ENDOBRONCHIAL BRACHYTHERAPY AS A PALLIATIVE INTERVENTION reviewing 20

ENDOBRONCHIAL BRACHYTHERAPY AS A PALLIATIVE INTERVENTION: reviewing 20 years of experience in an Australian centre Matthew Knox MBBS(Hons) Andrej Bece MBBS BApp. Sci(Hons) FRANZCR Joseph Bucci MBBS FRACP FRANZCR John Moses MBBS(Hons) FRACP Peter Graham MBBS FRANZCR Grad. Cert(Bioethics) Grad. Dip(Med. Stats)
ENDOBRONCHIAL BRACHYTHERAPY (EBB) Historic Indications § Sole curative treatment for localised endobronchial lesions § Concurrent first-line curative treatment with EBRT as a “boost” § Palliation of symptoms (with or without bronchial stenting/laser therapy/ cryotherapy/etc. )

“…EBRT alone is more effective for palliation than EBB alone… “ “. . . For patients previously treated by EBRT and who are symptomatic… EBB should be considered in selected cases. ” Reveiz L, Reuda JR, Cardona AF. Palliative endobronchial brachytherapy for NSCLC. Cochrane Database Syst Rev. Dec 2012; 12: CD 004284

DYSPNOEA (ACUTE OR CHRONIC) Up to 69% of patients with advanced lung cancer PERSISTENT COUGH Up to 86% of all lung cancer patients HAEMOPTYSIS Up to 20% of all lung cancer patients Farbicka P, Nowicki A. Palliative care in patients with lung cancer. Contemp Oncol. 2013; 17(3): 238 -45

AIM OF RESEARCH Aims § Characterise the EBB program at St George Hospital § Demonstrate the efficacy of EBB in alleviating symptoms in a select patient group § Promote EBB as a valuable and relevant option for the palliative management of lung cancer

METHODS Study Design Analysis § Retrospective audit of 95 EBB cases in 86 patients § Response defined as clinical improvement in presenting symptom(s) § Electronic and paper files § Review of all EBB cases occurring at St George Hospital (1997 -2016) § Both inpatient and outpatient settings § Primarily descriptive results § All further comparative analyses of categorical data involved chi-square calculations
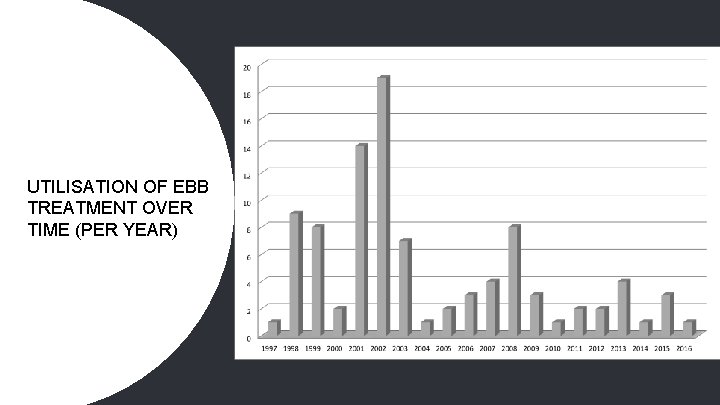
UTILISATION OF EBB TREATMENT OVER TIME (PER YEAR)
RESULTS - DEMOGRAPHICS Results Gender Female = 30 (32%) Male = 65 (68%) Age [mean (range)] 68. 73 (31 - 88) Tumour Origin Primary Lung = 69 (73%) Metastatic = 26 (27%) Histology [most common] Squamous Cell Carcinoma (lung) Poorly Differentiated Large Cell Carcinoma (lung) Adenocarcinoma (lung) Metastatic Adenocarcinoma Metastatic Squamous Cell Carcinoma Other 33 (35%) 17 (18%) 12 (13%) 3 (3%) 13 (14%) Indication for EBB Haemoptysis Obstruction Residual Disease 26 (27%) 77 (81%) 6 (6%) Lost to Follow-Up 13 (14%)
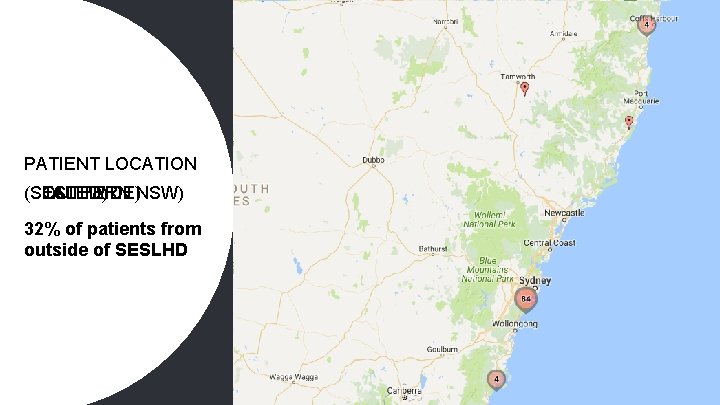
PATIENT LOCATION (SOUTHERN NSW) (SESLHD) (STATEWIDE) 32% of patients from outside of SESLHD

RESULTS – CHARACTERISE PREVIOUS EBRT All EBRT Treatments Previous EBRT 84 (88%) Time to EBB (months) [mean (range)] 18. 04 (0 -> 91) When EBRT first (N=67) Time to EBRT (months) [mean (range)] 1. 6 (0 -> 8) When EBB first (N=10) Type of EBRT Dosage by Type (Gy) [median (range)] Radical EBRT Palliative EBRT 38 (48%) 41 (52%) 60. 5 (50 --> 66) 30 (7. 5 --> 48)
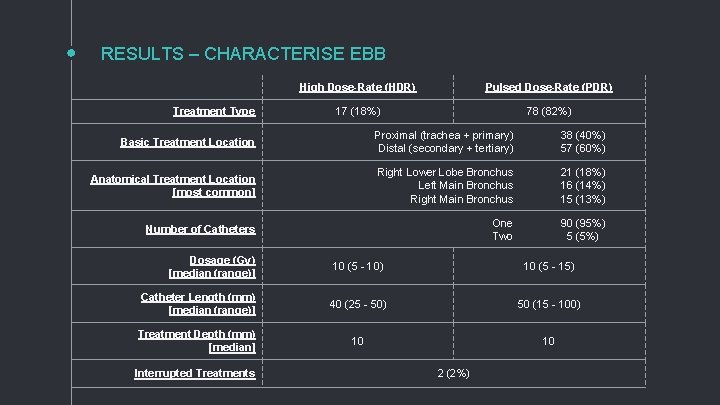
RESULTS – CHARACTERISE EBB Treatment Type High Dose-Rate (HDR) Pulsed Dose-Rate (PDR) 17 (18%) 78 (82%) Basic Treatment Location Proximal (trachea + primary) Distal (secondary + tertiary) 38 (40%) 57 (60%) Anatomical Treatment Location [most common] Right Lower Lobe Bronchus Left Main Bronchus Right Main Bronchus 21 (18%) 16 (14%) 15 (13%) Number of Catheters One Two 90 (95%) 5 (5%) Dosage (Gy) [median (range)] 10 (5 - 10) 10 (5 - 15) Catheter Length (mm) [median (range)] 40 (25 - 50) 50 (15 - 100) Treatment Depth (mm) [median] 10 10 Interrupted Treatments 2 (2%)
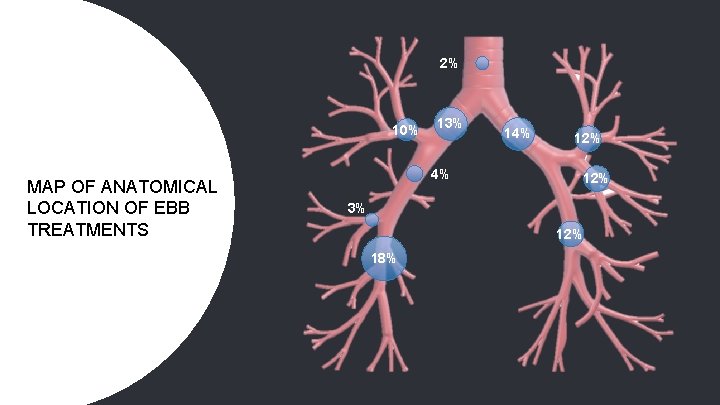
2% 10% MAP OF ANATOMICAL LOCATION OF EBB TREATMENTS 13% 4% 12% 12% 3% 12% 18%
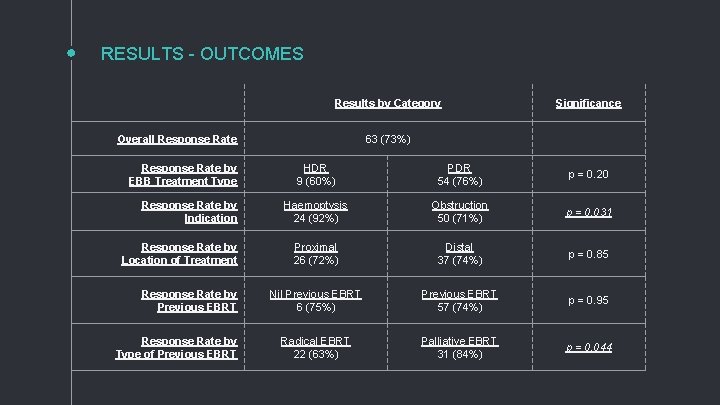
RESULTS - OUTCOMES Results by Category Overall Response Rate by EBB Treatment Type Response Rate by Indication Response Rate by Location of Treatment Response Rate by Previous EBRT Response Rate by Type of Previous EBRT Significance 63 (73%) HDR 9 (60%) PDR 54 (76%) p = 0. 20 Haemoptysis 24 (92%) Obstruction 50 (71%) p = 0. 031 Proximal 26 (72%) Distal 37 (74%) p = 0. 85 Nil Previous EBRT 6 (75%) Previous EBRT 57 (74%) p = 0. 95 Radical EBRT 22 (63%) Palliative EBRT 31 (84%) p = 0. 044
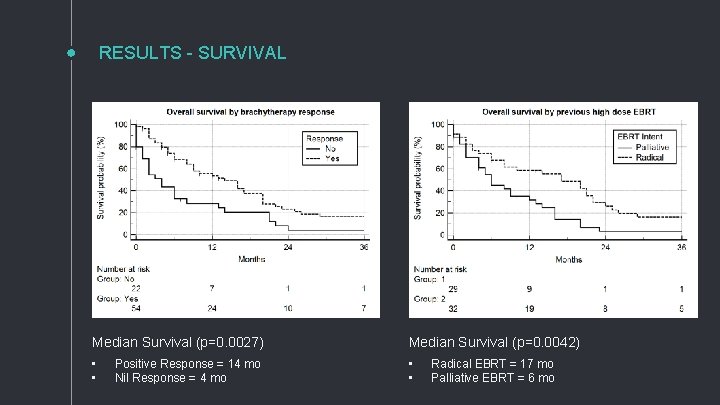
RESULTS - SURVIVAL Median Survival (p=0. 0027) Median Survival (p=0. 0042) • • Positive Response = 14 mo Nil Response = 4 mo Radical EBRT = 17 mo Palliative EBRT = 6 mo

OVERALL RESPONSE RATE 73% of all patients had a clinical response PALLIATION OF HAEMOPTYSIS 92% response rate (vs obstruction = 71%) [p = 0. 031] RESPONSE WITH PREVIOUS EBRT 63% (radical EBRT) vs 84% (palliative EBRT) [p = 0. 044] survival advantage for radical EBRT (17 mo vs 6 mo) [p = 0. 0042]

DISCUSSION Centralised Delivery § Barriers to implementation § Logistical Barriers (equipment, ongoing supply of radioisotopes) § Technical Barriers (quality assurance programs, skill and training of staff) § Integration with existing programs § Prostate/gynaecological/breast brachytherapy programs require similar logistical and technical demands

DISCUSSION Limitations Literature § Retrospective data set § Limited data published, with even less from Australia § Variable data quality, particularly with regard to defining clinical response § Missing data (e. g. EBRT plans from other centres) § Patients lost to follow-up § We present one of the larger data sets in the literature (largest from Australia) § We draw similar conclusions to those from other literature

CONCLUSIONS Effective Palliation Haemoptysis Safety ◦ 73% overall response to clinical symptoms ◦ Particularly effective (92% response rate) ◦ Low toxicity (nil grade 2 or greater toxicities) Re-Irradiation Centralised Service ◦ Viable treatment option after definitive EBRT ◦ Large geographical areas may be served by dedicated tertiary centres

ANY QUESTIONS? You can contact me at: matthew. knox@unsw. edu. au
- Slides: 19