ENDOCRINE PANCREAS o Diabetes Mellitus o Islet Cell

ENDOCRINE PANCREAS

o Diabetes Mellitus o Islet Cell tumors

INTRODUCTION o One million islets of Langerhans o Several types of cells “Immunohistochemistery” n ß (beta) -> 70% insulin n А (alpha)-> 20% glucagons n D (delta) -> 5 -10% somatostatin n P. P Cell -> 1 -2% pancreatic polypeptide n Other rare cells: D 1 cells VIP ( vasoactive intestinal polypeptide ) Enterochromaffin cells 5 HT-(serotonin) - - -
o Each type of pancreatic islet cells may give mainly benign tumour -> (ADENOMA) called Islet cell tumours: Insulinoma Glucagonoma Somatostatinoma VIPoma Carcinoid tumours Gastrinoma n Multiple Endocrine Neoplasia (MEN)
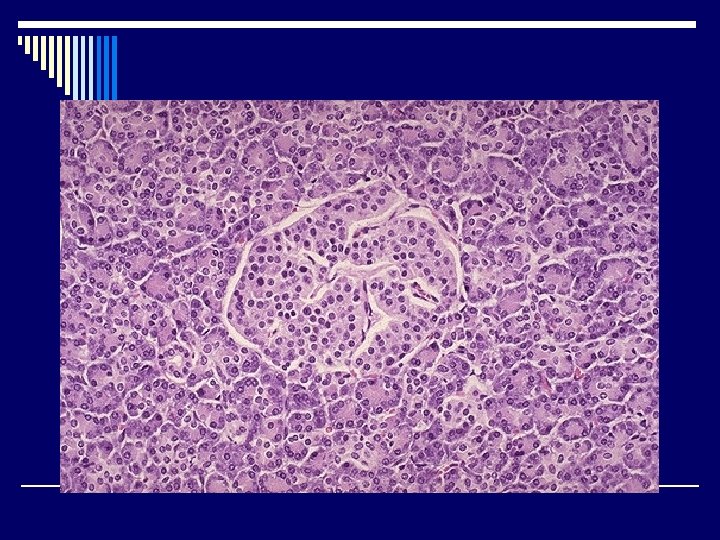
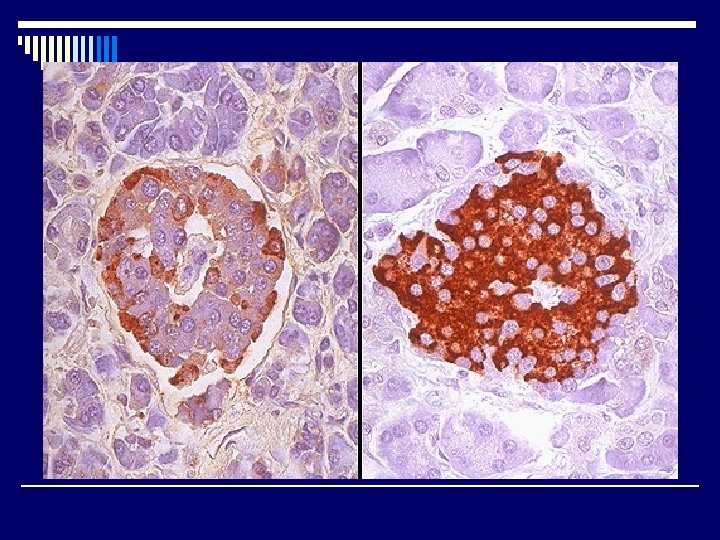

DIABETES MELLITUS

DEFINITION o Diabetes Mellitus is a chronic disorder of carbohydrate, fat, and protein metabolism. o In which there is impaired glucose utilization due to defective or deficient insulin secretory response inducing hyperglycemia

CLASSIFICATION o Primary (idiopathic) Diabetes Mellitus n Type-1 (Insulin Dependent Diabetes Mellitus) p Type-1 A (immune mediated) p Type-1 B (idiopathic) n Type-2 (Non-insulin Dependent Diabetes Mellitus) p* Non-obese NIDDM p * Obese NIDDM p * Maturity onset diabetes of the young (MOD) p * Gestational DM

o Secondary Diabetes Mellitus: - Chronic pancreatitis p- Post pancreatectomy p- Hormonal tumours (acromegaly, Cushing’s ---) p- Drugs (corticosteroids) p- Haemochromatosis p- Genetic disorders e. g. lipodystrophy p- Gestational DM p

Primary Diabetes Mellitus is by far the most common in our countery and worldwide. Type 1 and type 2 have different pathogenetic and metabolic characeristics. Simillar long term comlications occur in both types.

o MODY (maturity-onset DM of the Young): n n n Young Rare Linked to chrom. 7 & 20 Autosomal dominant Mild hyperglycemia

o ACUTE METABOLIC COMPLICATIONS:

Diabetic Ketoacidosis coma: n n In Type I Diabetes Mellitus Due to severe insulin deficiency with increase glucagons. Decrease insulin lipolysis free fatty acids Increase Glucagon oxidation of FFA in liver Ketoacidosis Coma

Non ketotic Hyperosmolar Coma: n n n In Type II DM (NIDDM) Elderly Uncontroled DM Sustained hyperglycemic diuresis Severe dehydration coma Lack of symptoms (nausea, vomiting and respiratory difficulties) Delay the seeking of medical attention. o Hypoglycemia Coma

Morphology & Late Complications o Depends on : n n n - Duration - Metabolic control - Genetic factors

o Microangiopathy: Thickening of basement membrane PAS + Advanced glycosylation end product. n - Renal Glomeruli ( (nephropathy n - Retina ( (retinopathy n - Nerves (neuropathy)

o Atherosclerosis: n n - Myocardial infarction Cerebral stroke. Aortic aneurysm. Gangrene of lower extremities


o Neuropathy: n n n - Symmetric peripheral neuropathy. - Sexual impotence. -Bowel and bladder dysfunction.

Diabetic Nephropathy Glomerular involvement : o 1. 2. Diffuse glomerulosclerosis. Nodular glomerulosclerosis “ Kimmel. Stiel – Wilson lesion ” Nephrotic Syndrome Arteriolosclerosis: Pyelonephritis (acute & chronic) o o n * Necrotizing papillitis.

Diabetic Ocular complications: o - Retinopathy : n Non – proliferative retinopathy ( hemorrhage, oedema, exudates microaneurysms and microangiopathy) n Proliferative retinopathy Neovascularization and fibrosis blindness (macula ) o - Vitrous hemorrhage. o - Cataract formation. o - Glaucoma *Diabetes Mellitus are more susceptible to infection.

ISLET CELL TUMOURS o Rare o Adult o Multiple / solitary o May be functional o Mainly benign / can be malignant
ISLET CELL TUMOURS Three Syndromes: 1. Hyperinsulinism & hypoglycemia : n n (insulinoma) of Beta cells solitary adenomas multiple Can be malignant
ISLET CELL TUMOURS 2. Zollinger – Ellison Syndrome (Gastrinoma) n n - Multiple ulcer disease - Gastric hypersecretion - Islet cell tumour Malignant 60% & benign 40% 3. MEN (1, 2 A, 2 B)
- Slides: 27