Endovenous Radiofrequency Ablation of the Saphenous Vein The

Endovenous Radiofrequency Ablation of the Saphenous Vein The VNUS Closure® Procedure VN 20 -86 -E 4/09
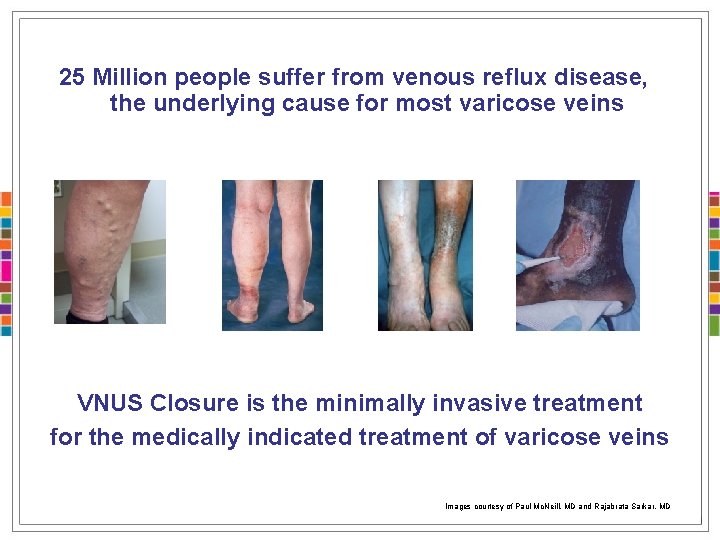
25 Million people suffer from venous reflux disease, the underlying cause for most varicose veins VNUS Closure is the minimally invasive treatment for the medically indicated treatment of varicose veins Images courtesy of Paul Mc. Neill, MD and Rajabrata Sarkar, MD
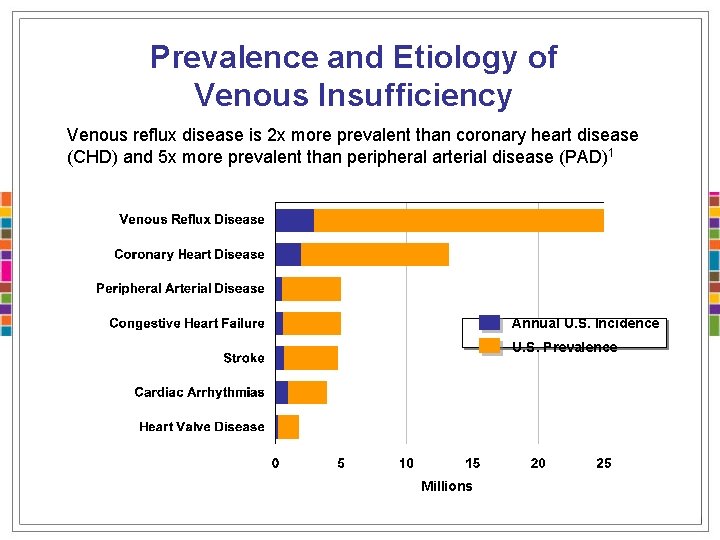
Prevalence and Etiology of Venous Insufficiency Venous reflux disease is 2 x more prevalent than coronary heart disease (CHD) and 5 x more prevalent than peripheral arterial disease (PAD)1 Annual U. S. Incidence U. S. Prevalence Millions

Prevalence and Etiology of Venous Insufficiency Of the estimated 25 million people with symptomatic superficial venous reflux 1 : • Only 1. 7 million seek treatment annually 2 • Over 23 million go untreated Prevalence by Age and Gender 3, 4 Age Female Male 20 - 29 8% 1% 40 - 49 41% 24% 60 - 69 72% 43%
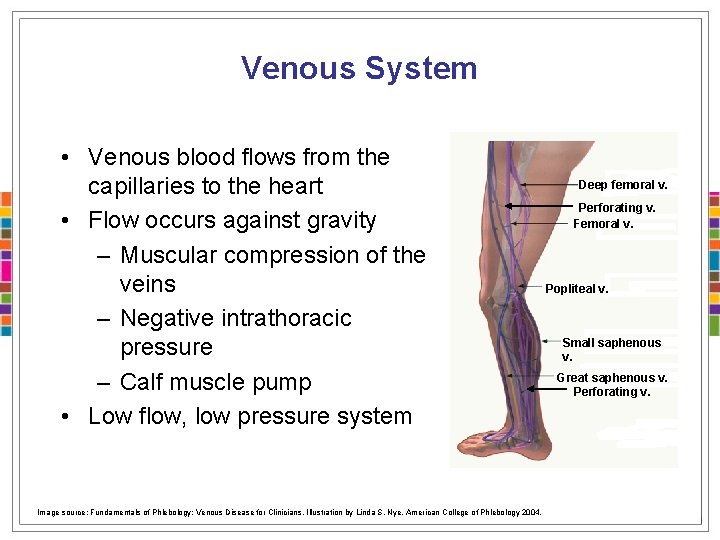
Venous System • Venous blood flows from the capillaries to the heart • Flow occurs against gravity – Muscular compression of the veins – Negative intrathoracic pressure – Calf muscle pump • Low flow, low pressure system Image source: Fundamentals of Phlebology: Venous Disease for Clinicians. Illustration by Linda S. Nye. American College of Phlebology 2004. Deep femoral v. Perforating v. Femoral v. Popliteal v. Small saphenous v. Great saphenous v. Perforating v.
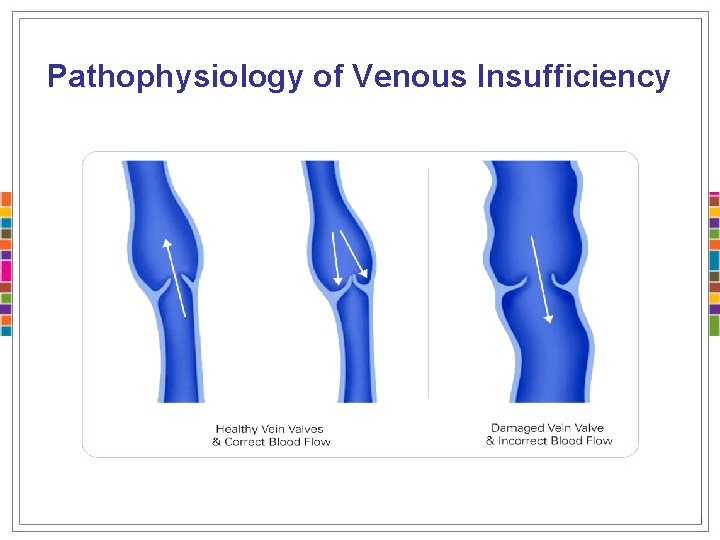
Pathophysiology of Venous Insufficiency

Risk Factors and Symptoms of Venous Insufficiency Risk factors of venous insufficiency: Symptoms of venous insufficiency: • Gender • Leg pain, aching, or cramping • Age • Burning or itching of the skin • Heredity • Leg or ankle swelling • Pregnancy • “Heavy” feeling in legs • Standing occupation • Skin discoloration or texture changes • Obesity • Open wounds or sores • Prior injury or surgery • Restless legs • Sedentary lifestyle • Varicose Veins
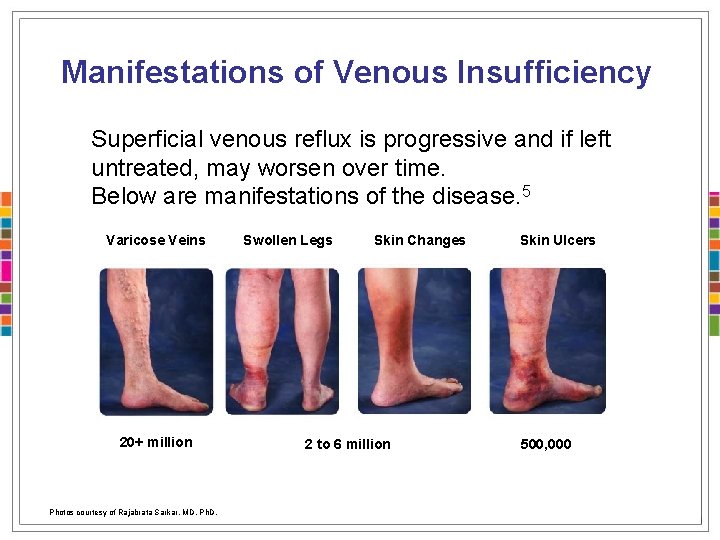
Manifestations of Venous Insufficiency Superficial venous reflux is progressive and if left untreated, may worsen over time. Below are manifestations of the disease. 5 Varicose Veins 20+ million Photos courtesy of Rajabrata Sarkar, MD, Ph. D. Swollen Legs Skin Changes 2 to 6 million Skin Ulcers 500, 000

CEAP Classifications Clinical Classifications of Venous Insufficiency (CEAP) • • • Class 0 - No visible or palpable signs of venous disease Class 1 - Telangiectasias or reticular veins Class 2 - Varicose veins Class 3 - Edema Class 4 - Skin changes • (4 a) Skin changes including pigmentation or venous eczema • (4 b) Skin changes with lipodermatosclerosis • Class 5 - Healed venous ulceration • Class 6 - Active venous ulceration

The VNUS Closure® System • The VNUS Closure System is a minimally invasive treatment alternative for patients with symptomatic superficial venous reflux and varicose veins • Using a catheter-based approach, the VNUS Closure. FAST™ catheter delivers radiofrequency (RF) energy to the vein wall • RF energy creates conductive heating that contracts the vein wall collagen, thereby occluding the vein
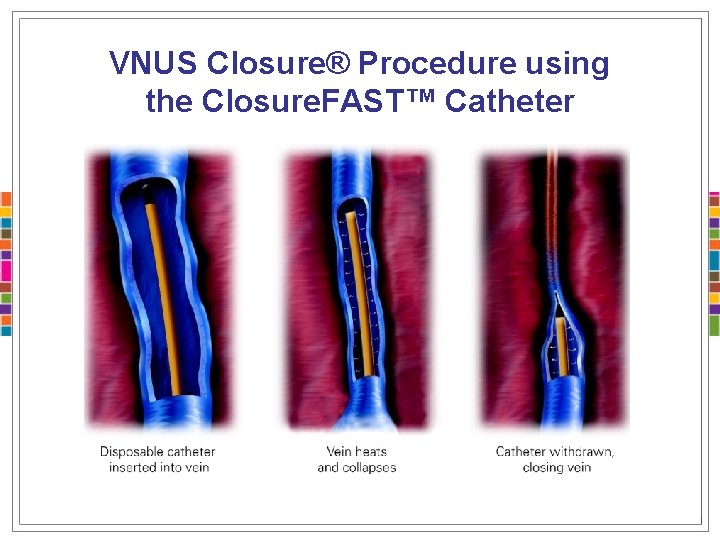
VNUS Closure® Procedure using the Closure. FAST™ Catheter

Efficacy of the Closure. FAST™ Catheter The Closure. FAST™ catheter ablates the vein in 7 cm segments with 20 -second treatment cycles, resulting in vein shrinkage and occlusion. Interim data from a multicenter prospective study have shown 97. 4% vein occlusion 1 year posttreatment. 6
Radiofrequency Ablation Procedure Video

Ablation Comparison (simulation in beef liver)
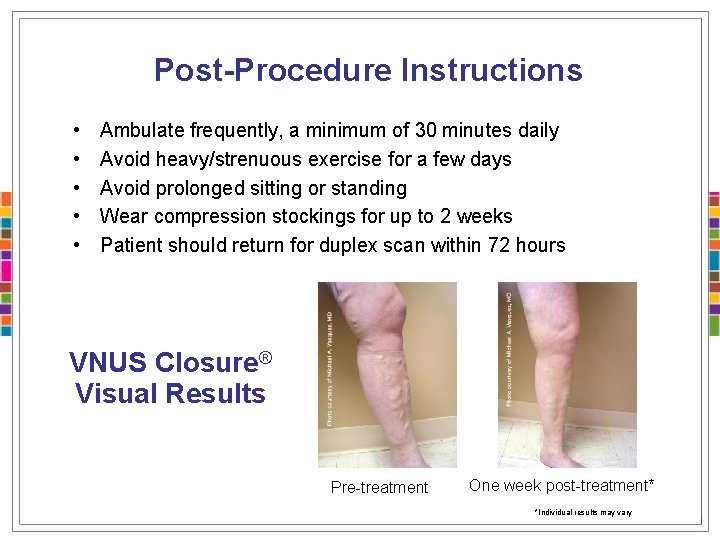
Post-Procedure Instructions • • • Ambulate frequently, a minimum of 30 minutes daily Avoid heavy/strenuous exercise for a few days Avoid prolonged sitting or standing Wear compression stockings for up to 2 weeks Patient should return for duplex scan within 72 hours VNUS Closure® Visual Results Pre-treatment One week post-treatment* *Individual results may vary

RECOVERY Trial 7 A Prospective, Multi-Center, Randomized Study Purpose - Determine if patient recovery and other short term outcomes are different between radiofrequency and laser treatment – Six center, single-blinded randomized trial of Closure. FAST vs. Endovenous Laser – 69 patients; 87 limbs treated (46 CLF; 41 EVL) – Patient follow up at 2, 7, 14, and 30 days after treatment
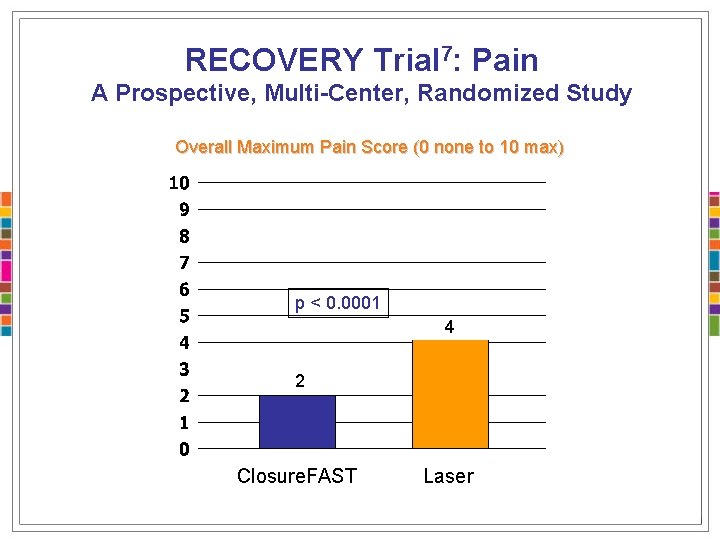
RECOVERY Trial 7: Pain A Prospective, Multi-Center, Randomized Study Overall Maximum Pain Score (0 none to 10 max) p < 0. 0001 4 2 Closure. FAST Laser
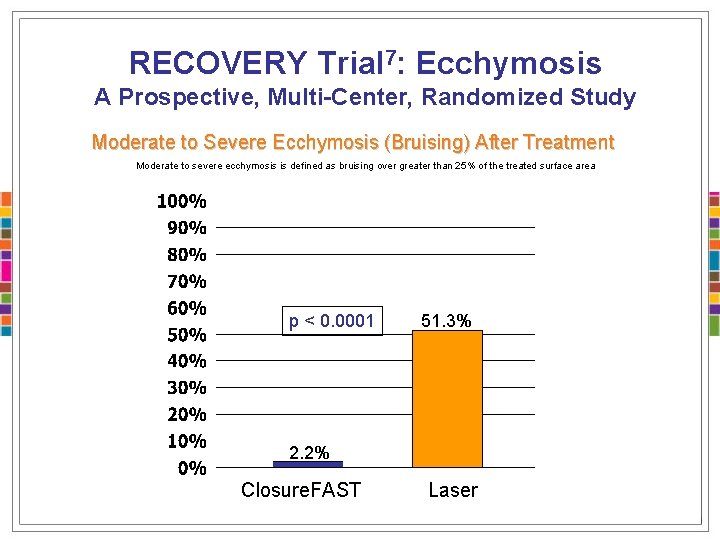
RECOVERY Trial 7: Ecchymosis A Prospective, Multi-Center, Randomized Study Moderate to Severe Ecchymosis (Bruising) After Treatment Moderate to severe ecchymosis is defined as bruising over greater than 25% of the treated surface area p < 0. 0001 51. 3% 2. 2% Closure. FAST Laser
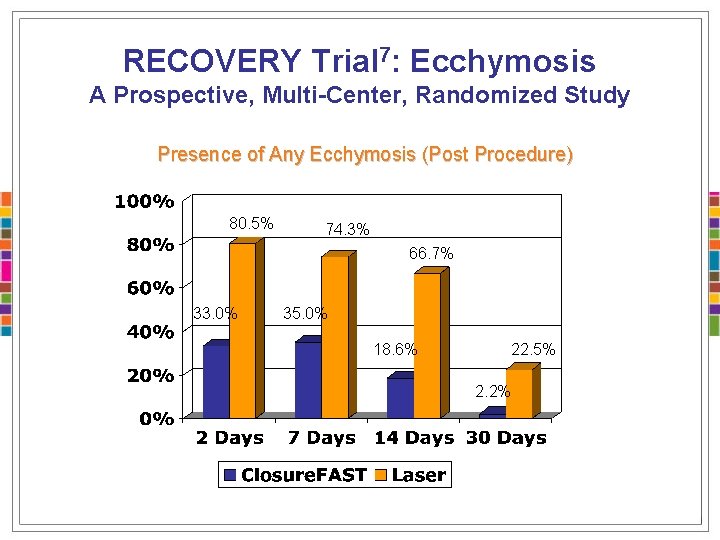
RECOVERY Trial 7: Ecchymosis A Prospective, Multi-Center, Randomized Study Presence of Any Ecchymosis (Post Procedure) 80. 5% 74. 3% 66. 7% 33. 0% 35. 0% 18. 6% 22. 5% 2. 2%

RECOVERY Trial 7: Conclusion A Prospective, Multi-Center, Randomized Study Compared to laser, RF treatment with Closure. FAST produced significantly – Less pain p < 0. 0001 – Less tenderness p = 0. 0008 – Less bruising p < 0. 0001 – Fewer adverse events p = 0. 021

Closure. FAST™ Catheter Indication: • The Closure. FAST Catheter is intended for endovascular coagulation of blood vessels in patients with superficial venous reflux Contraindications: • Patients with thrombus in the vein segment to be treated Potential Risks & Complications: • Potential complications include, but are not limited to, the following: vessel perforation, thrombosis, pulmonary embolism, phlebitis, hematoma, infection, adjacent nerve injury, skin burns, deep vein thrombosis
Venous leg ulcers Venous Ulcers Treat the source, not just the symptom
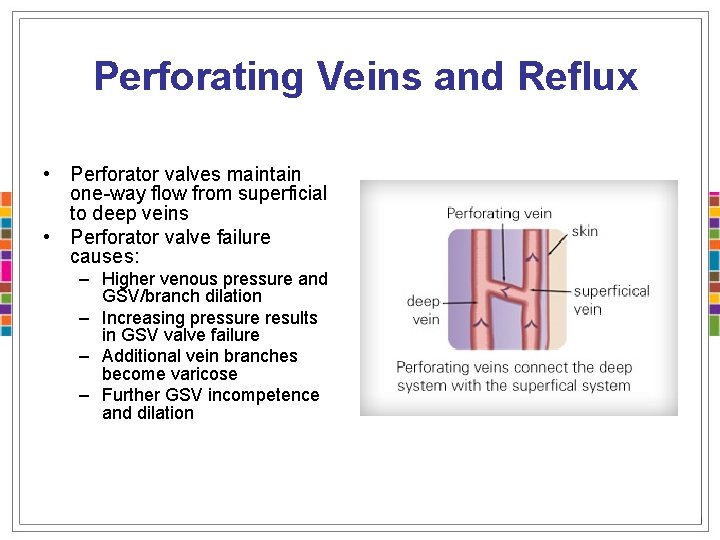
Perforating Veins and Reflux • Perforator valves maintain one-way flow from superficial to deep veins • Perforator valve failure causes: – Higher venous pressure and GSV/branch dilation – Increasing pressure results in GSV valve failure – Additional vein branches become varicose – Further GSV incompetence and dilation
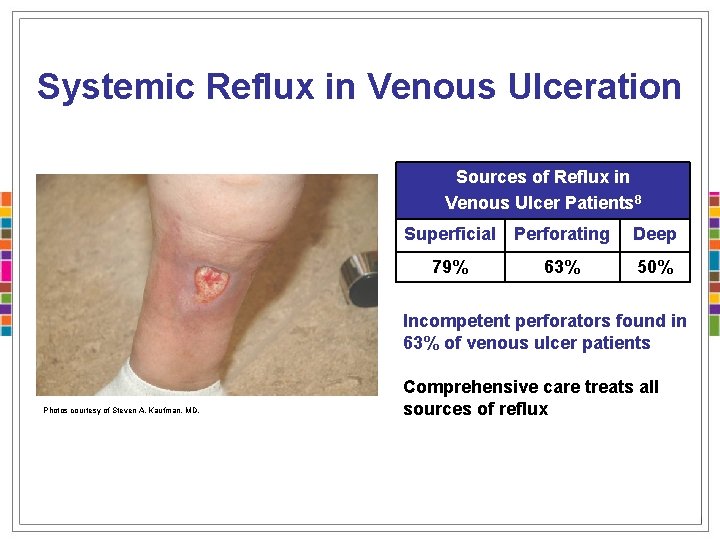
Systemic Reflux in Venous Ulceration Sources of Reflux in Venous Ulcer Patients 8 Superficial Perforating 79% 63% Deep 50% Incompetent perforators found in 63% of venous ulcer patients Photos courtesy of Steven A. Kaufman, MD. Comprehensive care treats all sources of reflux

VNUS Closure. RFS™ VNUS Closure. RFS Benefits: • Minimally invasive • Outpatient procedure • Quick patient recovery • Only device cleared by the FDA for the endovenous ablation of incompetent perforator veins Click graphic to play video

Venous Ulcer Patient Outcomes • Treating the underlying cause of venous ulceration results in improved clinical outcomes • Treating both the superficial and perforator hypertension results in: – Faster ulcer healing time – Lower ulcer recurrence rate than with compression therapy alone 9, 10
References 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. American Heart Association, SIR, Brand et al. “The Epidemiology of Varicose Veins: The Framingham Study” US Markets for Varicose Vein Treatment Devices 2006, Millennium Research Group 2005. Coon WW, Willis PW, Keller JB: Venous thromboembolism and other venous disease in the Tecumseh Community Health Study Circulation 1973; 48: 839 -846. Barron HC, Ross BA. Varicose Veins: A guide to prevention and treatment. NY, NY: Facts on File, Inc. [An Infobase Holdings Company]; 1995; vii. White JV, Ryjewski C. Chronic venous insufficiency. Perspect Vasc Surg Endovasc Ther 2005; 17: 319 -27 Dietzek A, Two-Year Follow-Up Data From A Prospective, Multicenter Study Of The Efficacy Of The Closure. FAST Catheter, 35 th Annual Veith Symposium. November 19, 2008. New York. Alameida JI. Lessons Learned After 2000 Endovenous Ablations. 34 th Veith Symposium. Nov 14 -18, 2007. New York Hanrahn L. et al. Distribution of valvular incompetence in patients with venous stasis ulceration. JVS 13, 6, 805 -812 June 1991 Jamie R Barwell, Colin E Davies, Comparison of surgery and compression with compression alone in chronic venous ulceration (ESCHAR study): randomized controlled trial, THE LANCET, Vol 363, June 04 Nelzen O. Fransson I. True long-term healing and recurrence of venous leg ulcers following SEPS combined with superficial venous surgery: a prospective study. Eur J Vasc Endovasc Surg 34, 605 -612 (2007)
- Slides: 27