Enteric Typhoid fever Epidemic louse borne typhus Leptospirosis

Enteric (Typhoid) fever Epidemic (louse borne) typhus Leptospirosis EDYTA GRĄBCZEWSKA Nicolaus Copernicus University Ludwik Rydygier Collegium Medicum in Bydgoszcz

Enteric (Typhoid ) fever Typhus abdominalis
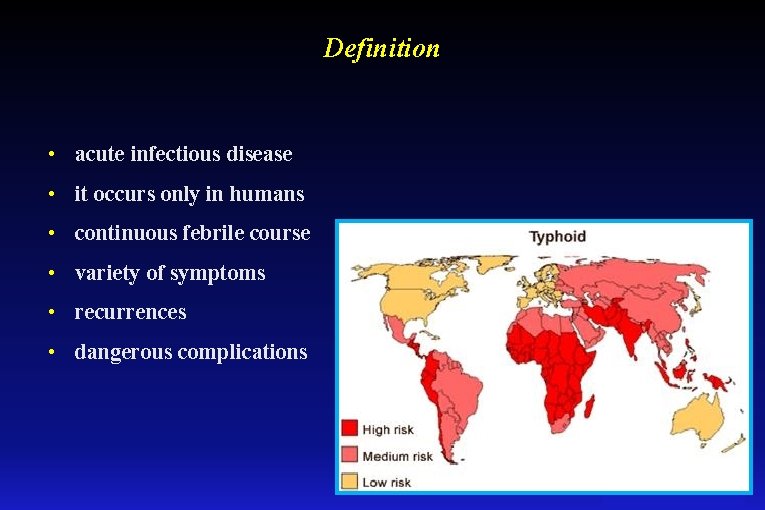
Definition • acute infectious disease • it occurs only in humans • continuous febrile course • variety of symptoms • recurrences • dangerous complications

Epidemiology worldwide occurrence 17 -22 milion cases each year leading to 200 000 -600 000 deaths • more frequently in the areas with poor public sanitation system, poor hygiene, inadequate sewage treatment • the germ reservoir and source of infection is only a human - a sick person or a asymptomatic carrier

Epidemiology • infective material: mainly feces, less frequently urine, very seldom vomits • routes of spreading: - water (extent of outbreak depends on a number of people using the source of water) - food and milk (milk forms advantageous environment for the bacteria survival) - insects (flies) mechanical transfer of typhus rods from faeces onto food - sporadic cases - direct contact with the carrier (important role in spreading) or the sick person
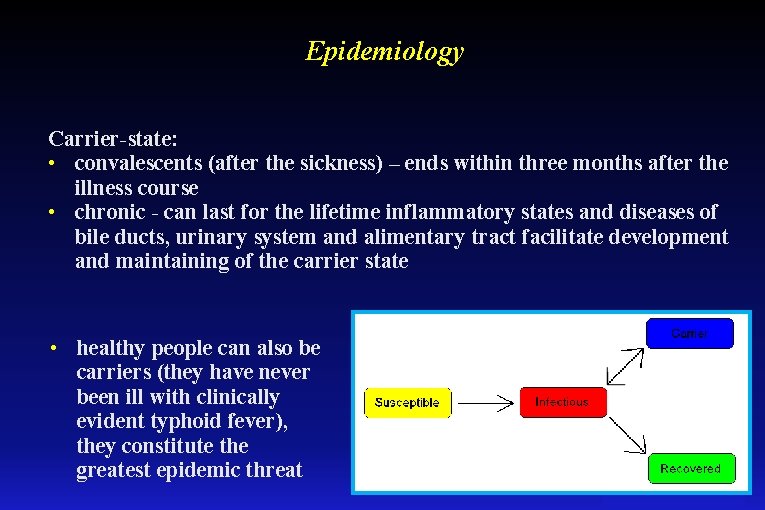
Epidemiology Carrier-state: • convalescents (after the sickness) – ends within three months after the illness course • chronic - can last for the lifetime inflammatory states and diseases of bile ducts, urinary system and alimentary tract facilitate development and maintaining of the carrier state • healthy people can also be carriers (they have never been ill with clinically evident typhoid fever), they constitute the greatest epidemic threat
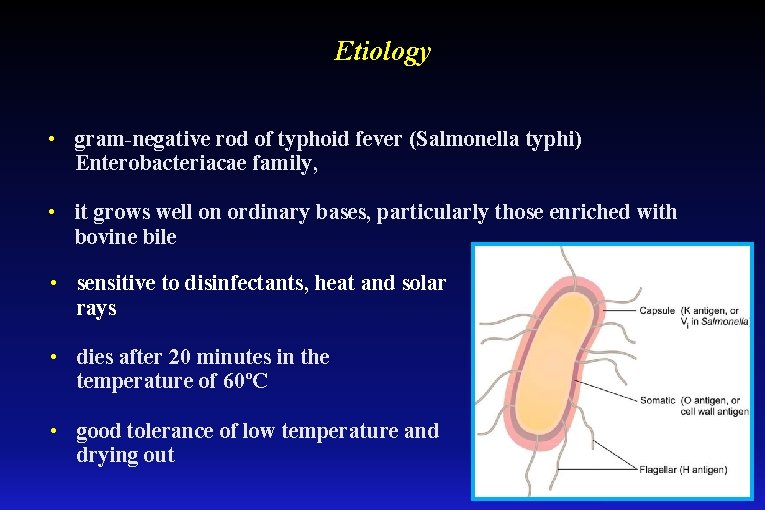
Etiology • gram-negative rod of typhoid fever (Salmonella typhi) Enterobacteriacae family, • it grows well on ordinary bases, particularly those enriched with bovine bile • sensitive to disinfectants, heat and solar rays • dies after 20 minutes in the temperature of 60ºC • good tolerance of low temperature and drying out
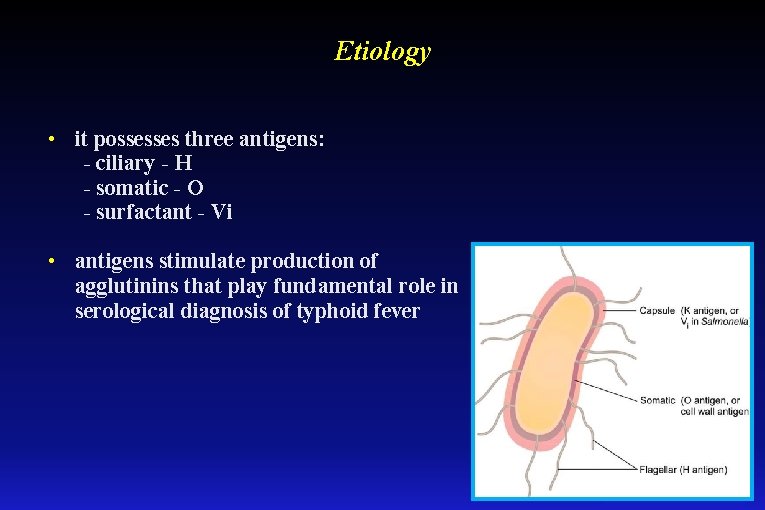
Etiology • it possesses three antigens: - ciliary - H - somatic - O - surfactant - Vi • antigens stimulate production of agglutinins that play fundamental role in serological diagnosis of typhoid fever
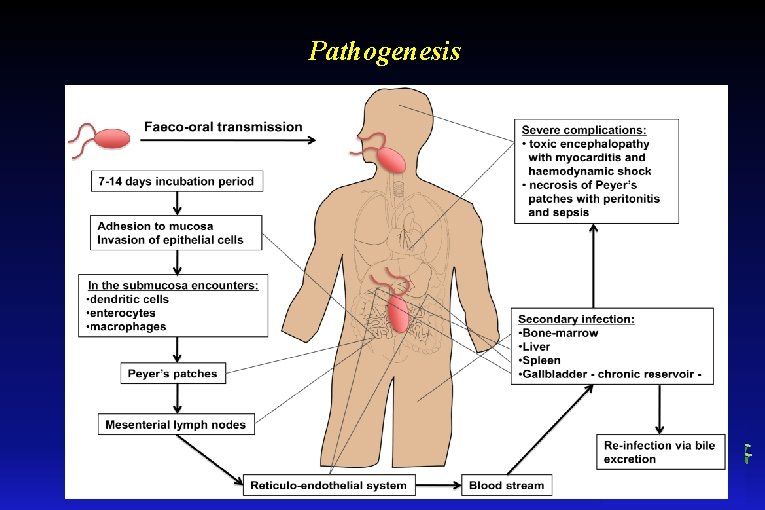
Pathogenesis

Phases of clinical course Endotoxin damage: CNS, heart, bone marrow, vegetative system, liver, spleen 10 -14 days I week II-III week IV week Incubation period Increasing of symptoms Full development of the disease Recovery

Clinical course - I phase • average incubation period 10 -14 days, in extreme case up to 7 -28 days • phase I period – incubation/prodromes: ü worsening of health condition and appetite ü generally bad condition ü occasional headaches ü subfebrile temperatures

Clinical course - II phase Phase II period – increasing of symptoms (stadium incrementi): • gradual increase of fever (after 3 -7 days it reaches the level of 39 -40) • severe headaches • unspecific muscles pains • bleeding from the nose – children often have vomits, catarrhal bronchitis, angina • meningeal symptoms • the patient becomes apathetic • characteristic stupor (inanity) up to the complete insensibility

Clinical course - II phase In the physical examination: • tongue dry, covered in brown fur, sharply separated at edges and tip, • abdomen flatulent, painful, borborygm • enlargement of liver (tender) and spleen, • the circulatory system symptoms (lowered RR , pulse dicrotic, bradycardia - disproportionately slow to temperature)
Clinical course - III phase • phase III period - full development of the disease (stadium acmes): in the second week - maximal intensity of symptoms • strong headaches, especially in the forehead area • stupor that disables consciousness of the patient, daze, raving, occasional mobility excitement (status typhosus) • strong thirst (the only stimulus that forces the patient to interact with other people) • Sleepless
Clinical course - III phase In the physical examination: • dry and cracked lips • dry tongue • scarce and sticky saliva • dried up conjunctiva • facial features sharpened and hollowed • flatulent abdomen • diaphragm movements may be limited ( hepatosplenomegaly)

Clinical course - III phase • phase III period - full development of the disease - continued - noticeable enlargement of painless spleen (continues till the end of the disease) • discrepancy between pulse and fever (conspicuous acceleration of the pulse may be an expression of complications) • in some case diarrhea can be infrequent (2 -3 t. /a day) or very frequent (10 or more) • continuous occurrence of bronchitis - sometimes its symptoms prevail (pneumotyphus)
Clinical course - III phase • on the skin of the abdomen, lower part of the chest and in some exceptional cases on the limbs characteristic rash, the so called (roseola) – very scarce, sometimes only 3 -4 pale pink spots, slightly raised above the skin, round approx. 1 -4 mm in diameter, disappear when pressed - low RR - the daily amount of urine decreases - stools (without pain or tenesmus) constipated or loose, alkaline, with appearance of the pea soup
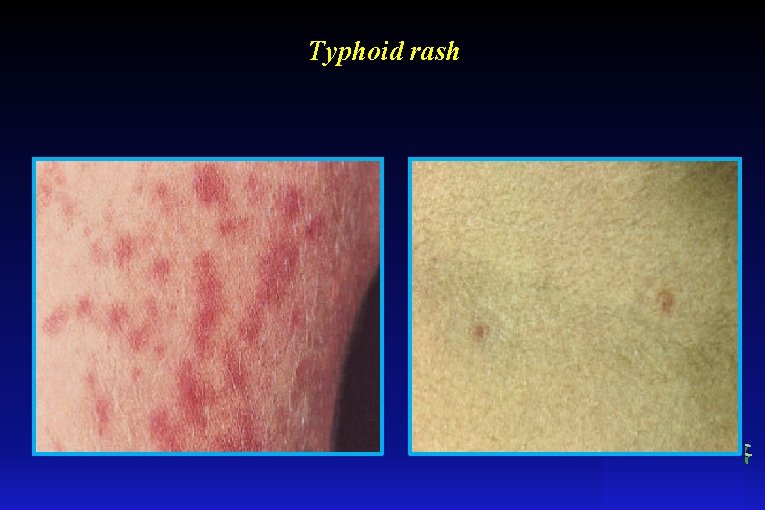
Typhoid rash

Clinical course - IV phase Phase IV – recovery (stadium sanationis): • improvement of the general well-being • lowering of the body temperature • symptoms of daze disappear • spleen diminishes • tongue clears • return of appetite - craving for food • diarrhea recedes, convalescents are weak, pale

Complications
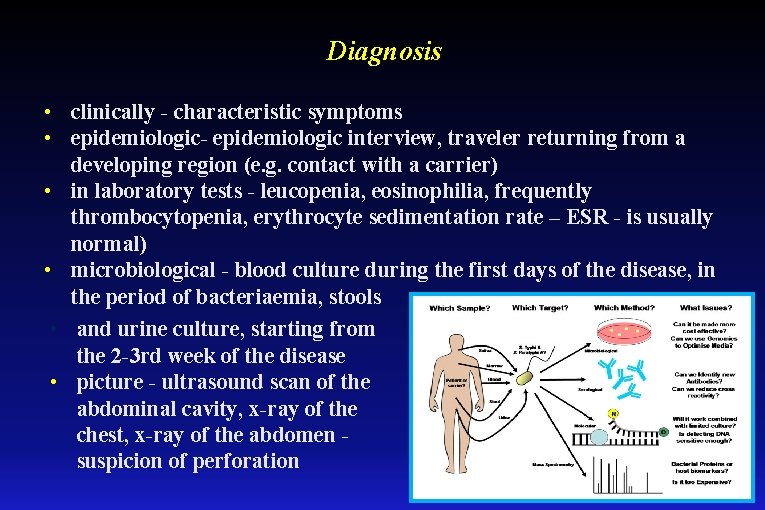
Diagnosis • clinically - characteristic symptoms • epidemiologic- epidemiologic interview, traveler returning from a developing region (e. g. contact with a carrier) • in laboratory tests - leucopenia, eosinophilia, frequently thrombocytopenia, erythrocyte sedimentation rate – ESR - is usually normal) • microbiological - blood culture during the first days of the disease, in the period of bacteriaemia, stools • and urine culture, starting from the 2 -3 rd week of the disease • picture - ultrasound scan of the abdominal cavity, x-ray of the chest, x-ray of the abdomen - suspicion of perforation

Diagnosis Serologic reaction – the classic Vidal’s agglutination reaction. None of theses tests is sufficiently sensitive or specific to replace culture-based methods for the diagnosis enteric fever • in the second week of the disease, in the blood appear the antibodies that are specific for antigens H and O • reliable reaction: in the titre 1: 200 and higher with antigen O over 1: 400 with antigen H • the day of the test is important, the previous incidence of typhus or vaccine against it - the reaction should be repeated several times with one week intervals, the increasing titre of the reaction is decisive • passive haemagglutination reaction with antigen O Salmonella typhi - its value is equal to Vidal’s reaction value

Differentiation • various infectious febrile diseases origins: common cold, influenza, paratyphoid fever, septicaemia, tuberculosis, brucellosis, tularemia, leptospirosis, EBV, CMV, viral hepatitis, malaria • non-infectious febrile diseases origins: endocarditis, lymphoma, proliferative diseases
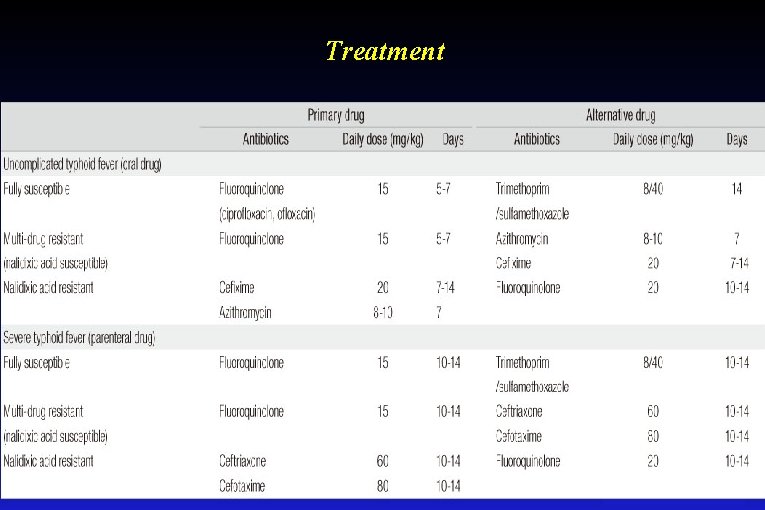
Treatment

Treatment Symptomatic: • compensation of hydro-electrolyte disorders, • monitoring of circulation and renal system functions disorders • in case of shock symptoms - steroids for 3 -5 days • recurrences in 5 -15% cases, most frequently 7 -15 days after termination of antibiotic

Prevention • common vaccinations only in the event of epidemic risk, also people travelling to the endemic areas (two types of vaccine Ty 21 a an oral live attenuated S. typhi vaccine given days 1, 3, 5, 7 with booser every 5 years; and Vi CPS a parenteral vaccine consisting of purified Vi polysaccharide from the bacterial capsule, given in 1 dose with a booster every 2 years. • observing personal hygiene • proper water supply • appropriate utilization of waste • control of sanitary and working conditions in gastronomy and food industry • treatment and control of carriers • disinfection of premises and objects that the sick person had contact with examination of convalescents for the carrier-state

Prevention Mary Mallon (September 23, 1869 – November 11, 1938), better known as Typhoid Mary, was the first person in the United States identified as an asymptomatic carrier of the pathogen associated with typhoid fever. She was presumed to have infected 49 people, three of whom died, over the course of her career as a cook. She was twice forcibly isolated by public health authorities and died after a total of nearly three decades in isolation.

Leptospirosis

Leptospirosis • it is a globally important zoonotic disease, caused by spirochetes of the genus Leptosira. Is also known as Weil|’s disaese, canicola fever, 7 day’s fever. Weil’s disease came to signify, severe leptospirosis characterized by diverse clinical findings: fever, jaundice, acute renal injury, refractory shock, hemorrhage especially pulmonary hemorrhage. • etiologic agent: - above 250 pathogenic serotypes - in human indentify often: L. caniola, L. icterohaemoragica, L. pomona, Grippotyhosa Leptospira icterohaemorrhagiae

Leptospirosis • motile, Gram negative, Spirochaete: - to visualize the spirochetes directly in culture or in clinical specimens dark-field or phase-contrast microscopy - leptospires are difficult to isolate in pure culture - susceptible: high temperature, disinfection • reservoir– rodents, small mamals, farm animals, dogs • animals eliminate bacteria with urine. Leptospira icterohaemorrhagiae

Epidemiology • the incidence of the disaese is 3 – 21 cases per year (Poland) It is estimated that seven to ten million people are infected by leptospirosis a year. The number of deaths this causes is not clear. The disease is most common in tropical areas of the world but may occur anywhere

Epidemiology Sources of infection: rats, dogs, cattle, pigs • Route of infection – (human-to-human transmission does not occur. It’s sporadic human infection. It can be occupation-related case, and case related enviromental exposure) - direct contact with sick animal - work on reclamation and sewer system - water containing animal urine (lake, swimmingpool) Contaminated agents; - contaminated water - contaminated soil - blood • Portal of entry - damage skin, mucosae membrane of nose - conjuctiva - respiratory tract – inhalation (laboratory-acquired infection rarely)
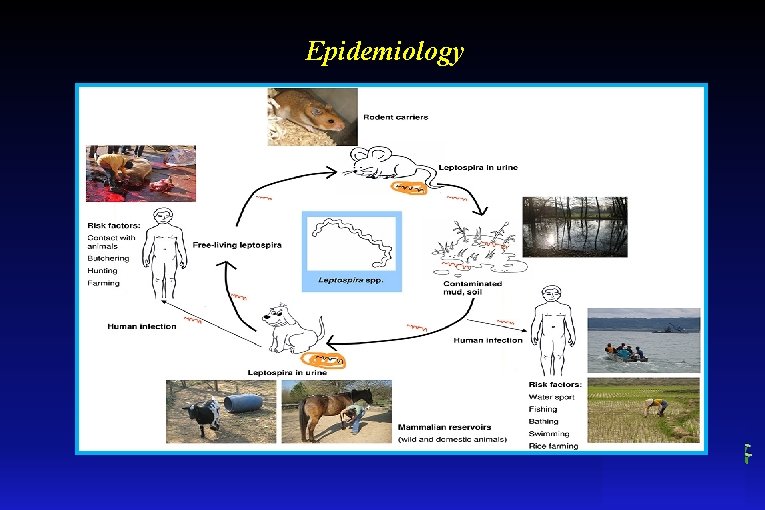
Epidemiology
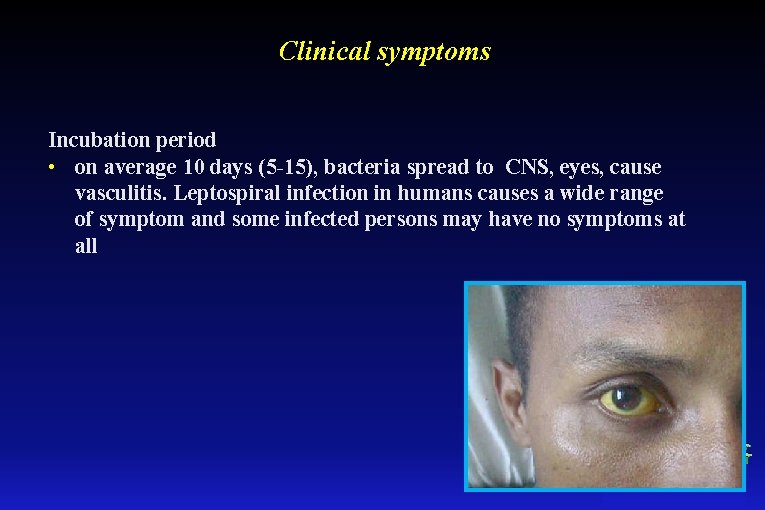
Clinical symptoms Incubation period • on average 10 days (5 -15), bacteria spread to CNS, eyes, cause vasculitis. Leptospiral infection in humans causes a wide range of symptom and some infected persons may have no symptoms at all

Clinical symptoms Biphasic course of disaese • I phase (leptospiremia) lasts 3 -10 days: at the begining flu-like symptoms (fever, chills, myalgia, intense headache, conjuctival suffusion, hepatosplenomegaly) The first phase (mild leptospirosis) resolves, and the patient is briefly asymptomatic until the second phase (severe leptospirosis) begins. 90 percent of cases of the disease are mild leptospirosis and without any specific treatment and the rest develop to severe leptospirosis • II phase (immunological) - affected heart, liver damage, renal failure - affected brain, menigitis, encephalitis > 50% cases - optic neuritis, peripheral neuropathy
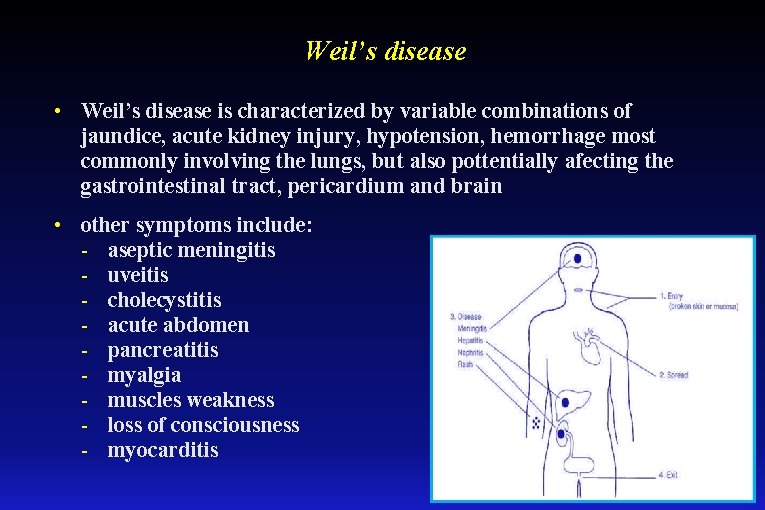
Weil’s disease • Weil’s disease is characterized by variable combinations of jaundice, acute kidney injury, hypotension, hemorrhage most commonly involving the lungs, but also pottentially afecting the gastrointestinal tract, pericardium and brain • other symptoms include: - aseptic meningitis - uveitis - cholecystitis - acute abdomen - pancreatitis - myalgia - muscles weakness - loss of consciousness - myocarditis
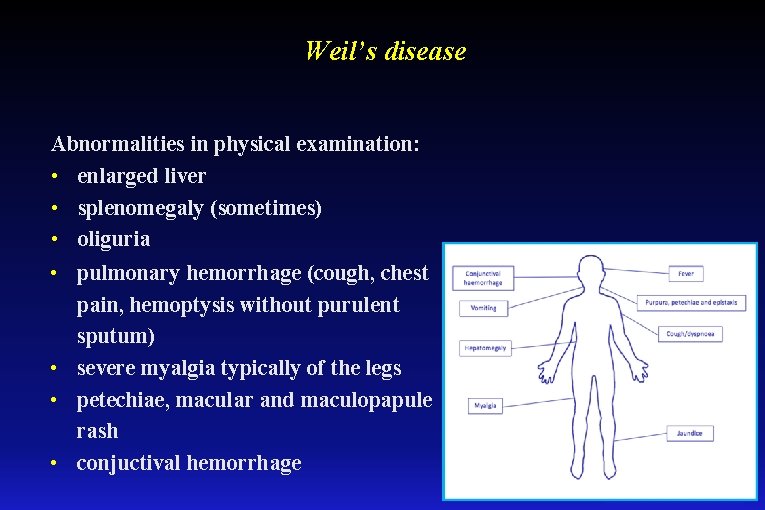
Weil’s disease Abnormalities in physical examination: • enlarged liver • splenomegaly (sometimes) • oliguria • pulmonary hemorrhage (cough, chest pain, hemoptysis without purulent sputum) • severe myalgia typically of the legs • petechiae, macular and maculopapule rash • conjuctival hemorrhage

Diagnostic test • Laboratory tests: - leucocytosis with increased of count of neutrophils - thrombocytopenia - hemolytic anemia mild to moderate - elevation: aminotransferase, creatine kinase, urea, alkaline phosphtase, creatinine, bilirubin - decline; INR - urinalysis may show abnormalitis of the sediment : leukocytes, erythrocytes, hyalin and granular cases. • CSF: - cytosis 10 -1000 cells/ml - glucosae in normal range - protein <100 mg/ml

Diagnostic test • Etiologic tests - culture – isolation bacteria from blood, urine, CSF - microscopic slide in dark-field or phase-contrast microscopy - PCR - serologic assays (ELISA, indirect hemagglutination, MAT – microscopic agglutination test) investigations should be repeated after 10 -14 days
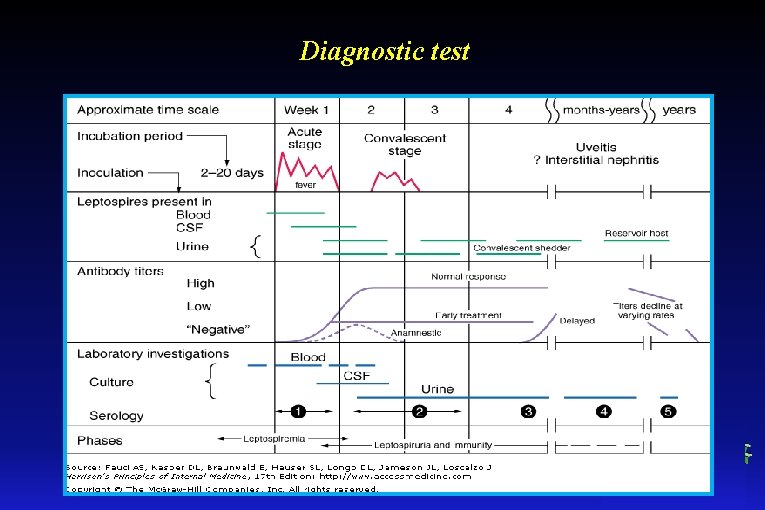
Diagnostic test
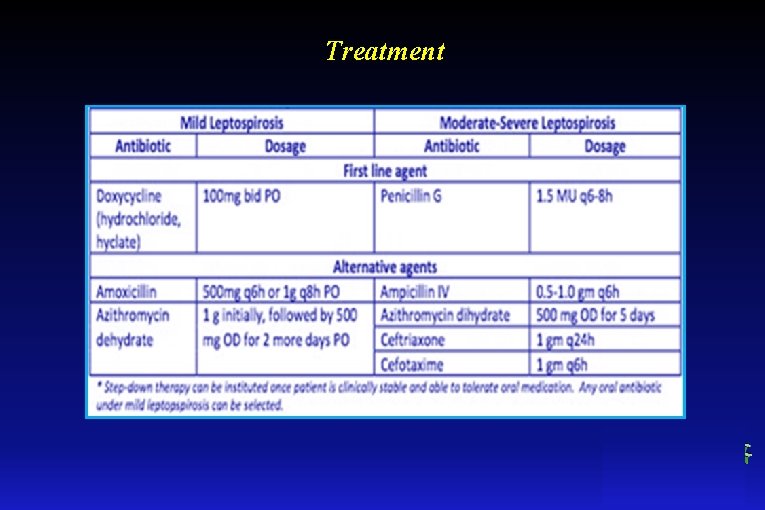
Treatment

Prevention • no vaccine is available for human leptospirosis • preventive strategies including prophylaxis with doxycycline have been variably effective in different settings • antibiotic prophylaxis can be considered for anticipated short-term, well-defined exposures such as those incurred during military training or specific adventure travel • long-term antibiotic prophylaxis has not been shown to be effective in preventing infection in high-transmission endemic settings

Epidemic (louse borne) typhus This is a form of typhus so named because the disease often causes epidemics following wars and natural disasters. The causative organism is Ricketssia prowazeki transmitted by the human body louse (Pediculus humanus corporis). Feeding on a human who carries the bacillus infects the louse. R. prowazekii grows in the louse's gut and is excreted in its feces. The disease is then transmitted to an uninfected human who scratches the louse bite (which itches) and rubs the feces into the wound. The incubation period is one to two weeks.

Epdemiology Typhus fever occurs in colder (i. e. mountainous) regions of Central and Eastern Africa, Central and South America, and Asia. In recent years, most outbreaks have taken place in Burundi, Ethiopia and Rwanda. Typhus fever occurs in conditions of overcrowding and poor hygiene, such as in prisons and refugee camps.

Clinical symptoms Sudden onset: • fever, headache, muscle pain, prostration, myalgia, cough • fever rising rapidly to 38 -40 º C • the 5 -th or 7 -th day appears rash which begins on the upper trunk then become generalized involving the entire body without face, palms and soles. The rash is macular, maculopapular, petechial and confluent. Skin necrosis and gangrena • potophobia, conjuctival injection, eyes pain • interstitial pneumonia • patient with untreated infections develop renal insufficiency, multiorgan involvement in which neurologic manifestations are frequently prominent. • confusion, coma
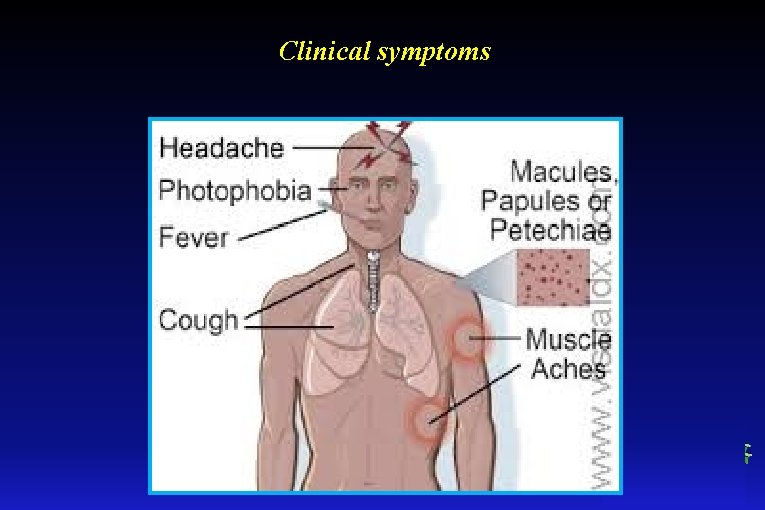
Clinical symptoms
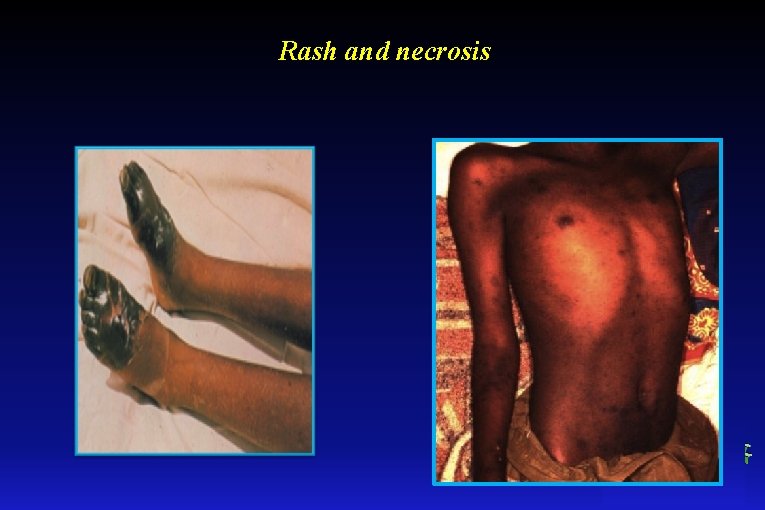
Rash and necrosis

Diagnostic tests Serological reactions in rickettsial infections

Treatment and prevention • doxycycline - 200 mg/d given in two divided doses 7 -10 days • prevention of epidemic typhus • control of body lice • clothes should be changed regulary • insecticides should be used every 6 weeks to control the louse population

Brill-Zinser disease • It is a recrudescent illness occuring years after acute epidemic typhus, probably as a result of wanig immunity. R. prowazekii remains latent for years, its reactivation results in sporadic cases of disease in louse-free populations or in epidemics in louseinfested population
- Slides: 50