Engaging Communities in the RAAM Clinic Process Blood

Engaging Communities in the RAAM Clinic Process Blood, sweat and tears: Tragedy, turmoil, sacrifice and frustration. The northern experience in opening de-centralized RAAM clinics and engaging Primary care in addictions medicine September 20, 2018 Dr. Mike Franklyn, MD CCFP, NE LHIN Regional RAAM Lead Stephanie Paquette, Mental Health and Addiction Lead, NELHIN Paola Folino, Regional RAAM Coordinator, Health Sciences North

CFPC COI Templates: Slide 1 DISCLOSURE OF FINANCIAL SUPPORT • This program has received financial support from [organization name] in the form of [describe support here – e. g. an educational grant]. • This program has received in-kind support from [organization name] in the form of [describe support here – e. g. logistical support]. • Potential for conflict(s) of interest: - [Speaker/Faculty name] has received [payment/funding, etc. ] from [organization supporting this program AND/OR organization whose product(s) are being discussed in this program]. - [Supporting organization name] [developed/licenses/distributes/benefits from the sale of, etc. ] a product that will be discussed in this
![CFPC COI Templates: Slide 2 FACULTY/PRESENTER DISCLOSURE • Faculty: [Speaker’s name] • Relationships with CFPC COI Templates: Slide 2 FACULTY/PRESENTER DISCLOSURE • Faculty: [Speaker’s name] • Relationships with](http://slidetodoc.com/presentation_image/5f3746d009885fc804a4771d0cf3821c/image-3.jpg)
CFPC COI Templates: Slide 2 FACULTY/PRESENTER DISCLOSURE • Faculty: [Speaker’s name] • Relationships with financial sponsors: - Grants/Research Support: [Pharma. Corp ABC] - Speakers Bureau/Honoraria: [XYZ Biopharmaceuticals Ltd. ] - Consulting Fees: Med. X Group Inc. - Patents: [Widget ABC] - Other: [Employee of XXY Hospital Group]

CFPC COI Templates: Slide 3 – This slide may be omitted if there is no C)I declared in the previous 2 slides MITIGATING POTENTIAL BIAS • [Explain how potential sources of bias identified in slides 1 and 2 have been mitigated by the scientific planning committee]. • Refer to “Quick Tips” document

Objectives of Presentation 1. To describe how a Hub and Spoke model has supported the development of RAAM clinics in Non-Urban centres. 2. To describe how a Coordinated Approach has facilitated the development of RAAM clinics in Non-Urban centres. 3. To describe how to overcome Access Issues related to non-urban centres. 4. To describe outstanding challenges and next steps for north eastern Ontario.
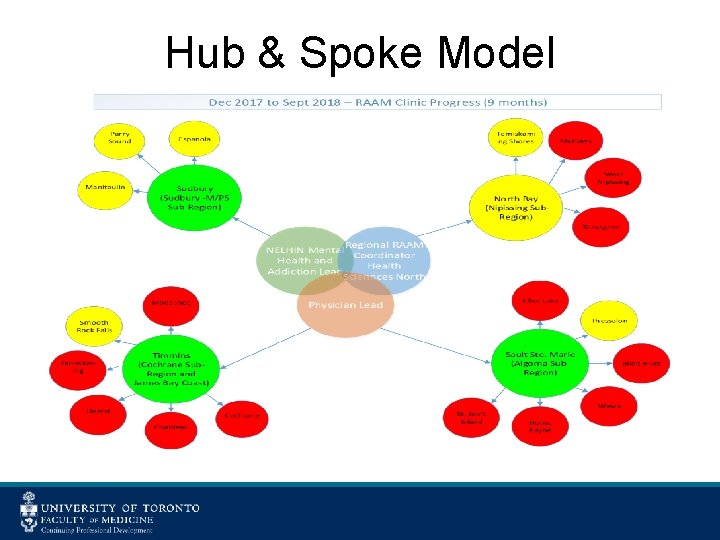
Hub & Spoke Model

Hub & Spoke Model • Support in Each Sub-Region is consistent, fairly distributed, and conducted in a standard way. • Fidelity to the Meta-phi model is maintained through a standard approach to development. • Successes and Challenges are shared

Hub Site Role • Development of RAAM clinic within Hub Site (followed a “timeline” across NE) • Phasing into respective spoke sites • Participate/engage in conversations support across region, attending 1 -1’s, attending COP, etc.
What is HSN’s Role? • Regional role supporting the development of clinics for the Hub Sites and the expansion to our districts spoke sites (Manitoulin Island, Parry Sound, Espanola) • What does this look like? – Sharing resources, templates – Monthly 1 -1 touch points – Quarterly regional community of practice meetings – Engagement sessions – Education & Academic detailing sessions
Phasing into Spoke Sites • Varies across the region, however most have been following sample action plan developed as a step by step • Trying to phase in 1 site at a time to ensure proper supports are in place and linkages to hub site however goal is to build capacity locally
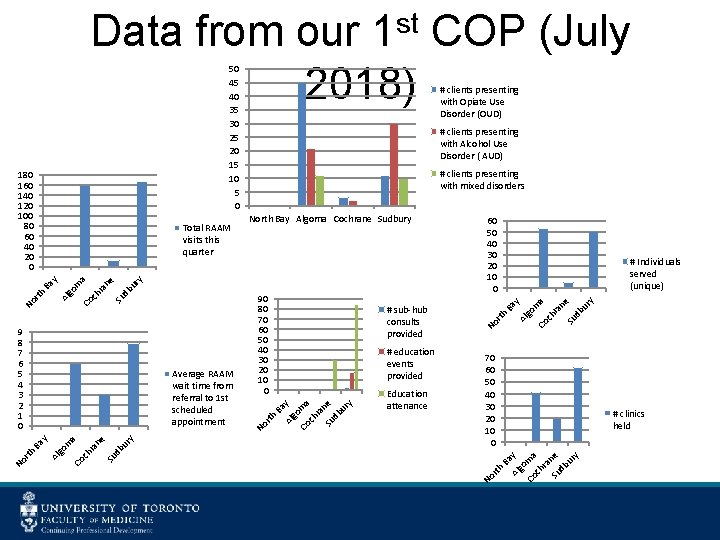
Data from our 1 st COP (July 2018) 50 45 40 35 30 25 20 15 10 5 0 ch a ra Su ne db ur y Ba Co rth No y db ur Su ra ne a Co ch y go m Ba Al # clinics held y Co Education attenance 70 60 50 40 30 20 10 0 go m ch a ra Su ne db ur y go m Al rth Ba y # education events provided rth # sub-hub consults provided # Individuals served (unique) Al ry db u ne 90 80 70 60 50 40 30 20 10 0 Su ra ch Co go m Al Ba y a Average RAAM wait time from referral to 1 st scheduled appointment rth North Bay Algoma Cochrane Sudbury No 9 8 7 6 5 4 3 2 1 0 No # clients presenting with mixed disorders ry db u ne Su ch ra go m Co No Al rth Ba y a Total RAAM visits this quarter # clients presenting with Alcohol Use Disorder ( AUD) No 180 160 140 120 100 80 60 40 20 0 # clients presenting with Opiate Use Disorder (OUD)
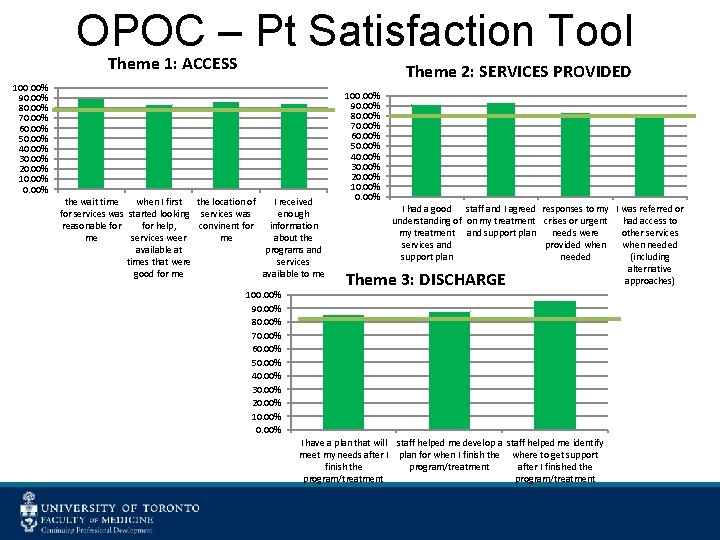

OPOC – Pt Satisfaction Tool Theme 1: ACCESS Theme 2: SERVICES PROVIDED 100. 00% 90. 00% 80. 00% 70. 00% 60. 00% 50. 00% 40. 00% 30. 00% 20. 00% 10. 00% the wait time when I first the location of I received for services was started looking services was enough reasonable for help, convinent for information me services weer me about the available at programs and times that were services good for me available to me 100. 00% 90. 00% 80. 00% 70. 00% 60. 00% 50. 00% 40. 00% 30. 00% 20. 00% 10. 00% I had a good staff and I agreed responses to my I was referred or understanding of on my treatment crises or urgent had access to my treatment and support plan needs were other services and provided when needed support plan needed (including alternative approaches) Theme 3: DISCHARGE I have a plan that will staff helped me develop a staff helped me identify meet my needs after I plan for when I finish the where to get support finish the program/treatment after I finished the program/treatment

What we did…and didn’t do • First we opened (Dec 2015) … then we starting planning • Who we wanted to engage: Communities, physicians, departments • What we did well: seeing and treating patients • What we needed to work on: building capacity, reintegrating patients into PC

Physician Engagement Academic Detailing V 1. 0 Dinner with physicians. V 2. 0 Impact level C Small group information sessions. Impact level B- V 3. 0 Small group case based sessions Impact level B+ Above with followup in office addiction consultation. Impact Level AV 4. 0 V 5. 0 Above with followup office based OST induction and ongoing support. Impact Level A+

Sudbury Dec 8/9 RAAM Summit Sudbury. Feb 1 (2 NAS workshops) Timmins Feb 6 -8 Moose Factory Feb 9 Espanola Feb 13 Parry Sound Feb 26 North Bay March 6 Manitoulin March 15 North Bay March 20 Collingwood March 22/23 Parry Sound March 27 PH Emergency Management Opioid Workshop Sudbury March 28 SSM/Algoma March 29/30 Sudbury April 3 (NAS Training) Thunder Bay April 16 SSM/Algoma April 27/28 Overdose Death Summit North Bay …. I forget the date I have been on the road so long……… Sudbury RAAM May 7/8 preceptorship Temiskaming May 3/4 Thunder Bay May 28 Day of Learning Timmins June 20/21


RAAM Duties Review META-PHI documents Handling physician initiated: -Calls -Consults -other RAAM docs and leads Pharmacy calls Conference calls META PHI COP other docs/LHINs Supervising mentoring docs/NP Attending community meetings: -Mental health -Addictions -Crisis planning -Education -FHT’s -Public Health -Local opiate crisis strategy/Task Force -Psychiatry - HSN pain clinic -HSN addiction consult service RAAM QAC RAAM physician recruiting Attending RAAM summits Attending OCFP regional MMAP meetings Budget meetings and planning Hospital based CME OB nurses ICN nurses Pediatricians ED Department Academic detailing sessions Visiting PCP offices for addiction consults Visiting PCP offices for inductions work on NOSM CPED Work on U of T CPED Work on META-PHI handbook and revisions Contribute to MET-list serve Meeting and calls with OTN Work of HQO committees Work on MOHLTC committees


What have we learned • Providers are interested … but hesitant • They would rather refer • They don’t want to act alone …. Need backup and support • Teachable skills …. Lots of education needed • Providers are sometimes willing to go outside their comfort zone for their own patients • Need to make it an introspective exercise … “look into your own practice” • Having a group approach to share resources & expertise has been very helpful

Challenges • • Keeping the “R” in Rapid Pathway back to Primary Care Engaging primary care providers Privacy concerns (i. e. using multiple organizations to support clinic, different EMRS…)

Delicate situations • Task forces to inform decisions • Why it is important to have the right provider • Leveraging community resources

Questions?
- Slides: 22