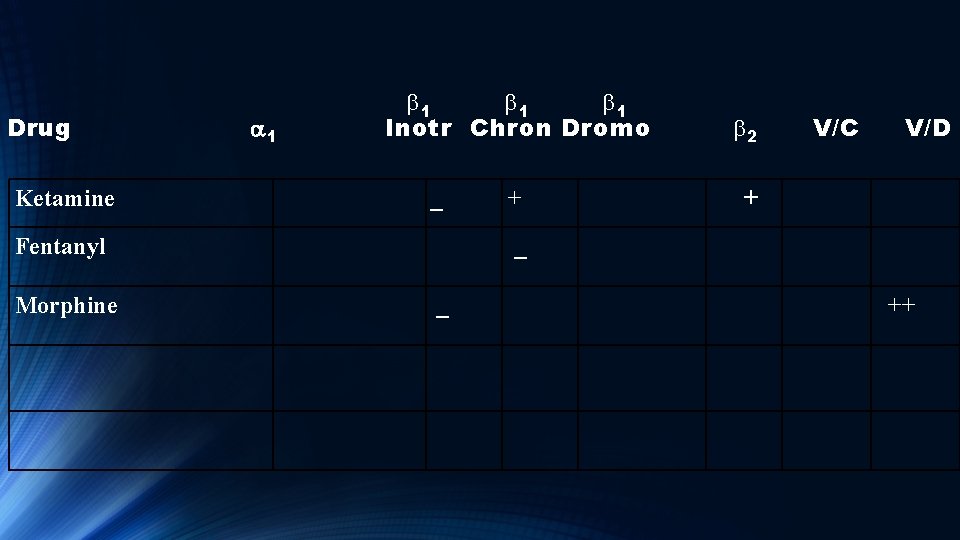
Drug b 1 b 1 Inotr Chron Dromo a 1 Ketamine Fentanyl Morphine V/C b 2 V/D + _ + _ ++

Morphine Lowers BP via decreasing alpha adrenergic tone mediated through the CNS.

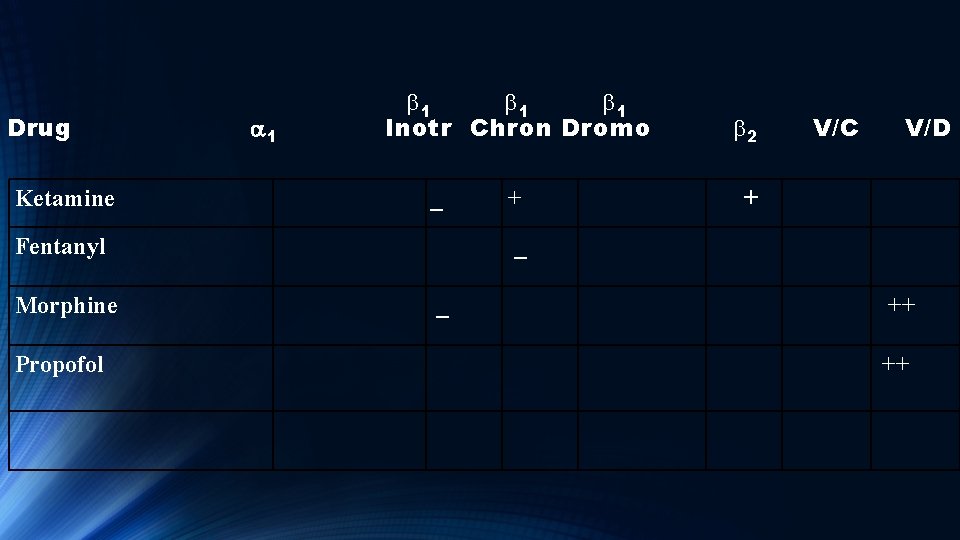
Drug b 1 b 1 Inotr Chron Dromo a 1 Ketamine Fentanyl Morphine Propofol V/C b 2 V/D + _ + _ ++

Propofol Can cause large reduction in MAP via venous and arterial vasodilation. It also blocks normal baroreceptor mediated tachycardia which would normally counteract these changes.

Drug a 1 Ketamine Fentanyl Morphine b 1 b 1 Inotr Chron Dromo V/C b 2 V/D + _ + _ ++ Propofol ++ Midazolam

Midazolam Has minimal CV effects. ie ‘a clean drug’. Since Fentanyl also has minimal CV effects, these two drugs have been used a lot together over the years.

Drug a 1 Ketamine Fentanyl Morphine b 1 b 1 Inotr Chron Dromo V/C b 2 V/D + _ + _ ++ Propofol ++ Midazolam Etomidate _ _ _ _

Etomidate Ultra short acting nonbarbiturate general anesthetic Onset of action – 30 – 60 seconds. Duration 2 – 3 minutes. Has minimal CV effects. Dosage: RSI 0. 3 mg/kg IV push over 30 - 60 seconds Procedural sedation: Initial: 0. 1 to 0. 2 mg/kg IV, followed by 0. 05 mg/kg every 3 to 5 minutes prn.

Questions ?

Mixing Phenylephrine and Epinephrine Phenylephrine: With a 5 ml syringe, draw 1 ml of 50 mg/ml (1 vial) Phenylephrine. Mix it in 100 cc minibag of normal saline Draw out 3 – 5 cc of solution. This is now Phenylephrine 100 mcg/ml Put labels on both the minibag and the syringe Dose is 50 – 100 mcg/min ie give 0. 5 – 1 ml q 2 -5 minutes. Action is within 1 minutes and lasts for 10 -20 min.

Mixing Phenylephrine and Epinephrine: Take a 10 cc N/S syringe. Discard 1 cc. Take a preloaded syringe of Epi 1: 10, 000 from the cardiac drawer. Take the bottom stopper off the syringe. With the 9 cc Saline syringe, draw out 1 cc Epi (1: 10, 000) You now have 10 mls of Epinephrine 10 mcg/ml Dose is 0. 5 – 2 ml (5 -20 mcg) q 2 -5 min Onset 1 minute, duration 2 -5 minutes.