Endocrine system Fatima Obeidat MD Department of Pathology

Endocrine system Fatima Obeidat, MD Department of Pathology and Laboratory Medicine

I. Thyroid diseases

I. Thyroiditis 1. Chronic Lymphocytic (Hashimoto) Thyroiditis - Is the most common cause of hypothyroidism in developed countries where iodine levels are sufficient. - It is characterized by gradual thyroid failure secondary to autoimmune destruction of the thyroid gland

- It is most prevalent between the ages of 45 and 65 years and is more common in women - It can affect children

Clinically , 1. Painless thyroid enlargement 2. In the usual clinical course, hypothyroidism develops gradually.

Hashimoto thyroiditis. Gross

2. Subacute Granulomatous (de Quervain’s) Thyroiditis - Is much less common than Hashimoto disease - More frequently in women than in men. - Is believed to be caused by a viral infection and a majority of patients have a history of an upper respiratory infection just before the onset of thyroiditis.

Clinical Features : - Acute onset characterized by neck pain ( with swallowing) , fever, and malaise. - - The leukocyte count is increased. - It is self-limited, with most patients returning to a euthyroid state within 6 to 8 weeks

3. Subacute Lymphocytic Thyroiditis : - Also is known as silent or painless thyroiditis. - And in a subset of patients the onset of disease follows pregnancy (postpartum thyroiditis).

4. Riedel thyroiditis, : - A rare disorder of unknown etiology, - Characterized by extensive fibrosis involving the thyroid and contiguous structures simulating a thyroid neoplasm clinically

Riedel thyroiditis - Clinically

Riedel thyroiditis-Gross

II. GRAVES DISEASE - It is characterized by a triad of manifestations: A. Thyrotoxicosis. - Caused by a diffusely enlarged, hyperfunctional thyroid, is present in all cases.
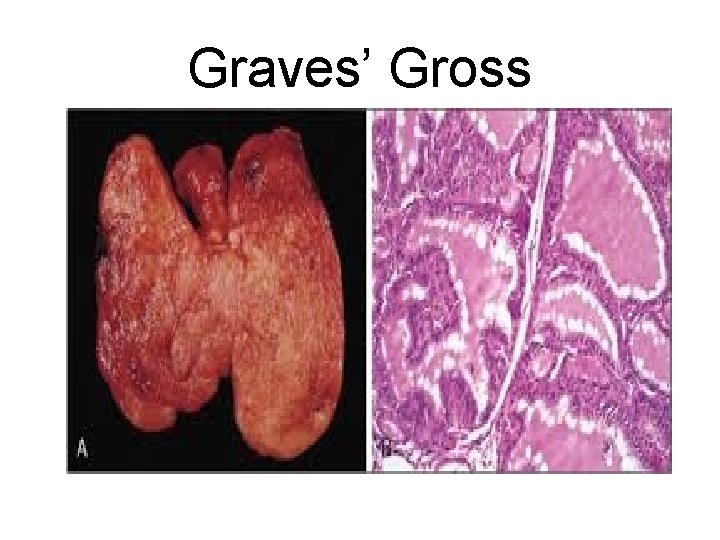
Graves’ Gross

B. Infiltrative ophthalmopathy with resultant exophthalmos in 40% of patients as a result of increased volume of the retroorbital connective tissues C. Infiltrative dermopathy –pretibial myxedema of skin – in about 10% of the cases

Exophthalmos
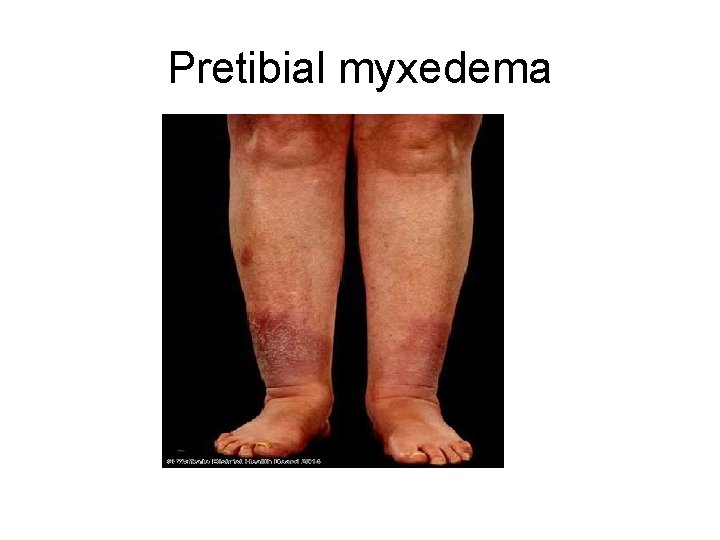
Pretibial myxedema

Laboratory findings in Graves’ disease - Elevated serum free T 4 and T 3 and depressed serum TSH

III. DIFFUSE AND MULTINODULAR GOITER - Enlargement of the thyroid, or goiter, is the most common manifestation of thyroid diseases.

Goiters can be endemic or sporadic. 1. Endemic goiter : - Occurs in geographic areas where the soil, water, and food supply contain little iodine. - The term endemic is used when goiters are present in more than 10% of the population in a given region.

2. Sporadic goiter : - Less common than endemic goiter. - Peak incidence in puberty or young adulthood, when there is an increased physiologic demand for T 4. - It may be caused by several conditions, including :

a. Ingestion of substances that interfere with thyroid hormone synthesis , such as excessive calcium and vegetables such as cabbage, and cauliflower.

Endocrine Pancreas Diabetes Mellitus

Laboratory studies: - Normal blood glucose levels are maintained in a very narrow range, usually 70 to 120 mg/d. L. - Diabetes Mellitus is diagnosed by any one of three criteria: 1. A random blood glucose concentration of 200 mg/d. L or higher, with classical signs and symptoms

2. A fasting glucose concentration of 126 mg/d. L or higher on more than one occasion 3. An abnormal oral glucose tolerance test (OGTT), in which the glucose levels is 200 mg/d. L or higher 2 hours after a standard carbohydrate load (75 g of glucose).

Notes: a. Persons with serum fasting glucose values < 110 mg/d. L, or < 140 mg/d. L for an OGTT, are considered euglycemic b. Those with fasting glucose > 110 but < 126 mg/d. L, or OGTT values of >140 but < 200 mg/d. L, have impaired glucose tolerance, known as prediabetes

Classification of Diabetes Mellitus TYPE 1 Diabetes : - It accounts for 10% of all cases - Is an autoimmune disease destructing pancreatic β cell leading to an absolute deficiency of insulin

- Most commonly develops in childhood, becomes manifest at puberty, and patients depend on exogenous insulin for survival; without insulin they develop complications - The classic manifestations of the disease occur late in its course, after 90% of the beta cells have been destroyed

Type 2 diabetes : - Accounts for 80% to 90% of cases - Caused by a combination of a. Peripheral resistance to insulin action b. An inadequate compensatory response of insulin secretion by βcells (relative insulin deficiency)

Pathogenesis : -Is a complex multifactorial disease. 1. Environmental factors, such as a sedentary life style and dietary habits 2. Genetic factors are also involved ,

. Long term complications of Diabetes : - There is extreme variability among patients in the time of onset , severity, and the particular organs involved but in persons with tight control of their diabetes, the onset may be delayed.

Morphology and clinical manifesations of complications 1. Diabetic Macrovascular Disease. : - The hallmark is accelerated atherosclerosis affecting the aorta , large and medium-sized arteries

Note; - Myocardial infarction due to Coronary artery atherosclerosis is the most common cause of death in diabetics - Gangrene of the lower extremities is 100 times more common in diabetics than in the general population

2. Diabetic Microangiopathy. : - Diffuse thickening of basement membranes, is most evident in the capillaries of the skin, skeletal muscle, retina and , renal glomeruli, - Despite the increase in the thickness of basement membranes, diabetic capillaries are more leaky than normal to plasma proteins.

- It underlies the development of diabetic nephropathy, retinopathy , and some forms of neuropathy - An indistinguishable microangiopathy can be found in aged nondiabetic patients,

3. Diabetic Nephropathy. : - Renal failure is second only to myocardial infarction as a cause of death from this disease :

Diabetic nephropathy, clinically - The earliest manifestation is the appearance of small amounts of albumin in the urine (> 30 but < 300 mg/day-( microalbuminuria). - Without specific interventions, some patients will develop overt nephropathy with macroalbuminuria (excretion of more than 300 mg/day) over the succeeding 10 to 15 years,

4. Ocular Complications of Diabetes: - DM currently is the fourth leading cause of acquired blindness in the United States and visual impairment, and blindness, is one of the morefeared consequences of longstanding DM. - Retinopathy, the most common pattern, consists of changes that are considered by many ophthalmologists to be virtually diagnostic of the disease

5 Diabetic Neuropathy. : - The most frequent pattern of involvement is that of a peripheral, symmetric neuropathy of the lower extremities affecting motor and sensory nerves particularly the latter and other forms include - Autonomic neuropathy produces disturbances in bowel and bladder function and sometimes sexual impotence,

Note - Glycemic control is assessed clinically by measuring the percentage of glycosylated hemoglobin, also known as Hb. A 1 C, which is formed by non-enzymatic addition of glucose moieties to hemoglobin in red cells.

- Hb. A 1 C is a measure of glycemic control over long periods of time (2 to 3 months) and is relatively unaffected by day-to-day Variations and an Hb. A 1 C below 7% is taken as evidence of tight glycemic control,
- Slides: 41