Episiotomy DEFINITION Episiotomy is incision of the pudenda
























- Slides: 44

Episiotomy DEFINITION -Episiotomy is incision of the pudenda. Perineotomy is incision of the perineum. The term episiotomy often is used synonymously with perineotomy, (a practice that we follow. ) The incision may be made in the midline, creating a median or midline episiotomy. It may also begin in the midline but be directed laterally and downward away from the rectum, termed a mediolateral episiotomy. ( lateral , J shaped) 1

Episiotomy Purposes of Episiotomy Substitution of a straight surgical incision, which is easier to repair, for the ragged laceration that otherwise might result. Postoperative pain is less and healing improved with an episiotomy compared with a tear. (appeared to be incorrect (Larsson and colleagues, 1991 ) It prevented pelvic floor complications—that is, vaginal wall support defects and incontinence. (A number of observational studies and randomized trials, however, showed that routine episiotomy is associated with an increased incidence of anal sphincter and rectal tears (Angioli, 2000; Eason, ) 2

Episiotomy Carroli and Mignini (2009) reviewed the Cochrane Pregnancy and Childbirth Group trials registry. There were lower rates of posterior perineal trauma, surgical repair, and healing complications in the restricted-use group. Alternatively, the incidence of anterior perineal trauma was lower in the routine-use group. With these findings came the realization that episiotomy did not protect the perineal body and contributed to anal sphincter incontinence by increasing the risk of third- and fourth-degree tears. Signorello and associates (2000) reported that fecal and flatus incontinence were increased four- to six fold in women with an episiotomy compared with a group of women delivered with an intact perineum. Even compared with spontaneous lacerations, episiotomy tripled the risk of fecal incontinence and doubled it for flatus incontinence 3

Episiotomy Why episiotomy is given --- aim & objective 1. Widens the introitus easy delivery 2. Reduces overstretching of vaginal fascia & muscles 3. Reduces compression on fetal head INDICATIONS: 1. Primi & multi with rigid perineum 2. When perineal tears are expected – big baby Face to pubis delivery breech, OP, MA Face Shoulder dystocia 3. Operative delivery forceps, vaccum 4. Prior perineal surgery—CPT , to avoid undoing of repair 4

Episiotomy Indications-ct The American College of Obstetricians and Gynecologists (2006) has concluded that restricted use of episiotomy is preferred to routine use. The procedure should be applied selectively for appropriate indications. These include fetal indications such as shoulder dystocia and breech delivery, forceps or vacuum extractor deliveries, occiput posterior positions, and instances in which failure to perform an episiotomy will result in perineal rupture. There is no substitute for surgical judgment and common sense. 5

Episiotomy Timing of Episiotomy If performed unnecessarily early, bleeding from the episiotomy may be considerable during the interim between incision and delivery. If it is performed too late, lacerations will not be prevented. Typically, episiotomy is completed when the head is visible during a contraction to a diameter of 3 to 4 cm. When used in conjunction with forceps delivery, most perform an episiotomy after application of the blades 6

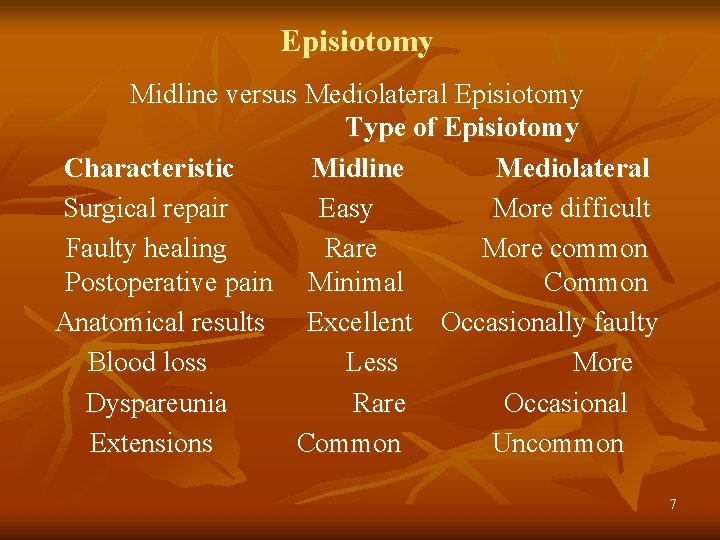
Episiotomy Midline versus Mediolateral Episiotomy Type of Episiotomy Characteristic Midline Mediolateral Surgical repair Easy More difficult Faulty healing Rare More common Postoperative pain Minimal Common Anatomical results Excellent Occasionally faulty Blood loss Less More Dyspareunia Rare Occasional Extensions Common Uncommon 7

Episiotomy ALL ARE THE ADVANTAGES IN MEDIAN-- LIKE Muscles not cut Less blood loss Repair easy PO-pain is < Heals nicely wound disruption is minimal Dysparunia is least BUT, STILL IT IS NOT GIVEN ROUTINELY---WHY ? If extended involves anal opening & rectum Can not be extended if required eg. Breech, OP, Operative SO, MEDIOLATERAL EPISIOTOMY IS ROUTINELY GIVEN 8

Episiotomy Except for the important issue of third- and fourthdegree extensions, midline episiotomy is superior. (Anthony and colleagues (1994) ) Kudish and co-workers (2006) advised against midline episiotomy with operative vaginal delivery because of an increased incidence of anal sphincter tears. 9

Episiotomy Repair Typically, episiotomy repair is deferred until the placenta has been delivered. (This policy permits undivided attention to the signs of placental separation and delivery. ) A further advantage is that episiotomy repair is not interrupted or disrupted by the obvious necessity of delivering the placenta, especially if manual removal must be performed. The major disadvantage is continuing blood loss until the repair is completed. 10

Episiotomy 1. 2. 3. 4. Technique There are many ways to close an episiotomy incision, but hemostasis and anatomical restoration without excessive suturing are essential for success with any method. Adequate analgesia is imperative. Blunt needles are suitable and likely decrease the incidence of needlestick injuries. The suture material commonly used is 2 -0 11 chromic catgut.

Episiotomy Sutures made of polyglycolic acid derivatives are also commonly used. -( vicryl 1 -0 or 2 -0 ) A decrease in postsurgical pain is cited as the major advantage of synthetic materials. ( However, closures with these materials occasionally require suture removal from the repair site because of pain or dyspareunia. ) Rapidly absorbed polyglactin 910 (Vicryl Rapids, Ethicon) is absorbed by 42 days 0 r standard polyglactin-vicryl 910 sutures absorbed by approximately 90 days. The continuous method is associated with less perineal pain ? 12

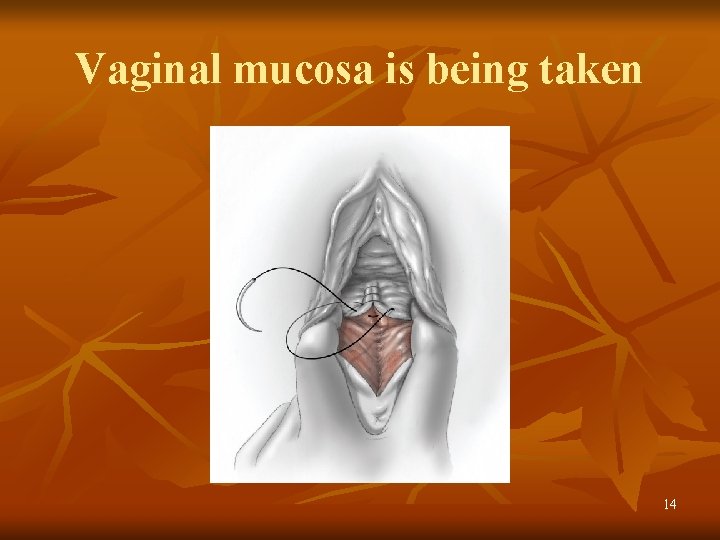
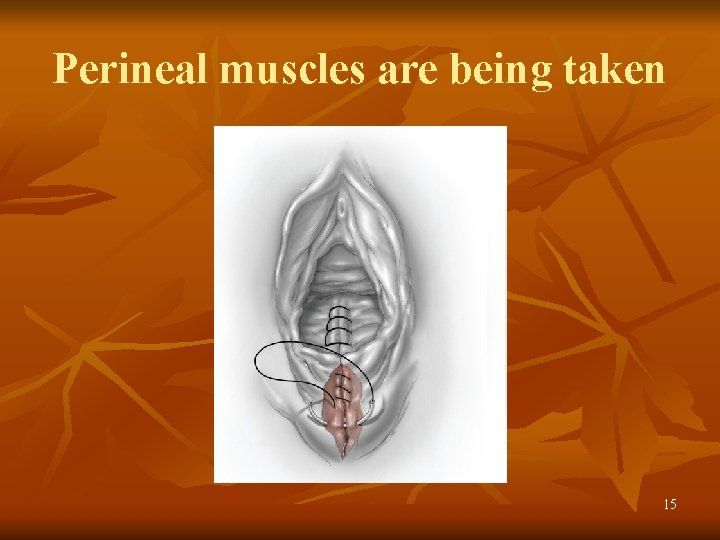
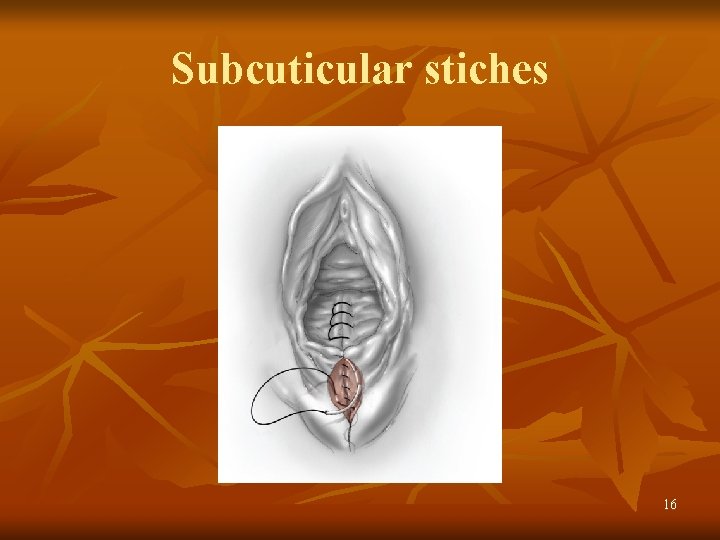
Episiotomy Repair of midline episiotomy. A. Disruption of the hymenal ring and bulbocavernosus and superficial transverse perineal muscle are seen within the diamondshaped incision following episiotomy. B. Absorbable 2 -0 or 3 -0 suture is used for continuous closure of the vaginal mucosa and submucosa. C. After closing the vaginal incision and reapproximating the cut margins of the hymenal ring, the needle and suture are positioned to close the perineal incision. D. A continuous closure with absorbable 2 -0 or 3 -0 suture is used to close the fascia and muscles of the incised perineum. E. The continuous suture is then carried upward as a subcuticular stitch. F The final knot is, tied proximally to the hymenal ring. 13

Vaginal mucosa is being taken 14

Perineal muscles are being taken 15

Subcuticular stiches 16

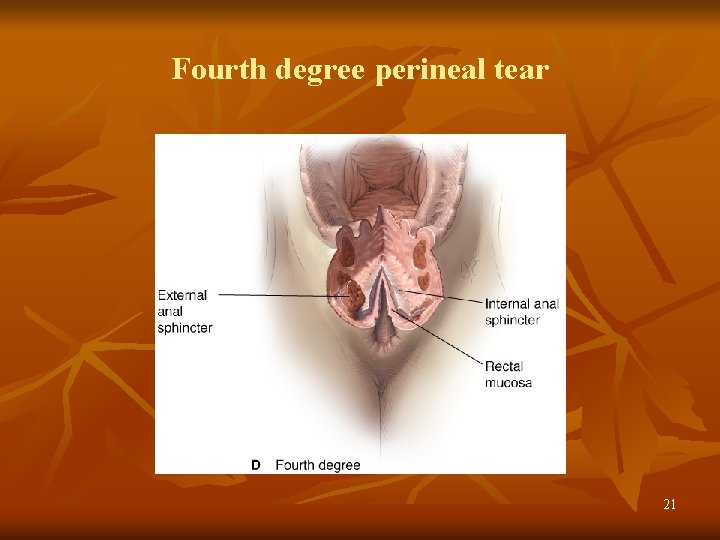
BIRTH CANAL INJURIES PERINEAL TEARS CAUSE: A). POWER– Rapid delivery in Precipitate labor Forceps delivery B). PASSAGE– Inelastic / rigid perineum– in elderly, scarred perineum narrow pubic arch presenting part moves posteriorly C). PASSANGER– Large fetus, Abnormal position –face to pubis Abnormal presentation-face DEGREES I II III Vaginal mucosa & perineal skin +…. . . +…………+ Perineal body --………. . +. . . . + Anal Sphin. And/or anal canal or rectum --…………+ Central tear or rupture of perineum =IV degree 17

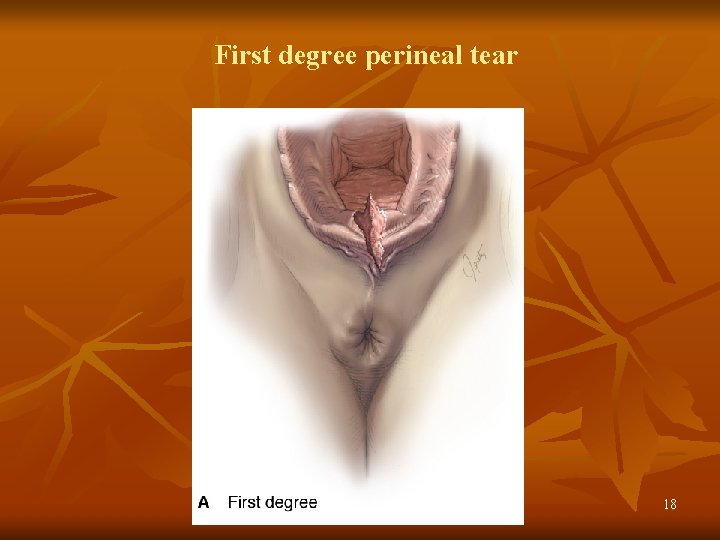
First degree perineal tear 18

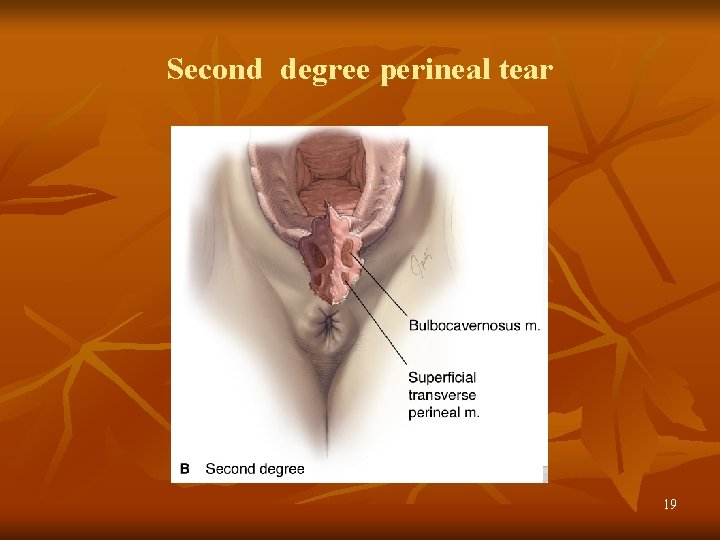
Second degree perineal tear 19

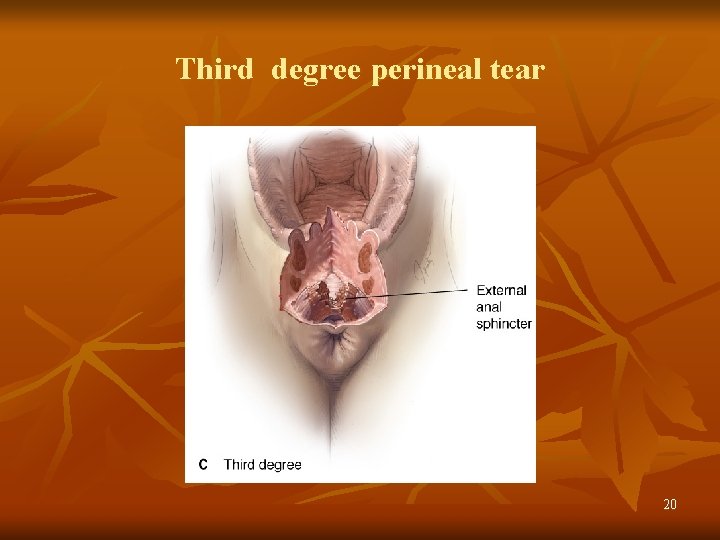
Third degree perineal tear 20

Fourth degree perineal tear 21

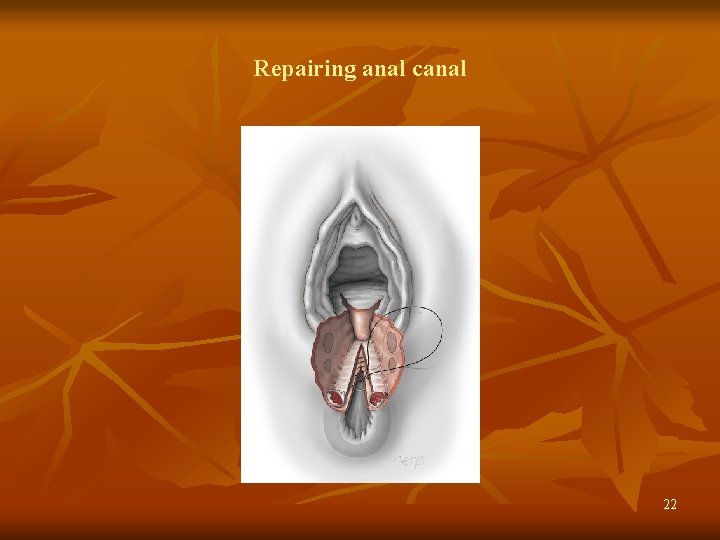
Repairing anal canal 22

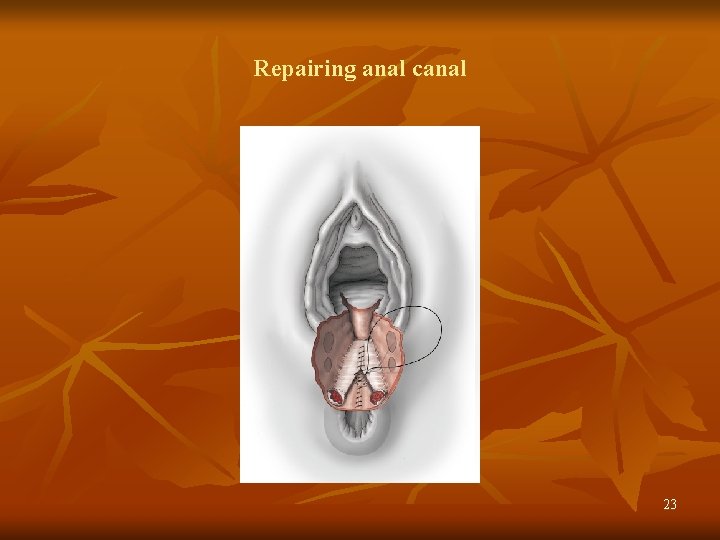
Repairing anal canal 23

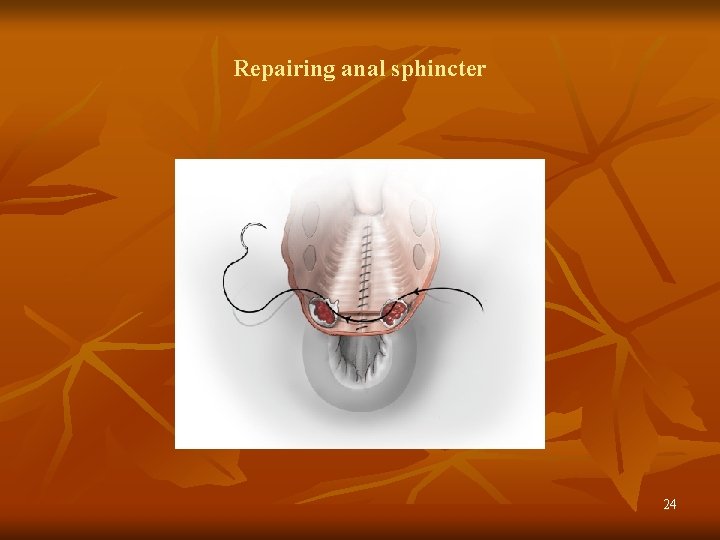
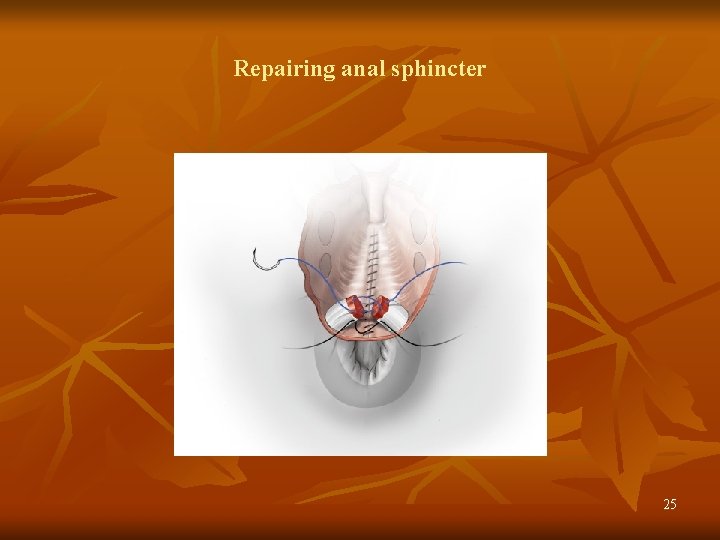
Repairing anal sphincter 24

Repairing anal sphincter 25

BIRTH CANAL INJURIES PREVENTION OF PERINEAL TEARS: 1. Maintain flexion of head till sub occiput hinges under SP 2. Avoid forcible delivery of head– ask patient not to bear down 2. Ritgen maneuver—Deliver head in between contractions 4. Timely episiotomy 5. Care during shoulder delivery—larger diameter delivers SUTURING & AFTER CARE– LIKE EPISIOTOMY 26

BIRTH CANAL INJURIES VAGINAL TEARS Usually seen with instrumental or manipulative delivery Varies depth wise & direction wise Suturing always with absorbable sutures—ch. catgut “ 0”/ vicryl 1 -0/ vicryl rapide COLPORRHEXIS= rupture of vault of vagina usually post fornix Primary= only vault, Secondary=vault + cervix Complete= peritoneum gets also open SUTURING by laparotomy if lower segment is also involved 27

BIRTH CANAL INJURIES CERVICAL TEARS CAUSES: 1. Cervical pathology-- Rigid scarred cervix– operations like amputation Very vascular cervix--- Placenta praevia 2. Strong uterine contractions – precipitate labor 3. Iatrogenic – Forceps with incompletely dilated cervix 4. Prolonged compression of cervix bet. Head & pelvis – annular detachment COMMONEST SITE : - Left lateral – LOL is common 28

BIRTH CANAL INJURIES HOW will U DIAGNOSE CERVICAL TEARS ? Suspect if uterus is hard contracted & excessive bleeding P/V is there Confirm by P/S exam trace cervix with swab holders Suture by figure of “ 8”s sutures by absorbable suture material DANGERS: - PPH, Broad lig. hematoma, with inf. cellulitis, thrombophlebitis Cervical incompetence mid trimester abortions 29

BIRTH CANAL INJURIES PELVIC HEMATOMA Blood collection between pelvic peritoneum above & perineal skin below– Type: - Above or below levator Supra levator (rare), Infra levator (common) Commonest type of infra levator hematoma is vulval hematoma INFRA LEVATOR HEMATOMA -- VULVAL HEMATOMA AETIOLOGY: 1. Improper hemostasis while suturing episiotomy or perineal tears 2. Paravaginal venous plexus rupture– spontaneous / instrumental delivery 30

BIRTH CANAL INJURIES PELVIC HEMATOMA DIAGNOSIS: SYMPTOMS: Severe pain on perineal region, rectal tenesmus may be there SIGNS: TPR BP– Shock Tense tender purple color swelling at vulva (over the suture line) TREATMENT: Explore under G/A --. Secure bleeder, obliterate dead space , AB , BT sos 31

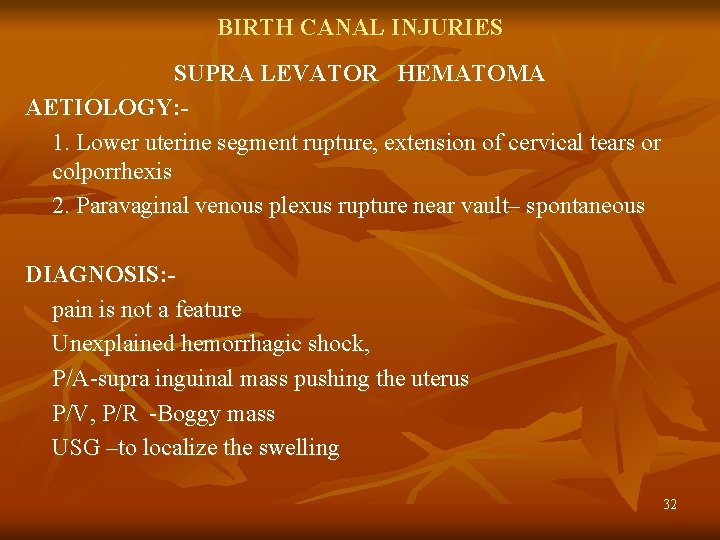
BIRTH CANAL INJURIES SUPRA LEVATOR HEMATOMA AETIOLOGY: 1. Lower uterine segment rupture, extension of cervical tears or colporrhexis 2. Paravaginal venous plexus rupture near vault– spontaneous DIAGNOSIS: pain is not a feature Unexplained hemorrhagic shock, P/A-supra inguinal mass pushing the uterus P/V, P/R -Boggy mass USG –to localize the swelling 32

BIRTH CANAL INJURIES TREATMENT: Laparotomy Open ant. Leaf of broad lig. evacuate hematoma , secure the bleeders, protect ureter, hysterectomy s o s, Internal iliac ligation s o s 33

BIRTH CANAL INJURIES RUPTURE OF UTERUS DEF: Break in continuity of uterine wall beyond 28 wks of pregnancy INCIDENCE: 1: 200 ---1: 2000 , static, ‘cause of increase in scar rupture now 34

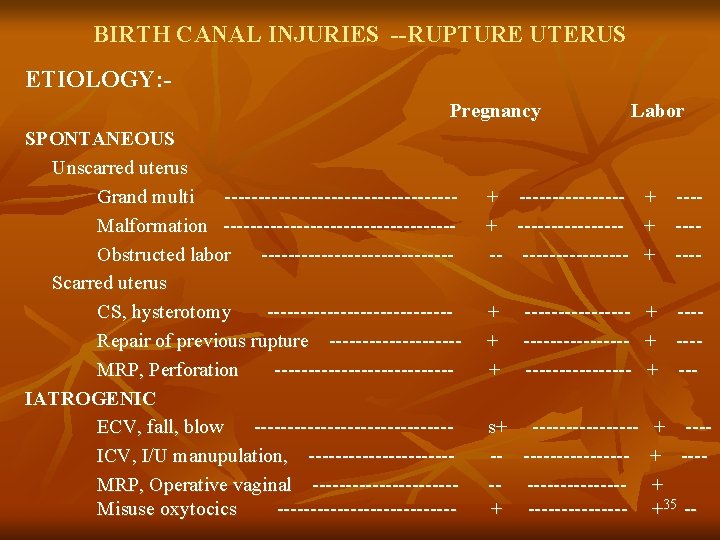
BIRTH CANAL INJURIES --RUPTURE UTERUS ETIOLOGY: Pregnancy SPONTANEOUS Unscarred uterus Grand multi -----------------Malformation -----------------Obstructed labor --------------Scarred uterus CS, hysterotomy --------------Repair of previous rupture ----------MRP, Perforation -------------IATROGENIC ECV, fall, blow ---------------ICV, I/U manupulation, -----------MRP, Operative vaginal -----------Misuse oxytocics -------------- Labor + + -- ----------------------- + + + ----------------------- + ---+ --- s+ -----------------+ -------- + ---+ +35 --

BIRTH CANAL INJURIES --RUPTURE UTERUS TYPE OF RUPTURE: Complete– peritoneum involved Incomplete– peritoneum intact SITE OF RUPTURE: SPONTANEOUS--- Upper segment Complete OBSTRUCTED LABOR --- Lower segment & extends to US on side OXYTOCICS----- Lower segment & extends to US on side SCARRED--------Over the scar 36

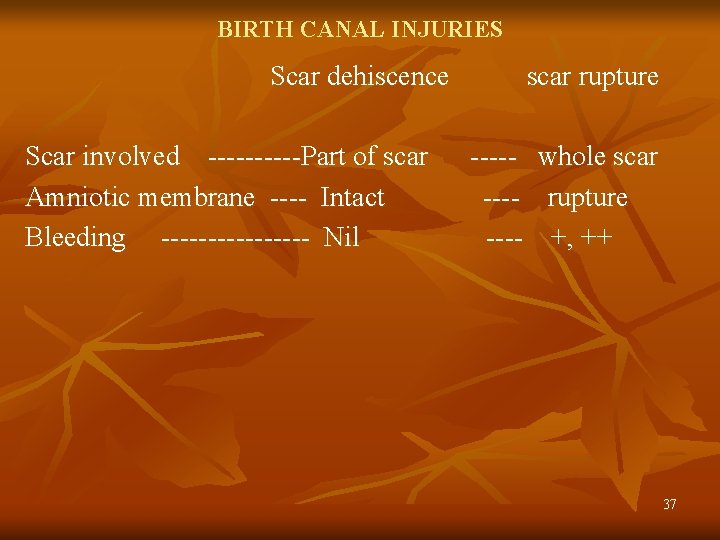
BIRTH CANAL INJURIES Scar dehiscence Scar involved -----Part of scar Amniotic membrane ---- Intact Bleeding -------- Nil scar rupture ----- whole scar ---- rupture ---- +, ++ 37

BIRTH CANAL INJURIES --RUPTURE UTERUS DIAGNOSIS: H/O etiological factors--- Grand multi, scar, perforation, versions, MRP oxytocics, prolonged obstructed labor, fall or blow, SYMPTOMS: LS scar rupture-----silent rupture Sense of giving way f/b acute abdomen collapse Vaginal bleeding IN obstructed labor >>> pains f/b pains stop f/b generalized pain 38

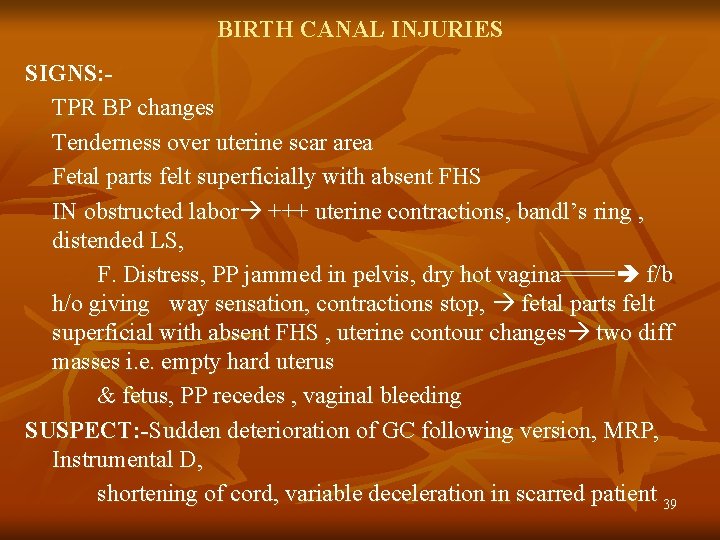
BIRTH CANAL INJURIES SIGNS: TPR BP changes Tenderness over uterine scar area Fetal parts felt superficially with absent FHS IN obstructed labor +++ uterine contractions, bandl’s ring , distended LS, F. Distress, PP jammed in pelvis, dry hot vagina==== f/b h/o giving way sensation, contractions stop, fetal parts felt superficial with absent FHS , uterine contour changes two diff masses i. e. empty hard uterus & fetus, PP recedes , vaginal bleeding SUSPECT: -Sudden deterioration of GC following version, MRP, Instrumental D, shortening of cord, variable deceleration in scarred patient 39

BIRTH CANAL INJURIES --RUPTURE UTERUS CAN IT BE PREVENTED: - ? ? ? -----YES ANTE NATAL 1. Pr. USCS, Hysterotomy, Pr. Rupture sutured === Elective CS to be done 2. CPD, Scarred uterus, Grand multi, ===== Hospital delivery 3. ECV ====== No G/A, No force 40

BIRTH CANAL INJURIES INTRA NATAL 4. Prolonged & obstructed labor == To be avoided, Treat early 5. Oxytocics ======== Sit with patient & monitor 6. Forceps with incomp. Dilated cervix Forbidden 7. IPV & Destructive operations === Judicious use or NO use 8. MRP ========= Be careful in hour glass contraction of uterus 41

BIRTH CANAL INJURIES --RUPTURE UTERUS TREATMENT: Resuscitation laparotomy or resuscitation+ laparotomy OPERATIONS DONE AT LAPAROTOMY A). HYSTERECTOMY– is choice unless sufficient reason is there to preserve it Sub total Hysterectomy v/s Total Hysterectomy B). REPAIR OF RUPTURE— If margins are clean & fresh (or freshen them) If patient wishes to preserve uterus for MC, Fertility C). REPAIR OF RUPTURE WITH TL— If fertility is not the issue SURGEON TO BE CALLED TO SHARE THE RESPONSIBILITY IF BLADDER INJURY IS ASSOCIATED 42

What is a lecture ? lecture is a process by which the knowledge is transferred from teacher’s notes to student’s notes without entering anybody’s brain 43

Episiotomy 44