EPIC Breastfeeding 2018 Program Breastfeeding Fundamentals Breastfeeding education

EPIC Breastfeeding ® 2018 Program “Breastfeeding Fundamentals” Breastfeeding education Copyright © 2007 Georgia Chapter, American Academy of Pediatrics. All rights reserved.

Faculty Disclosure Information • In accordance with ACCME* Standards for commercial support, all faculty members are required to disclose to the program audience any real or apparent conflict(s) of interest to the content of their presentation. I would like to disclose the following: * Accreditation Council for Continuing Medical Education

Program Objectives • Describe two risk factors of mothers choosing not to breastfeed • Discuss why physicians play critical roles in a woman’s decision to breastfeed • Demonstrate how to assist with effective breastfeeding techniques • Review access to lactation support services in the community

EPIC Program Funding This presentation is made possible by the Georgia Department of Public Health (DPH) through a contract managed and in partnership with Georgia Chapter - American Academy of Pediatrics (GA AAP). Neither DPH nor Contractor is responsible for any misuse or copyright infringement with respect to the material.

EPIC Breastfeeding Program Partners • Georgia Chapter - American Academy of Pediatrics • Georgia OB/GYN Society • Georgia Academy of Family Physicians • Centers for Disease Control & Prevention (CDC) • The Georgia Department of Public Health – Maternal and Child Health Program

AAP’s Breastfeeding Policy Statement “The American Academy of Pediatrics reaffirms its recommendation of exclusive breastfeeding for about 6 months, followed by continuation of breastfeeding for 1 year or longer as mutually desired by mother and infant. AAP Policy Statement: Breastfeeding and the Use of Human Milk, Feb. 13, 2013,
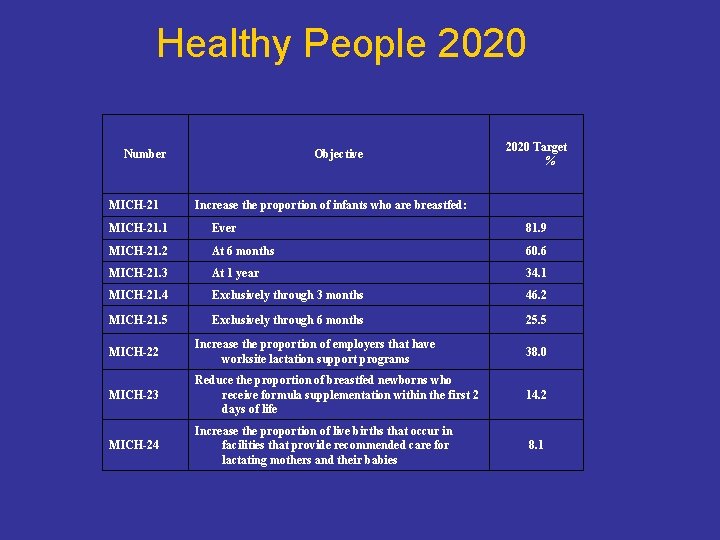

Healthy People 2020 Number MICH-21 Objective 2020 Target % Increase the proportion of infants who are breastfed: MICH-21. 1 Ever 81. 9 MICH-21. 2 At 6 months 60. 6 MICH-21. 3 At 1 year 34. 1 MICH-21. 4 Exclusively through 3 months 46. 2 MICH-21. 5 Exclusively through 6 months 25. 5 MICH-22 Increase the proportion of employers that have worksite lactation support programs 38. 0 MICH-23 Reduce the proportion of breastfed newborns who receive formula supplementation within the first 2 days of life 14. 2 MICH-24 Increase the proportion of live births that occur in facilities that provide recommended care for lactating mothers and their babies 8. 1
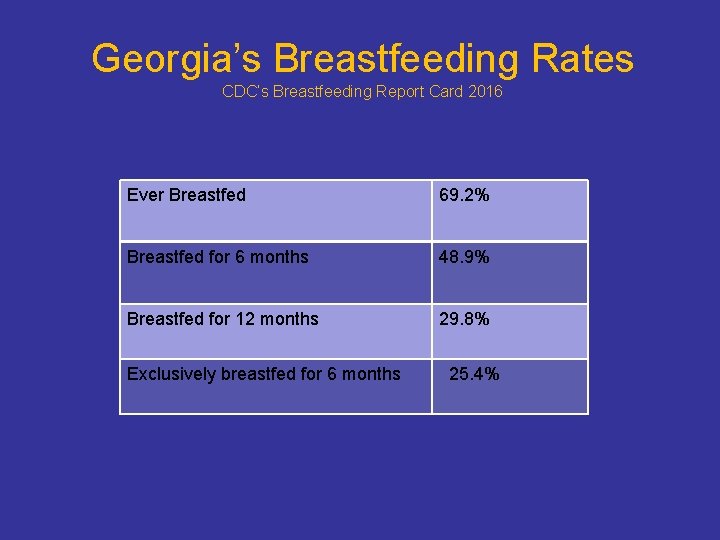
Georgia’s Breastfeeding Rates CDC’s Breastfeeding Report Card 2016 Ever Breastfed 69. 2% Breastfed for 6 months 48. 9% Breastfed for 12 months 29. 8% Exclusively breastfed for 6 months 25. 4%

60% of Mothers do not Breastfeed for as Long as they Intended • • • Issues with latch Concern about infant weight Medications Lack of family support Unsupportive hospital practices and policies • Unsupportive work place
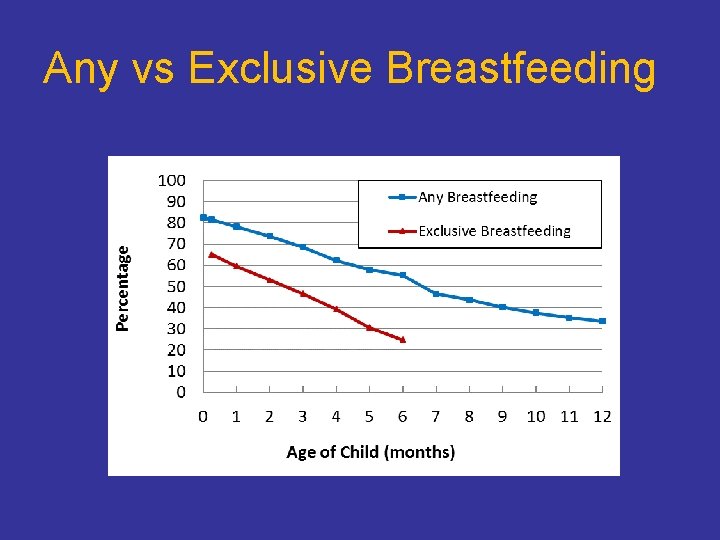
Any vs Exclusive Breastfeeding

Support for Minorities • It’s Only Natural • Launched by the Office of Women's Health • Discuss benefits, myths, and challenges • www. womenshealth. gov/itsonlynatural • Reaching our Sisters Everywhere (ROSE) • • Support and information for women of color Started here in Atlanta Baby Café Breastfeedingrose. org

Disease and Risk Reduction in Breastfed Infants and Children Acute Otitis Media 50% Atopic Dermatitis 42% Gastrointestinal Infections 64% Lower respiratory infections, hospital rate 72 -77% Asthma 26 -40% Obesity 24% Type I Diabetes 30% Type II Diabetes 40% Childhood Leukemia 20% http: //pediatrics. aappublications. org/c ontent/125/5/e 1048. short. A

Maternal Disease Risk Reduction from Breastfeeding Diabetes 12% Metabolic syndrome 8. 4% Ovarian Cancer 21% Breast Cancer 4. 3% Coronary Artery Disease 23% Aortic Calcifications 22% Coronary Calcifications 15% http: //pediatrics. aappublications. org/content/125/5/e 1048. short

Challenges for Physicians • Lack of breastfeeding knowledge and training • Discomfort examining and discussing breasts • Discomfort treating mother and baby • Lack of time • Concerns about reimbursement and coding

Early Breastfeeding is Crucial • Breastfeed within the first hour • Skin to Skin after delivery

What are Early Infant Feeding Cues? – Sucking sounds – Hand to mouth movements – Rapid eye movement – Soft cooing or sighing sounds – Restlessness Crying is a late hunger cue!
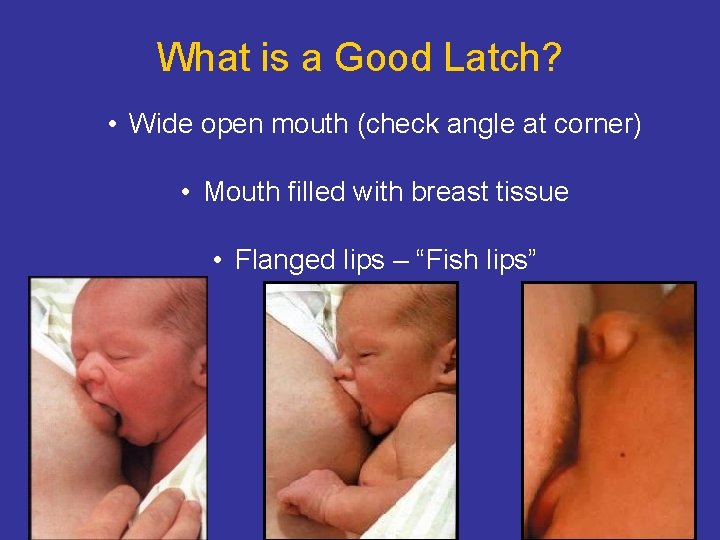
What is a Good Latch? • Wide open mouth (check angle at corner) • Mouth filled with breast tissue • Flanged lips – “Fish lips”

Jack Newman, MD Assisting with a Good Latch: •

What are the Signs of Effective Milk Transfer? • Audible swallowing • Appropriate output (i. e. urine/stools) • Weight gain of 5 oz a week after day 4

What Increases Milk Production? Milk Removal!

Role of Physicians Help parents develop realistic expectations

OB/Gyn Prenatal Visit • Mothers need to hear from their OB that breastfeeding is important • Encourage breastfeeding classes • Discuss why her breasts are changing • Educate the expectant mother and her partner • Do not give out any formula coupons or freebies with formula branding to patients

Pediatric/FP Prenatal Visit • Ask open ended questions – What are you thinking about breastfeeding? – What have your friends and family said about breastfeeding? – What breastfeeding plans do you have when returning to work? – What do you know about the benefits of breast milk? • Help mom set realistic expectations • Discuss potential barriers and suggest possible solutions

What are Maternal Risk Factors for Unsuccessful Breastfeeding? • • Breast surgery or trauma Breast or nipple abnormality Absence of prenatal breast changes Previous breastfeeding difficulty Birth interventions Separation from infant Mother’s perception of insufficient milk supply Unrelieved fullness or engorgement

What are Infant Risk Factors for Unsuccessful Breastfeeding? • • Birth interventions and/or trauma Prematurity Acute or chronic disease Oral anomalies Hyperbilirubinemia or hypoglycemia SGA, LGA or IUGR Persistent sleepiness or irritability Inability to maintain an effective latch
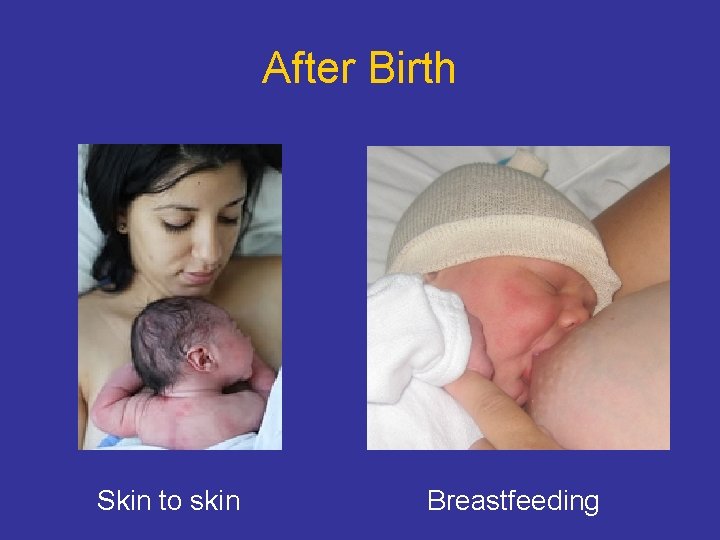
After Birth Skin to skin Breastfeeding

In the Hospital • Skin to skin after delivery • Baby stays with mom for first hour after delivery • Limit procedures • Rooming in – limit visitors • Exclusive breastfeeding is encouraged – Avoid use of supplements and pacifiers

Exclusive Breastfeeding • No food or drink other than breastmilk • Mothers own milk is the first choice • No promotion of breast milk substitutes, bottles or pacifiers given to parents. • If supplementation is necessary staff have specific protocols/policies to follow

Separation of Mother and Baby • Start pumping ASAP – Pump and hand express every 2 -3 hours – Use a hospital grade pump – Pump at baby’s bedside if possible • Hand expression – Increases volume collected – Can be used while single pumping – www. newborns. stanford. edu/Breastfeeding/ Hand. Expression • Encourage Skin to skin

Baby’s First Office Visit • What to Do… – Schedule visit within 1 -2 days of hospital discharge – Evaluate weight loss / gain – Evaluate breastfeeding frequency / duration – Evaluate outputs i. e. urine / stool – Look for signs of jaundice – Observe the baby breastfeed – Encourage support groups

Breast Problems to Avoid • Engorgement • Plugged milk ducts • Nipple Pain / Trauma • Mastitis • Candidiasis / Thrush
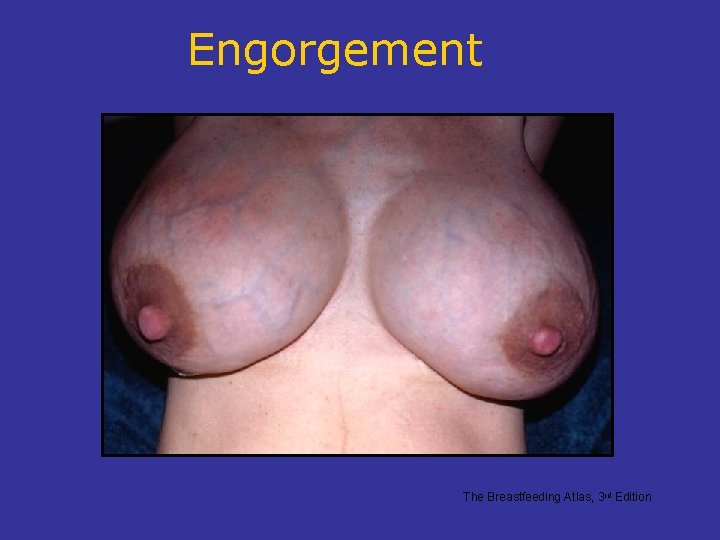
Engorgement The Breastfeeding Atlas, 3 rd Edition
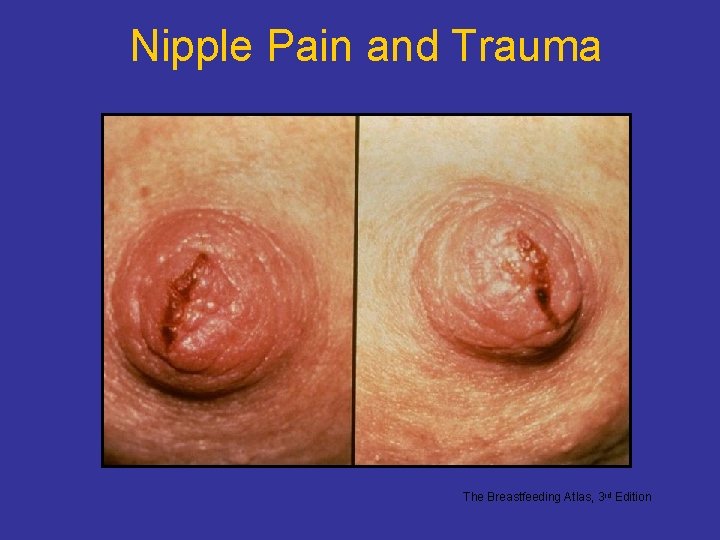
Nipple Pain and Trauma The Breastfeeding Atlas, 3 rd Edition
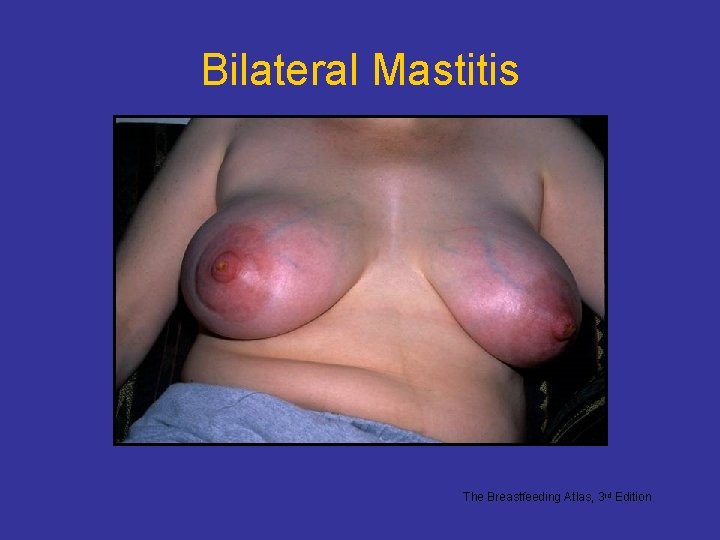
Bilateral Mastitis The Breastfeeding Atlas, 3 rd Edition

Plugged Duct • Presents as a hard, red, tender area on the breast • May progress into mastitis • Have the patient – Feed frequently on infected side – Massage area during breastfeeding – Change positioning at the breast – Check bra’s for correct fit and avoid underwire bras
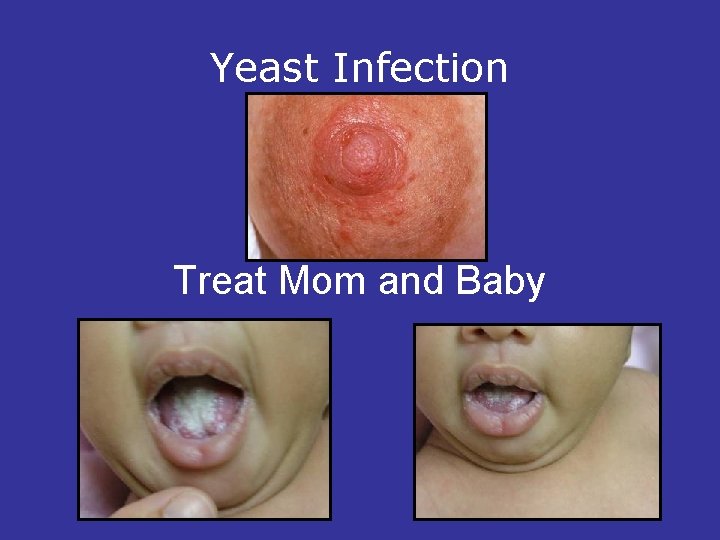
Yeast Infection Treat Mom and Baby

Maternal Emotions • Perinatal Mood Disorders • Edinburg Postpartum Depression scale • Every provider has responsibility to assess mother’s mood • Acknowledge and validate feelings of frustration, anxiety, inadequacy, etc. • Project Healthy Moms - Warmline in GA is 1. 800. 933. 9896(x 234)

Medications Usually the risk of NOT breastfeeding is greater than the risk of exposure through breastmilk Resources: • “Medication and Mothers Milk” • Lact. Med @ http: //toxnet. nlm. nih. gov/cgi-bin/sis/htmlgen? LACT • Poison control - 404. 616. 9000 or 1. 800. 222. 1222

Maternal Medications Short list of contraindicated medications: Lithium Phenindione Amiodarone Retinoids Chemotherapy agents Chloramphenicol Drugs of Abuse Ergotamine Gold salts Tetracyclines (chronic use >3 weeks) Radioactive Compounds

Hot Topics • Bed Sharing vs Co-sleeping • Pacifiers • Supplementation • Starting solids • Returning to work • Contraception • Milk Sharing • Vitamin D

ICD 10 Codes for the Infant P 92. 8 P 92. 3 Feeding problems, newborn Under feeding of the newborn R 68. 12 Fussy baby/infant P 59. 3 Jaundice (breastmilk) P 59. 9 Jaundice (unspecified) P 92. 6 Failure to thrive R 63. 6 Underweight Q 38. 1 Ankyloglossia

ICD 10 Codes for the Mother 092. 70 Unspecified disorders of lactation 092. 5 Suppressed lactation R 53. 83 Fatigue Z 39. 1 Care and examination of lactating mother 091. 03 Sore nipples 091. 23 Nonpurulent mastitis associated with lactation

The Breastfeeding Friendly Physician Office • Have a breastfeeding policy • Train staff • Provide a supportive environment – No free formula samples – No commercial advertisements • Encourage exclusive breastfeeding

Community Resources • Hospitals – Support groups – Lactation clinics • WIC – Breast pumps – Lactation assistance – Peer counselors • • • La Leche League Georgia Breastfeeding Coalition ZIPMilk Baby Café Licensed Lactation Consultants

“While breastfeeding may not seem the right choice for every parent, it is the best choice for every baby. ” Breastfeeding: Your Guide to a Healthy, Happy Baby, 2005

- Slides: 46