Enterocutaneous Fistula Symposium organized by the Committee on

Enterocutaneous Fistula Symposium organized by the Committee on Critical Care and Nutrition (2017) Philippine College of Surgeons

Objectives • To discuss the concept of intestinal failure/insufficiency • To discuss pathophysiology of different types of intestinal failure/insufficiency with focus on enterocutaneous fistula • To discuss management approaches to intestinal failure/insufficiency focusing on enterocutaneous fistulas

Intestinal failure or insufficiency • “Intestinal failure” - reduction in gut function below the minimum necessary for the absorption of macronutrients and/or water and electrolytes such that intravenous supplementation is required to maintain health and/or growth 1 • “Intestinal insufficiency or deficiency” - a reduction of absorptive function that does not require intravenous supplementation to maintain health and/or growth 2 1. Pironi L et al. ESPEN position paper. Definition and classification of intestinal failure in adults. Clin Nutr 2015. 2. O’Keefe SJD et al. Short bowel syndrome and intestinal failure: consensus definitions and overview. Clin Gastroentrol Hepatol 2006; 4: 6 -10
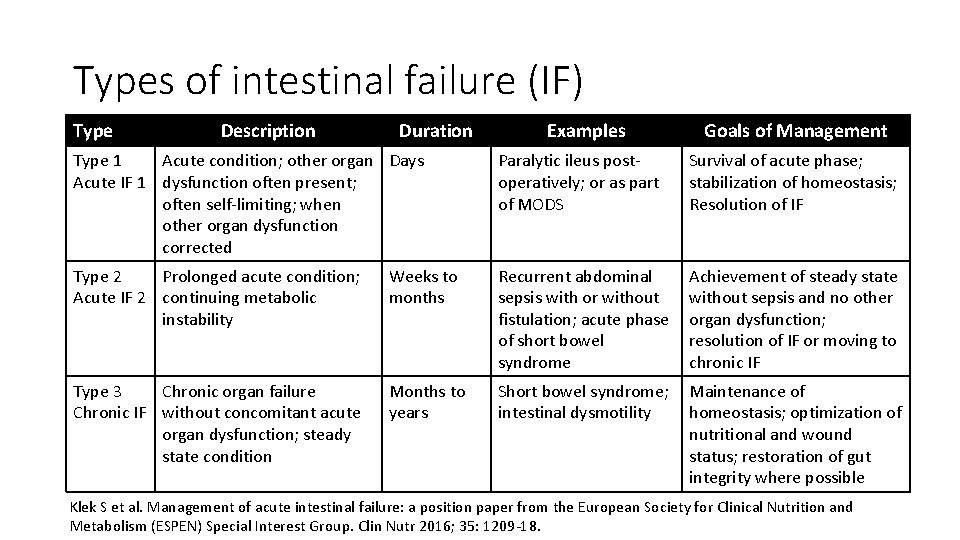
Types of intestinal failure (IF) Type Description Duration Examples Goals of Management Type 1 Acute condition; other organ Days Acute IF 1 dysfunction often present; often self-limiting; when other organ dysfunction corrected Paralytic ileus postoperatively; or as part of MODS Survival of acute phase; stabilization of homeostasis; Resolution of IF Type 2 Prolonged acute condition; Acute IF 2 continuing metabolic instability Weeks to months Recurrent abdominal sepsis with or without fistulation; acute phase of short bowel syndrome Achievement of steady state without sepsis and no other organ dysfunction; resolution of IF or moving to chronic IF Type 3 Chronic organ failure Chronic IF without concomitant acute organ dysfunction; steady state condition Months to years Short bowel syndrome; intestinal dysmotility Maintenance of homeostasis; optimization of nutritional and wound status; restoration of gut integrity where possible Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18.

Type 2 intestinal failure (IF) • Uncommon clinical condition accompanied by septic, metabolic and complex nutritional complications • Causes: • Consequence of trauma following an acute intestinal event necessitating massive enterectomy: • Intestinal volvulus • Strangulated hernia • Mesenteric thrombosis • Abdominal trauma • Complication of intestinal surgery often in a setting of considerable pre-existing co-morbidity: • Anastomotic leak • Unrecognized intestinal injury • Fistula formation • Abdominal wall dehiscence • Laparostomy/open abdomen Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18.

Type 2 intestinal failure (IF) • Causes (from British group): 1 • • 32% - surgical complications 21% - Crohn’s disease 14% - motility disorders 13% - vascular ischemia 8% - malignancy 2% - radiation injury 2% - celiac disease 8% - others • Annual incidence: 9 for every 1 million population 2 • In-hospital mortality: 9. 6 -13% 2 • Needs: 2 • Specialized IF units • Intensive care units with the capacity for multi-disciplinary IF team care 1. Lal S et al. Review article: intestinal failure. Aliment Pharmacol Ther 2006; 24: 19 -31. 2. Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18.

Enterocutaneous fistula • Types: • Low output: < 200 ml/day • Moderate output: 200 -500 ml/day • High output: > 500 ml/day Harris H. Lecture: Management of enterocutaneous fistula – ppt lecture. http: //www. ucsfcme. com/2011/slides/MSU 11001/16 Harris. Enterocutaneous. Fistulas. pdf

The SOWATS regimen for enterocutaneous fistula or temporary enterostomy • S – sepsis control • O – optimization of hydration and nutritional status • W – wound care • A – anatomy of the bowel and the fistula • T – timing of surgery • S – surgical planning Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18.

Sepsis control • Sepsis • leading cause of death in AIF • originates from the abdominal cavity • Immediate removal of source and/or adequate drainage mandatory • Severe sepsis • Clinical presentations of severe sepsis when no obvious source can be found due to poor nutritional status or the disease itself: • Tachcardia, fatigue, encephalopathy, fluid retention and edema, jaundice or signs of new or worsening organ failure • Laboratory: • Leucopenia or leukocytosis, isolated lymphopenia, low hemoglobin, reduced plasma albumin or transferrin levels, abnormal liver function tests Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18.

Sepsis control • Targeted antimicrobial therapy based on culture results is sufficient in only a minority of patients • It is imperative to identify and treat the cause of sepsis: • Drainage of abdominal abscess (percutaneous or open) • Consider non-abdominal cause of sepsis: • Pneumonia is the most common cause • CVP line is also a common cause • Secondary fungal infection secondary to prolonged sepsis and exposure to antibiotics (no probiotics*) Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18. * me


Optimizing hydration and nutritional status • During the initial phase • Directed towards achieving hemodynamic stability with fluid and electrolyte replacement • Thereafter, controlling fluid losses and covering energy needs are the main tasks • Fluid management • Fluid resuscitation should be done first before nutrition can be given • Know the intraoperative fluid balance (Positive fluid accumulation? ) • Accumulated fluid balance should be done daily – a decreasing value is good, increasing? – very bad • Use a balanced electrolyte solution, not dextrose containing for your maintenance fluids not unless there are electrolyte abnormalities that need to be corrected

Optimizing hydration and nutritional status • Fluid flux in the small intestines = 6 -8 liters daily • 80% absorbed in the jejunum and ileum > only 150 ml enter the colon • The colon can reabsorb 5 liters of water in 24 h • For massive intestinal resection • Intestinal loss of water is inversely proportional to the length of remnant bowel > gets worse when there is concomitant partial or total colon resection • End-jejunostomy or proximal ileostomy develop dehydration and electrolyte abnormalities (mainly magnesium, potassium or sodium) • Ileal resection results to greater losses compared to jejunum due to massive diarrhea secondary to the effect of bile salts and steatorrhea Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18.

Absorption of micronutrients Adapted from: Sriram K. Micronutrients: lecture in ppt.

Optimizing hydration and nutritional status • The magnitude of the intestinal losses is greatest in the early period after resection and may be aggravated by concomitant factors like sepsis and intestinal dysmotility • Fluids should be infused to cover all losses and to maintain a urine output of 25 ml/hr. • Sometimes go beyond 30 -40 ml/kg/day • Strict fluid balance monitoring is required (avoid positive accumulated fluid balance of more than 75% of the interstitial fluid volume or should not go beyond 9% of the actual/ideal body weight) • interstitial fluid volume = 12% of actual/ideal body weight; value is in liters • Electrolyte losses should be strictly monitored with accompanying serum electrolyte monitoring

Optimizing hydration and nutritional status • Nutritional requirements • 30 kcal/kg/day (ideal body weight) • 1. 5 - 2. 0 g/kg/day protein • Complete vitamin and trace elements daily • Avoid refeeding • Route and suggested macro and micronutrient supplementation: • Oral intake will always be insufficient • Enteral feeding to as much as the bowel is capable • Supplemental parenteral nutrition when enteral nutrition cannot provide minimum of 60% computed requirements • If there is good financial status: provide glutamine, fish oil, anti-oxidants, arginine

Optimizing hydration and nutritional status • Distal feeding • Exercises negative feedback on bilio-pancreatic secretions or ”ileal brake” > helps reduce diarrhea and/or losses of nutrients and electrolytes 1, 2 • Fistuloclysis or chyme reinfusion • Fistuloclysis – infusion of enteral formulas or effluents (from the fistula) which are reinfused back to the bowels • Reduces the need for increased volumes of either enteral or parenteral nutrition 1. Visschers RGJ et al. Treatment strategies in 135 consecutive patients with enterocutaneous fistulas. World J Surg 2008; 32: 445 -53. 2. Van Citters GW et al. Ileal brake: neuropeptidergic control of intestinal transit. Curr Gastroenterol Rep 2006; 8(5): 367 -73.

Wound care • Crucial in the treatment of AIF: • • Wound care Stoma care Skin care Collection of intestinal output and wound discharge • Ideally needs a team (physician, nurse, stoma care specialist) • Additional techniques: • Suction drain • Planned cleaning • Nutritionals that hasten wound healing: glutamine-HMB-arginine combination, omega-3 -fattys acids + glutamine combinations (hasten the resolution process)* Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18. * me

Other supportive measures • Protocols should be developed for the following: • Oral care • Catheter care • Mobilization • Implementing the FAST-HUG concept (will be discussed in a separate lecture)

Surgical approaches (ATS component) • Drainage of intra-abdominal abscess • Antimicrobials should always accompany surgery • When a small bowel is opened do not attempt anastomosis when there is peritonitis (exteriorize both ends) • Early surgery should be limited only to sepsis control • Reconstructive surgery may be done only after weeks or months or when patients have gone into the chronic IF stage • To correct nutritional deficiencies • To have optimal wound healing Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18.

Intestinal failure associated liver disease (IFALD) • Shown by abnormal liver function test which are usually mild and normalize after the initiation of enteral feeding, even if PN is continued • Causes: • PN related (overfeeding, type of PN – higher glucose content + omega-6 -FA lipids alone) • IF related (SBS or Short Bowel Syndrome, oral fasting, bacterial overgrowth, disruption of the enterohepatic cycle, drugs especially antibiotics) • Systemic and/or abdominal inflammation related (sepsis or intra-abdominal infections) Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18.

Intestinal failure associated liver disease (IFALD) • Management: • Treatment of non-nutritional causes (e. g. gallbladder stones or sepsis) • Optimization of parenteral nutrition (using the newer PN formulas with MCT, omega-3 -FA, olive oil combinations and lower glucose contents) • Reinstatement of oral or enteral intake when not contraindicated • Chyme reinfusion at the distal end • May need to give these: • Pharmacological treatment like ursodeoycholic acid, choline and taurine • Or if worse gets to worst – intestinal with or without liver transplantation Klek S et al. Management of acute intestinal failure: a position paper from the European Society for Clinical Nutrition and Metabolism (ESPEN) Special Interest Group. Clin Nutr 2016; 35: 1209 -18.

Thank You
- Slides: 23