Eosinophilic Pneumonia Eosinophilic Pneumonia Or ChurgStrauss Syndrome Case


































- Slides: 45

Eosinophilic Pneumonia

Eosinophilic Pneumonia Or Churg-Strauss Syndrome?

Case Report- J. N. , 40 WF • Admitted 9/19/03 – 9/24/03 for fever, congestion, dyspnea, chest tightness, abdominal cramps, and diarrhea • Extensive PMH Asthma since age 17 Immunotherapy Prednisone use since age 20 Hx nasal polyp surgery Hx IVIG for Hypogammaglobulinemia Osteoporosis

Initial Laboratory Eval • • • CXR, later CT scan – Dr. Hamilton Hgb 14. 9 Hct 44. 5 Platelets 412 K WBC 19. 5 Neutrophils 62% Eosinophils 31% • ESR 50

Additional Laboratory Data • • BNP 309 • TSH 1. 16 • INR 1. 2 • Ig. A 243 (69 -309) • Ig. E 711 (0 -180) • Ig. G 1450 (613 -1295) • Ig. M 207 (53 -334) • • Ig. G sub 1 597 (240 -1118) Ig. G sub 2 537 (124 -549) Ig. G sub 3 32 (21 -134) Ig. G sub 4 609 (7 -89) ANA <1: 40 RA negative Crypto Ag negative Histoplasma Ag negative

More Laboratory Data • Neutrophil Cytoplasmic • Bronchoscopy Data AB <1: 16 AFB neg Blood cultures neg Routine cult neg Legionella Neg(urine) Fungus-yeast, - crypto Strept. Pneumo neg(urine) Stool parasites neg Biopsy – Dr. O’Dell Fungal Serology neg

Hospital Course • Rx – O 2, albuterol, ipratropium, Cefepime, Azithromycin, Bactrim, Solu. Medrol Bronchoscopy 9/22 – bronchitis, mucous Home on Prednisone 20 mg. BID

Later Outpatient Data • • • WBC (on 10/2) 10. 4 with 1% Eos P-ANCA neg C_ANCA neg Anti-myeloperoxidase neg Anti-proteinase neg Atypical ANCA neg

Pulmonary Eosinophilia - Causes • • • Drug and Toxin Induced Helminthic and Fungal Infection Acute Eosinophilic Pneumonia Chronic Eosinophilic Pneumonia Churg – Strauss Syndrome Others

Drug and Toxin Induced Eosinophilic Lung Disease • Nitrofurantoin, Ampicillin, NSAIDs, Pentamidine. • Phenytoin, L-Tryptophan, Ranitidine, Trazadone • Metals, Scorpion stings, Heroin, Cocaine, Dust, Smoke, Scotchguard, Sulfite exposure, Organic chemicals

Helminthic/Fungal Infection related • Transpulmonary larvae migration-Loffler’s Ascaris lumbricoides Hookworm Strongyloides stercoralis • Pulmonary Parenchymal Invasion Helminths, e. g. Paragonimiasis • Heavy hematogenous seeding-Trichinosis, Strongyloidiasis, Schistosomiasis, Cutaneous and visceral larva migrans

Helminthic/Fungal Infection related • Tropical Pulmonary Eosinophilia Wuchereria bancrofti Brugia malayi Allergic Broncho-Pulmonary Aspergillosis

Acute Eosinophilic Pneumonia • Acute, febrile, hypoxic, RF often, mechanical ventilation • Bx - DAD, hyaline membranes • Blood eosinophilia absent • HIV often

Chronic Eosinophilic Pneumonia • Subacute, cough, fever, dyspnea, wheeze, sweats • Asthma precedes/accompanies in 50% • CXR –”photographic negative” of CHF in less than 1/3. Occasional pleural effusion, cavitations • Bx - Giant cells, BOOP often

Churg – Strauss Syndrome Allergic granulomatosis and angiitis • • • Vasculitis Sinusitis, asthma, blood eosinophilia Lung, skin, cardiovascular, GI, nervous Patchy opacities Bx-eosinophilic infiltrates, eosinophilic vasculitis, necrotizing granulomas, and necrosis

Allergic Broncho-Pulmonary Aspergillosis Come back January 14, 2004

Other Causes of Pulmonary Eosinophilia • • Idiopathic Hypereosinophilic Syndrome Idiopathic Lung Diseases Neoplasms Nonhelminthic Infections – Cocci and rarely Tuberculosis

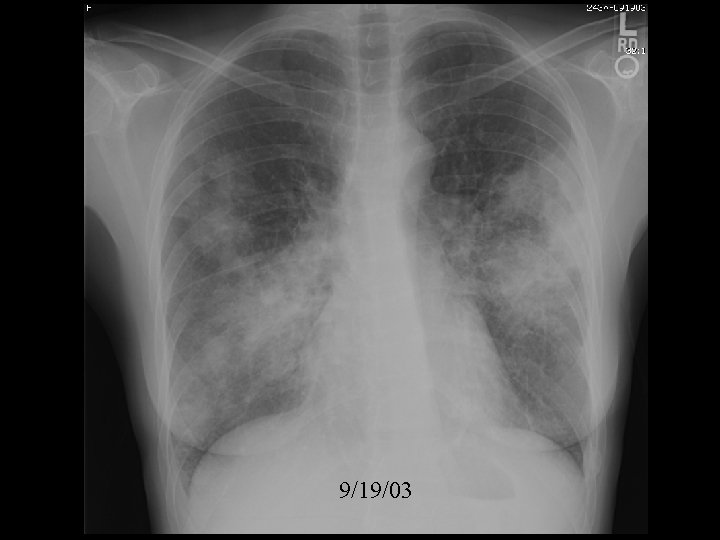
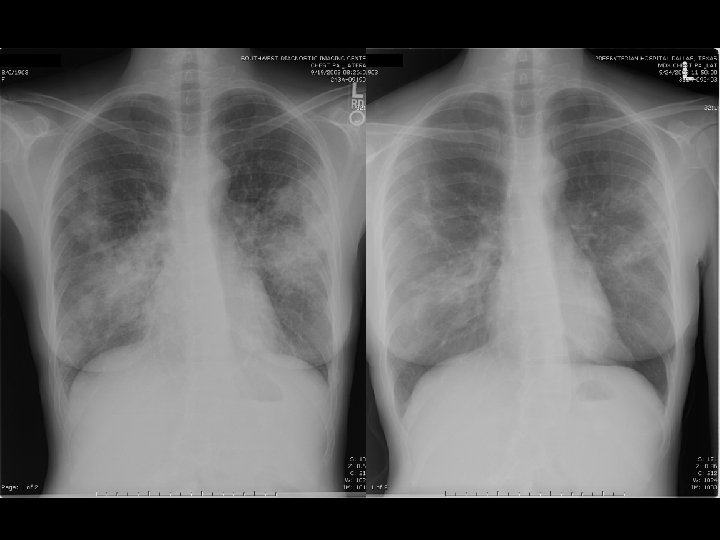
9/19/03

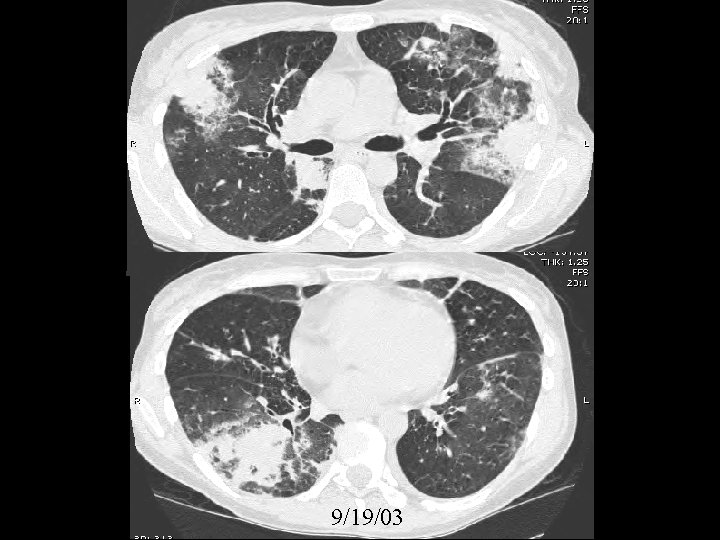
9/19/03

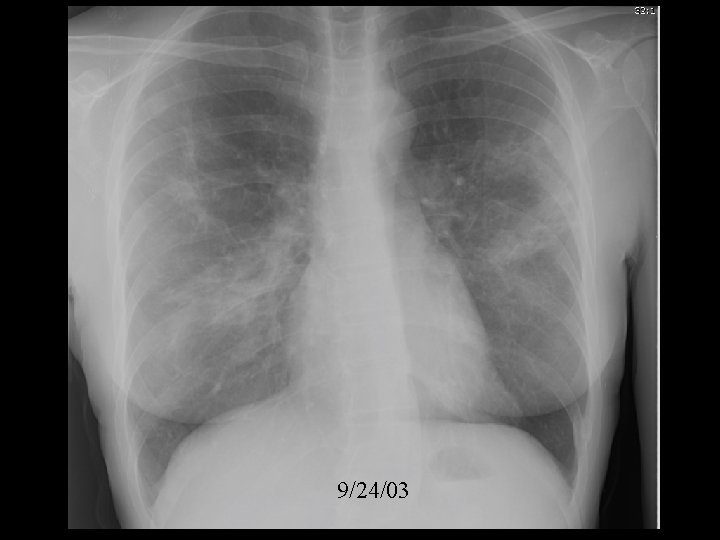
9/24/03


Differential diagnosis for peripheral, bilateral airspace disease • • Eosinophilic pneumonia BOOP BAC Sarcoid






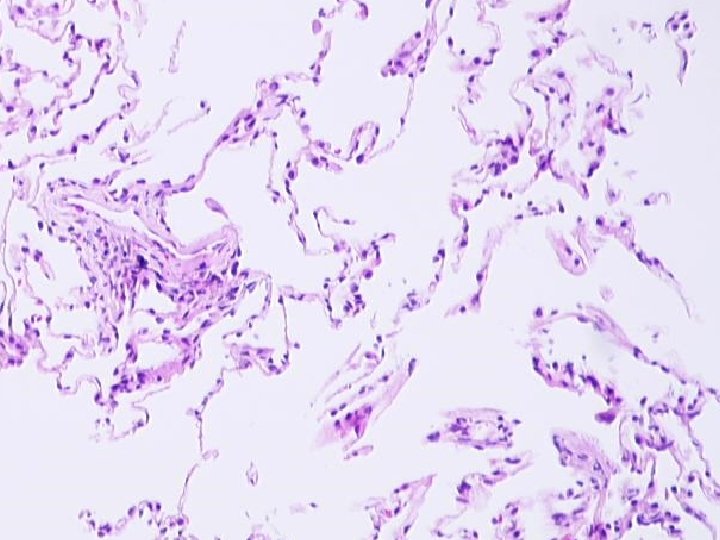
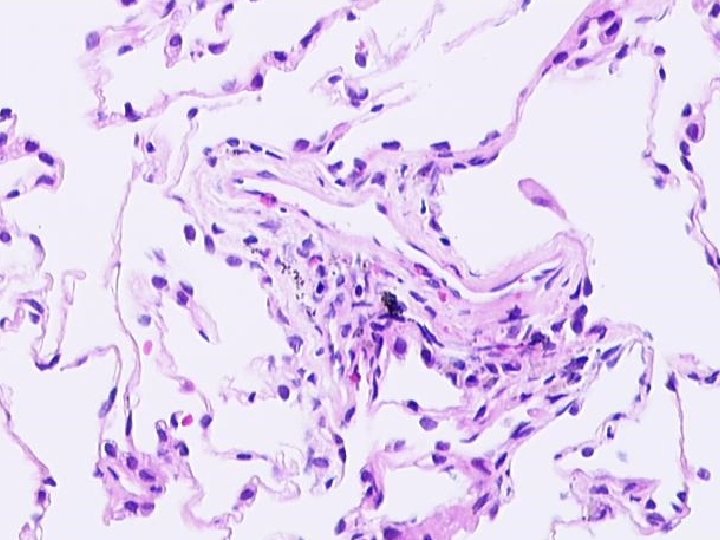
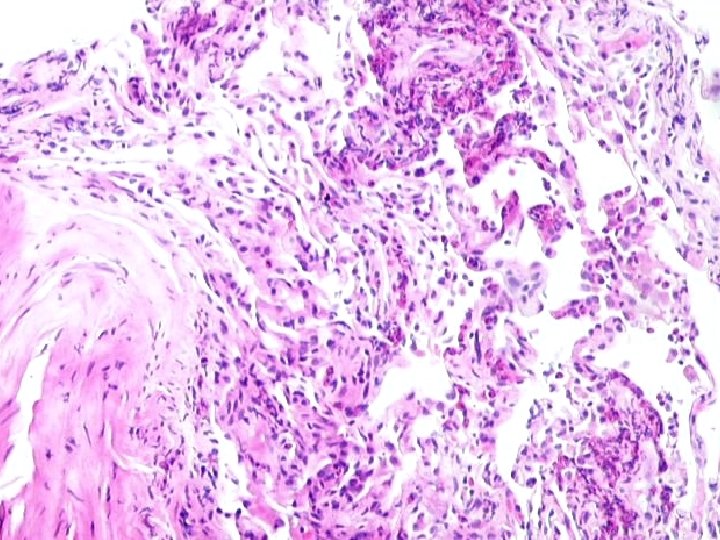
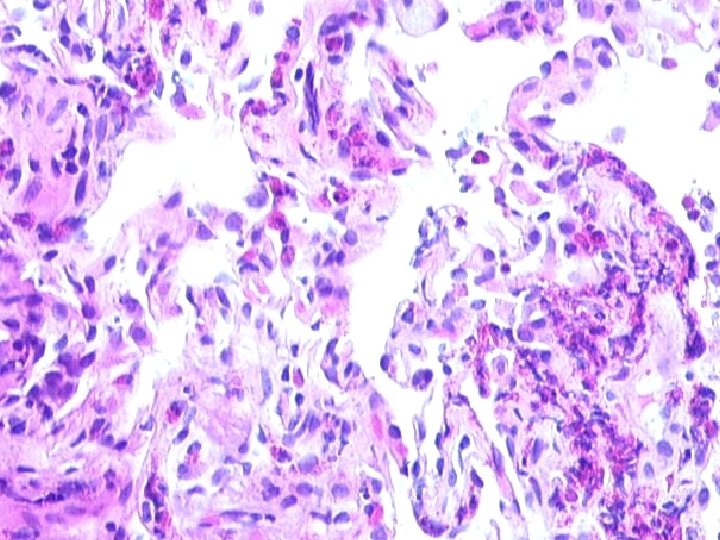
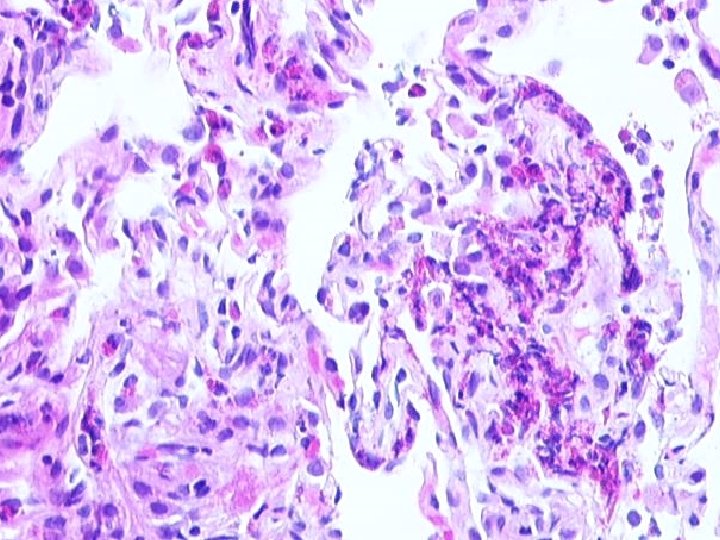
Eosinophilic Pneumonia • Eosinophils in alveolar spaces and/or interstitium • Variable: organizing pneumonia alveolar macrophages granulomas mild vascular inflammation

Etiology Idiopathic – – Chronic eosinophilic pneumonia Acute eosinophilic pneumonia Simple eosinophilic pneumonia (Loeffler’s) Incidental eosinophilic pneumonia

Etiology Secondary Eosinophilic Pneumonia – Infection: parasites, fungi – Drugs – Immunologic: asthma, allergic bronchopulmonary fungal disease, collagen vascular disease, Churg-Strauss syndrome – Systemic: HIV, malignancy, idiopathic hypereosinophilia syndrome

Significant Histologic Findings • • • Vasculitis: Churg-Strauss syndrome drug toxicity Asthmatic bronchitis: asthma chronic eosinophilic pneumonia allergic bronchopulmonary fungal disease Infectious agents: fungus parasites

Dr. Brodsky’s Presentation

CHURG-STRAUSS SYNDROME (ALLERGIC GRANULOMATOSIS AND ANGITIS) MULTI SYSTEM DISORDER n Allergic Rhinitis n Asthma n Peripheral Blood Eosinophilia n Lung involvement most common followed by skin n Cardiovascular, GI, CNS

CHURG-STRAUSS SYNDROME Approximately 10% of systemic vasculitis patients. n No gender predominance n Median age – 50, but may appear in late 30’s n Uncommon after 65 n

CHURG-STRAUSS SYNDROME ETIOLOGY n n n n Autoimmune Disorder Allergic Features Heightened T Cell Immunity (Pulmonary angiocentric granulomatosis) Altered humoral immunity (Hyperglobulinemia, Ig. E, RF) Immune Complexes (vasculitis, IC’s, P ANCA) Rare complication with leukotriene receptor antogonists Rare complication with free based cocaine

CHURG-STRAUSS SYNDOME CLINICAL FEATURES Prodromal Phase-Second and Third decadesatopic disease, allergic rhinitis, asthma n Eosinopilic Phase-Eosinophilia, infiltration of multiple organs-lung, GI tract. n Vasculitic Phase-Third and Fourth Decades-life threatening systemic vasculitis medium and small vessels. Constitutional complaints n

CHURG-STRAUSS SYNDROME CLINICAL FEATURES Asthma-precedes vasculitis by 8 -10 years: Usually chronic, severe, steroid dependent. n Nasal and Sinus Disease: nasal obstruction, recurrent sinusitis, nasal polyposis, chronic otitis n Skin disease-sub Q nodules extensor surfaces, hands, legs. Palpable purpura, nodules (67%) n Cardiovascular Disease-pericarditis, CHF, MI’s (50% of deaths) n

CHURG-STRAUSS SYNDROME CLINICAL FEATURES Neurologic Disease-peripheral neuropathy mononeuritis multiplex, strokes (75%) n Renal Disease-focal segmental GN with crescents, necrosis, P ANCA (80%) n GI Disease-Abdominal pain, diarrhea, GI Bleeding, Colitis (59%) n Muscoloskeletol disease-Myalgias, migiatory polyarthralgias, arthritis (uncommon) n

CHURG-STRAUSS SYNDROME LABORATORY FEATURES n n n n n Eosinophilia – 5, 000 -9, 000 NC/NC Anemia ESR Ig. E Circulating Immune Complexes Hyperglobulinemia +RF P ANCA IL 2 R BAL – 33% Eos

CHURG-STRAUSS SYNDROME RADIOGRAPHIC FEATURES n n n n Transient patchy opcacities (75%) without lobar or segmental distribution Axillary, peripheral distribution Diffuse Interstitial/Miliary pattern Pulmonary Hemorrhage Nodular Disease Pleural effusions (exudative, Eos) (30%) Pulmonary arteries enlarged, vasculitis sign

CHURG-STRAUSS SYNDROME PATHOLOGY n n n Eosinophilic Infiltrates Extensive Necrosis Eosinophilic Giant Cell Vasculitis, small arteries and veins Interstitial and perivascular granulomas Eosinophilic Lymphadenopathy

CHURG-STRAUSS SYNDROME TREATMENT n n n Corticosteroids: 0. 5 to 1. 5 mg/kg for 6 -12 wks Monitor ESR, EOS, CXR Late relapses uncommon; 70% 5 yr survival Inhaled Steroids CTX, AZA, IVIG Poorer Prognosis: Cardiac Failure or MI, Cerebral hemorrhage, Renal Failure, GI bleed

CHURG-STRAUSS SYNDROME ACR CLASSIFICATION CRITERIA n n n Asthma Eosinophilia – 10% or greater Mononeuritis multiplex or polyneuropathy Migratory or transient pulmonary opacities Paranasal sinus abnormalities Bx evidence of eosinophilic vasculitis/tissue eosinophils

ACUTE EOSINOPHILIC PNEUMONIA n n n Acute febrile illness of short duration Hypoxemic Respiratory Failure Diffuse pulmonary opacities on CXR BAL Eosinophilia >25% Lung Bx – eosinophilic infiltrates (Acute and/or organizing DAD/eosinophils) Dx of exclusion (Drugs, Infections, Asthma, Atopic Disease)

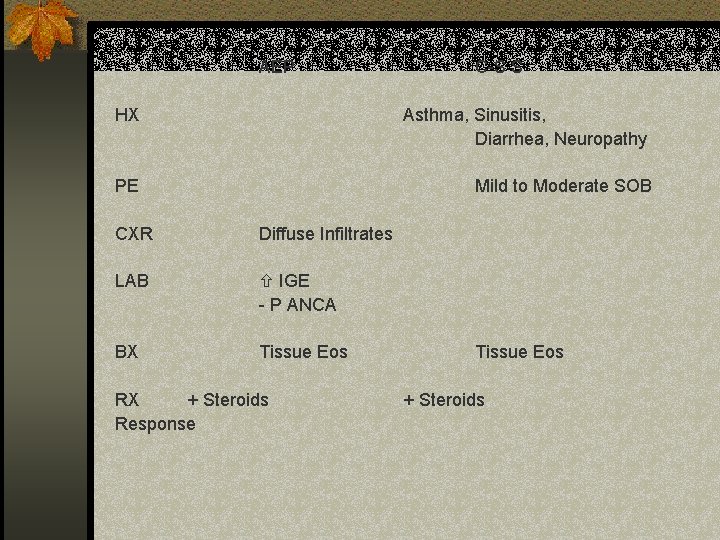
AEP C-S S HX Asthma, Sinusitis, Diarrhea, Neuropathy PE Mild to Moderate SOB CXR Diffuse Infiltrates LAB IGE - P ANCA BX Tissue Eos RX + Steroids Response Tissue Eos + Steroids