Enteral Parenteral Nutrition 1 Enteral Tube Feedings Enteral

Enteral & Parenteral Nutrition 1
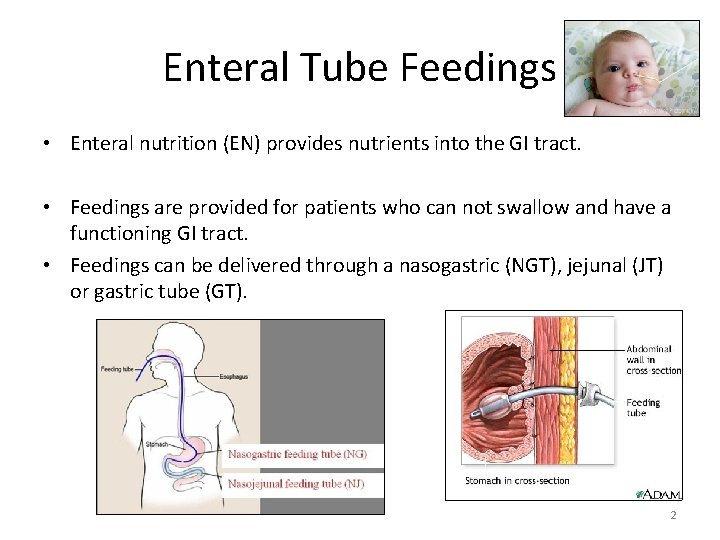
Enteral Tube Feedings • Enteral nutrition (EN) provides nutrients into the GI tract. • Feedings are provided for patients who can not swallow and have a functioning GI tract. • Feedings can be delivered through a nasogastric (NGT), jejunal (JT) or gastric tube (GT). 2

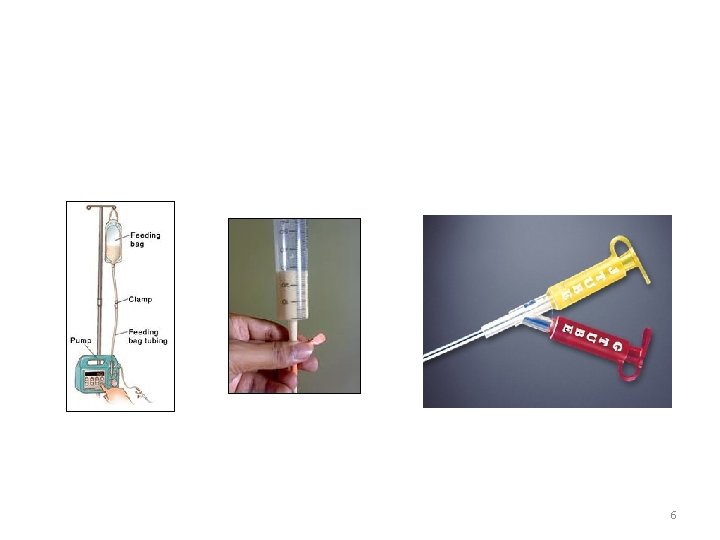
Enteral Tube Feedings Procedure: • Start at full strength • Slow rate • Increase every 8 -12 hours as ordered • Assess for signs of intolerance • High gastric residuals, nausea, cramping, vomiting and diarrhea • Assess for complications • Aspiration, Diarrhea, Bacterial contamination, Tube occlusion, delayed gastric emptying 3

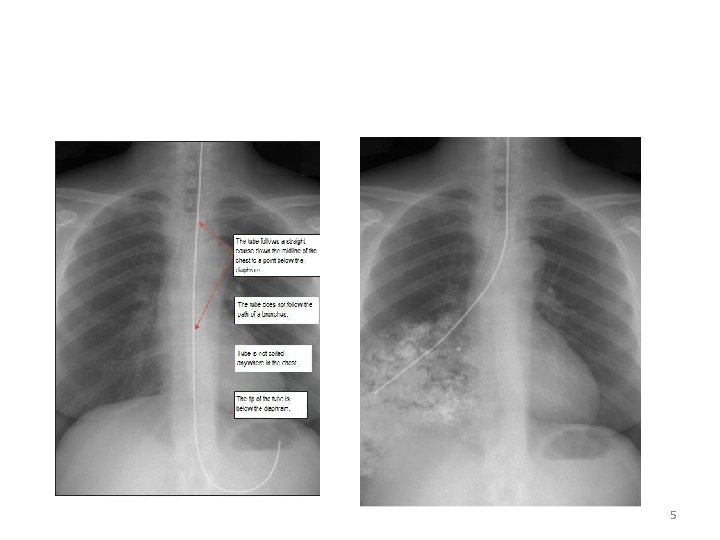
Tube Placement • The most reliable method for verification of placement of small-bore feeding tubes is x-ray film examination. • Check p. H of gastric aspirate, < 4 • Observe aspirate color • Do not use auscultation method 4
5
6

Nursing Diagnosis Risk for Aspiration r/t NGT feeding Outcome: Patient will maintain patent airway and clear lung sounds. Nursing Interventions 1. Determine if patient is at high risk for aspiration: coughing, hx of GERD, nasotracheal suction, an artificial airway, decreased LOC, and lying flat. 2. Keep HOB up to 30 -45 degrees at all times 3. Measure gastric residual volumes every 4 -6 hrs. 1. 250 ml or more on 2 consecutive assessments: delayed gastric emptying or if 500 ml on assessment 2. Discuss follow up with HCP 7

Nursing Diagnosis Risk for Aspiration r/t NGT feeding 1. Stop feedings if aspiration occurs 2. Administer metoclopramide (Reglan) if ordered 3. Monitor for nausea, vomiting, cramping and diarrhea and tube occlusion. 4. Increase rate per order 8

Parenteral Nutrition • Parenteral nutrition (PN) is a form of specialized nutrition support in which nutrients are provided intravenously. • A basic PN formula is a combination of amino acids, hypertonic dextrose (10 -50%), electrolytes, vitamins, and trace elements. • Fat emulsions: provides calories and fatty acids – Delivered through • Central venous catheter • Peripheral line (rarely) pg 1021 9

Parenteral Nutrition • If using a CVC that has multiple lumens, use a port that is exclusively dedicated for the TPN. Label it! • Verify the HCP’s order • Inspect the solution for particulate matter • Always use an infusion pump • First 24 -48 hrs: delivers 50% of estimated needs and then rate has will be increased (run at 40 -50 ml) 10

Parenteral Nutrition: Complications • Catheter-related Problems – Pneumonthorax • Sudden sharp chest pain, dyspnea, and coughing • Monitor for 24 hrs – Air embolus • Occurs during insertion of the catheter or when changing the tubing or cap. • Turn pt to left side and have pt perform a Valsalva maneuver (hold breath and bear down during catheter insertion to help prevent air embolus • Keep IV system closed 11

Parenteral Nutrition: Complications • Catheter-related Problems – Catheter occlusion • If sluggish or no flow, stop infusion and flush with NS or heparin (per protocol). • Attempt to aspirate clot or follow protocol for thrombolytic agent (urokinase) – Sepsis • Fever, chills, or glucose intolerance and positive blood culture • Change tubing q 24 hrs • Hang bag for only 24 hr; lipids 12 hrs • Check to see if solution needs a filter 12

Parenteral Nutrition: Complications • Metabolic alterations – Electrolyte and mineral imbalances – Hyperglycemia • Thirst, HA, lethargy, increased urination. • Monitor BS q 6 hrs • Give insulin – Hypoglycemia • • Diaphoresis, shakiness, confusion, loss of consciousness Do not abruptly discontinue TPN Taper rate Give IV bolus of dextrose – Dehydration 13
- Slides: 13