Epidemiology and burden Parkinsons disease 1 Prevalence of

Epidemiology and burden Parkinson’s disease 1

Prevalence of Parkinson’s disease 2
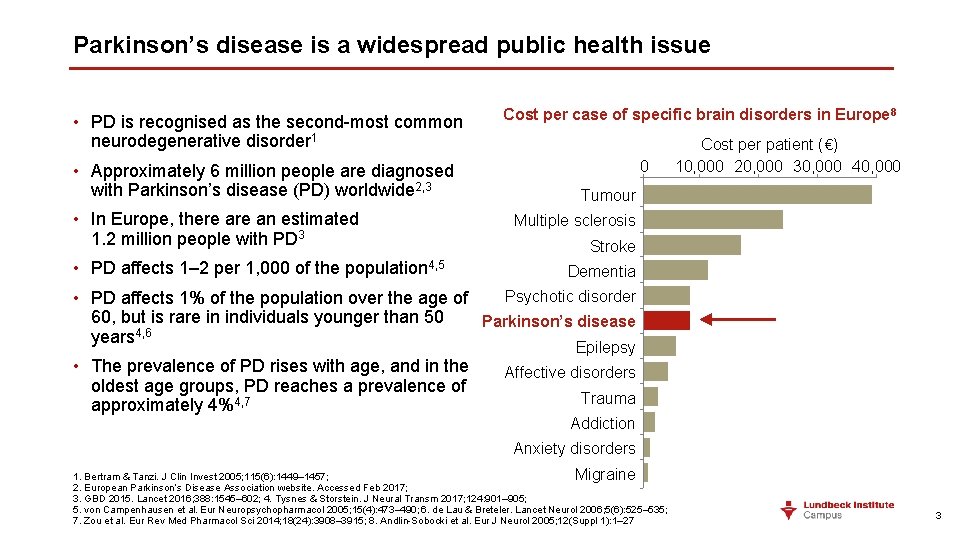
Parkinson’s disease is a widespread public health issue • PD is recognised as the second-most common neurodegenerative disorder 1 • Approximately 6 million people are diagnosed with Parkinson’s disease (PD) worldwide 2, 3 • In Europe, there an estimated 1. 2 million people with PD 3 • PD affects 1– 2 per 1, 000 of the population 4, 5 Cost per case of specific brain disorders in Europe 8 0 Cost per patient (€) 10, 000 20, 000 30, 000 40, 000 Tumour Multiple sclerosis Stroke Dementia Psychotic disorder • PD affects 1% of the population over the age of 60, but is rare in individuals younger than 50 Parkinson’s disease 4, 6 years • The prevalence of PD rises with age, and in the oldest age groups, PD reaches a prevalence of approximately 4%4, 7 Epilepsy Affective disorders Trauma Addiction Anxiety disorders Migraine 1. Bertram & Tanzi. J Clin Invest 2005; 115(6): 1449– 1457; 2. European Parkinson’s Disease Association website. Accessed Feb 2017; 3. GBD 2015. Lancet 2016; 388: 1545– 602; 4. Tysnes & Storstein. J Neural Transm 2017; 124: 901– 905; 5. von Campenhausen et al. Eur Neuropsychopharmacol 2005; 15(4): 473– 490; 6. de Lau & Breteler. Lancet Neurol 2006; 5(6): 525– 535; 7. Zou et al. Eur Rev Med Pharmacol Sci 2014; 18(24): 3908– 3915; 8. Andlin-Sobocki et al. Eur J Neurol 2005; 12(Suppl 1): 1– 27 3

Prevalence of Parkinson’s disease in the USA • Prevalence describes the number of people with a given condition at a given time (often expressed per 100, 000 people)1 • Estimates vary, but there approximately 1 million people in the USA living with PD 2 • Incidence rates describe the number of new cases of a given condition arising over a given time, usually per year, often expressed per 100, 000 people 1 • The incidence rate in the USA has been approximated to be 13. 4 per 100, 0003 • This rate rises rapidly over the age of 60 years 3 1. Oxford Concise Medical Dictionary. 2007; 2. Michael J. Fox foundation website. Accessed Feb 2017; 3. Van Den Eeden et al. Am J Epidemiol 2003; 157(11): 1015– 1022 4

Prevalence of Parkinson’s disease in Europe • A meta-analysisa comparing studies • This meta-analysis identified estimating the prevalence of PD in several problems which may give various European countries gave rise to the variation in estimates: 1 prevalence rates of 108– 257 per • Differences in methodology 100, 000 people 1 • Differences in diagnostic criteria • Differences in the type and design of • When considering only older the surveys people (>60 years old) this rate • Variations in age categories (i. e. , some increased to 1, 280– 1, 500 per surveys stop at >75 years whereas 1 100, 000 people some stop at >90 years old) The prevalence of PD is difficult to measure; however, the disease is more commonly found in older individuals a. A meta-analysis is a study using data from several other studies 1. von Campenhausen et al. Eur Neuropsychopharmacol 2015; 15: 473– 490 5
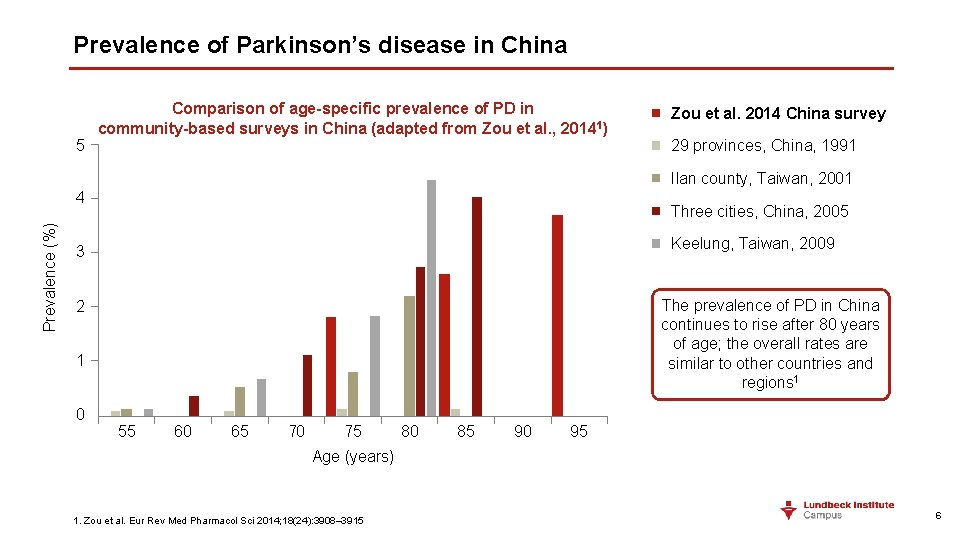
Prevalence of Parkinson’s disease in China 5 Comparison of age-specific prevalence of PD in community-based surveys in China (adapted from Zou et al. , 20141) Zou et al. 2014 China survey 29 provinces, China, 1991 Ilan county, Taiwan, 2001 Prevalence (%) 4 Three cities, China, 2005 Keelung, Taiwan, 2009 3 The prevalence of PD in China continues to rise after 80 years of age; the overall rates are similar to other countries and regions 1 2 1 0 55 60 65 70 75 80 85 90 95 Age (years) 1. Zou et al. Eur Rev Med Pharmacol Sci 2014; 18(24): 3908– 3915 6
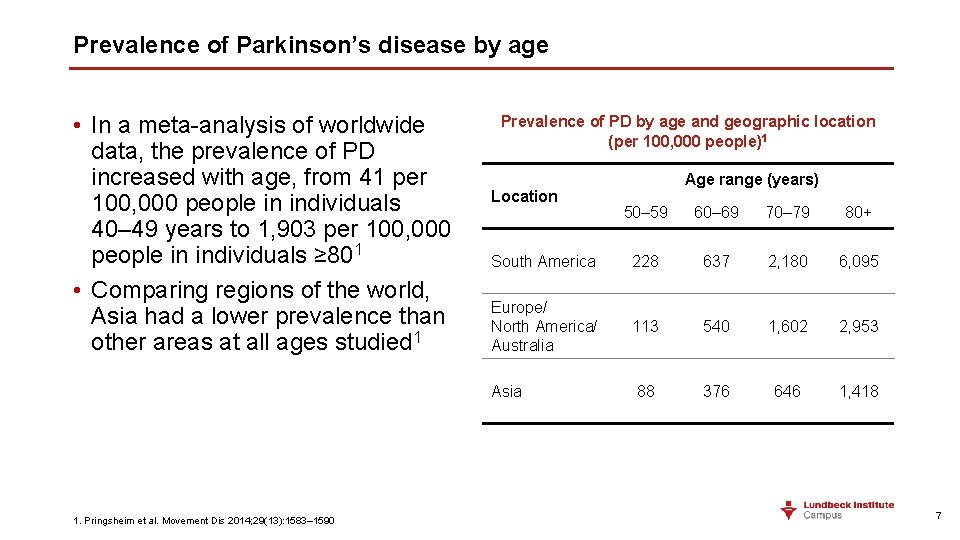
Prevalence of Parkinson’s disease by age • In a meta-analysis of worldwide data, the prevalence of PD increased with age, from 41 per 100, 000 people in individuals 40– 49 years to 1, 903 per 100, 000 people in individuals ≥ 801 • Comparing regions of the world, Asia had a lower prevalence than other areas at all ages studied 1 1. Pringsheim et al. Movement Dis 2014; 29(13): 1583– 1590 Prevalence of PD by age and geographic location (per 100, 000 people)1 Location Age range (years) 50– 59 60– 69 70– 79 80+ South America 228 637 2, 180 6, 095 Europe/ North America/ Australia 113 540 1, 602 2, 953 Asia 88 376 646 1, 418 7
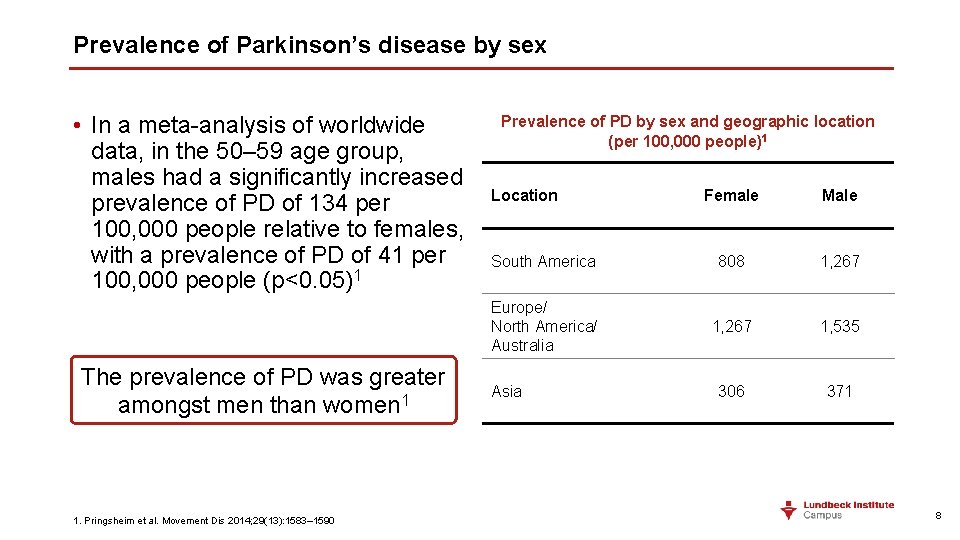
Prevalence of Parkinson’s disease by sex • In a meta-analysis of worldwide data, in the 50– 59 age group, males had a significantly increased prevalence of PD of 134 per 100, 000 people relative to females, with a prevalence of PD of 41 per 100, 000 people (p<0. 05)1 The prevalence of PD was greater amongst men than women 1 1. Pringsheim et al. Movement Dis 2014; 29(13): 1583– 1590 Prevalence of PD by sex and geographic location (per 100, 000 people)1 Location Female Male South America 808 1, 267 Europe/ North America/ Australia 1, 267 1, 535 306 371 Asia 8
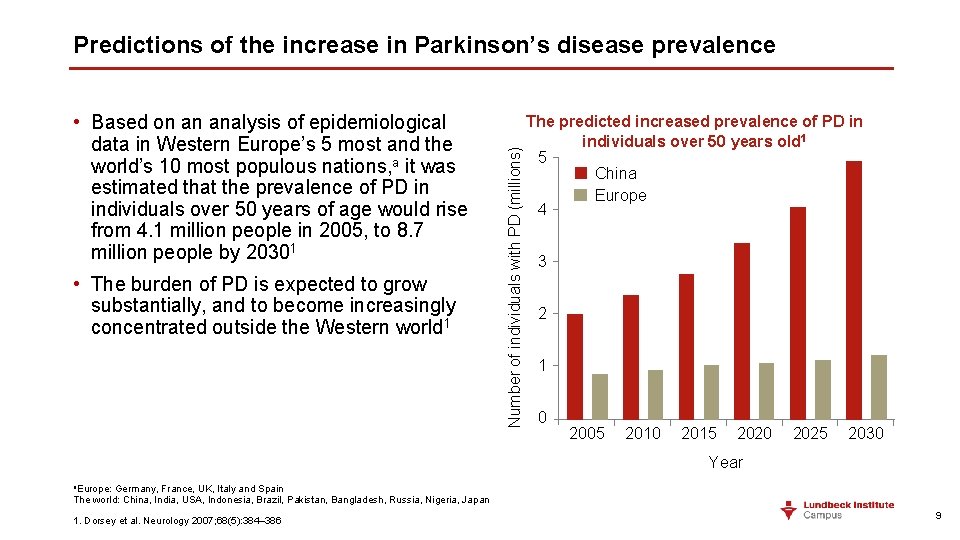
• Based on an analysis of epidemiological data in Western Europe’s 5 most and the world’s 10 most populous nations, a it was estimated that the prevalence of PD in individuals over 50 years of age would rise from 4. 1 million people in 2005, to 8. 7 million people by 20301 • The burden of PD is expected to grow substantially, and to become increasingly concentrated outside the Western world 1 Number of individuals with PD (millions) Predictions of the increase in Parkinson’s disease prevalence The predicted increased prevalence of PD in individuals over 50 years old 1 5 China Europe 4 3 2 1 0 2005 2010 2015 2020 2025 2030 Year a. Europe: Germany, France, UK, Italy and Spain The world: China, India, USA, Indonesia, Brazil, Pakistan, Bangladesh, Russia, Nigeria, Japan 1. Dorsey et al. Neurology 2007; 68(5): 384– 386 9

Risk factors associated with Parkinson’s disease Risk factors 1, 2 • • Age Sex Genetics Pesticide exposure Dairy Melanoma Traumatic brain injury • • • Protective factors 1, 2 Smoking/tobacco use Caffeine Urate Physical activity NSAIDsa Calcium channel blockers The risk of developing PD is a balance of the effect of positive and negative factors on the genetic predisposition of an individual 2 a. Strongest evidence for ibuprofen, for other NSAIDs the evidence is mixed or poor; 1, 2 NSAID=nonsteroidal anti-inflammatory drug 1. Lee & Gilbert. Neurol Clin 2016; 34(4): 955– 965; 2. Ascherio & Schwarzschild. Lancet Neurol 2016; 15(12): 1257– 1272 10

The burden of Parkinson’s disease 11
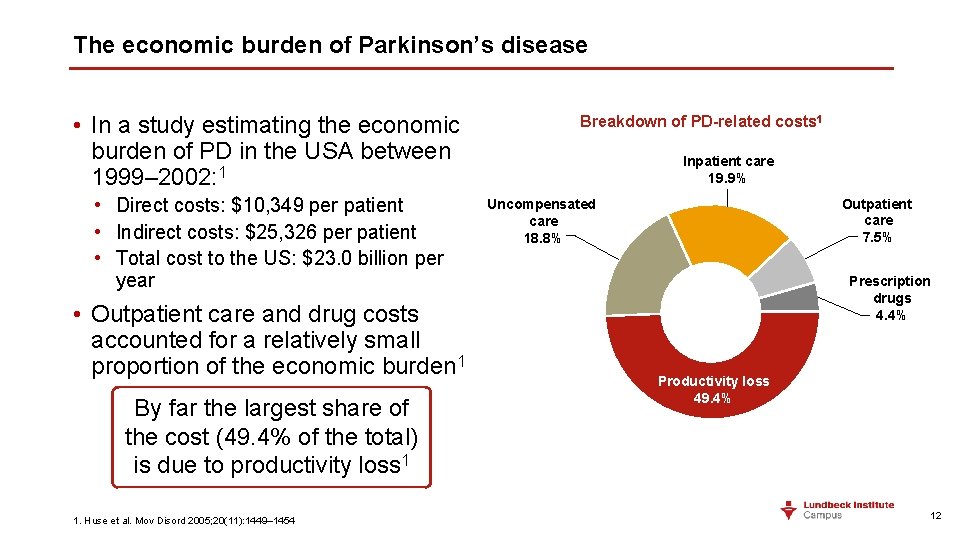
The economic burden of Parkinson’s disease • In a study estimating the economic burden of PD in the USA between 1999– 2002: 1 • Direct costs: $10, 349 per patient • Indirect costs: $25, 326 per patient • Total cost to the US: $23. 0 billion per year • Outpatient care and drug costs accounted for a relatively small proportion of the economic burden 1 By far the largest share of the cost (49. 4% of the total) is due to productivity loss 1 1. Huse et al. Mov Disord 2005; 20(11): 1449– 1454 Breakdown of PD-related costs 1 Inpatient care 19. 9% Outpatient care 7. 5% Uncompensated care 18. 8% Prescription drugs 4. 4% Productivity loss 49. 4% 12

The indirect costs of Parkinson’s disease • Indirect costs are the expenses incurred from the cessation or reduction of work productivity as a result of the morbidity and mortality associated with a given disease 1 • Indirect costs include: 1, 2 • • a. Excess Work loss Worker loss and replacement Lost/reduced productivity Absenteeism (habitual absence from work) • In one analysis within the USA, the indirect costs of PD represented 45% of the total excess costsa within the first year after diagnosis 2 • In several studies analysing the costs of PD, the indirect costs were greater than the direct costs 3 -5 costs defined as costs incurred by patients with PD minus the total incurred by a control population 1. Boccuzzi. In: Cardiovascular Health Care Economics. 2003; 2. Johnson et al. Pharmacoeconomics 2013; 31(9): 779– 806; 3. Martinez-Martín et al. PLo. S One 2015; 10(12): e 0145310; 4. Huse et al. Mov Disord 2005; 20: 1449– 1454; 5. Boland & Stacy. Am J Manag Care 2012; 18(7 Suppl): S 168– 175 13
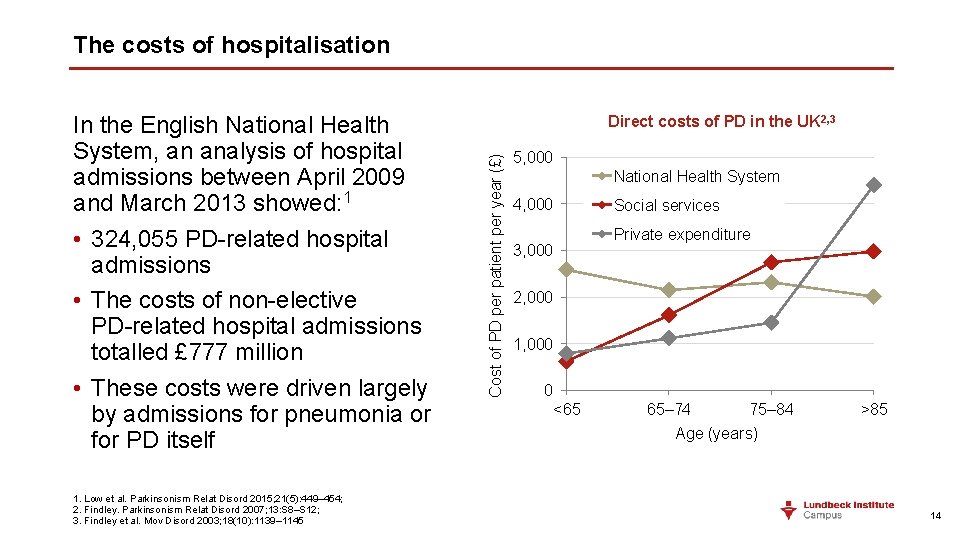
The costs of hospitalisation 1. Low et al. Parkinsonism Relat Disord 2015; 21(5): 449– 454; 2. Findley. Parkinsonism Relat Disord 2007; 13: S 8–S 12; 3. Findley et al. Mov Disord 2003; 18(10): 1139– 1145 Direct costs of PD in the UK 2, 3 Cost of PD per patient per year (£) In the English National Health System, an analysis of hospital admissions between April 2009 and March 2013 showed: 1 • 324, 055 PD-related hospital admissions • The costs of non-elective PD-related hospital admissions totalled £ 777 million • These costs were driven largely by admissions for pneumonia or for PD itself 5, 000 National Health System 4, 000 3, 000 Social services Private expenditure 2, 000 1, 000 0 <65 65– 74 75– 84 Age (years) >85 14
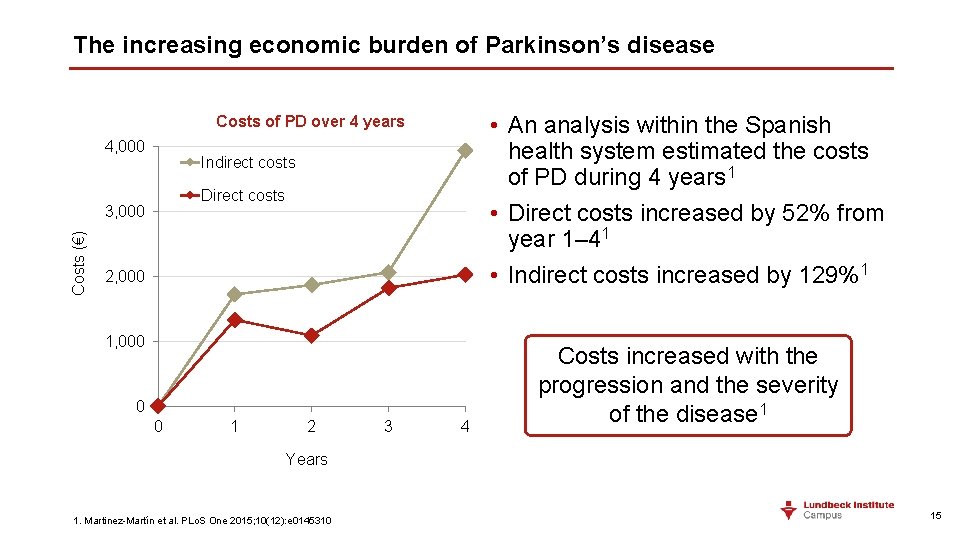
The increasing economic burden of Parkinson’s disease • An analysis within the Spanish health system estimated the costs of PD during 4 years 1 • Direct costs increased by 52% from year 1– 41 • Indirect costs increased by 129%1 Costs of PD over 4 years 4, 000 Indirect costs Direct costs Costs (€) 3, 000 2, 000 1, 000 0 0 1 2 3 4 Costs increased with the progression and the severity of the disease 1 Years 1. Martinez-Martín et al. PLo. S One 2015; 10(12): e 0145310 15
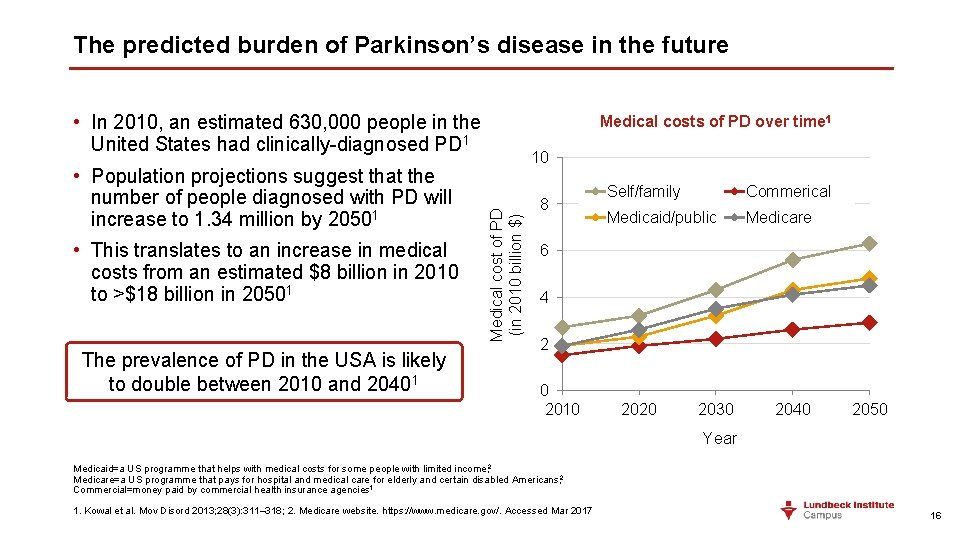
The predicted burden of Parkinson’s disease in the future • In 2010, an estimated 630, 000 people in the United States had clinically-diagnosed PD 1 • This translates to an increase in medical costs from an estimated $8 billion in 2010 to >$18 billion in 20501 The prevalence of PD in the USA is likely to double between 2010 and 20401 10 Medical cost of PD (in 2010 billion $) • Population projections suggest that the number of people diagnosed with PD will increase to 1. 34 million by 20501 Medical costs of PD over time 1 8 Self/family Commerical Medicaid/public Medicare 6 4 2 0 2010 2020 2030 2040 2050 Year Medicaid=a US programme that helps with medical costs for some people with limited income; 2 Medicare=a US programme that pays for hospital and medical care for elderly and certain disabled Americans; 2 Commercial=money paid by commercial health insurance agencies 1 1. Kowal et al. Mov Disord 2013; 28(3): 311– 318; 2. Medicare website. https: //www. medicare. gov/. Accessed Mar 2017 16

The burden of Parkinson’s disease on the patient • PD has a substantial impact on quality of life, driven by: • Motor symptoms 1 • Non-motor symptoms such as depression – roughly half of patients with PD suffer from some form of depression, but this is typically under-treated 1, 2 • Treatment-related side effects and complications – e. g. , psychosis, excessive daytime somnolence, impulse control disorders, dyskinesia, and motor fluctuations 3, 4 • In studies of US veterans: • Health-related quality of life scores among patients with PD were found to be lower than for all other diseases studieda – except spinal cord injury and depression 2 • Scores on the UPDRS (Unified Parkinson’s Disease Rating Scale; a scale which measures the severity of PD) correlated with quality of life indices 5 a. Including congestive heart failure, stroke, chronic low back pain, arthritis, diabetes, and angina/coronary heart disease 1. Boland & Stacy. Am J Manag Care 2012; 18(7 Suppl): S 168– 175; 2. Gage et al. J Neurol Neurosurg Psychiatry 2003; 74(2): 163– 169; 3. Jankovic & Aguilar. Neuropsychiatr Dis Treat 2008; 4(4): 743– 757; 4. Chapuis et al. Mov Disord 2005; 20(2): 224– 230; 5. Kleiner-Fisman et al. Health Qual Life Outcomes 2010; 8: 91 17
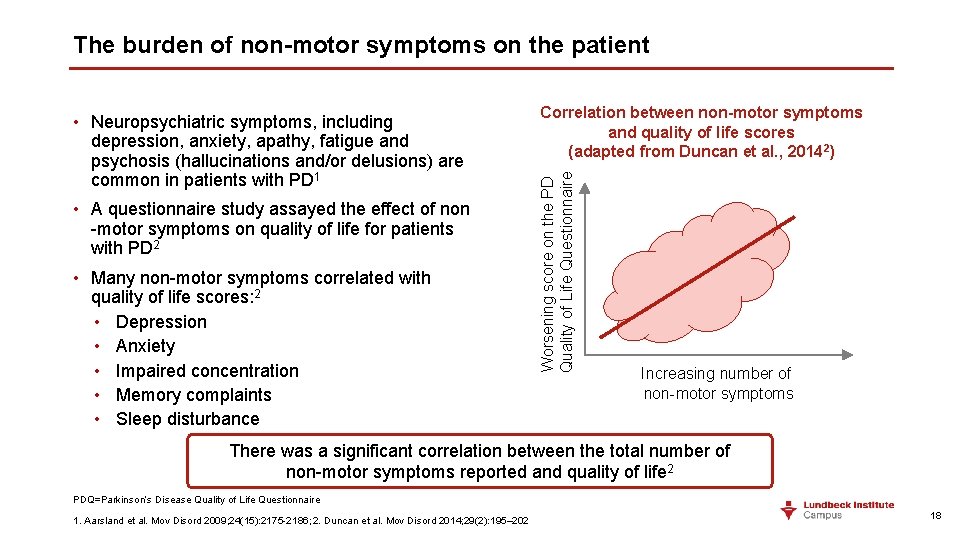
The burden of non-motor symptoms on the patient • A questionnaire study assayed the effect of non -motor symptoms on quality of life for patients with PD 2 • Many non-motor symptoms correlated with quality of life scores: 2 • Depression • Anxiety • Impaired concentration • Memory complaints • Sleep disturbance Correlation between non-motor symptoms and quality of life scores (adapted from Duncan et al. , 20142) Worsening score on the PD Quality of Life Questionnaire • Neuropsychiatric symptoms, including depression, anxiety, apathy, fatigue and psychosis (hallucinations and/or delusions) are common in patients with PD 1 Increasing number of non-motor symptoms There was a significant correlation between the total number of non-motor symptoms reported and quality of life 2 PDQ=Parkinson’s Disease Quality of Life Questionnaire 1. Aarsland et al. Mov Disord 2009; 24(15): 2175 -2186; 2. Duncan et al. Mov Disord 2014; 29(2): 195– 202 18
The burden of Parkinson’s disease on caregivers • Caregivers of patients with PD are almost always relatives, and are often elderly 1 • Caring for a patient with PD places a considerable burden on the caregiver 1 • Caregiver burdens include: 2 • • Health problems Modification of habits Economic loss Deterioration of quality of life 1. Peters. Focus on PD 2014; 24(1): 44– 48; 2. Martinez-Martin et al. Expert Rev Pharmacoecon Outcomes Res 2012; 12(2): 221– 230; 3. Aarsland et al. J Neurol Neurosurg Psychiatry 2007; 78(1): 36– 42 Patient-related variables that impact on the caregiver: 1 • Disability • Motor symptoms • PD symptoms • Medical comorbidities • Disease duration • Neuropsychiatric • Higher medical symptoms costs (including cognitive • Gait impairment, • Use of psychosis, apathy, antidepressants depression, and • Postural instability impulse control and falls disorders)3 • Quality of life 19

The burden of the cognitive symptoms of Parkinson’s disease on caregivers • The level of cognitive functioning of patients can pose particular challenges to the caregivers of patients with PD 1 • One study showed that individuals who are more cognitively impaired place a greater burden on caregivers: 1 • The poorest quality of life was reported by caregivers of patients with PD dementia • Impairments to a patient’s attention, memory, and executive function (e. g. , the ability to plan and solve problems) showed a strong relationship with caregiver burden • Attentional deficits were the strongest predictor of caregiver quality of life compared with other cognitive factors • Loss of attention in patients with PD may lead to increased caregiver responsibilities (to compensate for the attentional deficit), leading to reduced quality of life of the caregiver 1. Lawson et al. Int J Geriatr Psychiatry 2017; 32(12): 1362 -1370 20

“ Parkinson’s disease is a disease with growing prevalence and negative effects on quality of life Boland & Stacy. Am J Manag Care 2012; 18(7 Suppl): S 168– 175 21
- Slides: 21