ENT in Primary Care proposed management guidelines Alison













- Slides: 14

ENT in Primary Care proposed management guidelines Alison Hunt ENT Consultant ENT Dept MKUH

Discussion points to be covered • Tinnitus • Sensorineural Hearing loss • Vertigo • Snoring and OSA

Nature of tinnitus • Bilateral/unilateral • Pulsatile/non pulsatile • Subjective/objective – All patients should have oto-neurological examination – If pulsatile listen for bruits – Hearing test

General management of tinnitus • Explanation that tinnitus is benign in most cases • Sound therapy and distraction techniques help • Hearing aid where SNHL is very useful • Manage depression/ exacerbating psychological factors • If no better consider referral for tinnitus counseling

Management of tinnitus • Check hearing • Explain hearing test results and nature of tinnitus • If SNHL consider hearing aid/sound therapy/Tinnitus couselling • Unilateral tinnitus or asymmetric SNHL >15 d. B in 2 consecutive frequencies : MRI IAMS

Adult Unilateral Hearing loss • Sudden onset SNHL needs urgent PO high dose steroid, followed by E Clinic referral. Confirm with community hearing test and tympanogram. • Chronic hearing loss. – Unilateral SNHL requires MRI IAM (only refer to ENT if abnormal scan), consideration of hearing aid. – Symmetrical SNHL does not require referral unless rapid progression.

Vertigo in Primary care • General imbalance, "dizziness” or being “a bit wobbly” are NOT ENT RELATED SYMPTOMS. Suggest referral to falls clinic/medical review. • General imbalance in the elderly is NOT ENT related. – Suggest general medical work up in primary care /elderly care community/geriatrician review • 3 key questions in the history for ENT related true vertigo (spinning sensation). • 1 Does the patient experience true spinning? • 2 How long does it last, seconds minutes or hours? • 3 Is there associated hearing loss?

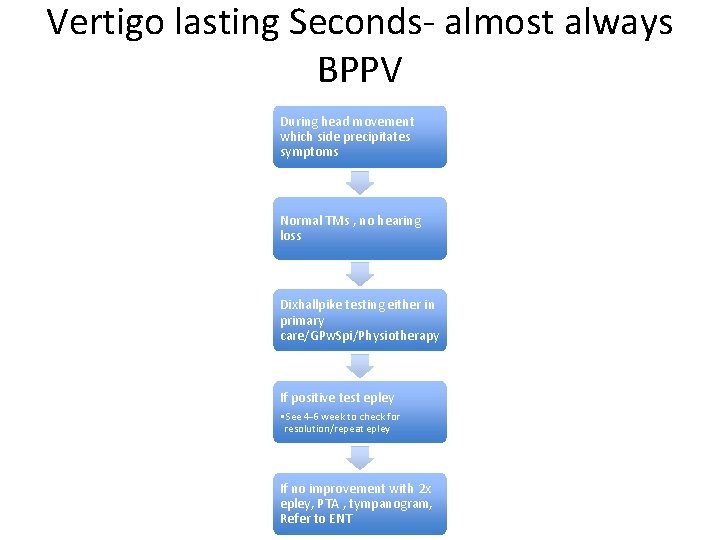
Vertigo lasting Seconds- almost always BPPV During head movement which side precipitates symptoms Normal TMs , no hearing loss Dixhallpike testing either in primary care/GPw. Spi/Physiotherapy If positive test epley • See 4 -6 week to check for resolution/repeat epley If no improvement with 2 x epley, PTA , tympanogram, Refer to ENT

Vertigo in Primary Care • Seconds- BPPV – ref to community GPWSp. I/physio for epley • Minutes to hours- vestibular neuronitis /labyrinthitis if – single episode. Prochlorperazine prn observe – multiple separate attacks consider Meniere's treatment/recurrent vestibulopathy +/- referral. • 1 -2 Days neuronitis/labyrinthitis. – Usually settles with prochlorperazine observe • 1 week or more and no recovery – consider CVA and medical referral first – Consider vestibular decompensation and refer.

Vertigo in Primary Care • All patients require hearing test. If asymmetric SNHL on testing, SNHL protocol will apply. • Patients with imbalance following episode of true vertigo will require balance physiotherapy in some form – Cawthorne-cooksey exercises – Referral to community physio

Vertigo in primary care • Acute/single episodes- prochlorperazine • Meniere's – low salt < 2 g day – Betahistine 16 mg TDS – Intermittent prochlorperazine for acute episodes

Vertigo in Primary Care • ? Only hospital referrals via GPw. Spi • ? Only those failing community management to be referred

Snoring • Simple Snoring vs OSA – Define in history – Epworth score for OSA • Do not require referral to ENT • Snoring-manage in community: TSH, BMI, Wt loss, tailor made mandibular advancement device via dentist (British Snoring and Sleep Apnoea Association) • OSA –ref to respiratory team to consider CPAP

Implementation and facilitating change • Access to hearing tests in the community promptly and interpretation of tests • Community vestibular physiotherapy – (Matt Search resigned post ? Alternative arrangements) • Tinnitus counselling in the community- could this be offered by community audiology team? • Hearing aid provision in the communityaccess/availability