Epidemiologic transition global burden of disease and emergence

Epidemiologic transition, global burden of disease, and emergence of NCDs Pascal Bovet, MD, MPH University Institute of Social and Preventive Medicine (IUMSP), Lausanne Consultant for NCD, Ministry of Health, Seychelles 7 th WHO-IUMSP International Seminar on the Public Health Aspects of NCDs Lausanne-Geneva, 3 -7 June 2013

Outline • The health transition • The driving engines: • Demographic transition • Epidemiological transition • Global burden • Trends of diseases • Fraction of the burden attributable to avoidable risk factors • Conclusions

Objectives • Describe the principles and different stages of the epidemiological transition • Describe the principles and main overall results of global burden of disease project What the participant will have achieved as a result of participating in the session • Be able to articulate the epidemiological and demographic engines driving the epidemiological transition • Be able to articulate the magnitude of the burden of disease according to time, regions, broad disease categories and main risk factors

The epidemiologic transition (health transition) • Described in the 1970 s (Omran, later Olshansky, Ault) – Relationship between socioeconomic development and health – Shift from communicable diseases and nutritional deficiencies to NCDs – Classification of 4 stages to relate socioeconomic and disease patterns • Provides a framework to understanding current and future health patterns and needs – Relevance for LICs experiencing early stages of health transition – Model for health planning, particularly where available data are scarce Omran AR. The epidemiologic transition: a key of the epidemiology of population change. Milbank Mem Fund Q 1971; 49: 509 -538 Olshansky & Ault. The fourth stage of epidemiologic transition: the age of delayed degenerative diseases. Milbank Mem Fund Q 1986; 64: 355 -91
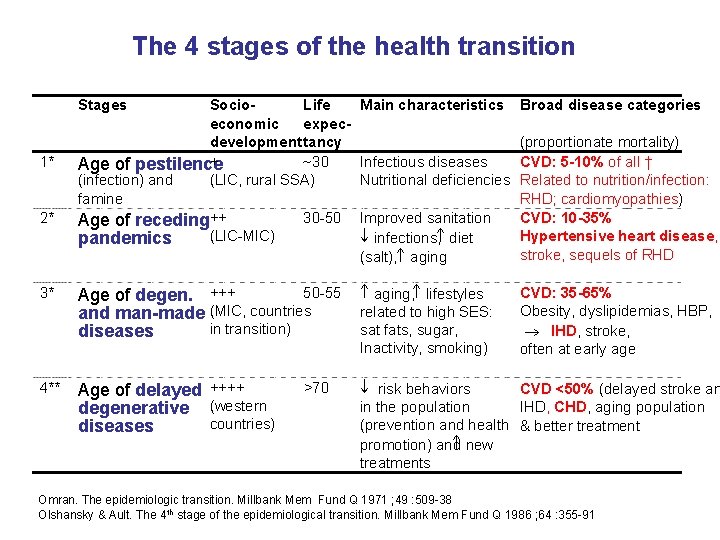
The 4 stages of the health transition Stages 1* 2* Socio. Life economic expecdevelopment tancy ~30 + Age of pestilence (LIC, rural SSA) (infection) and famine 30 -50 Age of receding++ (LIC-MIC) pandemics Main characteristics Broad disease categories (proportionate mortality) Infectious diseases CVD: 5 -10% of all † Nutritional deficiencies Related to nutrition/infection: RHD; cardiomyopathies) Improved sanitation : CVD: 10 -35% Hypertensive heart disease, infections, diet stroke, sequels of RHD (salt), aging 3* 50 -55 Age of degen. +++ and man-made (MIC, countries in transition) diseases aging, lifestyles related to high SES: sat fats, sugar, Inactivity, smoking) 4** Age of delayed ++++ degenerative (western countries) diseases risk behaviors CVD <50% (delayed stroke an IHD, CHD, aging population in the population (prevention and health & better treatment new promotion) and treatments >70 CVD: 35 -65% Obesity, dyslipidemias, HBP, ® IHD, stroke, often at early age Omran. The epidemiologic transition. Millbank Mem Fund Q 1971 ; 49 : 509 -38 Olshansky & Ault. The 4 th stage of the epidemiological transition. Millbank Mem Fund Q 1986 ; 64 : 355 -91
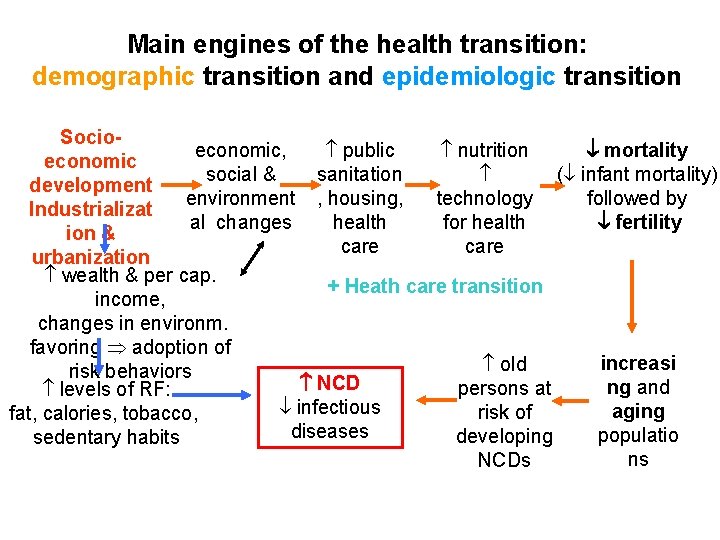
Main engines of the health transition: demographic transition and epidemiologic transition Socioeconomic, public nutrition mortality economic social & sanitation ( infant mortality) development environment , housing, technology followed by Industrializat al changes health for health fertility ion & care urbanization wealth & per cap. + Heath care transition income, changes in environm. favoring adoption of increasi old risk behaviors NCD ng and persons at levels of RF: infectious aging risk of fat, calories, tobacco, diseases populatio developing sedentary habits ns NCDs
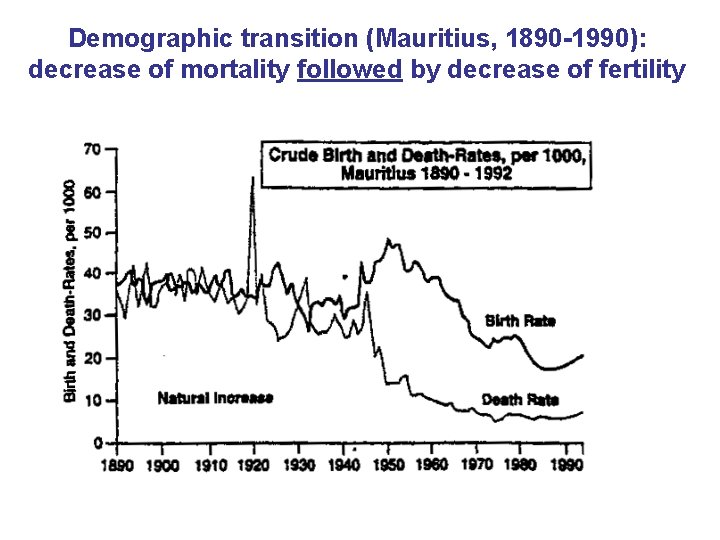
Demographic transition (Mauritius, 1890 -1990): decrease of mortality followed by decrease of fertility
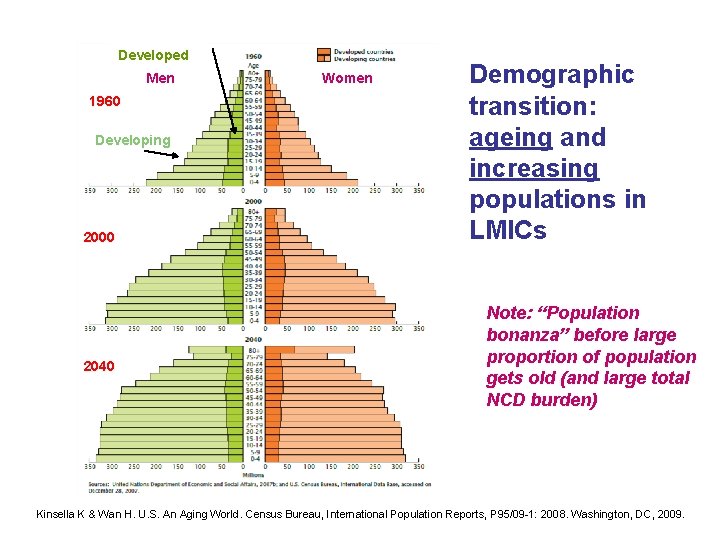
Developed Men 1960 Developing 2000 2040 Women Demographic transition: ageing and increasing populations in LMICs Note: “Population bonanza” before large proportion of population gets old (and large total NCD burden) Kinsella K & Wan H. U. S. An Aging World. Census Bureau, International Population Reports, P 95/09 -1: 2008. Washington, DC, 2009.

Changing socio-economic structures underlie large changes in behaviors (nutrition transition) • Shift from a preindustrial agrarian economy to industrialization – Less active physical activity for individuals – Higher availability of cheap processed foods (high fat, high carb. ) – More varied foods available to all • Profound changes in household technology (leads to less PA) – Food availability: canning, refrigeration, freezing, radiation, packaging – Food preparation: fossil fuels, electricity, appliances (cooker, mixers) – More varied foods at home • Dramatic shift in leisure activities for adults and children – Time spent for viewing television (sedentary habits) – Images/marketing brought to each household (alters consumption) – More time for leisure PA Adapted from Popkin B. The nutrition transition and obesity in the developing world. Nutr J 1991; 131: 871 -73

Globalization favors lifestyle transition (good and bad changes) • Trade liberalization (of world markets) and urbanization – Nutrition transition: fats, sugar (‘coca-colanisation’), ↓ complex carbohydrates – Supply larger than demand fuels competition & promotion (large portions, “all you can eat”, etc), reduces cost of $/calorie (fats, sugars): favors consumption – tobacco – But also allows for more varied foods (5 th stage of health transition) • Information & communication technologies – Global advertising & promotion of unhealthy lifestyles – But also allows promotion of potentially healthy behaviors • Urbanization and accelerated migration of populations – Acculturation facilitates adoption of unhealthy lifestyles – But increased incomes allow for potentially healthy activities

From traditional to modern food marketing. .

From ancient to modern work ….

From traditional to modern transportation. .
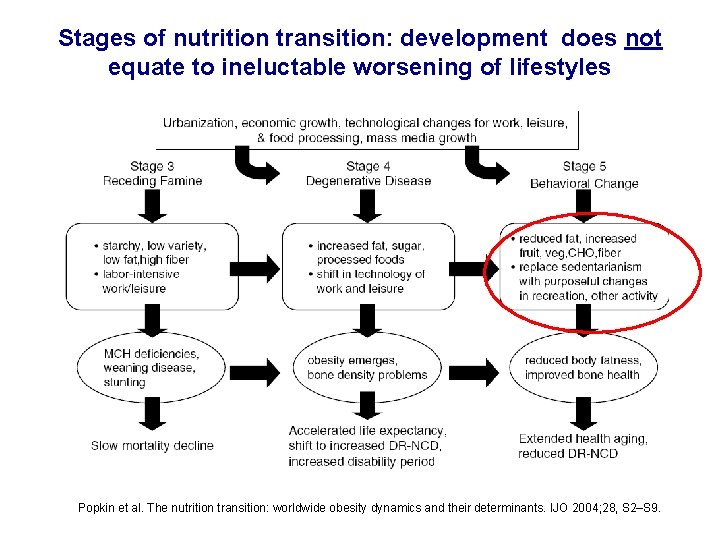
Stages of nutrition transition: development does not equate to ineluctable worsening of lifestyles Popkin et al. The nutrition transition: worldwide obesity dynamics and their determinants. IJO 2004; 28, S 2–S 9.
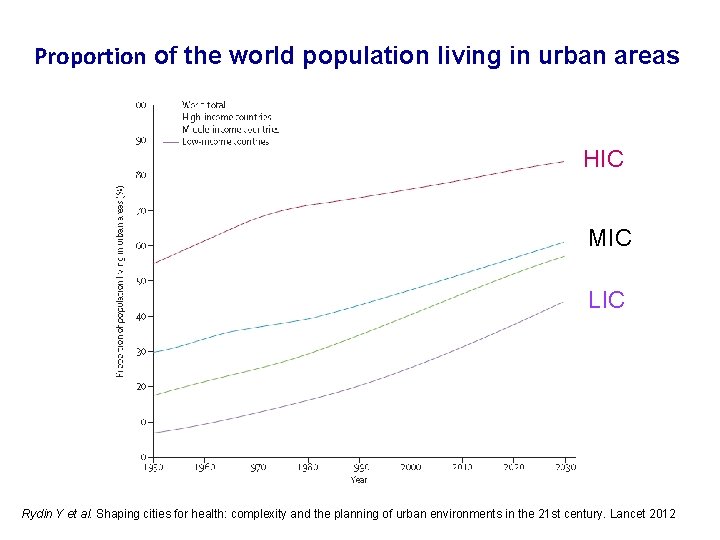
Proportion of the world population living in urban areas HIC MIC LIC Rydin Y et al. Shaping cities for health: complexity and the planning of urban environments in the 21 st century. Lancet 2012
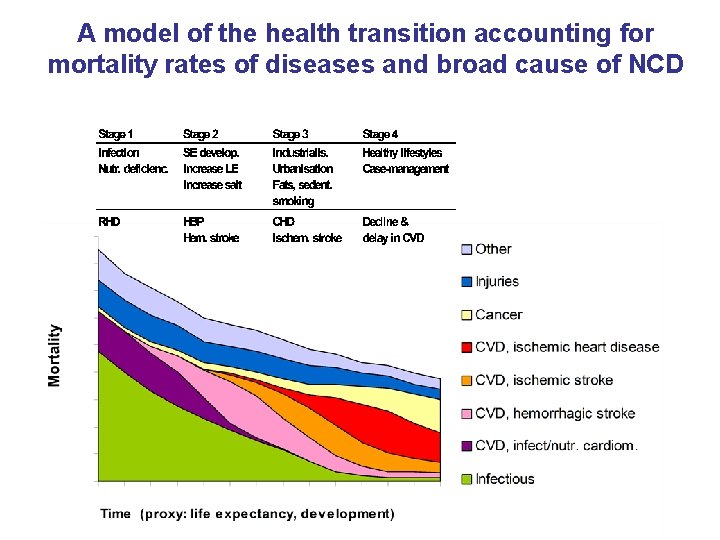
A model of the health transition accounting for mortality rates of diseases and broad cause of NCD
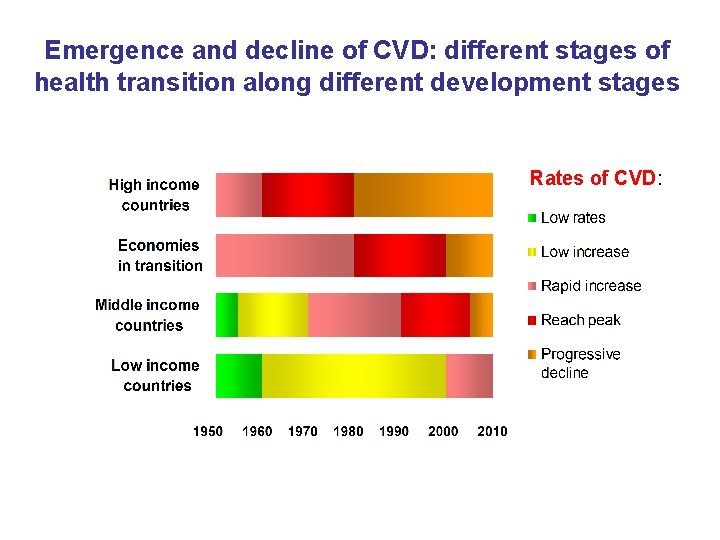
Emergence and decline of CVD: different stages of health transition along different development stages Rates of CVD:
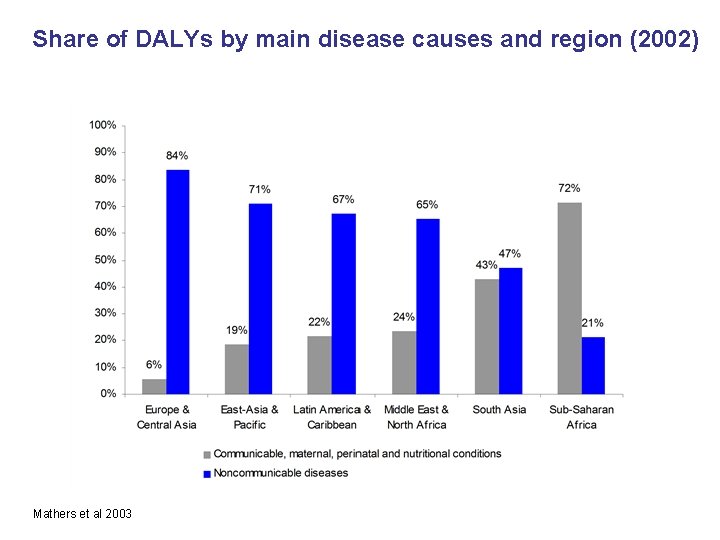
Share of DALYs by main disease causes and region (2002) Mathers et al 2003
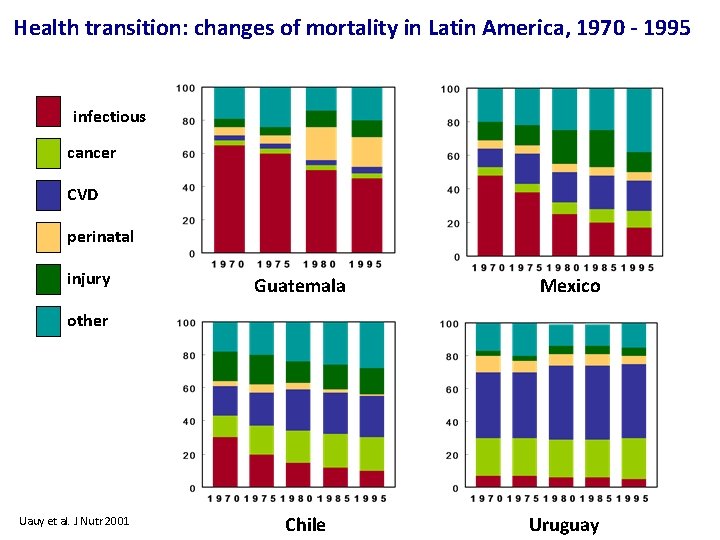
Health transition: changes of mortality in Latin America, 1970 - 1995 infectious cancer CVD perinatal injury Guatemala Mexico other Uauy et al. J Nutr 2001 Chile Uruguay
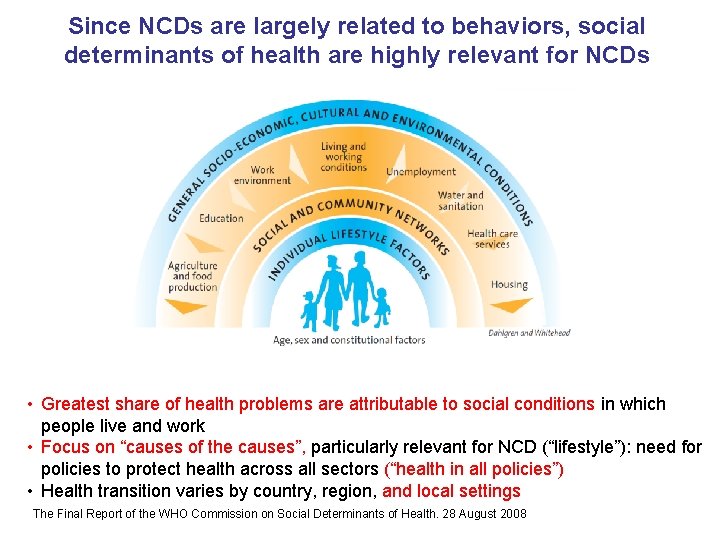
Since NCDs are largely related to behaviors, social determinants of health are highly relevant for NCDs • Greatest share of health problems are attributable to social conditions in which people live and work • Focus on “causes of the causes”, particularly relevant for NCD (“lifestyle”): need for policies to protect health across all sectors (“health in all policies”) • Health transition varies by country, region, and local settings The Final Report of the WHO Commission on Social Determinants of Health. 28 August 2008

A tale of two cities It is not urbanization itself, it is the kind of urbanization and/or city

What is global burden of diseases (GBD)? • Started as collaboration between WHO, WB and Harvard in the 1980 s • A standardized framework integrating all available epidemiological information on morbidity and mortality • All morbidity and mortality estimates are made internally consistent (e. g. all deaths add to 100%) using condition-specific epidemiology • Provides a quantitative assessment of the distribution of both diseases and their risk factors in populations • Common single metric to quantify health status (DALY) Comparable estimates across causes Consistent measure for use with intervention analyses • Allows to assess to which extent disease and risk for diseases could be avoided in different populations/regions
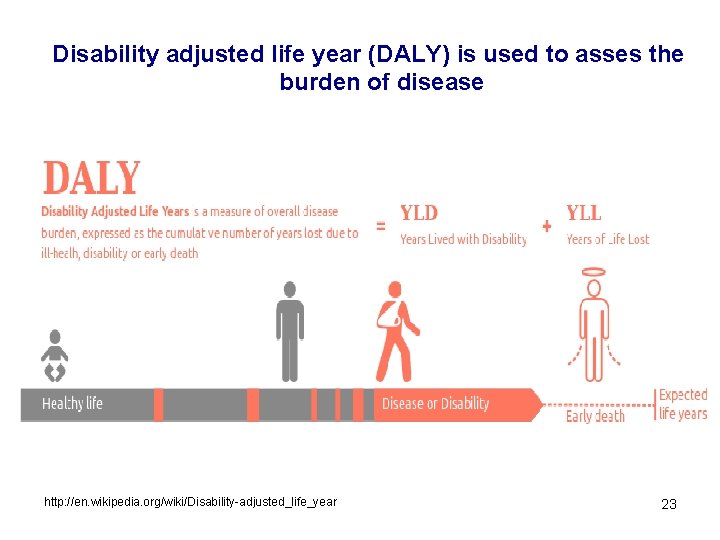
Disability adjusted life year (DALY) is used to asses the burden of disease http: //en. wikipedia. org/wiki/Disability-adjusted_life_year 23
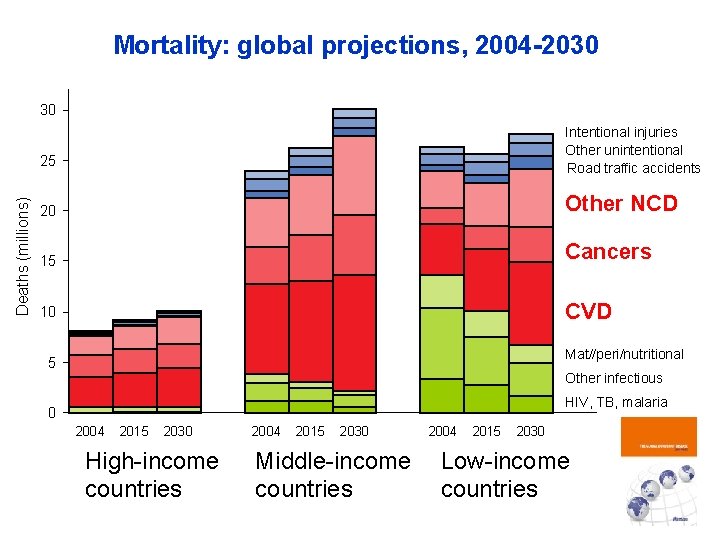
Mortality: global projections, 2004 -2030 30 Intentional injuries Other unintentional Road traffic accidents Deaths (millions) 25 20 Other NCD 15 Cancers 10 CVD Mat//peri/nutritional 5 Other infectious HIV, TB, malaria 0 2004 2015 2030 High-income countries 2004 2015 2030 Middle-income countries 2004 2015 2030 Low-income countries
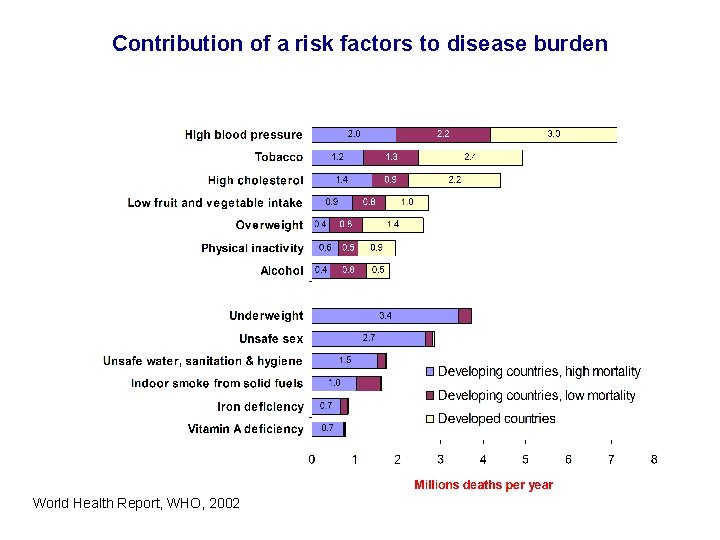
Contribution of a risk factors to disease burden World Health Report, WHO, 2002

Burden of diseases: web site of the Institute for Health Metrics and Evaluation (IHME) www. healthmetricsandevaluation. org/gbd
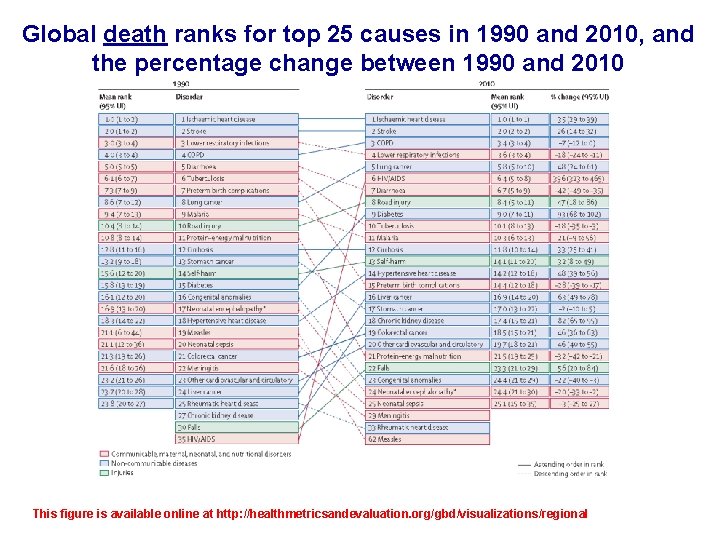

Global death ranks for top 25 causes in 1990 and 2010, and the percentage change between 1990 and 2010 This figure is available online at http: //healthmetricsandevaluation. org/gbd/visualizations/regional
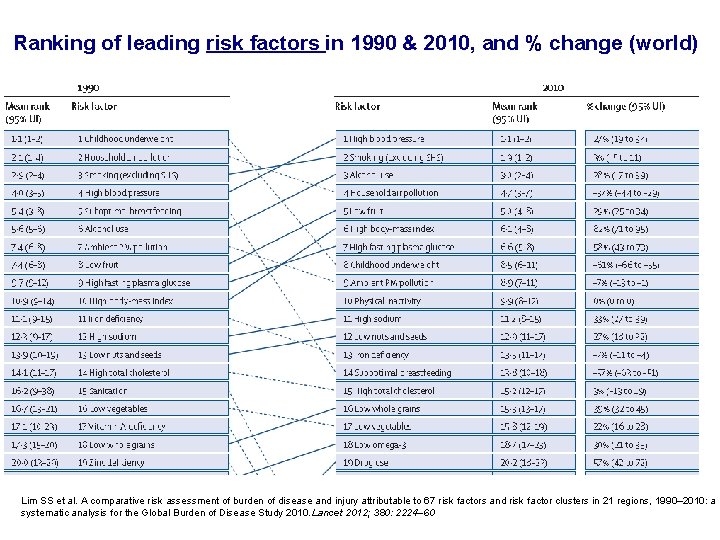
Ranking of leading risk factors in 1990 & 2010, and % change (world) Lim SS et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990– 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380: 2224– 60
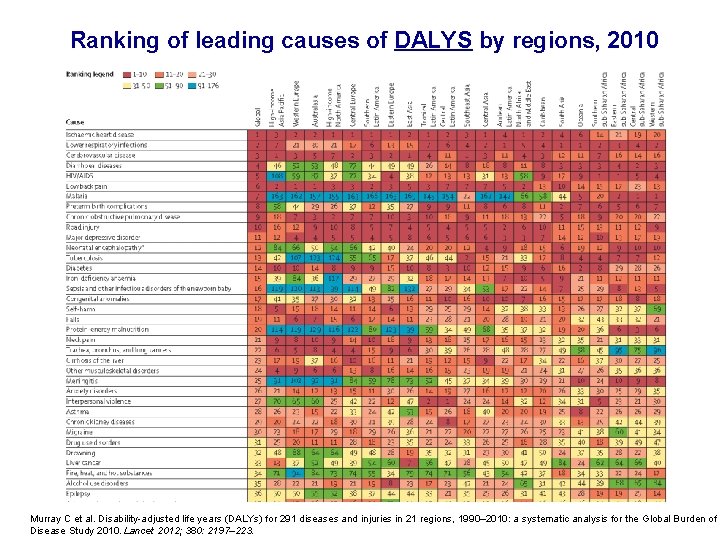
Ranking of leading causes of DALYS by regions, 2010 Murray C et al. Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990– 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380: 2197– 223.
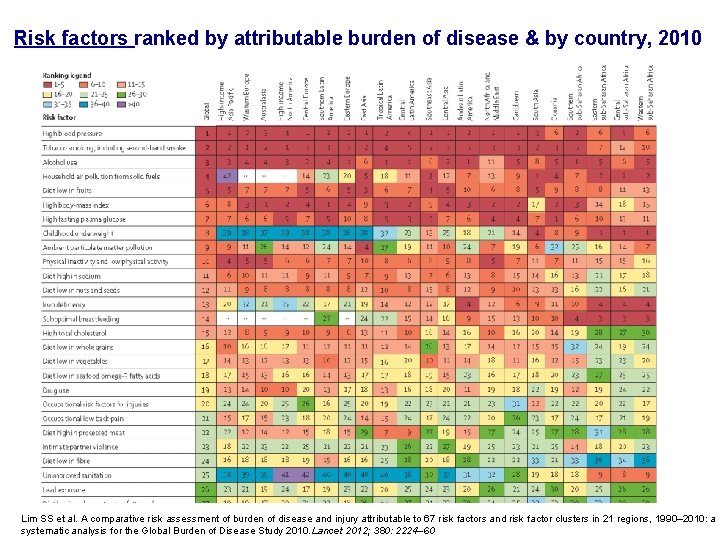
Risk factors ranked by attributable burden of disease & by country, 2010 Lim SS et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990– 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380: 2224– 60
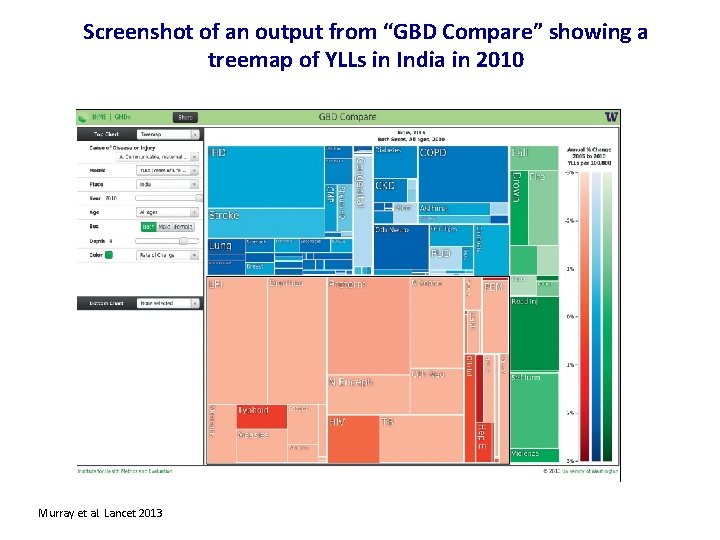
Screenshot of an output from “GBD Compare” showing a treemap of YLLs in India in 2010 Murray et al. Lancet 2013
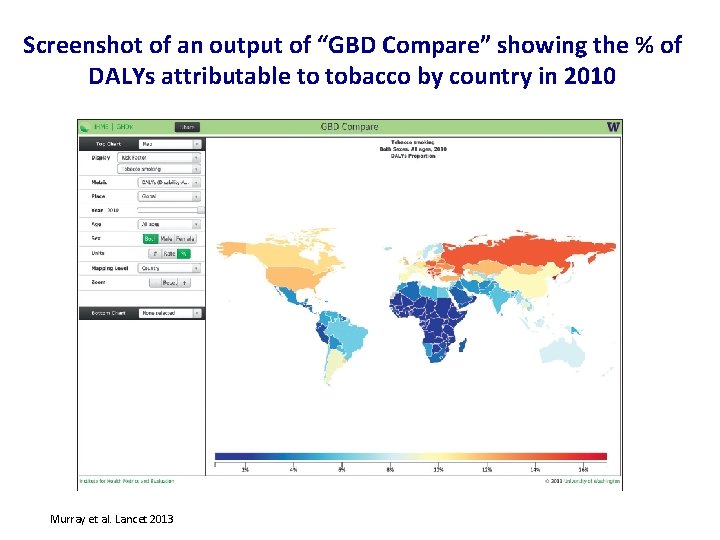
Screenshot of an output of “GBD Compare” showing the % of DALYs attributable to tobacco by country in 2010 Murray et al. Lancet 2013
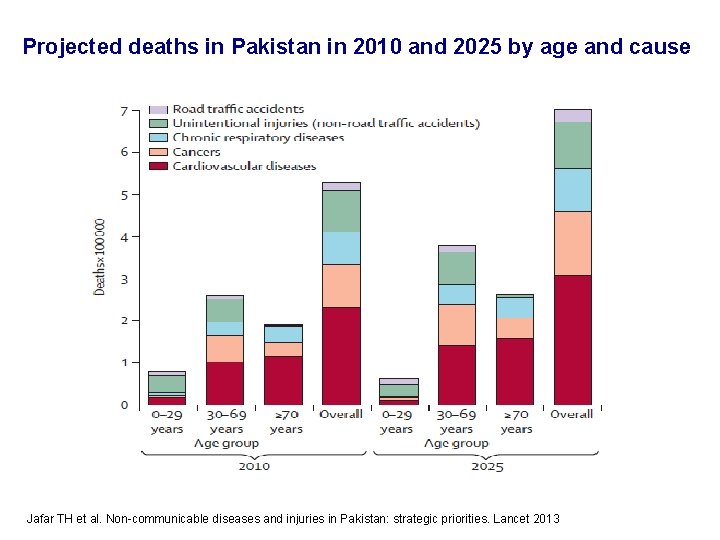
Projected deaths in Pakistan in 2010 and 2025 by age and cause Jafar TH et al. Non-communicable diseases and injuries in Pakistan: strategic priorities. Lancet 2013
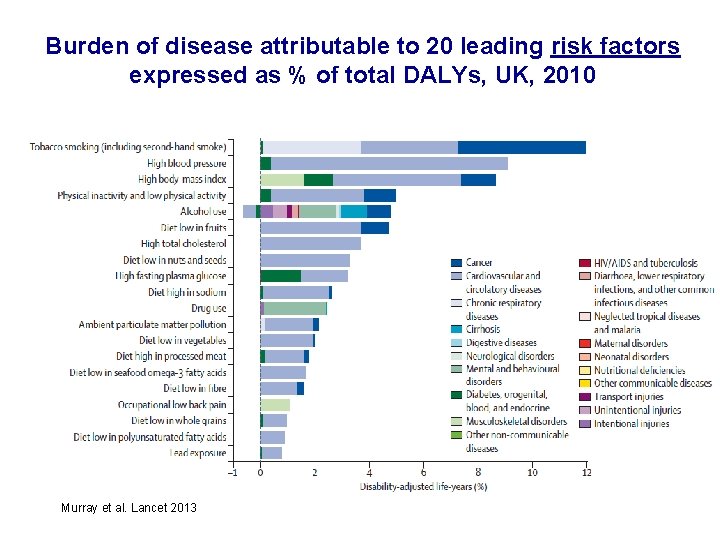
Burden of disease attributable to 20 leading risk factors expressed as % of total DALYs, UK, 2010 Murray et al. Lancet 2013
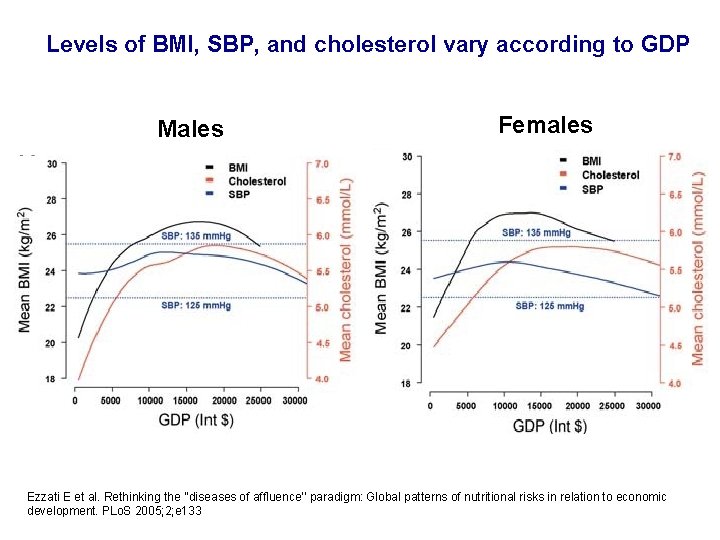
Levels of BMI, SBP, and cholesterol vary according to GDP Males Females Ezzati E et al. Rethinking the ‘‘diseases of affluence’’ paradigm: Global patterns of nutritional risks in relation to economic development. PLo. S 2005; 2; e 133
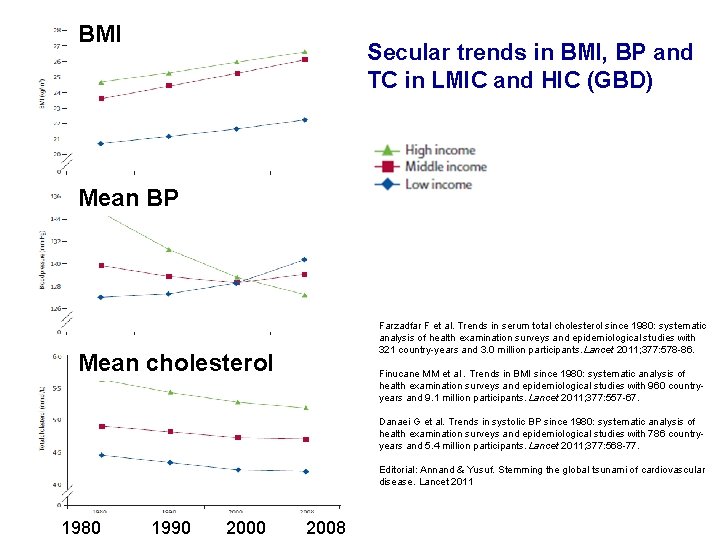
BMI Secular trends in BMI, BP and TC in LMIC and HIC (GBD) Mean BP Mean cholesterol Farzadfar F et al. Trends in serum total cholesterol since 1980: systematic analysis of health examination surveys and epidemiological studies with 321 country-years and 3. 0 million participants. Lancet 2011; 377: 578 -86. Finucane MM et al. Trends in BMI since 1980: systematic analysis of health examination surveys and epidemiological studies with 960 countryyears and 9. 1 million participants. Lancet 2011; 377: 557 -67. Danaei G et al. Trends in systolic BP since 1980: systematic analysis of health examination surveys and epidemiological studies with 786 countryyears and 5. 4 million participants. Lancet 2011; 377: 568 -77. Editorial: Annand & Yusuf. Stemming the global tsunami of cardiovascular disease. Lancet 2011 1980 1990 2008
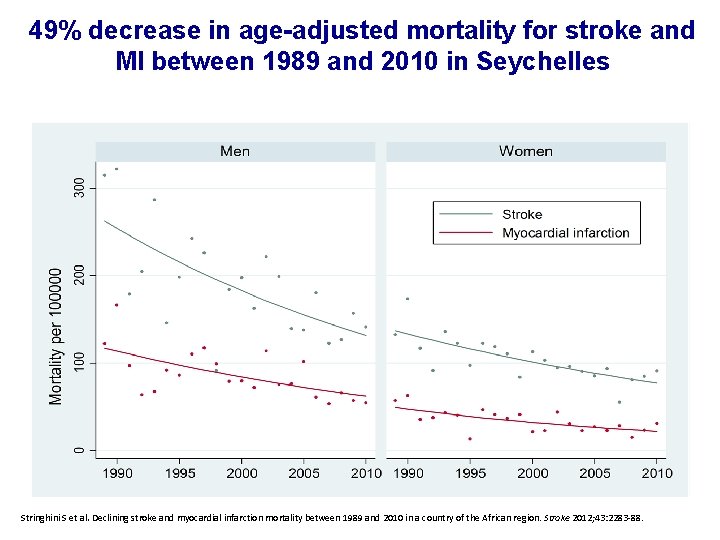
49% decrease in age-adjusted mortality for stroke and MI between 1989 and 2010 in Seychelles Stringhini S et al. Declining stroke and myocardial infarction mortality between 1989 and 2010 in a country of the African region. Stroke 2012; 43: 2283 -88.
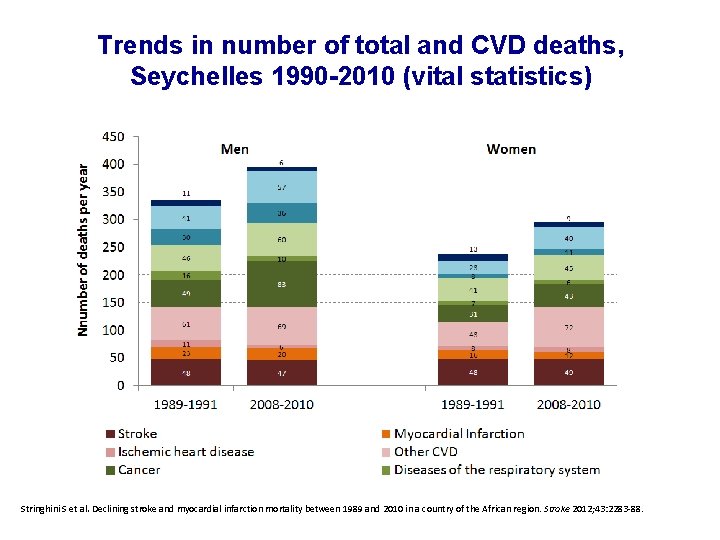
Trends in number of total and CVD deaths, Seychelles 1990 -2010 (vital statistics) Stringhini S et al. Declining stroke and myocardial infarction mortality between 1989 and 2010 in a country of the African region. Stroke 2012; 43: 2283 -88.
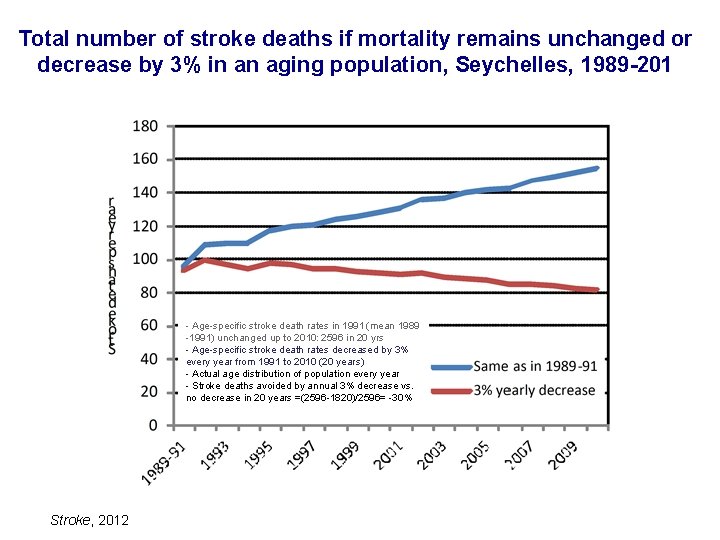
Total number of stroke deaths if mortality remains unchanged or decrease by 3% in an aging population, Seychelles, 1989 -201 - Age-specific stroke death rates in 1991 (mean 1989 -1991) unchanged up to 2010: 2596 in 20 yrs - Age-specific stroke death rates decreased by 3% every year from 1991 to 2010 (20 years) - Actual age distribution of population every year - Stroke deaths avoided by annual 3% decrease vs. no decrease in 20 years =(2596 -1820)/2596= -30% Stroke, 2012
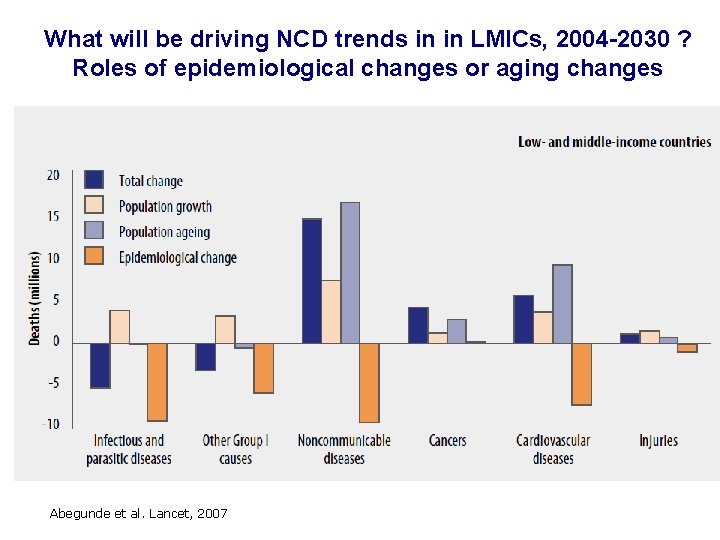
What will be driving NCD trends in in LMICs, 2004 -2030 ? Roles of epidemiological changes or aging changes Abegunde et al. Lancet, 2007
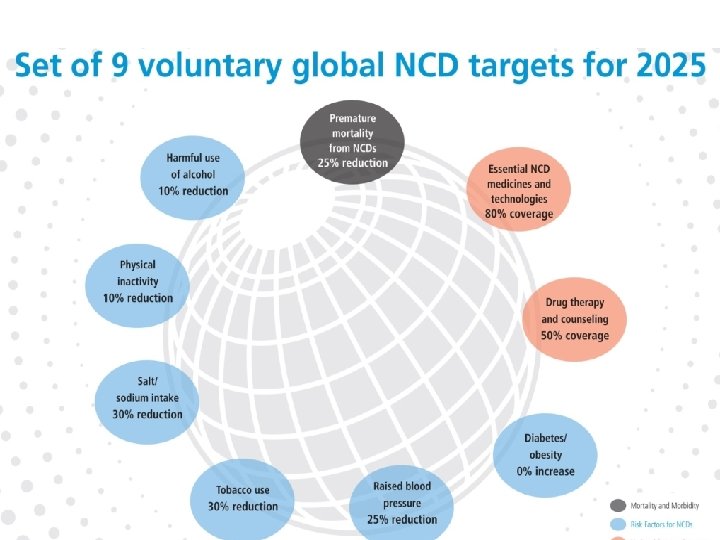

Health transition: a tool for anticipating and planning health response ! I skate where the puck will be Wayne Gretsky « Greatest hockey player of all time »
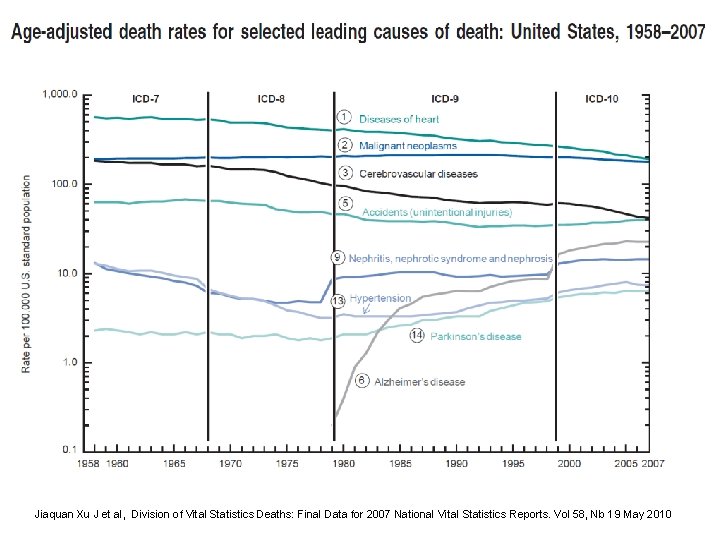
Jiaquan Xu J et al, Division of Vital Statistics Deaths: Final Data for 2007 National Vital Statistics Reports. Vol 58, Nb 19 May 2010

The health transition and GBD: some conclusions • Link between demographic/social changes and disease patterns • Patterns vary by region, country, region and within settings • Double burden of disease in many countries • Transition to NCDs is inevitable as populations are aging • Patterns of NCD will change over time (from CVD -> Cancer -> Neuro) • Need to reduce risk factors (and rates of NCDs) faster than aging of populations to contain (an eventually reduce) the total numbers of NCD deaths • Transition model provides rationale for prospective planning, also when epidemiological data are not available locally or NCDs are not yet preponderant • Good news : later transition stages predicts reduced rates of the “big four” NCDs (conditional to appropriate policy and health care response)
- Slides: 44