ENCEPHALITIS DR M B AMANULLAH Department of Pediatrics

ENCEPHALITIS DR. M. B. AMANULLAH. Department of Pediatrics Yenepoya Medical College

DEFINITIONS • ENCEPHALITIS is defined as an Inflammatory process of the central nervous system with dysfunction of brain. • In most patients both brain and meninges are involved resulting in meningoencephalitis • Mostly caused by viruses and sometimes by other microorganisms. • ENCEPHALOPATHY implies cerebral dysfunction due to non infectious causes like toxins, poisons, endocrinal, autoimmune disorders etc. Here there is no inflammatory process. It mimics encephalitis.

ETIOLOGY • Acute Encephalitis may be 1) PRIMARY : That is Direct invasion & replication of the virus leading to tissue necrosis eg: Encephalitis due to Herpes simplex, Arbo virus & rabies 2) PARAINFECTIOUS: post infectious inflammatory response characterised by immune mediated centralnervous system

ETIOLOGY ENCEPHALITIS : • VIRAL ; R. N. A viruses – Mumps, measles, rubella, enteroviruses • D. N. A. Viruses – Herpes simplex, CMV. • Epstein Barr, Pox Group. • ARBO viruses – Japanese B, West Nile. Russian spring summer. • Hiv, Rabies, Choriomeningitis virus, Dengue, slow viruse infections, Prions. • BACTERIAL : Pyogenic, Tubercular. • FUNGI: Candida , Cryptococcus, Mucormycosis. ENCEPHALOPATHY • Hypoxic encephalopathy • Metabolic - Diabetic ketoacidosis, uremia, hepatic coma • Fluid & Electrolyte disturbances. • Toxic / heavy metal poisoning, insecticides , substance abuse , alcohol. • Malignancies • Mitochondrial disorders

PATHOLOGY • Pathological changes are non specific except in Herpes Simplex encephalitis and rabies, where specific inclusions are demonstrable. • Gross examination of brain usually shows DIFFUSE EDEMA, CONGESTION & HEAMORRAGHES. • Microscopically, there may be PERIVASCULAR CUFFING with lymphocytes & Neutrophils. Neurons show Necrosis & degeneration , associated with neuronophagocytosis.

CLINICAL FEATURES • Clinical features are variable. The onset is usually sudden. The child will have high fever, headache , vomiting , mental confusion, irritability, apathy , loss of consciousness. • Often associated with Seizures. • Increased intracranial pressure results in hyperventilation, cardiorespiratory insufficiency, decerebration • Various palsies like hemiplegia, ocular palsy, cerebellar syndromes and speech disturbances may develop. • Lateralization to one side occurs frequently in Herpes Simplex Virus encephalitis.

TYPICAL FEATURES • Increased INTRACRANIAL PRESSURE & PAPILLEDEMA With evidence of BRAINSTEM DYSFUNCTION. • Unchecked brain swelling may lead to herniation at tentorial hiatus, compression of mid brain causing deteroriation in Conciousness , Pupillary abnormalities, ptosis, VI nerve palsy, ophthalmoplegia, paralysis of upward gaze, Cheyne Stokes breathing , hyperventilation and bradycardia may be observed. Herniation of cerebellum through the foramen
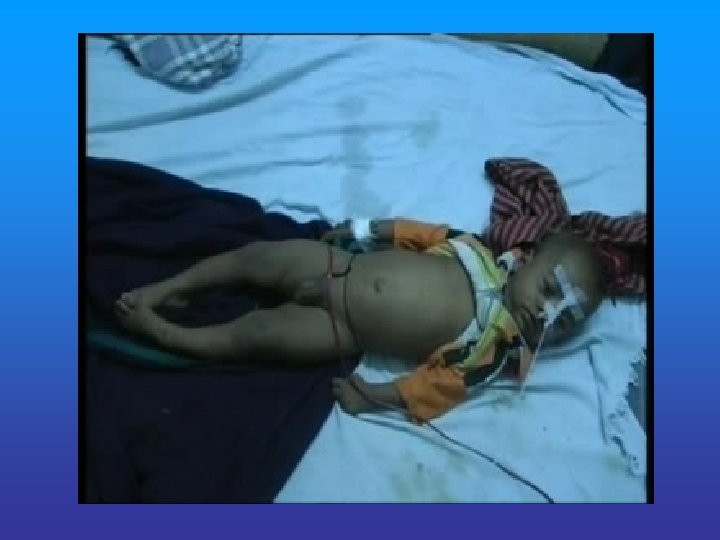

PROGNOSIS • The course of the Illness can be variable , from a mild illness with complete spontaneous recovery to very severe forms. • There may be severe Neurological residua, which may totally incapacitate the child.

DIAGNOSIS • Arrive at a precise etiological diagnosis by a Careful history, systemic examination, account of recent illnesses or exposure to toxins. LUMBAR PUNCTURE must be done if there is no papilledema. EEG , Neuroimaging Studies -C. T or MRI. Serum electrolytes, Blood sugar , Urea, Blood Ammonia, Metobolic Screening,

Diagnosis • Toxicologic studies to should be undertaken in suspected cases. • Other treatable causes such as Enteric encephalophathy, malaria, shigella, toxins, poisoning, diabetes mellitus & renal diseases should be ruled out.

LUMBAR PUNCTURE • CSF Shows Mild Pleocytosis (> 5 cells / cu. mm) – observed in 95% cases ( Initial polymorphonuclear & later lymphocytic ). • Slightly Elevated protein , and normal sugar. • Presence of RBCs in CSF is characteristic of Herpes simplex virus Encephalitis. • Viral culture , Serology & PCR may be performed on the CSF PCR is considerd as Primary

EEG • Typically shows DIFFUSE SLOW WAVE ACTIVITY in Encephalitis indicating difuse cerebral dysfunction but is not of diagnostic value. • Periodic latralized epileptiform discharges ( PLEDS) is Characteristic in HSV & other focal encephalitis.

NEUROIMAGING STUDY CT and MRI brain can help to diffentiate Viral encephalitis from metabolic or toxic disorders & Acute Disseminated Encephalomyelitis. BRAIN BIOPSY is rarely done nowadays.

DIFFERENTIAL DIAGNOSIS 1. 2. 3. 4. Brain abscess Cerebral malaria Tuberculosis Enteric encephalopathy 5. Acute Intermittent porphyria 6. Subdural empyema 7. Haemorrhagic stroke 8. Neoplasms of CNS 9. Para or post infectious encephalomyelitis 10. Atypical bacterial / fungal / parasitic infections of CNS 11. Toxic-metabolic encephalopathy 12. Septicemia 13. Collagen vascular disease 14. Endocarditis

TREATMENT - GENERAL • • • Treat in ICU Maintain Airway Maintain breathing Maintain Circulation – appropriate I. V. fluids Seizures should be controlled. Cerebral edema – – – Mannitol 1 -2 gm/ Kg infuse quickly Glycerol orally Diuretics Steroids Elective hyperventilation

TREATMENT • Should be managed in the ICU. • Air way Should be kept patent & assisted respiration given if necessary • HYPERPYREXIA is managed with vigorous hydrotherapy & antipyretics. • SHOCK is managed by infusion of appropriate fluid, Dextran or vasopressors. Dopamine or dobutamine

Treatment • SEIZURES are controlled by intravenous Diazepam & phenytoin. • Raised intracranial pressure is managed by I. V. Infusion of 20% Mannitol Solution given in 30 minutes and corticosteroids such as Dexamethasone.

HERPES SIMPLEX ENCEPHALITS • IS Caused by HERPES SIMPLEX TYPE II VIRUS • Clinical picture includes Fever of sudden onset, Mental confusion, Vomitting , Meningeal irritation, • Head ache and Papilledema. • Seizures & neurological deficits are common. • IMPORTANT DIAGNOSTIC CLUES ARE

TREATMENT - SPECIFIC • Should be instituted immediately. • At present HSE is the only treatable viral encephalitis: – Drug : Acyclovir ( Inj. Zovirax 250 mg vials) – Dose : 10 mg / kg IV infusion in 1 hr 8 hrly for 2 -3 wks. – Toxicity : Elevation of BUN and Creatinine , Thrombocytopenia , G. I. ( nausea, vomiting , diarrhea), Neurotoxicity (lethargy or obtundation, disorientation , confusion agitation , hallucination , tremors, seizures), Renal insufficiency (adjust dose ) • In Acyclovir resistant cases Foscarnet is the only drug available.

PROGNOSIS • Untreated HSVE has mortality of 70%. • On treatment mortality is 30 -40% • Complete recovery occurs in 38. 5% cases receiving early acyclovir.

JAPANESE ENCEPHALITIS • CAUSED BY SINGLE STRANDED RNA VIRUS OF THE FAMILY FLAVIVIRDAE • JE is a mosquito borne viral disease of humans as well as horses , pigs, and other domestic animals. • the vectors are night biting mosquito ie. • CULEX TRITATENIORHYNCUS SUMMAROSUS and CULEX VISHNUI.

CLINICAL FEATURES • After an INCUBATION PERIOD (between 4 to 14 days) cases typically progress through the following 4 stages • PRODROMAL ILLNESS (Lasting about 23 days) • ACUTE STAGE (lasting 3 -4 days) • SUB ACUTE STAGE ( lasting 7 -10 days) CONVALESNCE (lasting 4 -7 wk)

CLINICAL FEATURES • Onset may be characterized by abrupt onset of Fever , headache, respiratory symptoms, anorexia, • Abdominal pain , vomitting and sensory changes. • Psychotic episodes. • Grand mal epilepsy may be seen in some children (10 -24 percent of children)

CLINICAL FEATURES the Characteristic feature of JE is RAPIDLY CHANGING CENRTAL NERVOUS SYSTEM SIGNS ( eg hyperreflexia followed by hyporeflexia or plantar response that change ). SENSORIUM Of the patient may vary progressing to coma.

Diagnosis • JE should be suspected in patients who are exposed to night biting mosquitos in endemic areas • Acute phase serum collected early in the illness should be tested for VIRUS SPECIFIC Ig. M ANTIBODIES • Also a four fold or greater increase in Ig. G antibody titer in paired acute & convalesent sera. • VIRUS Can also be identified by PCR.

TREATMENT • NO Specific for treatment JE. • INTENSIVE SUPPORTIVE CARE & CONTROL OF SEIZURES.

PROGNOSIS • FATALITY RATES ARE HIGHEST IN CHILDREN IN THE AGE GROUP OF 5 -9 YRS. • Sequele is directly related to the severity and age of the patient. Most common in children younger than 10 yrs. • Common sequeles are MENTAL DETERIORATION • SEVERE EMOTIONAL INSTABILITY, PERSONALITY CHANGES,

PREVENTION OF ENCEPHALITIS. There are 3 types of JE vaccines, Mouse brain derived inactivated vaccine, cell culture derived inactivated vaccine and cell cuture derived live attenauated JE VACCINE (most efficacious ) CNS viral infections by Measles, Mumps , polio and varicella are preventable by appropriate vaccines. Control of insect vectors & adequate personal protection.

REFERENCES 1 2 3 4 5 6 7 8 Nelson Textbook of Pediatrics (2004), Behrman, Kliegman, Jenson (Eds. ) 17 th ed. Saunders , Philadelphia, U. S. Ghai Essential Pediatrics (2004). Ghai OP, Gupta P , Paul VK (Eds) 6 th ed. CBS Publ. N. Delhi Fundamentals of Pediatrics (2002) KE Elizabeth (ED. ) 2 nd ed. Paras Medical Publisher, Hyderabad Misra UK , Kalita J ; Diagnostic approach to patients with acute encephalitis. Reviews in Indian Neurology 2005, p 85 -103 Gupta PP ; Viral encephalitis. In Souvenir of Rajpedicon 2004. Sharma RB (Eds), Deptt. of Pediatrics Medical college Jodhpur. 2004. p 17 -21 Pangaria A, Sharma B, Kumar H, Mathew. V; Acute Encephalitis. Special Supplement Issue of The Raj. Med. Jour. 2004, 22 -28 Satishchandre P, Rav V, Shankar SK Herpes Simplex Encephalitis; clinicopathological and virological appraisal. Prog. in Clinical Neuro Sc. 1996. 11. 167 -186 Text book of pediatrics Piyush Guptha.

Questions on Encephalitis. 1) Discuss Etiology , Clinical manifestations & management of Viral Encephalitis. 2) C. S. F in Viral Encephalitis. 3) Japanese Encephalitis Vaccines. 4) Discuss the management & complications Herpes Encephalitis. 5) Write a short note on Subacute

MCQs on Encephalitis • 1) Early treatment with ACYCLOVIR on suspicion of Herpes Encephalitis is justified since it • A) prevents transmission of infection from person to person • B) prevents serious Sequales • C) controls Seizures.

MCQ • 2) Rapidly changing CNS signs are characteristic of a) Dengue fever b) Herpes encephalitis c) Japanese Encephalitis. 3) All of the following are caused by ARBO viruses except , a) Rabies b) Western Equine Encephalitis

MCQ • 4) one of the following drug is not used in the treatment of Herpes Encephalitis, • 1) Acylovir • 2) Gancyclovir. • 3) Oseltamvir • 4) Foscarnet.

MCQ • 5) SSPE (Subacute Sclerosing Pan encephalitis ) is a late complication of 1) Varicella 2) Herpes Encephalitis 3) Measles 4) Japanese Encephalitis

Thank you
- Slides: 36