Epidemiology and diagnosis of acute pulmonary embolism Dr

Epidemiology and diagnosis of acute pulmonary embolism Dr Sam Z Goldhaber Associate Professor of Medicine Harvard Medical School Staff Cardiologist Brigham and Women’s Hospital Boston, MA
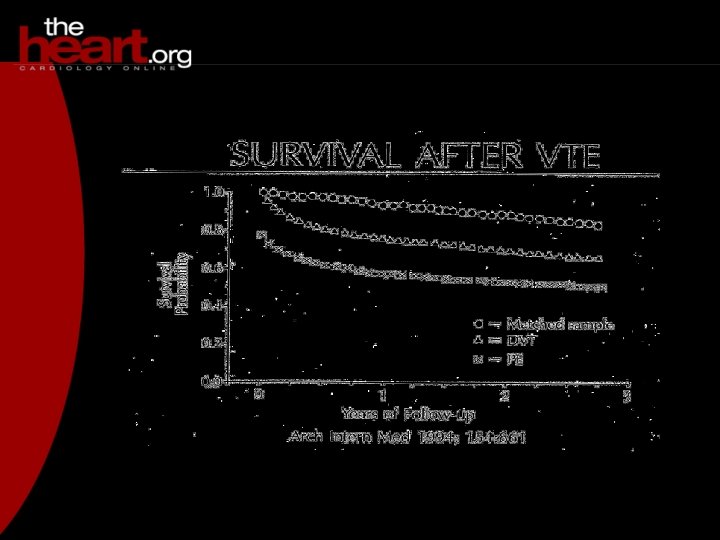
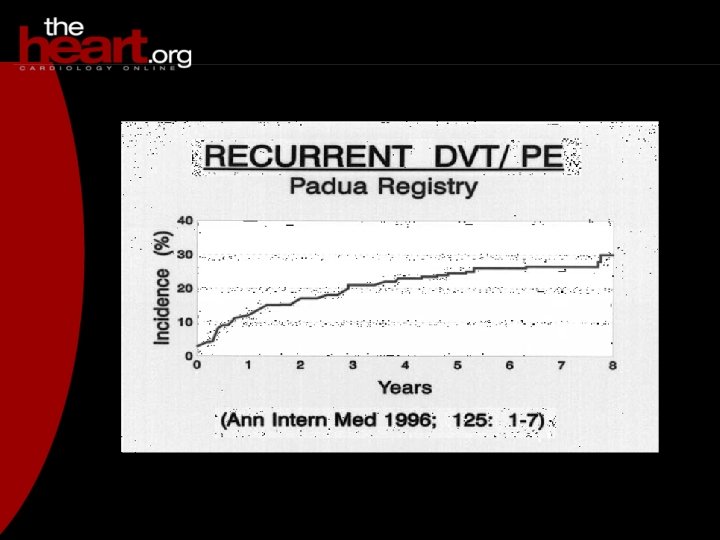

Risk factors for PE Nurses’ Health Study 1) Obesity (RR = 3. 0, with BMI >29) 2) Cigarette smoking (RR = 2. 1, with > 35 cigs/d) 3) Hypertension (RR = 1. 5) JAMA 1997; 277: 642

Hypercoagulability work-up High yield (> 20%) 1) Factor V Leiden – Genetic mutation that causes resistance to activated protein C 2) Plasma homocysteine level – Rx with folate, B 6, B 12 3) Lupus anticoagulant screen – Requires intensive anticoagulation; Possible steroid/ASA responsiveness

Leiden/recurrent VTE after discontinuing warfarin RR = 4. 7 (p = 0. 047) (PHS: Circulation 1995; 92: 2800) RR = 2. 4 (p < 0. 01) (Padua: NEJM 1997; 336: 399) No increased risk (Rintelen: Thromb Haemostas 996; 75: 229)

ACLA and VTE 412 Swedish patients 14% ACLA in men 17% ACLA in women 29% recurrence in ACLA positive vs 14% recurrence in ACLA negative 15% vs 6% 4 -year mortality Am J Med 998; 104: 332

Prothrombin gene mutation 1) risk DVT/PE (Ann Intern Med 1998; 129: 89) 2) risk cerebral vein thrombosis (NEJM 1998; 338: 1793)

Hypercoagulability work-up Low yield 1) antithrombin III deficiency (spurious value on heparin) 2) protein C deficiency (spurious value on warfarin, BCP or when pregnant) 3) protein S deficiency (spurious value on warfarin, BCP or when pregnant)

Signs/Sx PE (n = 131) Observation Dyspnea Chest pain Cyanosis Hemoptysis Syncope Rate 77% 55% 18% 13% 10% Arch Intern Med 1991; 151: 933
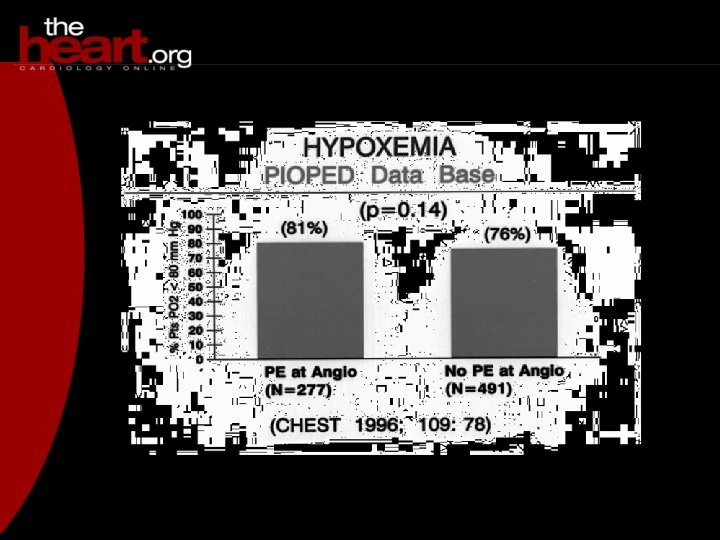
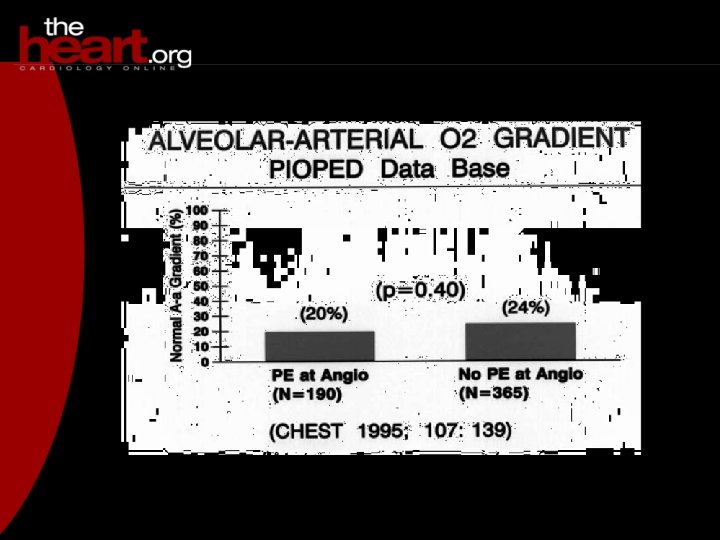
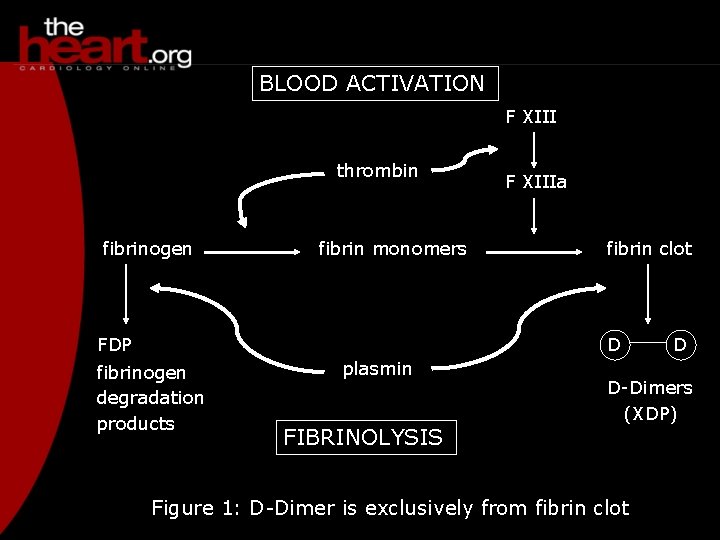
BLOOD ACTIVATION F XIII thrombin fibrinogen fibrin monomers FDP F XIIIa fibrin clot D fibrinogen degradation products plasmin FIBRINOLYSIS D D-Dimers (XDP) Figure 1: D-Dimer is exclusively from fibrin clot

D-Dimer for PE diagnosis Overview of 9 trials (n = 908) ELISA assay; 38% have positive scans/PAgrams Sensitivity 97% Specificity 45% PPV NPV 50% 94% Thromb Haemostas 1994; 71: 1 -6

High probability lung scans are insensitive for PE Scan interpretation Sensitivity (%) Specificity (%) High 41 97 59% of patients with PE have non-high probability scans JAMA 1990; 263: 2753 -9
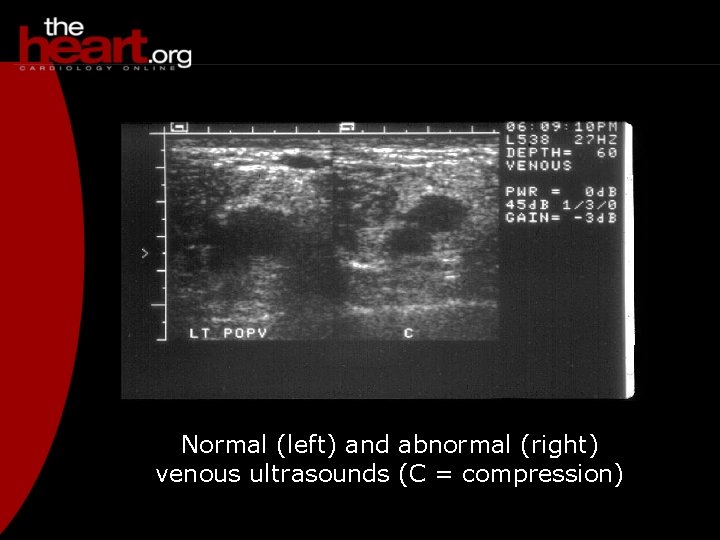
Normal (left) and abnormal (right) venous ultrasounds (C = compression)

Venography for suspected PE Venography Pulmonary angiography Positive Negative Positive 29 11 Negative 12 22 Total 41 33 Hull et al. Ann Intern Med 1983; 98: 891
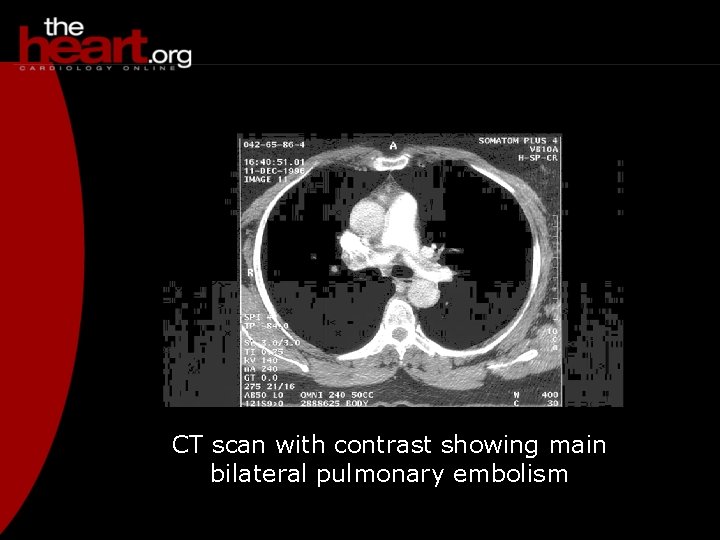
CT scan with contrast showing main bilateral pulmonary embolism
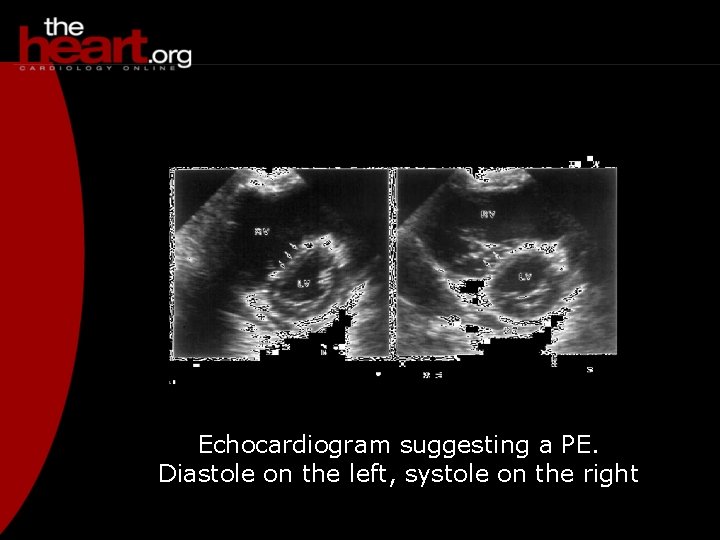
Echocardiogram suggesting a PE. Diastole on the left, systole on the right

PE diagnosis strategy Lung (or CT) scan High probability Intermediate Normal TREAT or low probability STOP W/U High D-dimer Normal D-dimer CONTINUE W/U STOP W/U If leg U/S normal If Echo normal PAgram (or CT)
- Slides: 20