ePharmacy Claims Best Practices Ve HU Session 115

e-Pharmacy Claims Best Practices Ve. HU Session #115 May 24, 2005

Faculty • Greg Laird, RPh, Pharmacy Operations Mgr Eastern Kansas HCS – VAMC Topeka • Janet Graham, RPh, Pharmacy ADPAC VAMC Louisville • Judy Petersen, RPh, Pharmacy ADPAC VAMC Saginaw 2

Objectives • Provide an overview of e-Pharmacy • Identify business practice changes that accompany e-Pharmacy • Discuss latest updates and changes • Help prepare users for national release of active software 3

e-Pharmacy Introduction • e-Pharmacy software facilitates billing of prescriptions to third party payers • Used to process claims for patients with prescription co-insurance • Sends real-time electronic claims to third parties via VISTA • Receives replies back from the payers e. g. accepted or rejected • Monitors status of claims 4

ECME • Software used is Electronic Claims Management Engine • It is an off-shoot of the Indian Health Service VISTA program used for the same function • Transmits NCPDP 5. 1 standard fields of information on Rx and patient to third party 5

Pharmacy Set-up and Registration • IRM/ITS loads the software • Pharmacy ADPAC registers Pharmacy and assigns menus • Dormant build allows the site to begin insurance plan matching • Active build provides functionality for actual claims processing 6

Why e-Pharmacy • As many as 10% of the veterans we treat nationwide have third party Rx coverage • We can capture some of our pharmacy expenses by billing their third parties • HIPAA established national standards for electronic claims processing through the National Council for Prescription Drug Programs (NCPDP) • Many third parties will no longer accept paper claims 7

Billing Rules • Currently using e-Pharmacy only for claims that follow federal billing regulations • The charge is $45/prescription • Charge is independent of days supply • Can bill for Rxs for NSC condition – even if patient has greater than 50% SC eligibility • SC Rxs and Rxs connected to Treatment Indicators, (e. g. AO/MST/IR, etc. ) are not billed • Patient’s VA copay is currently reduced by amounts collected from third party 8
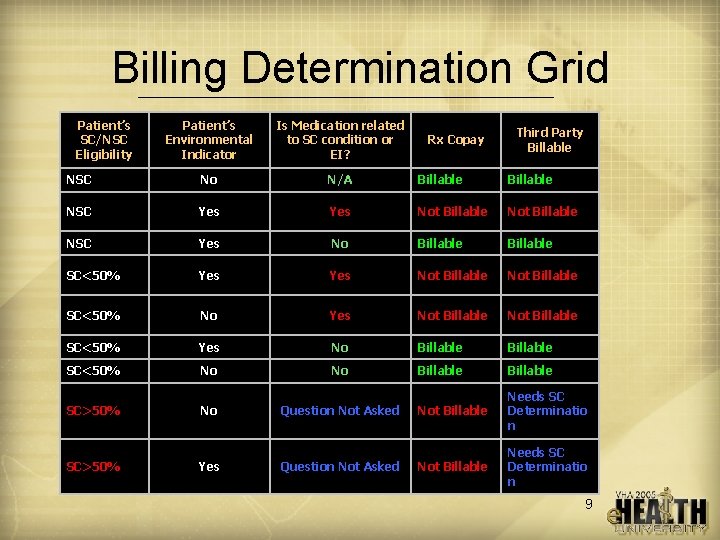
Billing Determination Grid Patient’s SC/NSC Eligibility Patient’s Environmental Indicator Is Medication related to SC condition or EI? NSC No N/A Billable NSC Yes Not Billable NSC Yes No Billable SC<50% Yes Not Billable SC<50% No Yes Not Billable SC<50% Yes No Billable SC<50% No No Billable SC>50% No Question Not Asked Not Billable Needs SC Determinatio n SC>50% Yes Question Not Asked Not Billable Needs SC Determinatio n Rx Copay Third Party Billable 9

Sensitive Drugs US Code of Federal Regulations prevents VA from informing third parties that patients have AIDS, Sickle Cell Anemia, Drug Abuse, or Alcohol Abuse without the patients permission (VA Handbook 1605. 1, Subpart 14) • If we send claims for medications exclusively used to treat those conditions we may be violating privacy regulations • Release of Information permissions now obtained and maintained manually • Currently, no national electronic ROI system to automate this process. 10

Sensitive Drugs Continued • Interim fix is to place an 0 or M in the DEA, Special Hdlg Field (3) in Drug File (50) of drugs like Lamivudine, etc. • This prevents Rxs for those drugs from transmitting claims • Issue being discussed at CBO level • If it is determined we need to have this permission for billing third party Rxs there will be software developed to enhance process 11

Other Billing Aspects • Only legend drugs and some OTCs like insulin and diabetic test strips are billed • Add an ‘E’ to DEA Special Handling Field to flag these OTC items so they will bill • Not to change an Rx from a 90 to a 30 days supply just to get a claim to go through • Unless reject is a DUR or Refill too Soon, label will print and Rx will be filled without Pharmacy intervention • Provider DEA number is pulled from New Person file (#200) • If DEA number is not found in New Person file software defaults to facility DEA number 12
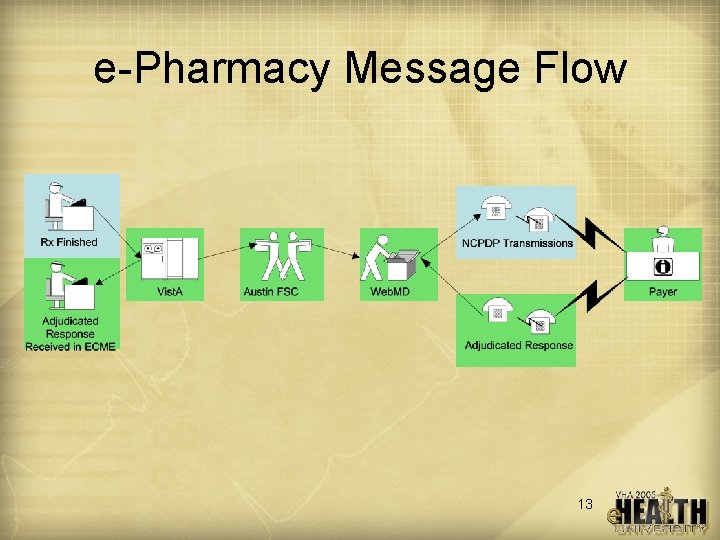
e-Pharmacy Message Flow 13

Acres of Acronyms • • • • NCPDP NABP# DUR DAW FDB BIN PCN ECME BPS OPECC IHS AAC FSC HIPAA National Council for Prescription Drug Programs National Association of Boards of Pharmacy # Drug Utilization Review Dispense as Written First Data Bank Identification Number Processor Control Number Electronic Claims Management Engine Namespace for ECME Package Outpatient Pharmacy Electronic Claims Coordinator Indian Health Service Austin Automation Center Financial Services Center Health Insurance Portability and Accountability Act 14

Pharmacy Business Practice Changes 15

When e-Pharmacy Claims are submitted/resubmitted • Rx Finish • Rx Release • Rx Edit (* field changed) • Rx Renew • Rx Copy When e-Pharmacy Claims are canceled/reversed • Rx Delete • Rx Return to Stock • Automatic claim reversal for payable Rxs not released within sitedefined time period – Local & CMOP Rxs 16

Claims Transmission – Rx Finish • • Claim is transmitted when new Rx is finished Software automatically chooses a product NDC from drug file using the following logic: – First checks appropriate new multiple field called NDC BY OUTPATIENT SITE (field #32 in file #50) Choose from: . 01 1 2 OUTPATIENT SITE LAST LOCAL NDC LAST CMOP NDC – If no “last” NDC exists, uses data from NDC field (field #31 of file #50) 17

Claims Transmission - Rx Finish (cont. ) • Message lines show a claim is being sent • If messaging takes longer than site-defined timeout, finishing RPh goes to next Rx • Average Beta-test turn-around time for Beta Sites for last 6 months is ~10 seconds • ECME Time-Out is site-configurable 18
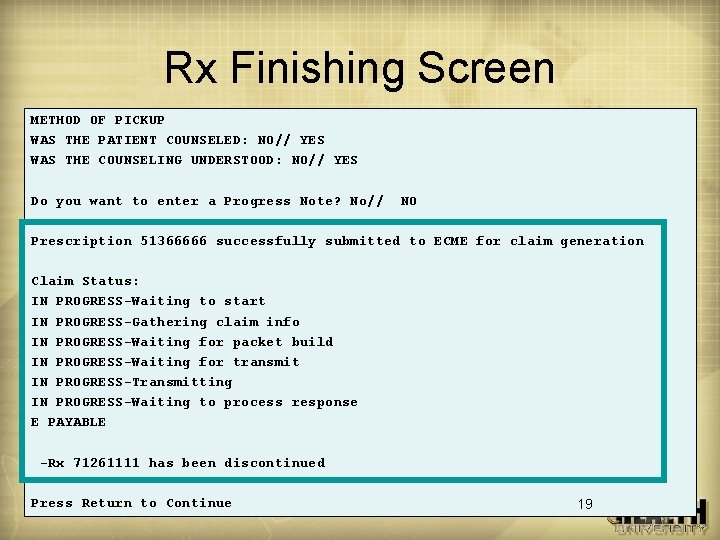
Rx Finishing Screen METHOD OF PICKUP WAS THE PATIENT COUNSELED: NO// YES WAS THE COUNSELING UNDERSTOOD: NO// YES Do you want to enter a Progress Note? No// NO Prescription 51366666 successfully submitted to ECME for claim generation Claim Status: IN PROGRESS-Waiting to start IN PROGRESS-Gathering claim info IN PROGRESS-Waiting for packet build IN PROGRESS-Waiting for transmit IN PROGRESS-Transmitting IN PROGRESS-Waiting to process response E PAYABLE -Rx 71261111 has been discontinued Press Return to Continue 19

Other Times Claims are Initially Submitted • At finish for electronic (CPRS) orders as well as back door entry of new Rxs • Directly after the ‘Now Refilling’ message for local window and local mail fills • When Rxs are pulled from suspense 20

DUR Rejections • DURs occur when a third party determines there are safety issues involved with an Rx claim submission • Can be due to high dose, drug interaction, excessive utilization etc. • With e-Pharmacy medication information is now shared, and rejections can also occur as a result of the linked profiles • Third party usually returns NCPDP rejection code 88 to indicate a DUR 21

DUR Rejections (cont. ) • OP V 7. 0 will store DUR reject information, e. g. date/time, rejection text, reason etc. • RPh will need to be involved with DUR resolution and may need to consult provider • Sometimes may fill without resolving rejection with third party – RPh closes reject • VISTA label will not print until resolved, overridden, or closed 22

Refill Too Soon Rejections • Happens when third party determines Rx is being processed too early compared to the last time Rx was filled • Reasons: – Third parties refill early policy may be different from VA policy – Patient may also be getting at another Pharmacy – Provider may have increased dose or frequency • NCPDP rejection code sent back from third party is 79 23

Refill Too Soon Rejections (cont. ) • RPh may choose to ignore reject and continue with fill process • VISTA OP v 7. 0 will have a ‘Third Party DUR/Refill Too Soon Rejects Processing’ option that will – Display DUR and Refill Too Soon rejection messages – Display third party and patient information needed for consultation – Provide ability to input over-ride codes if needed to get claim to go through – Set aside Rx to work claim at a later date or time 24
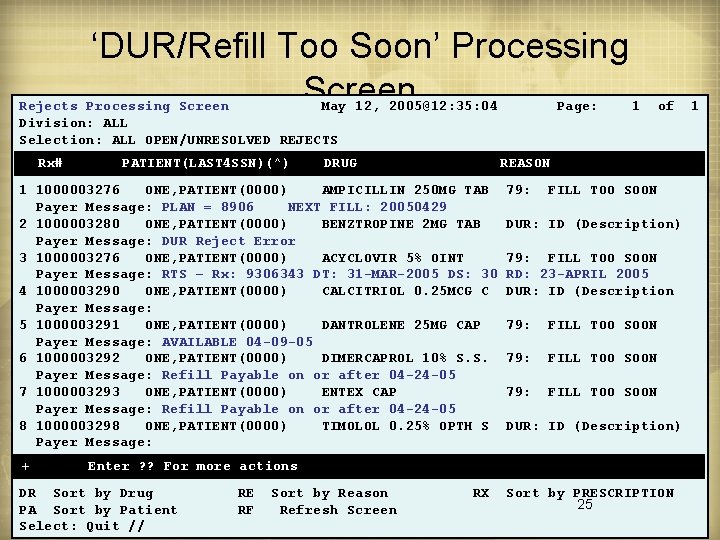
‘DUR/Refill Too Soon’ Processing Screen Rejects Processing Screen May 12, 2005@12: 35: 04 Division: ALL Selection: ALL OPEN/UNRESOLVED REJECTS Rx# PATIENT(LAST 4 SSN)(^) DRUG 1 of REASON 1 1000003276 ONE, PATIENT(0000) AMPICILLIN 250 MG TAB Payer Message: PLAN = 8906 NEXT FILL: 20050429 2 1000003280 ONE, PATIENT(0000) BENZTROPINE 2 MG TAB Payer Message: DUR Reject Error 3 1000003276 ONE, PATIENT(0000) ACYCLOVIR 5% OINT Payer Message: RTS – Rx: 9306343 DT: 31 -MAR-2005 DS: 30 4 1000003290 ONE, PATIENT(0000) CALCITRIOL 0. 25 MCG C Payer Message: 5 1000003291 ONE, PATIENT(0000) DANTROLENE 25 MG CAP Payer Message: AVAILABLE 04 -09 -05 6 1000003292 ONE, PATIENT(0000) DIMERCAPROL 10% S. S. Payer Message: Refill Payable on or after 04 -24 -05 7 1000003293 ONE, PATIENT(0000) ENTEX CAP Payer Message: Refill Payable on or after 04 -24 -05 8 1000003298 ONE, PATIENT(0000) TIMOLOL 0. 25% OPTH S Payer Message: + Page: 79: FILL TOO SOON DUR: ID (Description) 79: FILL TOO SOON RD: 23 -APRIL 2005 DUR: ID (Description 79: FILL TOO SOON DUR: ID (Description) Enter ? ? For more actions DR Sort by Drug PA Sort by Patient Select: Quit // RE RF Sort by Reason Refresh Screen RX Sort by PRESCRIPTION 25 1
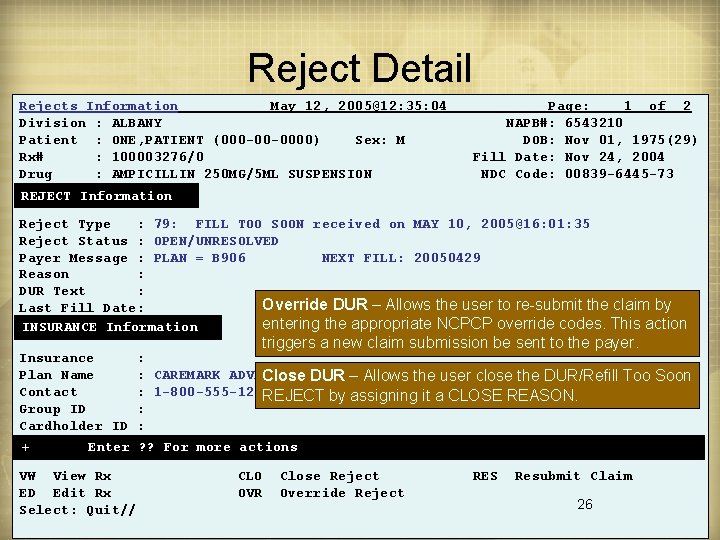
Reject Detail Rejects Information May 12, 2005@12: 35: 04 Division : ALBANY Patient : ONE, PATIENT (000 -00 -0000) Sex: M Rx# : 100003276/0 Drug : AMPICILLIN 250 MG/5 ML SUSPENSION Page: 1 of 2 NAPB#: 6543210 DOB: Nov 01, 1975(29) Fill Date: Nov 24, 2004 NDC Code: 00839 -6445 -73 REJECT Information Reject Type : 79: FILL TOO SOON received on MAY 10, 2005@16: 01: 35 Reject Status : OPEN/UNRESOLVED Payer Message : PLAN = B 906 NEXT FILL: 20050429 Reason : DUR Text : Override DUR – Allows the user to re-submit the claim by Last Fill Date: entering the appropriate NCPCP override codes. This action INSURANCE Information Insurance Plan Name Contact Group ID Cardholder ID + triggers a new claim submission be sent to the payer. : : CAREMARK ADVANCE RECAP Close DUR CLAIMS – Allows the user close the DUR/Refill Too Soon : 1 -800 -555 -1234 REJECT by assigning it a CLOSE REASON. : : Enter ? ? For more actions VW View Rx ED Edit Rx Select: Quit// CLO OVR Close Reject Override Reject RES Resubmit Claim 26
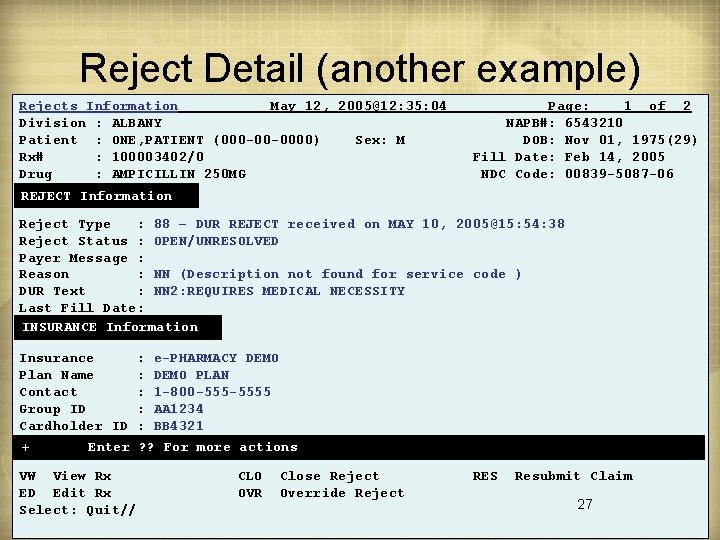
Reject Detail (another example) Rejects Information May 12, 2005@12: 35: 04 Division : ALBANY Patient : ONE, PATIENT (000 -00 -0000) Sex: M Rx# : 100003402/0 Drug : AMPICILLIN 250 MG Page: 1 of 2 NAPB#: 6543210 DOB: Nov 01, 1975(29) Fill Date: Feb 14, 2005 NDC Code: 00839 -5087 -06 REJECT Information Reject Type : 88 – DUR REJECT received on MAY 10, 2005@15: 54: 38 Reject Status : OPEN/UNRESOLVED Payer Message : Reason : NN (Description not found for service code ) DUR Text : NN 2: REQUIRES MEDICAL NECESSITY Last Fill Date: INSURANCE Information Insurance Plan Name Contact Group ID Cardholder ID + : : : e-PHARMACY DEMO PLAN 1 -800 -5555 AA 1234 BB 4321 Enter ? ? For more actions VW View Rx ED Edit Rx Select: Quit// CLO OVR Close Reject Override Reject RES Resubmit Claim 27

DUR Processing - Overrides • DUR overrides obtained by using a set of three NCPDP service codes – Reason for Service – Why the claim rejected, e. g. HD – High Dose – Professional Service – what was done to justify filling, e. g. M 0 – Prescriber Consulted – Result of Service – e. g. 1 G, Filled, with Prescriber Approval 28

DUR Processing – Documentation • New section on the medication profile screen for unresolved DUR or Fill to Soon rejects • In the ECME activity log section of each prescription 29
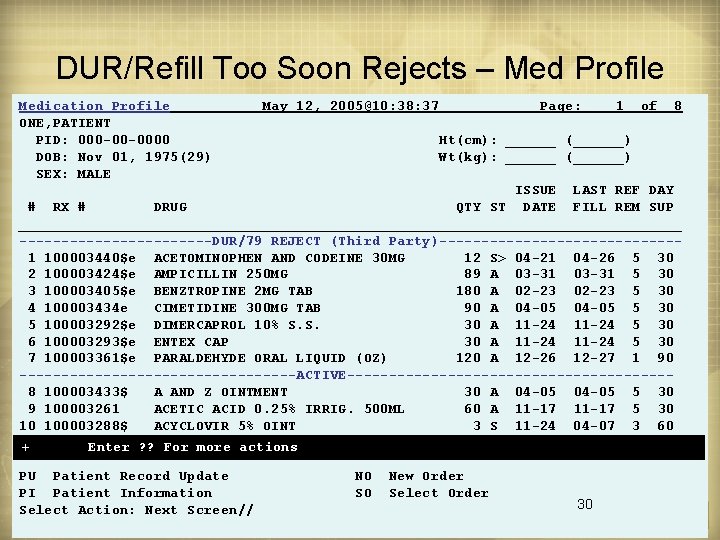
DUR/Refill Too Soon Rejects – Med Profile Medication Profile ONE, PATIENT PID: 000 -00 -0000 DOB: Nov 01, 1975(29) SEX: MALE May 12, 2005@10: 38: 37 Page: 1 of 8 Ht(cm): ______ (______) Wt(kg): ______ (______) ISSUE LAST REF DAY # RX # DRUG QTY ST DATE FILL REM SUP ________________________________________ ------------DUR/79 REJECT (Third Party)--------------1 100003440$e ACETOMINOPHEN AND CODEINE 30 MG 12 S> 04 -21 04 -26 5 30 2 100003424$e AMPICILLIN 250 MG 89 A 03 -31 5 30 3 100003405$e BENZTROPINE 2 MG TAB 180 A 02 -23 5 30 4 100003434 e CIMETIDINE 300 MG TAB 90 A 04 -05 5 30 5 100003292$e DIMERCAPROL 10% S. S. 30 A 11 -24 5 30 6 100003293$e ENTEX CAP 30 A 11 -24 5 30 7 100003361$e PARALDEHYDE ORAL LIQUID (OZ) 120 A 12 -26 12 -27 1 90 -----------------ACTIVE-------------------8 100003433$ A AND Z OINTMENT 30 A 04 -05 5 30 9 100003261 ACETIC ACID 0. 25% IRRIG. 500 ML 60 A 11 -17 5 30 10 100003288$ ACYCLOVIR 5% OINT 3 S 11 -24 04 -07 3 60 + Enter ? ? For more actions PU Patient Record Update PI Patient Information Select Action: Next Screen// NO SO New Order Select Order 30

DUR/Refill Too Soon Rejects – Activity Log ECME DUR: # Date/Time Rx Ref Pharmacist STATUS ======================================== 1 11/29/04@11: 39: 22 ORIGINAL SMITH, KANSAS F RPH UNRESOLVED DUR REASON: LD (LOW DOSAGE ALERT) DUR TEXT : MIN DAILY DOSAGE 1. 00 ECME REFILL TOO SOON: # Date/Time Rx Ref Pharmacist STATUS ======================================== 1 11/29/04@11: 39: 22 ORIGINAL SMITH, KANSAS F RPH UNRESOLVED 79: REFILL TOO SOON 31

Claims Transmission Rx Release (manual) • During the VISTA manual release process staff compares NDC on initial transmission with NDC used to fill Rx • If a different NDC is used, releasing staff must select the dispensed NDC from list • If ECME sees a different NDC for the Rx, it reverses and resubmits the claim with the correct NDC 32
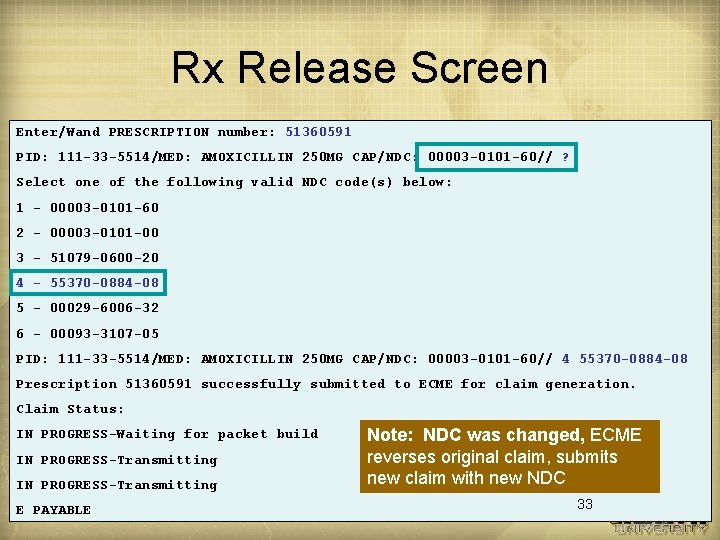
Rx Release Screen Enter/Wand PRESCRIPTION number: 51360591 PID: 111 -33 -5514/MED: AMOXICILLIN 250 MG CAP/NDC: 00003 -0101 -60// ? Select one of the following valid NDC code(s) below: 1 - 00003 -0101 -60 2 - 00003 -0101 -00 3 - 51079 -0600 -20 4 - 55370 -0884 -08 5 - 00029 -6006 -32 6 - 00093 -3107 -05 PID: 111 -33 -5514/MED: AMOXICILLIN 250 MG CAP/NDC: 00003 -0101 -60// 4 55370 -0884 -08 Prescription 51360591 successfully submitted to ECME for claim generation. Claim Status: IN PROGRESS-Waiting for packet build IN PROGRESS-Transmitting E PAYABLE Note: NDC was changed, ECME reverses original claim, submits new claim with new NDC 33
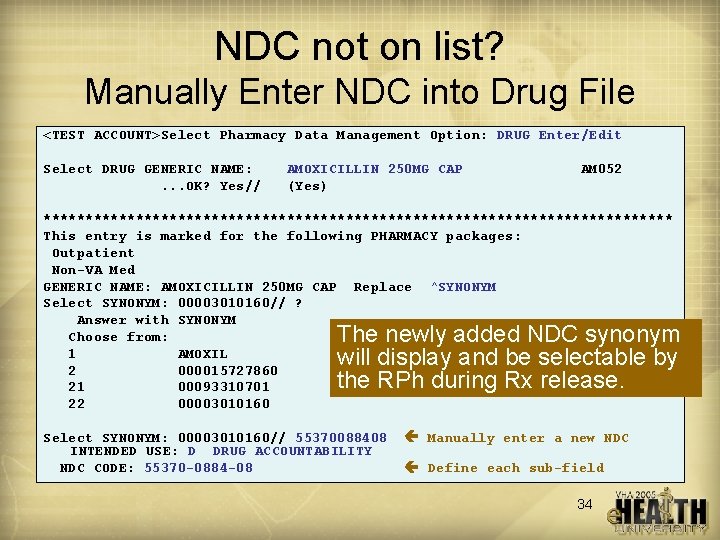
NDC not on list? Manually Enter NDC into Drug File <TEST ACCOUNT>Select Pharmacy Data Management Option: DRUG Enter/Edit Select DRUG GENERIC NAME: . . . OK? Yes// AMOXICILLIN 250 MG CAP (Yes) AM 052 ************************************** This entry is marked for the following PHARMACY packages: Outpatient Non-VA Med GENERIC NAME: AMOXICILLIN 250 MG CAP Replace ^SYNONYM Select SYNONYM: 00003010160// ? Answer with SYNONYM Choose from: 1 AMOXIL 2 000015727860 21 00093310701 22 00003010160 The newly added NDC synonym will display and be selectable by the RPh during Rx release. Select SYNONYM: 00003010160// 55370088408 INTENDED USE: D DRUG ACCOUNTABILITY NDC CODE: 55370 -0884 -08 Manually enter a new NDC Define each sub-field 34

NDC Help • Software automatically chooses a product NDC from drug file using the following logic – First checks appropriate new multiple field called NDC BY OUTPATIENT SITE (field #32 in file #50) Choose from: . 01 1 2 OUTPATIENT SITE LAST LOCAL NDC LAST CMOP NDC – If no “LAST” NDC exists, uses data from NDC field (field #31 of file #50) • NDC transmitted at finish will be the NDC used at release for the last payable NDC for that drug • Laser labels print NDC and ‘ 3 rd Party Rx’ on the patient Rx information portion • The NDC of a released Rx may be changed through PPP e. g. if NDC error was made at release • Note the ‘e’ after the Rx# - used to flag a prescription that had an electronically billable status 35
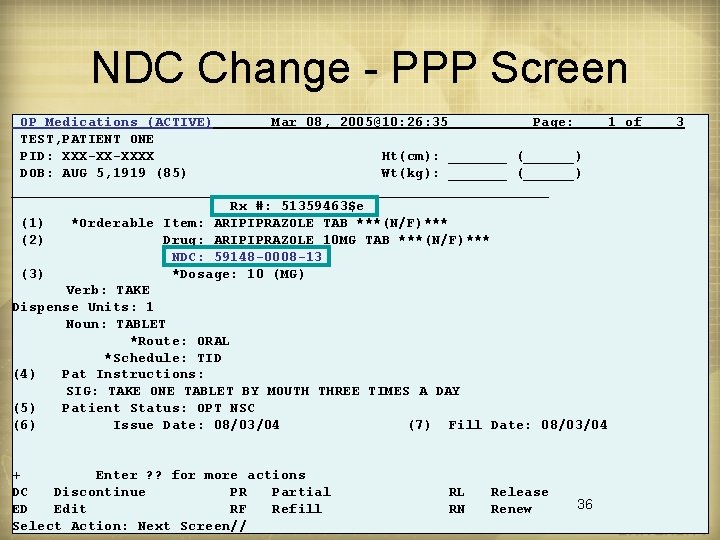
NDC Change - PPP Screen OP Medications (ACTIVE) Mar 08, 2005@10: 26: 35 Page: 1 of TEST, PATIENT ONE PID: XXX-XX-XXXX Ht(cm): _______ (______) DOB: AUG 5, 1919 (85) Wt(kg): _______ (______) ________________________________ Rx #: 51359463$e (1) *Orderable Item: ARIPIPRAZOLE TAB ***(N/F)*** (2) Drug: ARIPIPRAZOLE 10 MG TAB ***(N/F)*** NDC: 59148 -0008 -13 (3) *Dosage: 10 (MG) Verb: TAKE Dispense Units: 1 Noun: TABLET *Route: ORAL *Schedule: TID (4) Pat Instructions: SIG: TAKE ONE TABLET BY MOUTH THREE TIMES A DAY (5) Patient Status: OPT NSC (6) Issue Date: 08/03/04 (7) Fill Date: 08/03/04 + Enter ? ? for more actions DC Discontinue PR Partial ED Edit RF Refill Select Action: Next Screen// RL RN Release Renew 36 3

Laser Label Information PHONE IN OR MAIL THIS REFILL REQUEST Follow the refill instructions provided with your prescription. For Refill Call XXX-XXXX PATIENT ONE TEST XX-XXXX RX# 51360591 MAR 6, 2005 Fill 1 of 1 3 rd Party Rx Qty: 30 Days supply: 10 AMOXICILLIN 250 MG CAP 55370 -0884 -08 11 refills left until MAR 6, 2006 COPAY TOPEKA-589 A 5 (Bar Code) 37

Rx Release Screen (cont. ) Enter/Wand PRESCRIPTION number: 603 -5917462 Prescription Number 3618281 A Released No Refill(s) to be Released No Partial(s) to be Released Enter/Wand PRESCRIPTION number: 603 -5917465 ***WARNING***: 3 rd Party Drug Utilization Review rejection (Plan: ANTHEM PRESCRIPTION MGMT. ) STOP! You need to determine if intervention is required or if Rx can be dispensed, as is, to the patient. 38

Rx Release Screen (cont. ) Enter/Wand PRESCRIPTION number: 603 -5917462 Prescription Number 3618281 A Released No Refill(s) to be Released No Partial(s) to be Released Enter/Wand PRESCRIPTION number: 603 -5917465 ***WARNING***: 3 rd Party Drug Utilization Review rejection (Plan: ANTHEM PRESCRIPTION MGMT. ) Do you want to (P)ROCESS or (H)OLD Rx? P// PROCESS Enter 'P' to fill Rx COMMENTS: 90 DAY FILL RPh is prompted to enter reason for processing DUR Enter your Current Signature Code: SIGNATURE VERIFIED PID: 000 -00 -0000/MED: FORMOTEROL FUMARATE 12 MCG/NDC: 00085 -1401 -01// 00085 -1401 -01 Prescription Number 3876057 Released No Refill(s) to be Released No Partial(s) to be Released Enter/Wand PRESCRIPTION number: 39

Automated Release (OPAI) • For sites using automation that releases Rx through a vendor driven process • If bi-directional interface is present Vist. A will compare vendor NDC to Last Local NDC field • If same NDC then nothing else happens • If different but 11 digits long, ECME will use the vendor NDC for the claim (reverse/resubmit) • If NDC is not 11 digits, ECME will use conversion logic and resubmit • If NDC cannot be determined then ECME will reverse claim 40

Overview of when Claims are Submitted CMOP/Local When the claim is generated New Window Local At the end of finish process, prior to the ‘Q’ prompt Refill Window Local At the end of refill, prior to ‘Q’ prompt New Mail Local When the Rx is pulled from Suspense Refill Mail Local At the end of refill, prior to ‘Q’ prompt and/or When the Rx is pulled from Suspense New Mail CMOP When the Rx is pulled from Suspense Refill Mail CMOP At the end of refill, prior to ‘Q’ prompt and/or When the Rx is pulled from Suspense Mail or Window CMOP or Local At Medication Release (if a claim has not been generated or the Rxs initial claim was reversed or the NDC is changed). After Rx edit of fields implicated in claim Routing 41

Signature Log • Third Parties require documentation that Rxs were picked up by patient – requirement doesn’t apply to mailed Rxs • The trailing document of the laser labels will display third party information for log • Information also displays with non-third party Rxs • Manual signature logs can be pasted into a notebook 42

Signature Log (cont. ) • Logs need to be readily available for 3 rd party audits for 3 years, then filed for another 3 years • Electronic signature devices can be used in lieu of paper signature logs • Eventual goal is to have VA-wide electronic signature log process 43

Signature Log Sample VAMC TOPEKA, KS 66622 589 A 5 (99999/) Ph. XXX-XXXX By Signing below You acknowledge receipt of the following Rx’s Rx# 51360123 MAY 6, 2005 Fill 1 of 1 ____ Pt. Sig. ________________ Caremark Relationship________ Counseled? ____ Test, Patient One 44

CMOP Processing • Claims are sent when Rxs are pulled from suspense • CMOP transmissions will have a 60 second delay to allow third party claims to process and return messages to come back • If a DUR or Refill Too Soon reject occurs or if claim information is not returned from third party, Rx will not be transmitted 45

CMOP Processing (cont. ) • DUR/Refill Too Soon rejections and nonadjudicated Rxs will be placed into the DUR holding mechanism and processed as previously mentioned • Staff will be notified by e-mail or view alerts 46
![Sample CMOP Error Message Subj: 603 CMOP Error Encountered [#1071857] 04/27/05@21: 01 16 lines Sample CMOP Error Message Subj: 603 CMOP Error Encountered [#1071857] 04/27/05@21: 01 16 lines](http://slidetodoc.com/presentation_image_h2/6eb824c2543b8e43685485c9b8eb187b/image-47.jpg)
Sample CMOP Error Message Subj: 603 CMOP Error Encountered [#1071857] 04/27/05@21: 01 16 lines From: POSTMASTER In 'IN' basket. Page 1 *New* -------------------------------------An error has been encountered while processing prescription data for the Consolidated Mail Outpatient Pharmacy system. Date/Time Process Error Type : : : Description : RX # APR 27, 2005@21: 01 Data Validation Invalid or missing data Fill Data Field SSN NAME 1234567 Refill #4 Patient Address 000 -00 -0000 ECME, TEST PATIENT C Action Taken: Rx's not sent to CMOP but still suspended for transmission. Recommended action: Correct invalid data. 47

CMOP Processing (cont. ) • Claims are resubmitted if release data returned from CMOP changes NDC • NDC matching is more complicated than for local fills • Sometimes NDCs returned from CMOP are not in correct format • Sometimes a prepackaged NDC is used that third party does not recognize • CMOP software standardization will improve process 48

ECME Claims Tracking • Menu options for tracking and evaluating claims are available • User screen monitors claims processing in real time • Reports for rejected claims, number of total claims processed, claims transmittal time etc. are available 49
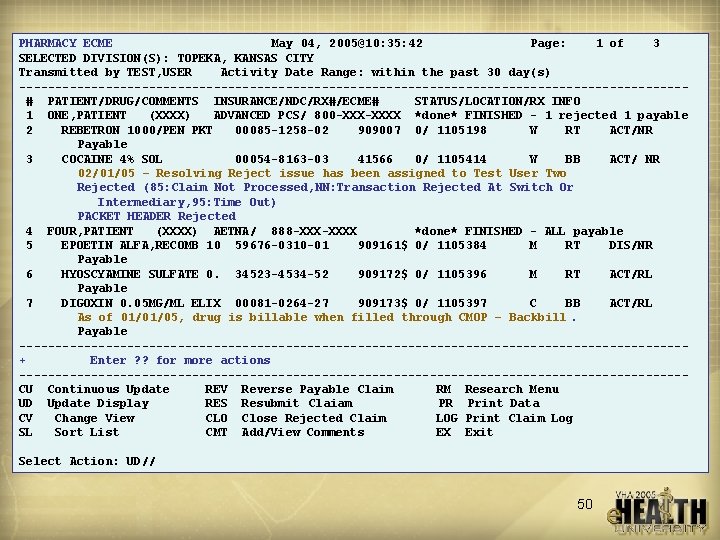
PHARMACY ECME May 04, 2005@10: 35: 42 Page: 1 of 3 SELECTED DIVISION(S): TOPEKA, KANSAS CITY Transmitted by TEST, USER Activity Date Range: within the past 30 day(s) ----------------------------------------------# PATIENT/DRUG/COMMENTS INSURANCE/NDC/RX#/ECME# STATUS/LOCATION/RX INFO 1 ONE, PATIENT (XXXX) ADVANCED PCS/ 800 -XXXX *done* FINISHED - 1 rejected 1 payable 2 REBETRON 1000/PEN PKT 00085 -1258 -02 909007 0/ 1105198 W RT ACT/NR Payable 3 COCAINE 4% SOL 00054 -8163 -03 41566 0/ 1105414 W BB ACT/ NR 02/01/05 – Resolving Reject issue has been assigned to Test User Two Rejected (85: Claim Not Processed, NN: Transaction Rejected At Switch Or Intermediary, 95: Time Out) PACKET HEADER Rejected 4 FOUR, PATIENT (XXXX) AETNA/ 888 -XXXX *done* FINISHED - ALL payable 5 EPOETIN ALFA, RECOMB 10 59676 -0310 -01 909161$ 0/ 1105384 M RT DIS/NR Payable 6 HYOSCYAMINE SULFATE 0. 34523 -4534 -52 909172$ 0/ 1105396 M RT ACT/RL Payable 7 DIGOXIN 0. 05 MG/ML ELIX 00081 -0264 -27 909173$ 0/ 1105397 C BB ACT/RL As of 01/01/05, drug is billable when filled through CMOP – Backbill. Payable ----------------------------------------------+ Enter ? ? for more actions ----------------------------------------------CU Continuous Update REV Reverse Payable Claim RM Research Menu UD Update Display RES Resubmit Claiam PR Print Data CV Change View CLO Close Rejected Claim LOG Print Claim Log SL Sort List CMT Add/View Comments EX Exit Sample ECME User Screen Select Action: UD// 50

ECME Screen – shows DUR PHARMACY ECME Feb 28, 2005@13: 41: 15 Page: 1 of 1 All prescriptions for patient ECME, TEST PATIENT C With activity in the past 1 day(s) # PATIENT/PRESCRIPTION COMMENTS 1 done ECME, TEST PATIENT C ** FINISHED ** rejected ** 2 EXP IPRATROPIUM BR 0. 03% N RL MAY 11@13: 03 Rejected (88: DUR Reject Error, E 7: + Enter ? ? for more actions CU Continuous update PA Print all RES UD Display update LOG Print claim log CLO CV Change View screen RCA Request cancellation EX DIS Dismiss patient REV Reverse a paid claim Select Action: UD// >>> Resubmit a claim Close Claim(s) Exit Enter > to see more info about reject reason 51

ECME Screen – shows DUR PHARMACY ECME Feb 28, 2005@13: 41: 15 Page: 1 of 1 All prescriptions for patient ECME, TEST PATIENT C With activity in the past 1 day(s) # PATIENT/PRESCRIPTION COMMENTS 1 done ECME, TEST PATIENT C ** FINISHED ** rejected ** 2 EXP IPRATROPIUM BR 0. 03% N Reject Error): DUR Reject Error (8098066. 00061) Contacted Payer – DUR created because patient got Ipratropium at Walgreens on April 26 <<< Enter ? ? for more actions CU Continuous update PA Print all RES UD Display update LOG Print claim log CLO CV Change View screen RCA Request cancellation EX DIS Dismiss patient REV Reverse a paid claim Select Action: UD// Resubmit a claim Close Claim(s) Exit 52

ECME Screen –Reject 76 PHARMACY ECME Feb 28, 2005@13: 41: 15 Page: 1 of 1 All prescriptions for patient ECME, TEST PATIENT D With activity in the past 1 day(s) # PATIENT/PRESCRIPTION COMMENTS 1 done ECME, TEST PATIENT D ** FINISHED ** rejected ** 2 ACT FELODIPINE 5 MG SA TAB RL APR 25@14: 26 Rejected(76: Plan Limitations Exc: Enter ? ? for more actions CU Continuous update PA Print all RES UD Display update LOG Print claim log CLO CV Change View screen RCA Request cancellation EX DIS Dismiss patient REV Reverse a paid claim Select Action: UD// >>> Resubmit a claim Close Claim(s) Exit Plan Limitation Reject 53

ECME Screen –Reject 76 PHARMACY ECME Feb 28, 2005@13: 41: 15 Page: 1 of 1 All prescriptions for patient ECME, TEST PATIENT F With activity in the past 1 day(s) # PATIENT/PRESCRIPTION COMMENTS 1 done ECME, TEST PATIENT F ** FINISHED ** rejected ** 2 ACT FELODIPINE 5 MG SA TAB please notify patient; 30 is max days - call 800 Enter ? ? for more actions CU Continuous update PA Print all RES UD Display update LOG Print claim log CLO CV Change View screen RCA Request cancellation EX DIS Dismiss patient REV Reverse a paid claim Select Action: UD// >>> Resubmit a claim Close Claim(s) Exit CBO negotiating with Payers to pay VA for 90 -day fills. 54

Top 10 ECME Rejects 1. Plan Limitation Exceeded (90 DAY) - 54% 2. Non-Matched Product (NDC) – 12% 3. Claim Too Old – 9% 4. Non-Matched Cardholder – 8% 5. Refill Too Soon – 4% 6. Product/Service Not Covered (NDC) 4% 7. Transmission Stopped – 3% 8. M/I Days Supply (90 Day) – 2% 9. Pharmacy Not Contracted with Plan – 2% 10. M/I Processor Control Number – 2% 55

DAW Processing • DAW stands for Dispense as Written • Set of NCPDP codes used to inform third party why a brand or generic product was used for Rx fill • Some claims reject because we use brand name products of drugs with generics available (e. g. Coumadin®) 56

DAW Code Descriptions DAW Code 0 1 2 3 4 5 6 7 8 9 DAW Description No Product Selection Indicated Substitution Not Allowed by Prescriber Substitution Allowed-Patient Requested Product Dispensed Substitution Allowed-Pharmacist Selected Product Dispensed Substitution Allowed-Generic Drug Not in Stock Substitution Allowed-Brand Drug Dispensed as a Generic Override Substitution Not Allowed-Brand Drug Mandated by Law Substitution Allowed-Generic Drug Not Available in Marketplace Other 57

DAW Processing (cont. ) • Using correct DAW code may be crucial to getting payable claim • Will have the ability to change DAW through patient prescription processing etc. • The default value used will be 0 • Not many rejects for this during Beta test 58
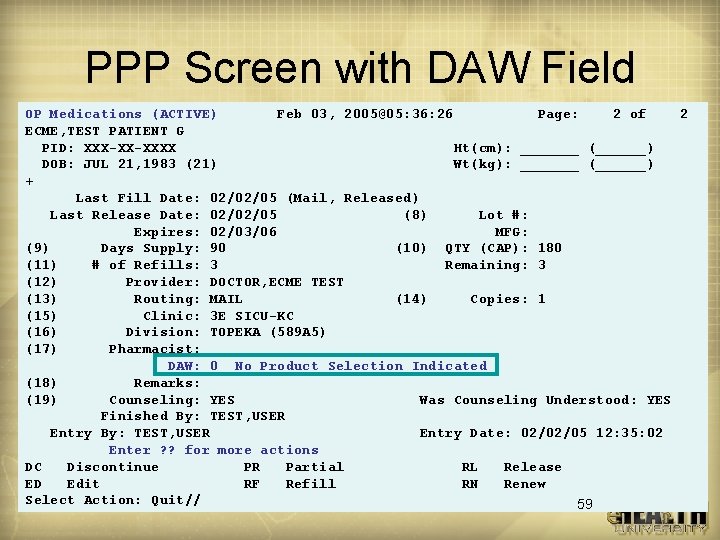
PPP Screen with DAW Field OP Medications (ACTIVE) Feb 03, 2005@05: 36: 26 Page: 2 of 2 ECME, TEST PATIENT G PID: XXX-XX-XXXX Ht(cm): _______ (______) DOB: JUL 21, 1983 (21) Wt(kg): _______ (______) + Last Fill Date: 02/02/05 (Mail, Released) Last Release Date: 02/02/05 (8) Lot #: Expires: 02/03/06 MFG: (9) Days Supply: 90 (10) QTY (CAP): 180 (11) # of Refills: 3 Remaining: 3 (12) Provider: DOCTOR, ECME TEST (13) Routing: MAIL (14) Copies: 1 (15) Clinic: 3 E SICU-KC (16) Division: TOPEKA (589 A 5) (17) Pharmacist: DAW: 0 No Product Selection Indicated (18) Remarks: (19) Counseling: YES Was Counseling Understood: YES Finished By: TEST, USER Entry Date: 02/02/05 12: 35: 02 Enter ? ? for more actions DC Discontinue PR Partial RL Release ED Edit RF Refill RN Renew Select Action: Quit// 59

Claims Processing – OPECC • OPECC stands for Outpatient Pharmacy Electronic Claims Coordinator • Each site is to have one and most likely will come from billing operations • Coordinates all the third party Rx claims processing • Handles the bulk of the rejection resolution • Will need to interact and consult with Pharmacy staff 60

Non-Pharmacy Functions • Updating patient insurance information • BIN/PCN matching • Following-up non-DUR/Refill Too Soon or DAW claim rejections • Exceptions will be if Pharmacy needs to assist the OPECC in determining NDC used, prior authorizations, etc. • New background job checks for payable Rxs not released within site-defined time period – initiates an automatic claims reversal • Includes Local & CMOP Rx’s 61

Challenges to Address • • CBO is working with payers to accept 90 fills NDC format – must be 11 -digits Repackaged Drugs – NDC not valid Dispensing units a problem* – For example third parties want insulin quantities expressed in ml and inhalers in gms – We use a unit of ‘each’ • Billing Tricare and Champ. VA* – These claims use a cost plus fee billing structure – Will probably not fill if not paid *Software solution apportioned to the next iteration 62

Challenges to Address (cont. ) • Other functionality apportioned to the next iteration – – Prior Authorizations Billing for Compounds Barcode scanning of product during manual fill Billing Patients Secondary and Tertiary Insurance Companies – Billing for Partial Fills – Sensitive Diagnosis and ROI Issue 63

Pharmacy Lessons Learned • Mark billable OTCs • Use Drug Accountability to build/maintain NDC entries • Important for Billing and Insurance people to – do the BIN and PCN matching to the Insurance groups – update patient insurance and cardholder information • Release Rxs in a timely manner – impact on copay and third party claims • Instruct filling techs about label changes and have them alert releasing RPh to third party Rx 64

Added Benefits, Other Factors • Increase Revenue • NDC on laser label can be used as a product checker when manually filling • System provides potentially valuable clinical information on drug interactions, allergies, and overuse/misuse of medications • Positions us for a larger role in health benefit plans in future • There will be education directed at Pharmacy users in the upcoming months – There will be other training provided to users through PBM, Employee Education System and OI National Training and Education Office • CBO is following up overall assessment of revenue collection and have a prototype report in final testing at this time 65

References • HSD&D Project web site – HIPAA NCPDP Connection for EDI Pharmacy (e. Pharmacy) Software Requirement Specifications (SRS) Iteration III Version 1. 0 March 2005 – http: //tspr. vista. med. va. gov/warboard/anotebk. asp? proj=698&Type=Active • e-Pharmacy Claims on Vist. A University – http: //vaww. vistau. med. va. gov/Vista. U/e-bp/e-pharmacy. htm 66

Questions 67

Thank You 68
- Slides: 68