Enterobius vermicularis Taxonomical position Phylum Class Order Super
Enterobius vermicularis

Taxonomical position • • Phylum : Class : Order : Super family : Family : Genus : Species : Nematoda Secernentea Oxyurida Oxyuroidea Oxyuridae Enterobius vermicularis

Common names: • Pin worm • Thread worm • Seat worm History: • ‘Leukart’ – first described the complete life cycle in 1865

Distribution: • Cosmopolitan • More common in temperate and cold climate than warm climate Habitat: LARGE INTESTINE - Caecum - Appendix - Ascending colon

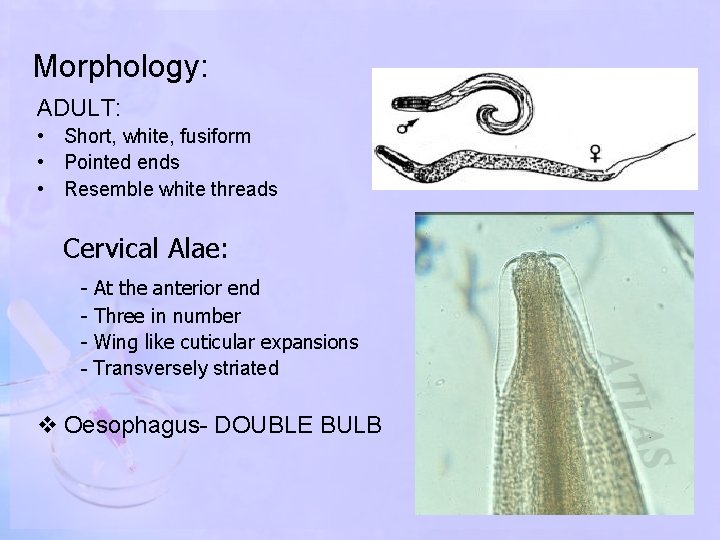
Morphology: ADULT: • Short, white, fusiform • Pointed ends • Resemble white threads Cervical Alae: - At the anterior end - Three in number - Wing like cuticular expansions - Transversely striated v Oesophagus- DOUBLE BULB
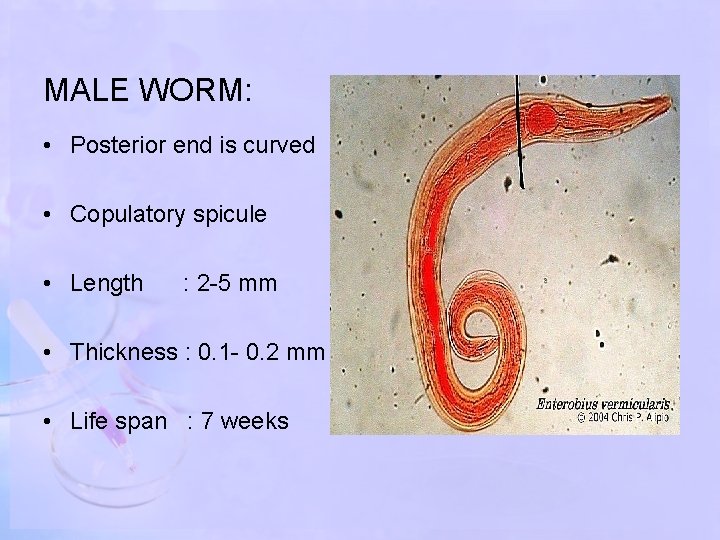
MALE WORM: • Posterior end is curved • Copulatory spicule • Length : 2 -5 mm • Thickness : 0. 1 - 0. 2 mm • Life span : 7 weeks

FEMALE WORM: • Thin, pointed, pin like tail • Reproductive organs - T shaped - paired ü OVIPAROUS • Length : 8 - 13 mm • Thickness: 0. 3 - 0. 5 mm • Life span : 5 - 13 weeks

EGG: • Colourless, non-bile stained • Shape: Planoconvex • Shell : Double layered Transparent • Sticky outer albuminous layer o Contains ‘tadpole shaped’, coiled larva • Viable up to 2 weeks

LIFE CYCLE


Life cycle: • Simplest of all the intestinal worms • Host : MONOXENOUS- single host – Human • Infective form: embryonated egg • Route: Faeco-oral transmission • Eggs transform in to larvae in 5 weeks in small intestine • Larva undergo moulting in ileum and finally mature in to adult in caecum with in 15 to 30 days • Male dies after fertilization
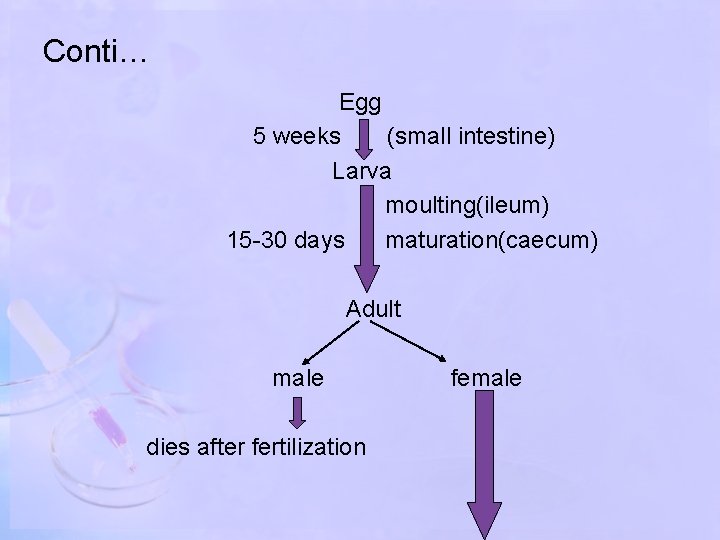
Conti… Egg 5 weeks (small intestine) Larva moulting(ileum) 15 -30 days maturation(caecum) Adult male dies after fertilization female

Conti… migrate to rectum come out through anus during night time Eggs laid on perineal, peri anal skin

Conti… Ø 1 worm = 5000 – 17000 eggs Ø Become infective in 6 hrs Ø Completes life cycle in 2 weeks – 2 months

Pathogenesis: • Adult worm: • Egg: - mucoid secretions – adherence of egg - irritation - Characteristic NOCTURNAL PERINEAL / PERIANAL ITCHING
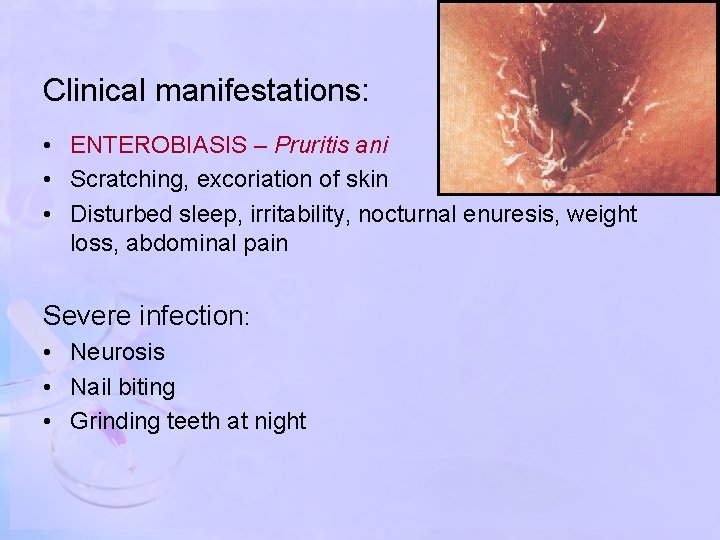
Clinical manifestations: • ENTEROBIASIS – Pruritis ani • Scratching, excoriation of skin • Disturbed sleep, irritability, nocturnal enuresis, weight loss, abdominal pain Severe infection: • Neurosis • Nail biting • Grinding teeth at night

Complications: • • • Vulvo- vaginitis Chronic salpingitis Prostatitis Urethritis Endometritis Granulomata with dead worms, eggs

Epidemiology: • Group infection: School children • Prevalent in temperate countries • USA, European countries • Source: Infected humans others like bedding, night clothing, table tops, door knobs, taps etc. , • Transmission: Auto infection contaminated articles / direct contact inhalation of eggs Retroinfection

Diagnosis: • H/O perianal pruritis LAB DIAGNOSIS: • Demonstration of Adult worm: - On the surface of stool sample - On the perianal skin - In the stool after an enema • Demonstration of Eggs: - As they are seldom excreted in faeces, stool sample is not useful for diagnosis
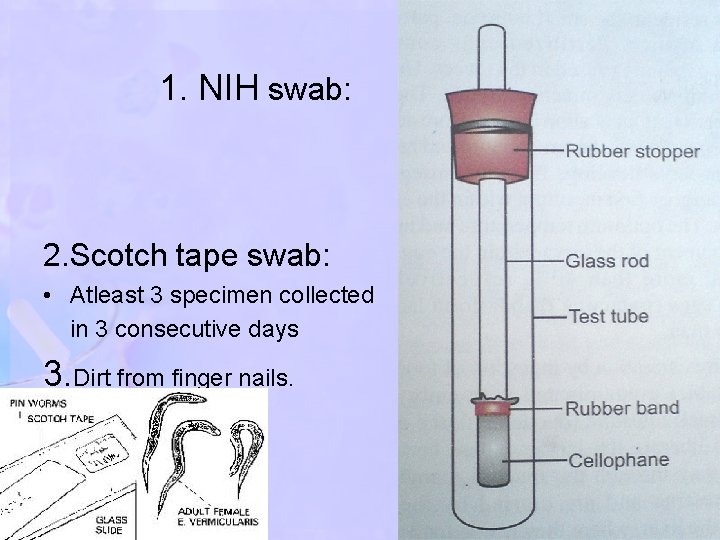
1. NIH swab: 2. Scotch tape swab: • Atleast 3 specimen collected in 3 consecutive days 3. Dirt from finger nails.
Treatment: • Single dose: Pyrantel - 11 mg/kgwt Mebendazole - 100 mg/kgwt Albendazole - 400 mg/kg wt • Piperazine - 65 mg / kg wt – 1 week • Pyrantel causes spastic paralysis of the worm

Prophylaxis: • Health education on personal hygiene • Group chemotherapy

THANK YOU
- Slides: 24