Endometrial Cancer ASSOCIATE PROFESSOR Iolanda Blidaru MD Ph

Endometrial Cancer ASSOCIATE PROFESSOR Iolanda Blidaru MD, Ph. D
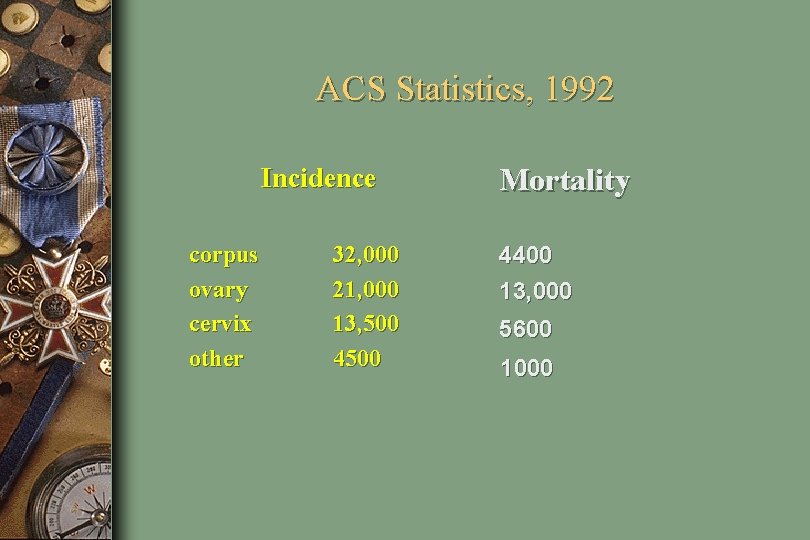
ACS Statistics, 1992 Incidence corpus ovary cervix other 32, 000 21, 000 13, 500 4500 Mortality 4400 13, 000 5600 1000

Epidemiology. Physiopathology. Two different pathogenetic types of endometrial cancer 1. Estrogendependent tumors u u unopposed E exposure, hyperplasia of the endometrium as initial step, younger perimenopausal women, better differentiated, better prognosis. 2. Estrogen-independent tumors unopposed E exposure uno association with hyperplasia of the endometrium; arise on atrophic endometrium u. Older, postmenopausal, thin women uless differentiated

Risk Factors u Age u Hyperestrogenism (ERT, COC, Tamoxifen) u Nulliparity / Infertility u Obesity, Hypothyroidism, Hypertension u Menstrual characteristics (nulliparity, early menarche, late menopause) u Diabetes u Atypical Hyperplasia u Others: smoking, dietary factors

Preinvasive Lesions = Endometrial Hyperplasia u Simple Hyperplasia u Complex Hyperplasia u Atypical Hyperplasia: simple / complex (dg. endometrial biopsy, D+C, total hysterectomy) u Treatment: progestins (MPA), hysterectomy, Gn. RH-a

Endometrial carcinoma Histopathology u Endometrioid Adenocarcinoma (80%): G 1, G 2, G 3; ER, PR. u Papillary Serous Adenocarcinoma u Clear Cell Adenocarcinoma u Squamous Cell Carcinoma u Sarcomas (malignant mixed Mullerian tumors, leiomyosarcoma, endometrial stromal sarcoma)

Clinical findings and diagnosis uuterine bleeding in postmenopausal patients (90%) u recurrent intermenstrual bleeding (over 40 years) u atrophic vaginitis u the uterus +/- enlarged, +/- fixed (parametrial, adnexial and/or intraperitoneal spread) u hematometria or pyometria

u. Any genital bleeding occuring during postmenopause must be investigated to exclude endometrial carcinoma.

Investigations u Endometrial method biopsy - the diagnostic endometrial lavage, aspiration cytology, cytology from endocervix and posterior vaginal fornix, hysteroscopy u US, MRI (uterine invasion, lymph node involvement) u Estrogen and progesterone receptors u u Chest X-ray, computed tomography of the abdomen, urography, Routine blood counts, urinalysis, sigmoidoscopy, liver function tests, blood urea nitrogen, serum creatinine, glycemia

Differential diagnosis u leiomyoma, endometrial hyperplasia with DUB, cervical polyps u cervical, tubal, ovarian carcinoma u atrophic vaginitis u in the premenopausal patient complications of early pregnancy
Staging: Surgical

Endometrial CA Staging STAGE I (Add tumor grade to each stage) Ia Ib Ic Limited to endometrium <1/2 myometrial thickness >1/2 myometrial thickness
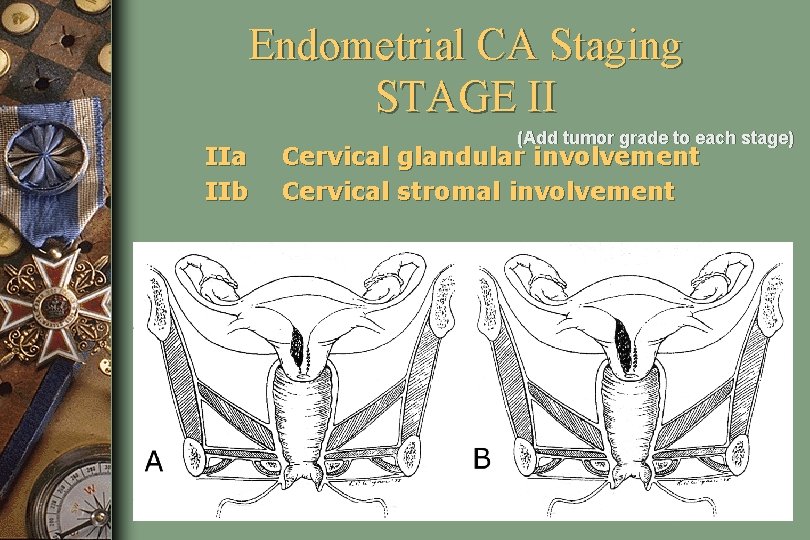
Endometrial CA Staging STAGE II IIa IIb (Add tumor grade to each stage) Cervical glandular involvement Cervical stromal involvement
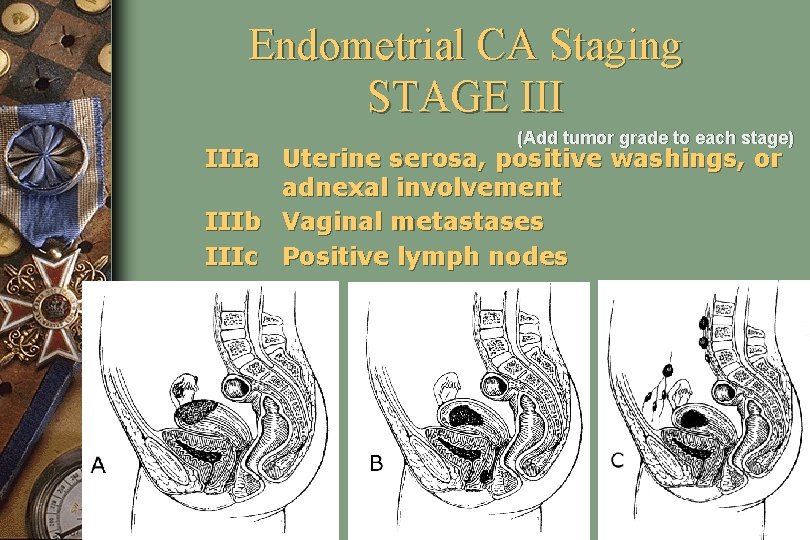
Endometrial CA Staging STAGE III (Add tumor grade to each stage) IIIa Uterine serosa, positive washings, or adnexal involvement IIIb Vaginal metastases IIIc Positive lymph nodes
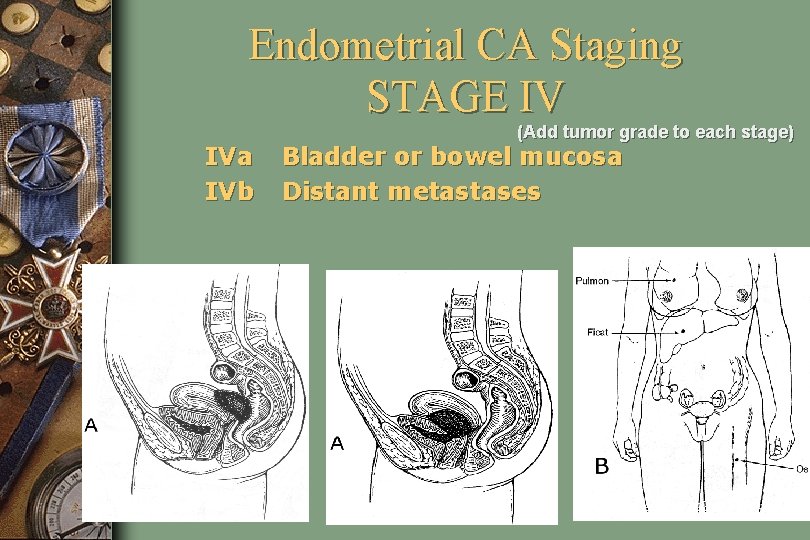
Endometrial CA Staging STAGE IV IVa IVb (Add tumor grade to each stage) Bladder or bowel mucosa Distant metastases

Treatment of Endometrial Adenocarcinoma: u Surgery → staging in majority of patients Extrafascial total abdominal hysterectomy / Bilateral salpingooophorectomy, peritoneal washings, +/LND (lymphadenectomy) u RT u Progestins u Chemotherapy

Radical Hysterectomy u Removes corpus, cervix, parametria, upper third of vagina u Uterine arteries divided at origin u Ureters dissected through tunnel u Uterosacral ligaments divided near rectum u Typically combined with LND u Oophorectomy mandated

Treatment of Endometrial Adenocarcinoma: u Surgery u Radiotherapy u u -Adjuvant RT for high-risk patients postoperatively -No adjuvant RT if Ia, G 1 -2 with favorable histology -The only treatment in patients with inoperable stage I and stage II disease Progestins Chemotherapy

Complications of Radiation Therapy Acute: u Perforation u Fever u Diarrhea u Bladder spasm u Chronic: u Proctitis u Cystitis, u Fistula u Enteritis UTI

High-Risk Patients u Deep myometrial invasion u Positive nodes u Grade 3 tumor u Clear cell, papillary serous, squamous or undifferentiated histologies u Positive peritoneal cytology u Other extra-uterine spread

Primary Treatment of Uterine Sarcoma u Surgical staging u Single-agent chemotherapy, depending on histology and stage (ADR = adriamycin for leiomyosarcoma, endometrial stromal sarcoma; IFX = ifosfamide for malignant mixed Mullerian tumors) u RT does not appear to alter survival
- Slides: 21