Encephalitis Presented by Dr Manahil Definition u Encephalitis

Encephalitis Presented by : Dr: Manahil

Definition u Encephalitis is an inflammation of the brain parenchyma , presents as diffuse and or focal neuropsychological dysfunction.

Mortality and morbidity u They are related to host factors , such as preexisting CNS injury and the virulence of infecting organism. poor outcomes can be anticipated in infants younger than one year.

A etiology u 1 - infectious : viral agents such as HSV type 1 and 2 , VZV, EBV, measles , mumps , rubella, rabies , west nile virus , polio virus and HIV. u Bacterial agents : mycoplasma u Parasites and fungi : toxoplasma gondii u 2 - non infectious : demyelinating process in acute dissiminatd encephalitis.

Mode of transmission Agent Transmission HSV unknown VZV Direct contact (air) Influenza virus Direct contact(air) polio Fecal-oral route Rabies Dog and wild animals Mumps , measles Direct contact West nile , dengue virus Culex , aedes mosquitoes

Pathophysiology u . u In general the virus replicates outside the CNS and gains entry either by hematogenus spread or by traveling along neural (rabies, HSV, VZV) and olfactory (HSV) pathways Once cross BBB , the virus enters neural cells, with resultant destruction in cell functioning , perivascular congestion, hemorrhage, and inflammatory response diffusely affecting grey matter disproportionately to white matter.

u Focal pathology is the result of neuron cell membrane receptors found only in specific portions of the brain and accounts for regional tropism found with some viruses (HSV has predilection for the inferior and medial temporal lobes)

u In contrast to viruses that invade gray matter directly , acute disseminated encephalitis and post infectious encephalomyelitis , secondary to measles , EBV, CMV, are immune mediated process , which result in multifocal demyelination of perivenous white matter.

Clinical presentaion History u Acuity and severity of presentation correlate with prognosis. u The general viral prodrome is several days long (fever, headache, nausea and vomiting, lethargy and myalgia) u The specific prodrome in VZV, EBV, CMV , measles and mumps include rash, lymphadenopathy hepatosplenomegaly and parotid enlargement. u

u The classic presentation is encephalopathy with diffuse or focal neurologic symptoms , including the following : u Behavioral and personality changes , decreased level of consciousness. u Stiff neck , photophobia , lethargy.

Generalized or localized seizures. u Acute confusion or amnestic state. u Flaccid paralysis. u Less common symptoms include headache and other complaints of meningismus. u Neonatal HSV infection symptoms may occur in any combination u

u Skin, eye , and mouth lesions(early presntation) u Encephalitis-change inlevel of alertness, irritability, seizures, poor feeding u Evidence of wide spread , disseminated disease such as rash or shock

Physical Examination The signs of encephalitis may be diffuse or focal (80%of pt with HSE present with focal findings) as follows: u Altered mental status and or personality changes u Focal finding , such as hemi paresis, focal seizures, and autonomic dysfunction u Movement disorders u

Ataxia u Cranial nerve defects u Dysphagia u Meningismus u Unilateral sensory motor dysfunction u HSV infection in the neonate age(1_45 days): u Herpetic skin lesion over the presenting surface from birth u

u Keratoconjunctivitis u Oropharyngeal involvement (buccal mucosa, tongue) u Seizures , irritability, bulging fontanels u Additional signs of disseminated HSV, such as shock, jaundice and hepatomegaly.

Differentials u u u u u Brain abcess Meningitis Cerebral malaria Hypo glycemia Status epilepticus Subarachnoid hemorrhage SLE TB Others(head trauma, intra cranial tumor, acute confusional states secondary to drugs, toxins psychosis

Lab studies CBC: finding are within normal u Serum electrolyte: within normal u Serum glucose: base line for CSF glucose u LFT: to adjust antibiotic dose u CSF polymerase chain reaction: PCR for DNA HSV is 100% specific within first 25_45 hours. u HSV culture( from lesions, CSF and blood u

u Heterophile antibody and cold agglutinins for EBV u Serologic tests for toxoplasmosis
Imaging studies u Brain CT u In toxoplasmosis , contrast enhanced CT reveals several nodular or ring enhancing lesions u MRI : in HSV it shows several foci of increased T 2 signal intensity in medial temporal lobes and inferior frontal gray matter

Other tests EEG : in HSE paroxysmal lateral epileptiform discharges are observed. u CSF analysis u brain biopsy (96%sensitivity)(1 00% specifity) u
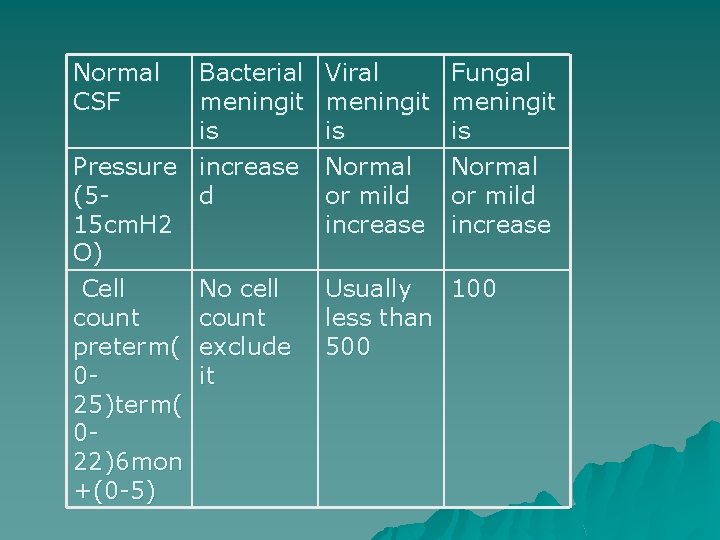
Normal CSF Bacterial meningit is Pressure increase (5 d 15 cm. H 2 O) Cell No cell count preterm( exclude 0 it 25)term( 022)6 mon +(0 -5) Viral meningit is Normal or mild increase Fungal meningit is Normal or mild increase Usually 100 less than 500

Micro Gram stain organism(no 80%effectiv ne) e No organism India ink 8090%effectiv e Glucoseeugl ycemia(>50 %serum)hy per(>30%) decrease normal Sometimes decrease Protein preterm(65150)term(20 170)6 mon(1 5 -45) Usually>150 mg/dl Mildly increased Increased>1 000

Treatment u Consider airway protection in pt with altered mental status u Evaluate and treat for shock u Treat seizures u Stabilize alert pt with normal vital signs

u The goal of treatment for acutely ill pt is administration of first dose or doses acyclovir with or without antibiotics or steroids as quickly as possible.

Drugs u 1 -acyclovir (zovirax) : u Inhibits activity against HSV-1 and 2 u Dose (neonatal HSV 10 -15 mg/kg)IV 8 h u HSV encephalitis (10 mg/kg)IV 8 h u Side effect: nephrotoxic

u Foscarnet (foscavir): u Inhibit replication of CMV, HSV 1 , HSV 2 u Dose <12 y not established u >12 y 40 mg/kg IV 8 h (14 -26 days)

u Dexamethasone (decadron- dexasone): u Decrease inflammation by suppressing migration of polymorph onuclear leukocytes and reversing increased capillary permeability. u Dose : 0. 15 mg/kg IV 6 h u Monitor for adrenal insufficiency

Complications u Seizures u SIADH u Increase u Coma ICP

Prognosis u Depends on the virulence of the virus , age immune status, preexisting neurologic condition u The mortality rate in treated HSE averages 20% and is correlated with mental status changes at time of first dose of acyclovir.
- Slides: 29