Epilepsy DR Gheith A Bugaila MD American Epilepsy
Epilepsy DR. Gheith A. Bugaila, MD American Epilepsy Society 2010

Definitions • Seizure (Convulsion) • Clinical manifestation of synchronised electrical discharges of neurons • Epilepsy • Present when 2 or more unprovoked seizures occur at an interval greater than 24 hours apart • Provoked seizures • Seizures induced by disorders originating outside American Epilepsy Society 2010 the brain

• Aetiology of seizures • Epileptic § § § Idiopathic (70 -80%) Cerebral tumor Neurodegenerative disorders Neurocutaneous syndromes Secondary to § Cerebral damage: e. g. congenital infections, intraventricular hemorrhage § Cerebral dysgenesis/malformation: e. g. hydrocephalus § Non-epileptic § Febrile convulsions § Metabolic § Hypoglycemia § Hypo. Ca, Hypo. Mg, Hyper. Na, Hypo. Na § § Head trauma Meningitis Encephalitis Poisons/toxins American Epilepsy Society 2010
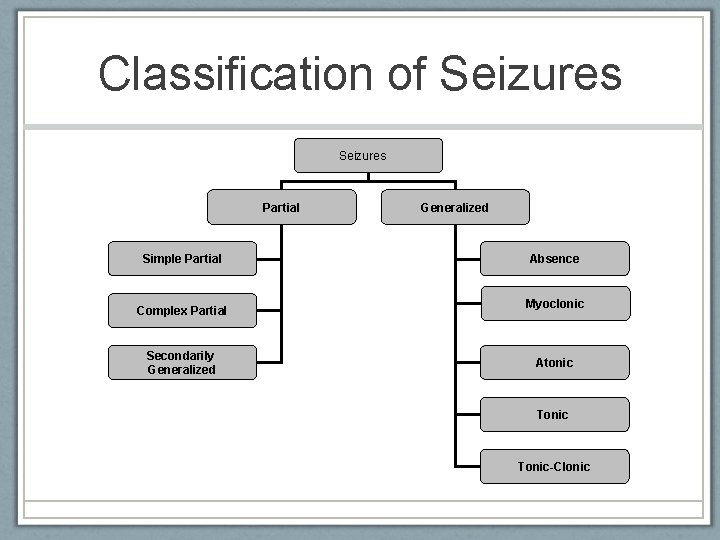
Classification of Seizures Partial Simple Partial Complex Partial Secondarily Generalized Absence Myoclonic Atonic Tonic-Clonic American Epilepsy Society 2010
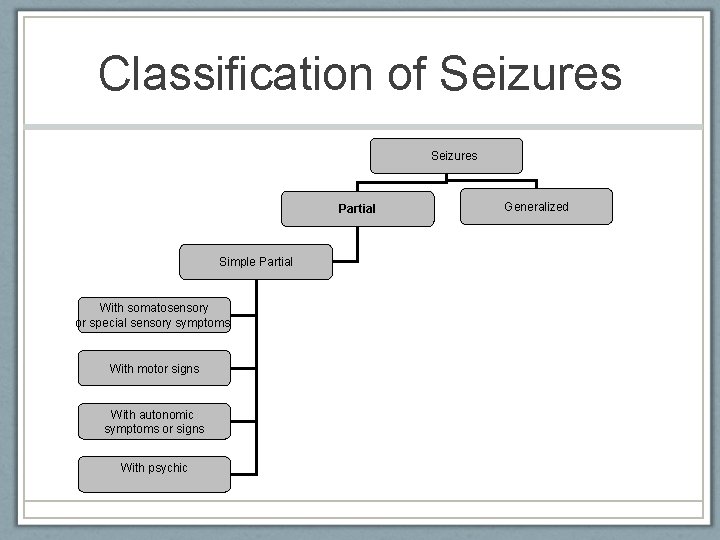
Classification of Seizures Partial Simple Partial With somatosensory or special sensory symptoms With motor signs With autonomic symptoms or signs With psychic American Epilepsy Society 2010 Generalized
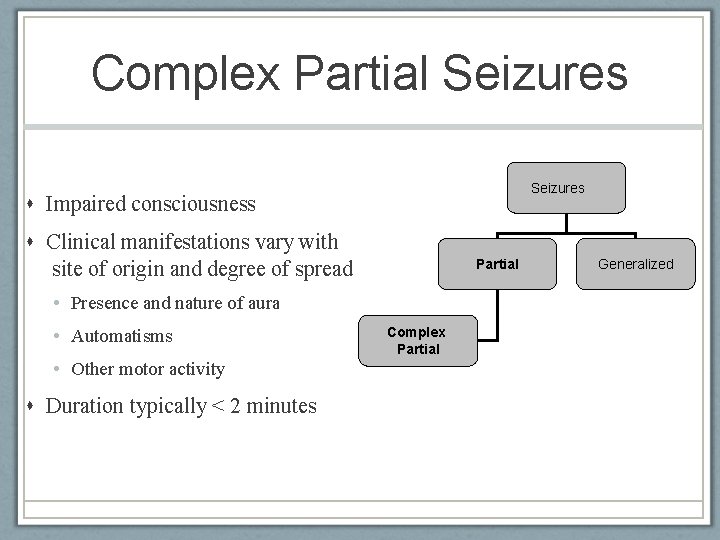
Complex Partial Seizures Impaired consciousness Clinical manifestations vary with site of origin and degree of spread Partial • Presence and nature of aura • Automatisms • Other motor activity Duration typically < 2 minutes American Epilepsy Society 2010 Complex Partial Generalized
Secondarily Generalized Seizures Begins focally Variable intensity, and duration of tonic (stiffening) and clonic (jerking) phases Typical duration 1 -3 minutes Postictal confusion, somnolence, with or without transient focal deficit American Epilepsy Society 2010
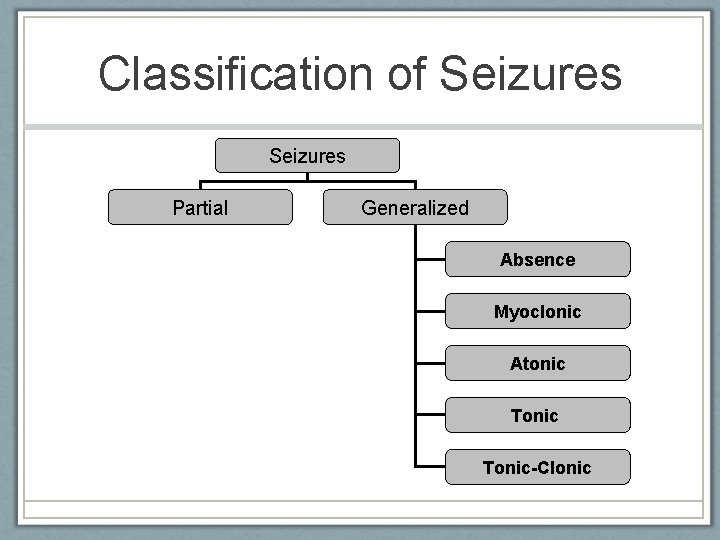
Classification of Seizures Partial Generalized Absence Myoclonic Atonic Tonic-Clonic American Epilepsy Society 2010
Typical Absence Seizures Brief staring spells (“petit mal”) with Seizures impairment of awareness 3 -20 seconds Sudden onset and sudden resolution Often provoked by hyperventilation Partial Generalized Onset typically between 4 and 14 years of age Often resolve by 18 years of age Normal development and intelligence American Epilepsy Society 2010 Absence
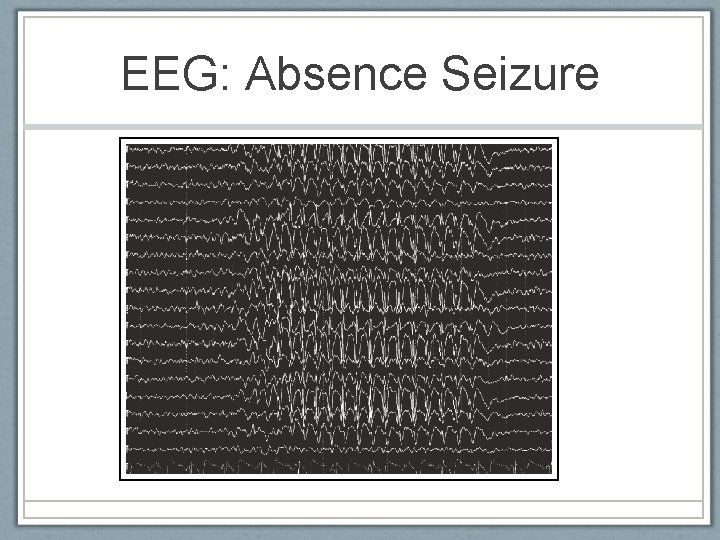
EEG: Absence Seizure American Epilepsy Society 2010
Myoclonic Seizures Epileptic Myoclonus Brief, shock-like jerk of a muscle or group of muscles Differentiate from benign, nonepileptic myoclonus (e. g. , while falling asleep) EEG: polyspike-wave discharges American Epilepsy Society 2010 Partial Generalized Myoclonic
Myoclonic Seizures American Epilepsy Society 2010
Tonic and Atonic Seizures Tonic seizures Symmetric, tonic muscle contraction of extremities with tonic flexion of waist and neck Duration - 2 -20 seconds. Partial Generalized Atonic seizures Tonic Sudden loss of postural tone When severe often results in falls When milder produces head nods or jaw drops. Atonic Consciousness usually impaired Duration - usually seconds, rarely more than 1 minute American Epilepsy Society 2010
Tonic and Atonic Seizures American Epilepsy Society 2010
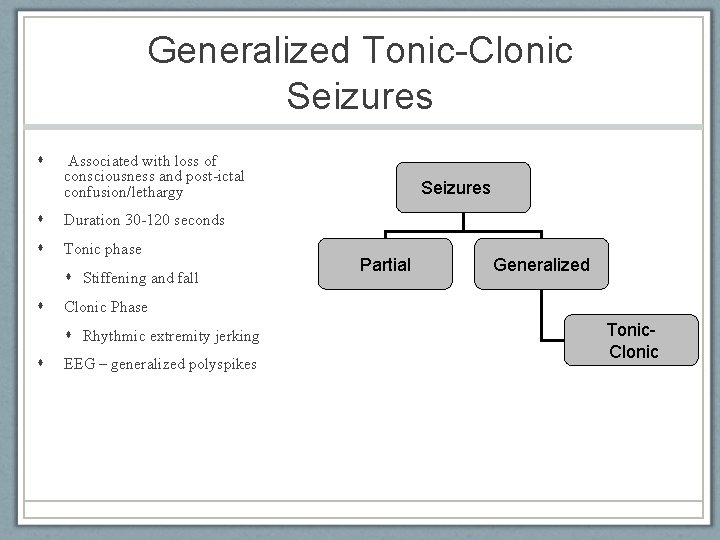
Generalized Tonic-Clonic Seizures Associated with loss of consciousness and post-ictal confusion/lethargy Duration 30 -120 seconds Tonic phase Stiffening and fall Partial Generalized Clonic Phase Rhythmic extremity jerking Seizures EEG – generalized polyspikes American Epilepsy Society 2010 Tonic. Clonic

Questions Raised by a First Seizure or not? Provoked? (ie metabolic precipitant? ) Seizure type? (focal vs. generalized) Evidence of CNS dysfunction? Syndrome type? Which studies should be obtained? Should treatment be started? Which drug should be used? American Epilepsy Society 2010

Evaluation of a First Seizure History, physical Blood tests: CBC, electrolytes, glucose, calcium, magnesium, phosphate, hepatic and renal function Lumbar puncture (only if meningitis or encephalitis suspected and potential for brain herniation is excluded) American Epilepsy Society 2010
Evaluation of a First Seizure, Con’t Blood or urine screen for drugs Electroencephalogram (EEG) CT or MR brain scan American Epilepsy Society 2010

Seizure Precipitants Metabolic and Electrolyte Imbalance Sedative or ethanol withdrawal Sleep deprivation Antiepileptic medication reduction or inadequate AED treatment Hormonal variations Stress Fever or systemic infection Concussion and/or closed head injury American Epilepsy Society 2010

Medical Treatment of First Seizure Whether to treat first seizure is controversial 16 -62% of unprovoked seizures will recur within 5 years Relapse rate may be reduced by antiepileptic drugs Relapse rate increased if: abnormal imaging abnormal neurological exam abnormal EEG family history Quality of life issues are important (ie driving) American Epilepsy Society 2010

Choosing Antiepileptic Drugs (cont. ) Monotherapy for Partial Seizures Best evidence and FDA indication: Carbamazepine, Oxcarbazepine, Phenytoin, Topiramate Similar efficacy, likely better tolerated: Lamotrigine, Gabapentin, Levetiracetam American Epilepsy Society 2010

Choosing Antiepileptic Drugs (cont. ) Monotherapy for Generalized-Onset Tonic-Clonic Seizures Best evidence and FDA Indication: Valproate, Topiramate Also shown to be effective: , Levetiracetam Phenytoin, Carbamazepine (may exacerbate absence and myoclonic ) Lamotrigine (may exacerbate myoclonic of symptomatic generalized epilepsies) American Epilepsy Society 2010

Choosing Antiepileptic Drugs (cont. ) Absence seizures Best evidence: Ethosuximide (limited spectrum, absence only) Valproate Also shown to be effective: Lamotrigine May be considered as second-line: Levetiracetam, Topiramate, , Clonazepam American Epilepsy Society 2010

Choosing Antiepileptic Drugs (cont. ) Myoclonic Seizures Best evidence: Valproate Levetiracetam (FDA indication as adjunctive tx) Clonazepam (FDA indication) Possibly effective: Topiramate American Epilepsy Society 2010

Adverse Effects of AEDs: Common Typically dose-related: Dizziness , Fatigue , Ataxia, Diplopia all AEDs Irritability levetiracetam Word-finding difficulty topiramate Weight loss/anorexia topiramate, Weight gain valproate (also associated with polycystic ovarian syndrome ) carbamazepine, gabapentin, pregabalin American Epilepsy Society 2010

Adverse Effects of AEDs: Serious Renal stones topiramate Anhydrosis, heat stroke topiramate Acute closed-angle glaucoma topiramate Hyponatremia carbamazepine, oxcarbazepine American Epilepsy Society 2010

Adverse Effects of AEDs: Serious Aplastic anemia valproate, carbamazepine Hepatic Failure valproate, lamotrigine, phenobarbital Peripheral vision loss vigabatrin Rash phenytoin, lamotrigine, carbamazepine American Epilepsy Society 2010

Discontinuing AEDs Seizure freedom for 2 years Favorable factors • • Control achieved easily on one drug at low dose No previous unsuccessful attempts at withdrawal Normal neurologic exam and EEG Primary generalized seizures Consider relative risks/benefits (e. g. , driving, pregnancy) American Epilepsy Society 2010

Non-Drug Treatment/ Lifestyle Modifications Adequate sleep Avoidance of alcohol, stimulants, etc. Avoidance of known precipitants, eg computer, TV … Stress reduction — specific techniques American Epilepsy Society 2010

Patient Selection for Surgery Epilepsy syndrome not responsive to medical management • Unacceptable seizure control despite maximum tolerated doses of 2 -3 appropriate drugs Epilepsy syndrome amenable to surgical treatment American Epilepsy Society 2010

Surgical Treatment Potentially curative • Resection of epileptogenic region (“focus”) Palliative • Partial resection of epileptogenic region • Disconnection procedure to prevent seizure spread • Callosotomy American Epilepsy Society 2010

Status Epilepticus Definition • More than 10 minutes of continuous seizure activity or • Two or more sequential seizures without full recovery between seizures American Epilepsy Society 2010

Status Epilepticus (SE) A medical emergency • Adverse consequences can include hypoxia, hypotension, hyperthermia, rhabdomyolysis and neuronal injury • Goal: stop seizures as soon as possible American Epilepsy Society 2010

SE Treatment Algorithm One commonly used treatment algorithm is: First 5 minutes: • Check emergency ABC’s • Give O 2 • Obtain IV access • Begin ECG monitoring • Check fingerstick glucose • Draw blood for, Magnesium, Calcium, Phosphate, CBC, LFTs, AED levels, ABG, troponin • Toxicology screen (urine and blood). American Epilepsy Society 2010

SE Treatment Algorithm 6 -10 minutes • Thiamine 100 mg IV; 50 ml of D 50 IV unless adequate glucose known. • Lorazepam 4 mg IV over 2 mins; if needed repeat in 5 mins. • If no rapid IV access give diazepam 20 mg PR or midazolam 10 mg intranasally, buccally or IM. American Epilepsy Society 2010

SE Treatment Algorithm 10 -20 minutes: • If seizures persist, begin phenytoin 15 -20 mg/kg at 25 -50 mg/min or fosphenytoin 20 mg/kg IV at 150 mg/min, with blood pressure and ECG monitoring. S/E hypotension and AV conduction abnormalities • Then give a maintenance dose IF seizure persist Intubate the pateint and give continues iv midazolam Or continues iv propofol Or iv phenobarbital American Epilepsy Society 2010 >Now the pt is intubated and under generalized

Differential Diagnosis of seizure Syncope Cardiac (Arrhythmia) Non-Cardiac Syncope (Vasovagal) Metabolic (Hypoglycemia) Movement Disorders (Paroxysmal Dyskinesia) Or psychogenic seizures American Epilepsy Society 2010
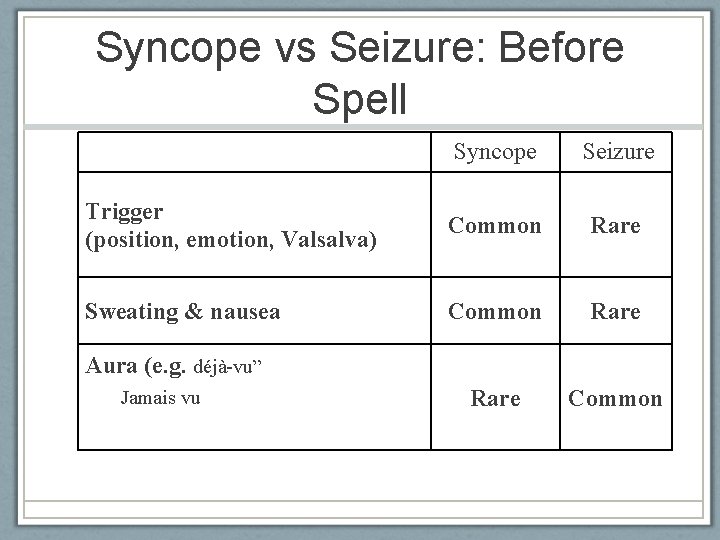
Syncope vs Seizure: Before Spell Syncope Seizure Trigger (position, emotion, Valsalva) Common Rare Sweating & nausea Common Rare Common Aura (e. g. déjà-vu” Jamais vu American Epilepsy Society 2010
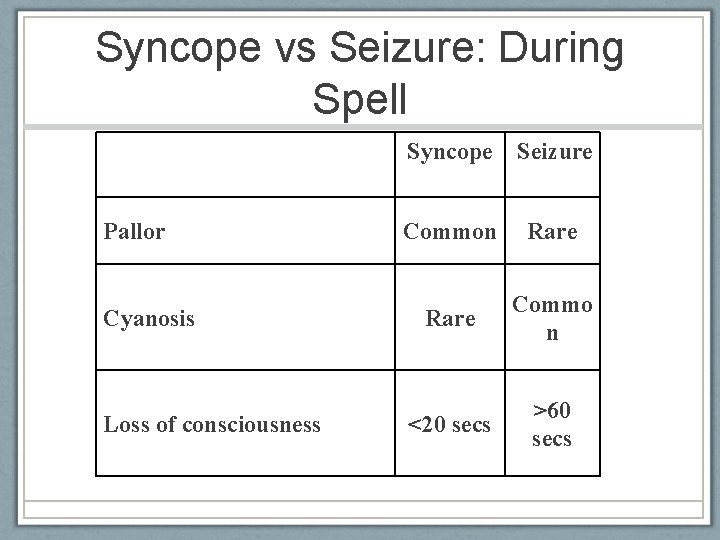
Syncope vs Seizure: During Spell Pallor Cyanosis Loss of consciousness American Epilepsy Society 2010 Syncope Seizure Common Rare Commo n <20 secs >60 secs
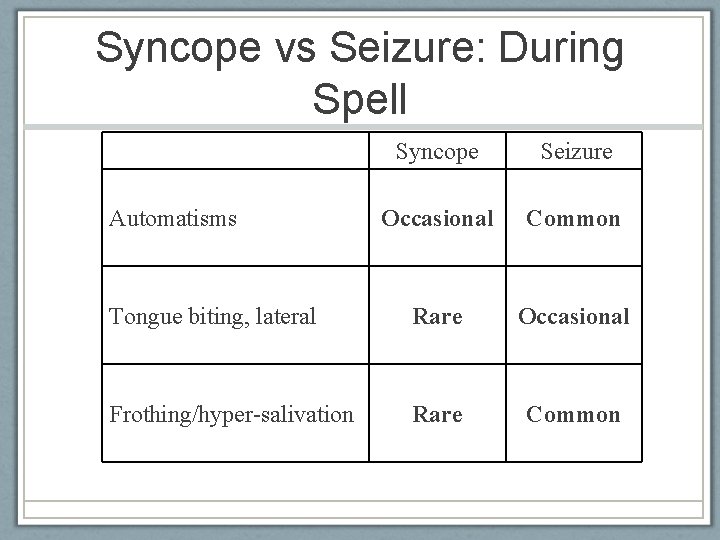
Syncope vs Seizure: During Spell Syncope Seizure Occasional Common Tongue biting, lateral Rare Occasional Frothing/hyper-salivation Rare Common Automatisms American Epilepsy Society 2010
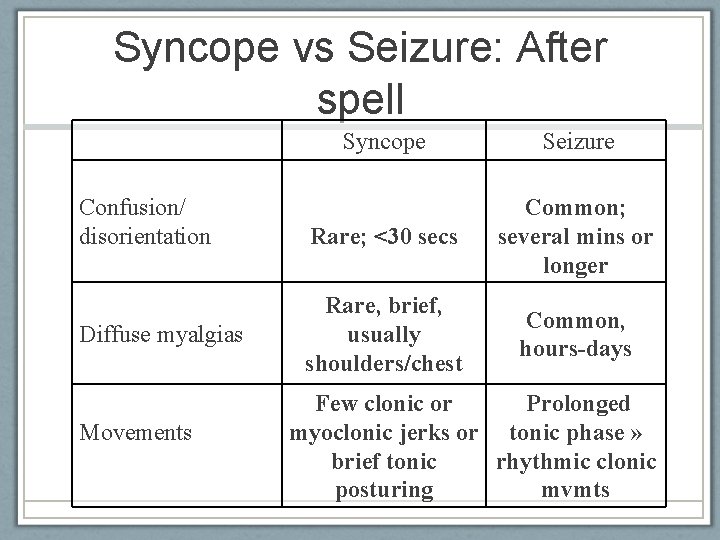
Syncope vs Seizure: After spell Confusion/ disorientation Diffuse myalgias Movements American Epilepsy Society 2010 Syncope Seizure Rare; <30 secs Common; several mins or longer Rare, brief, usually shoulders/chest Common, hours-days Few clonic or Prolonged myoclonic jerks or tonic phase » brief tonic rhythmic clonic posturing mvmts

Driving and Epilepsy Regulation varies • Required seizure-free period Usually one year also after drug withdraw should not drive for at least 6 months For public driving like taxi, bus should be seizure free for 10 yrs American Epilepsy Society 2010

First Aid Tonic-Clonic Seizure After seizure ends, turn person on LT side with face turned toward ground to keep airway clear(recovery position) Transfer to hospital needed for: • Multiple seizures or status epilepticus • Person is pregnant, injured, diabetic • New onset seizures DO NOT put any object in mouth or restrain American Epilepsy Society 2010

Pregnancy and Epilepsy 96% of pregnancies in mothers with epilepsy produce normal children Spontaneous abortions and pre-term birth are more common in women with epilepsy There is an increased rate of fetal malformations associated with antiepileptic drug exposure Seizures during pregnancy may be harmful Tonic-clonic seizures associated with intracranial hemorrhage, fetal bradycardia and lower IQ in children Status epilepticus associated with increased fetal and maternal mortality in some studies American Epilepsy Society 2010

Pregnancy and Epilepsy Guidelines for Management Before pregnancy • Attempt AED monotherapy with lowest effective dose • Consider switching AEDs prior to pregnancy, particularly if on valproate • Establish baseline therapeutic levels • Folate supplementation • 0. 4 – 5 mg/day American Epilepsy Society 2010

• 25 yrs female presented to ER with H/O recurrent seizures without regain consciousness between attacks, pt is unconscious and unresponsive , vitally stable , no signs of trauma and all lab investigation were normal , what to do ? • A. perform urgent CT scan brain • B. put pateint in recovery position • C. urgent EEG monitor • D. give her oral depakene • E. start iv phenytoin American Epilepsy Society 2010
- Slides: 46