Endometriosis By Lena Gowharji Ann is a 35
Endometriosis By… Lena Gowharji

• Ann, is a 35 year old lady, complaining of intermittent abdominal pain, bloating and sever dysmenorrhoea. She has a previous history of IBS, but recently noticed that her symptoms are all much worse in the week before her period. • On examination she is slim, the abdomen was distended, non tender, and no masses were felt. The uterus was anteverted, mobile and no abnormalities were found in the adnexia.

Endometriosis • Definition: Benign condition in which (hormone dependant) endometrial glands and stroma are present outside the uterine cavity and wall. • Its’ importance is due to its 1 - Distressing symptomatology 2 - Association with infertility 3 - Invasive potential (adjacent organs) 4 - Difficulty in being diagnosed

• Incidence: *Its estimated that 5 -15% of women have some degree of the disease. *1/3 of women with chronic pelvic pain have visualized endometriosis. *Its been noted in 5 -15% of women undergoing gynaecological laparotomies (an unexpected finding in 50% of these cases).

• Age: It classically presents in nulliparous infertile women in their 30 s. • However, it may occur at earlier ages (childhood and adolescents) and in such cases its associated with obstructive genital anomalies. • Following menopause, it regresses unless estrogen is prescribed. 5% of new cases develop in that age group.

• Pathogenesis: is not fully understood However 1 - genetic predisposition 2 - immunological changes have been reported to clearly play a role. • Several hypotheses have been used to explain the various manifestations of the disease and its various locations 1 - The Retrograde menstruation theory 2 - The Mullarian metaplasia theory 3 - The lymphatic spread theory 4 - The hematogenous spread theory

1 - The retrograde menstruation theory of Sampson: proposes that endometrial fragments that are shed during menstruation are transported through the fallopian tubes, then becoming implanted and growing in various intra-abdominal sites. (These endometrial fragments are viable and capable of growing in vivo and in vitro)

2 - The mullarian metaplasia theory of Meyer: proposes that endometriosis results from the metaplastic transformation of peritoneal mesothelium to endometrium under the influence of certain unidentified stimuli. 3 - The lymphatic spread theory of Halban: suggests that the lymphatics draining the uterus transport endometrial tissue to various pelvic site where it grows ectopically. *Endometrial tissue has been found in up to 20% of patients with the disease 4 - The haematogenous spread theory: explains the presence of endometrial tissue in distant sites (lung, axilla and forehead)

• Why don’t all menstruating women develop endometriosis? *It has be found that the amount of exposure to retrograde menstruation and the woman’s immunological response are most critical. *Researchers have found differences in the chemical composition and biological pathways of the endometrial cells in women who have endometriosis in comparison to those who don’t. They have also found a difference in the inflammatory mediators and growth factors in the peritoneal fluid of those with endometriosis in comparison to those without.

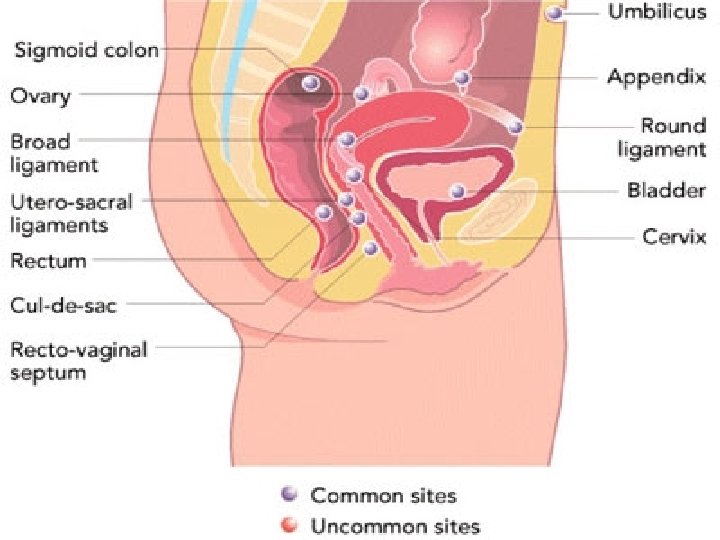
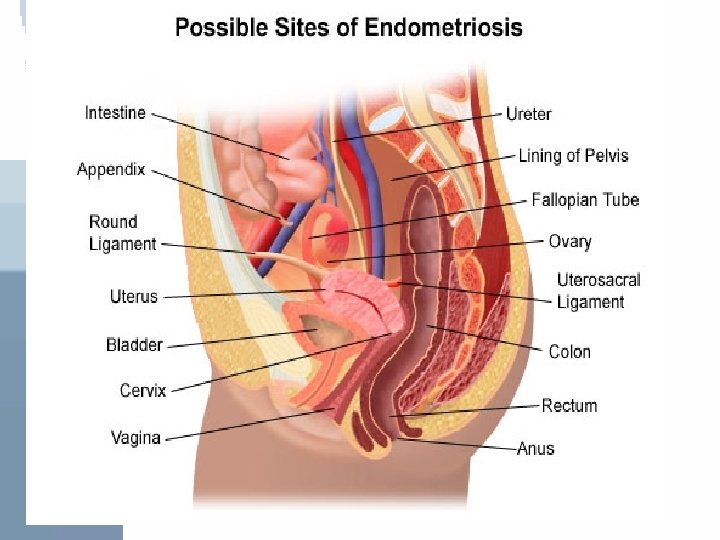
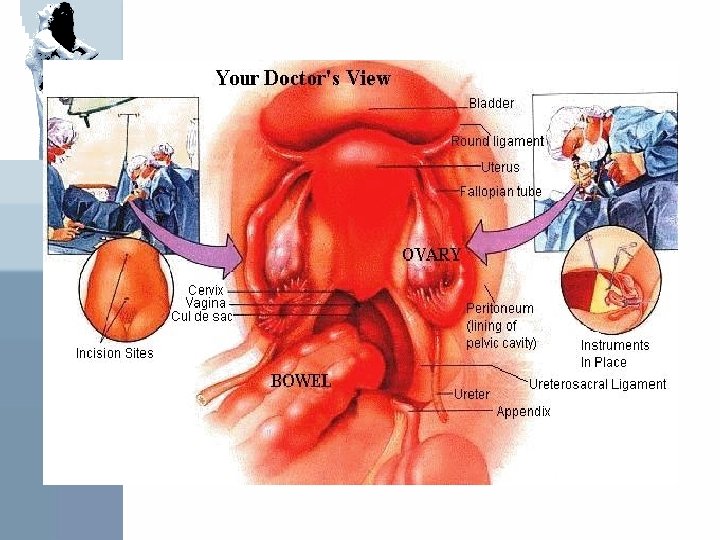
• Sites of occurrence: * Most commonly found in the dependant portions of the pelvis 1 - Ovaries (2 out of 3 women with endometriosis) 2 - Broad ligament 3 - Peritoneal surfaces of the cul-de-sac (uterosacral ligaments and post. Cervix) 4 - Rectovaginal septum * Quite frequently is the recto-sigmoid colon, appendix, and vesicouterine fold of the peritoneum involved. * Laparotomy scars esp. after c section or myomectomy or after the uterine cavity has been entered.

• Pathology: * The islands of endometriosis are sensitive to ovarian hormones. *Estrogen proliferation *Regression of corpus luteum and removal of estrogen and progesterone causes them to slough. *These sloughed debris induce a profound inflammatory response that causes significant pain and long term fibrosis.

• Macroscopical appearance: Depends on: site, size, time since implantation and day of the menstrual cycle. Colour is a good indicator and is determined by the vascularity of the lesion, the presence of fibrosis, the size of the lesion and the presence of residual sloughed material. It varies from red, brown, black, white-yellow. *Newer implants: red, blood filled active lesions *Older lesions: scarred with a puckered appearance.

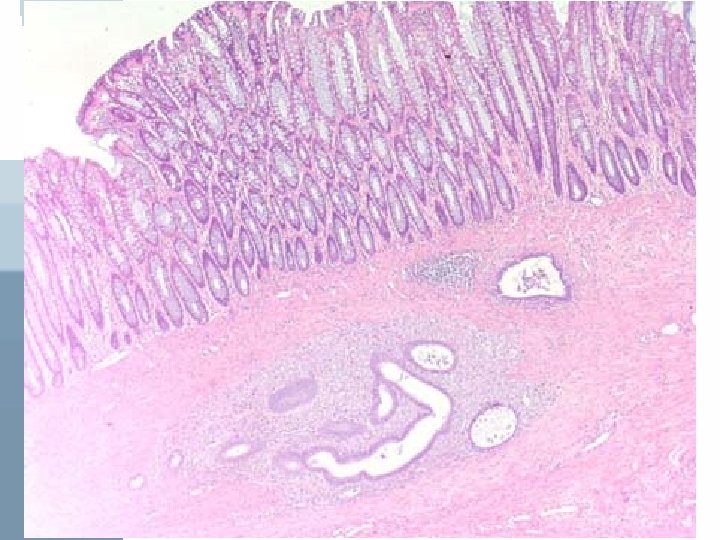
• Microscopically: 2 out of 4 must be present in the biopsied specimen to confirm Dx 1 - endometrial epithelium 2 - endometrial glands 3 - endometrial stroma 4 - hemosiderin laden macrophages

• Endometriosis of the Ovary: These are cysts filled with thick chocolate coloured fluid; which may have a black tarry consistency sometimes. * This characteristic fluid represents aged, haemolysed blood and desquamated epithelium. * The glands and stroma lining the cyst’s wall may be destroyed due to an increase in pressure. This leaves behind a fibrotic wall with infiltrating haemosiderin layden macrophages.

Risk factors for endometriosis: 1. Nulliparity. 2. Infertility. 3. Reproductive age (usually, late teens to 40 s). 4. A first-degree relative with endometriosis. 5. Regular menstrual cycle <27 days. 6. Prolonged menses of 8 or more days.

• Many patients are asymptomatic. • Others usually have no positive signs at examination.

The characteristic triad of symptoms: 1 - dysmenorrhea. 2 - dyspareunia. 3 - dyschezia.

Other symptoms: • Female reproductive tract: 1 - pre and postmenstrual spotting. 2 - cyclic pelvic pain. 3 - low sacral backpain (especially premenstually). 4 - infertility. 5 - diminished amount of menstrual flow. 6 - ovulatory pain and mid-cycle vaginal bleeding.

• If the Bladder is involved: 1 - cyclic hematuria/ dysuria. 2 - ureteric obstruction. • If the rectosigmoid colon is involved; 1 - premenstrual tensmus or diarrhea. 2 - obstruction.

Signs: • Tenderness on bimanual examination. • Tenderness or nodularity on the posterior vaginal fornix. • Uterosacral ligament tenderness or nodularity. • Cystic ovarian enlargement. • Fixation of adnexal structures. • Retroflexed uterus. • Episiotomy or cesarean section scars.

Differential diagnosis 1. Chronic pelvic inflammatory disease or recurrent acute salpingitis. 2. Hemorrhagic corpus luteum. 3. Benign or malignant ovarian neoplasm. 4. Ectopic pregnancy.

Diagnosis • History and examination • Pelvic U/S • Direct visualization of endometriotic lesions • Pathological examination of biopsy specimen Endometriosis in not a clinical diagnosis!

Diagnosis Suspected in afebrile patient with the characteristic triad: 1. Pelvic pain 2. Firm, fixed tender adnexal mass 3. Tender nodularity in cul-de-sac and uterosacral ligament

Diagnosis (CA 125) Frequently elevated in women with endometriosis Sensitivity only 20% to 30% Not used to diagnose endometriosis

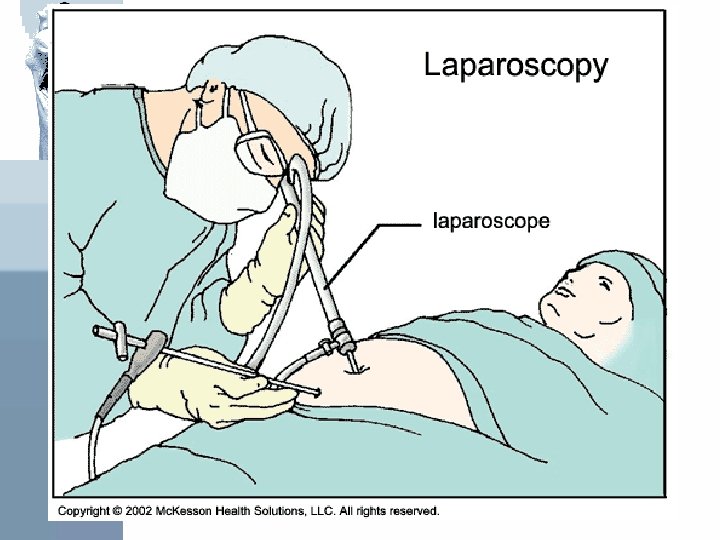
Diagnosis Definitive diagnosis is generally made by: • Characteristic gross • Histological findings Obtained by: Laproscopy or laprotomy Endometriosis in not a clinical diagnosis!
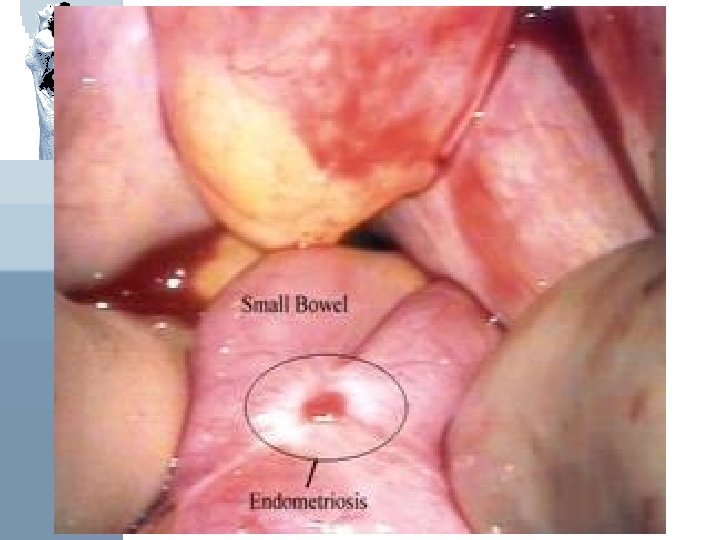

Diagnosis What do endometriosis lesions look like? • ‘’Classic’’ are red, dark brown, dark blue or black peritoneal implants • ‘’chocolate cysts’’ of the ovary • Clear vesicles • White or yellow spots or nodules • Normal appearing peritoneum (microscopic disease) • Later lesions appears as ‘’ powder burn’’ implants from thickened or scarred perilesional peritoneum
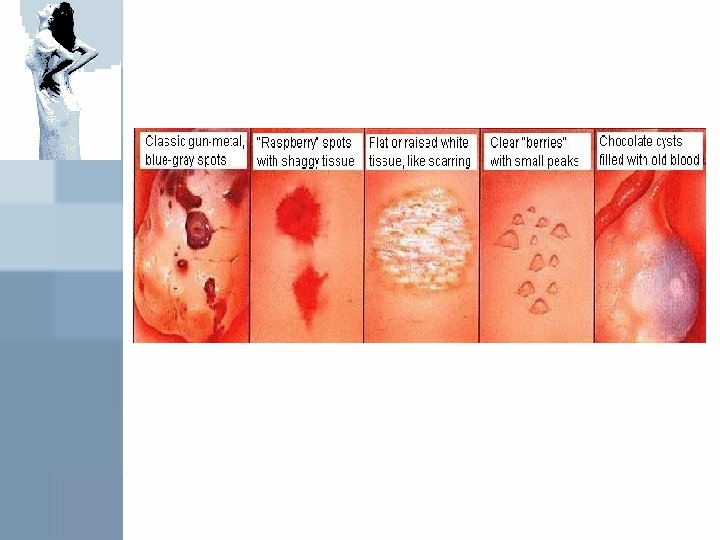
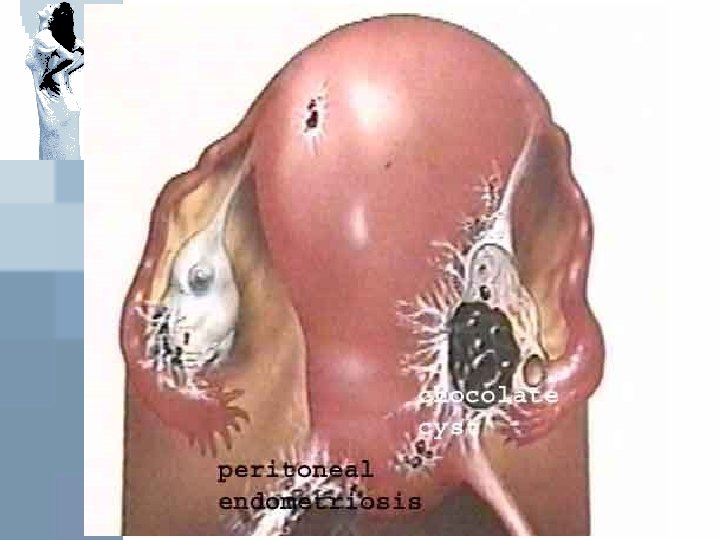
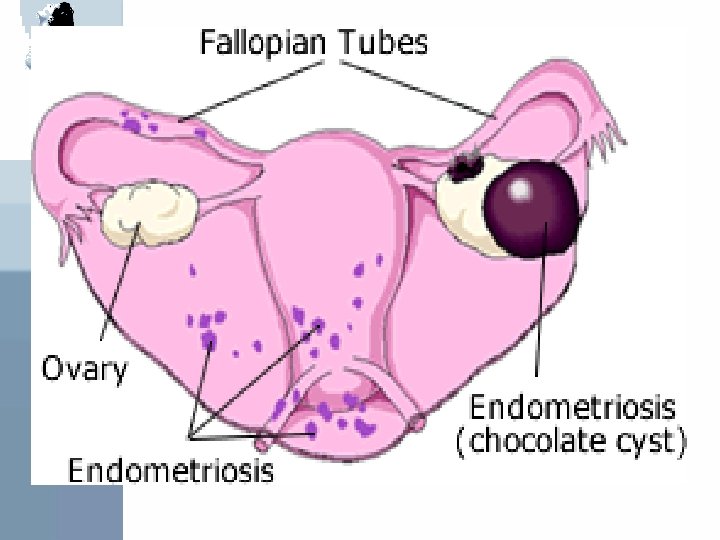

Diagnosis Unfortunately, even the most experienced surgoen may fail to identify endometriosis implants because: • The older implants may have a very subtle apperance • The deeper infiltration lesions may not be visible at the surface Biopsy of suspecious lesions improves diagnosis accuracy

Staging American Society of Reproductive Medicine (ASRM) Employs a staging protocol in an attempt to correlate Fertility potential with a quantified stage of endometriosis

Staging Initially started to be based on: 1 - Site of involvement 2 - extent of visualized disease And was modified to include: • Description of the color of the lesions • Percentage of surface involved in each lesion type • More detailed description of any endometriosis
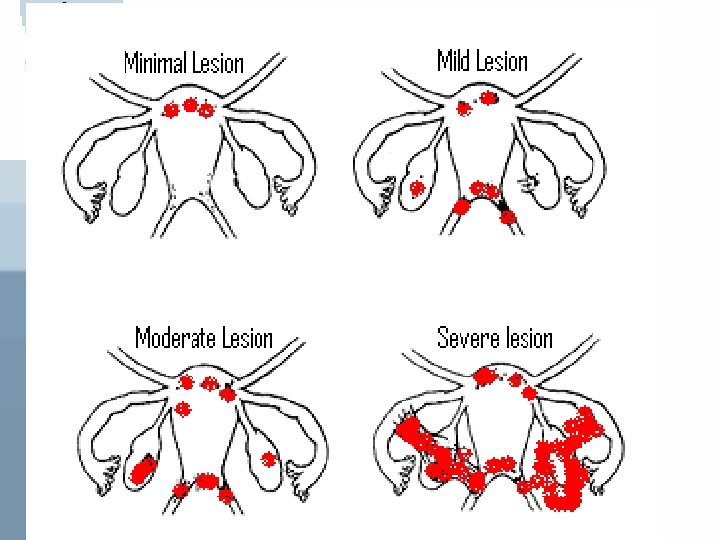
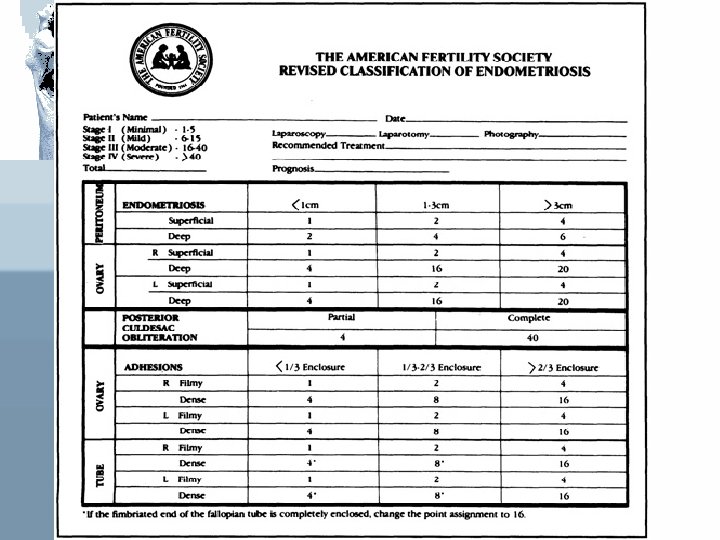
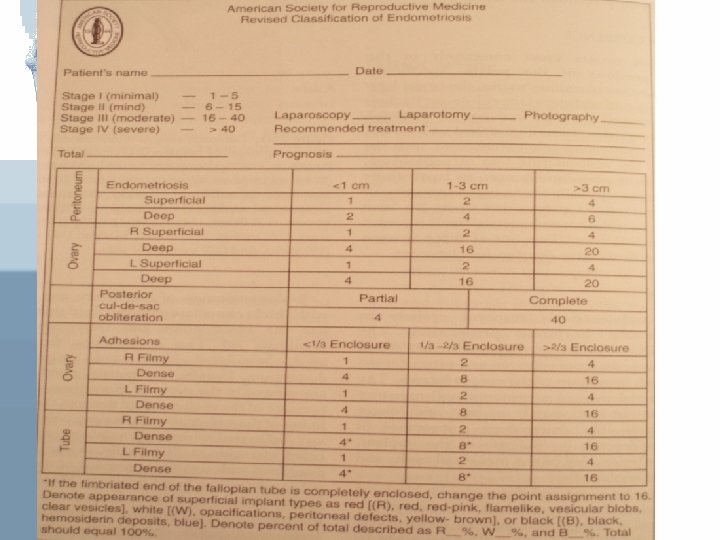

If the fimbriated end of fallopian tube is completely enclosed, change the point assignment to 16 Denote appearance of superficial implant type as RED [(R), red-pink, flamelike, vesicular blobs, clear vesicles] WHITE [(W), opicifications, peritoneal defect, yellow-brown] BLACK [(B), black, hemosiderin deposits, blue] Denote % of total described as R__%, W__%, B__%

Treatment 1. 2. 3. 4. 5. No treatment Non-hormonal treatment Hormonal treatment Surgical treatment Radiological treatment

I. No treatment • If small symptom less lesions • Patient observed & examined every 6 months

II. Non-hormonal treatment • If small lesions with mild symptoms • Analgesics are given for pain • Prostaglandin inhibitors (naproxen, ibuprofen) are given for pain and menorrhagia

III. Hormonal treatment Indications: 1. Severe symptoms with small pelvis lesions 2. Recurrence of symptoms after conservative surgery 3. May be given for a short time (6 -12 weeks) before surgery to make dissection easier 4. After conservative surgery to allow any residual lesion to regress 5. When operation is contraindicated or refused by the patient

1. Pseudo pregnancy • Ovulation and menstruation are inhibited for 9 months (6 -18 months) using a combined OCP or a progestogen alone to avoid the oestrogenic side effects • A combined contraceptive tablet is given daily • Oral medroxyprogesterone acetate (provera tablets) is givin in a dose of 1030 mg daily • Side effects of progestogens: headache, weight gain, fluid retention, breakthrough bleeding and depression

2. Pseudo menopause Danazol: • given orally 400 -800 mg/day for 6 -9 months • Weak synthetic androgen • Side effects: 1. Androgenic effects: acne, male alopecia, hirsutism, hoarseness of voice & hypertrophy of clitoris 2. Hypo-oestrogenic effects: hot flushes, sweating, atrophy of breasts, atrophic vaginitis, dry vagina, dyspareunia & decreased libido 3. Anabolic effects: weight gain & edema 4. Metabolic effects: impaired glucose tolerance, increased insulin requirements in diabetic cases, hepatic dysfunction. Blood pressure may be elevated 5. CNS: headache, sleep disorders, anxiety, depression & visual disturbance 6. GIT: nausea, vomiting & constipation 7. Muscloskeletal: muscle cramps & swelling of joints 8. Genitourinary: hematuria

2. Pseudo menopause Gn. RH (agonist): • Nafarelin (synarel): intranasally using a nasal spray, 200 micrograms twice daily • Goserelin (zoladex): 3. 6 mg injected SC every 4 weeks • Triptorelin ( decapeptyl): 3. 75 mg injected IM every 4 weeks • Side effects: hot flushes, dryness of the vagina, dyspareunia & reduced libido

3. Mifepristone 50 mg/day for 6 months

IV. Surgical treatment Indications: 1. Large lesions 2. When hormonal therapy fails • Surgery is conservative or radical

1. Conservative surgery • If young patients below 40 years • Pre-sacral neurectomy has been used to treat severe dysmenorrhea • Minimal to mild disease – can be removed by laser or electrocautery

2. Radical surgery • Patient above 40 years • Treatment is total hysterectomy & bilateral salpingo-oophorectomy
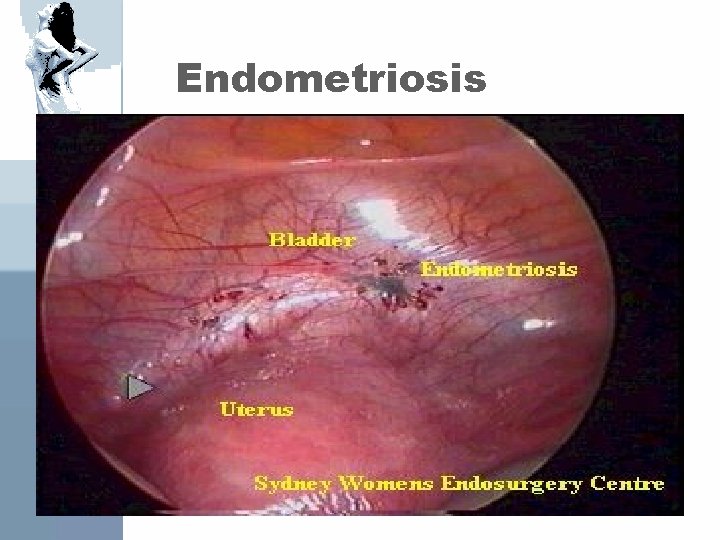
Endometriosis
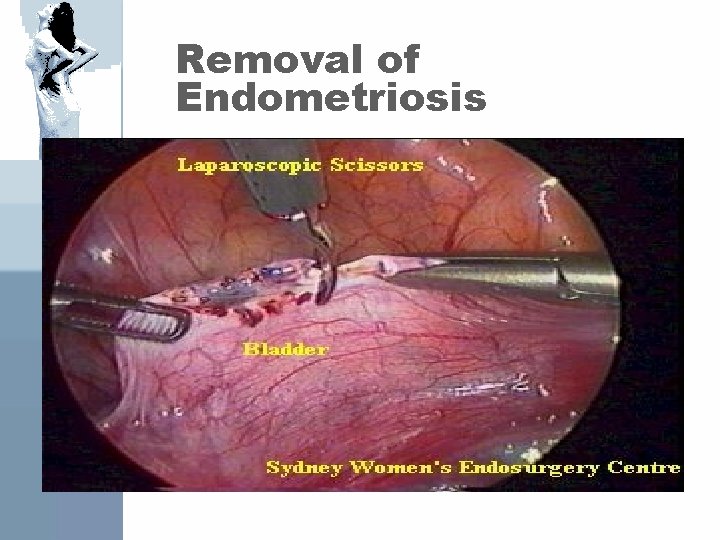
Removal of Endometriosis
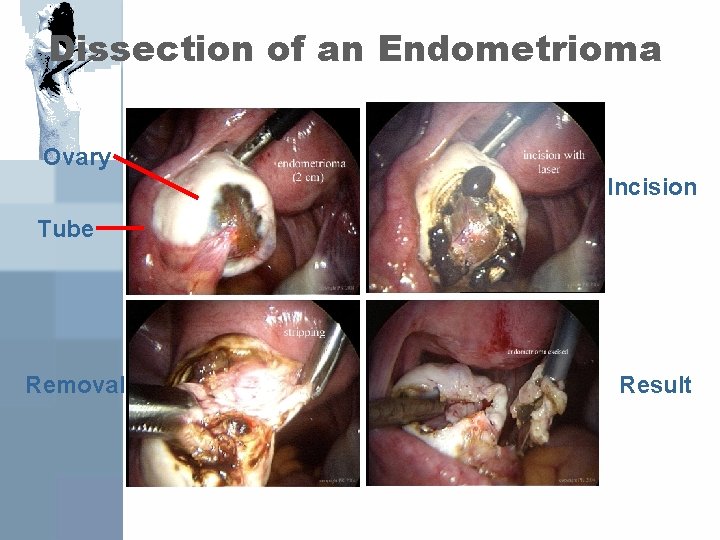
Dissection of an Endometrioma Ovary Incision Tube Removal Result

V. Radiological treatment • Induction of artificial menopause by external pelvic radiation cures the condition by causing atrophy of endometrial tissue • It is applied only in patients above 40 in whom operation can’t be done as in case of wide spread pelvic endometriosis (frozen pelvis) or endometriosis of the rectovaginal septum which is difficult to excise surgically

Thank you
- Slides: 58