Emerging Bolus Insulin Therapies in the Treatment of

Emerging Bolus Insulin Therapies in the Treatment of Type 1 and Type 2 Diabetes Bruce W. Bode, MD, FACE Atlanta Diabetes Associates Atlanta, Georgia
Goals of Intensive Insulin Therapy l Maintain near normal glycemia l Avoid short-term crisis l Minimize long-term complications l Improve the quality of life 0 12 Hours 24

ACE / AACE Targets for Glycemic Control A 1 C (Hb. A 1 c) < 6. 5 % Fasting/preprandial glucose< 110 mg/d. L Postprandial glucose < 140 mg/d. L ACE / AACE Consensus Conference, Washington DC August 2001

Insulin The most powerful agent we have to control glucose
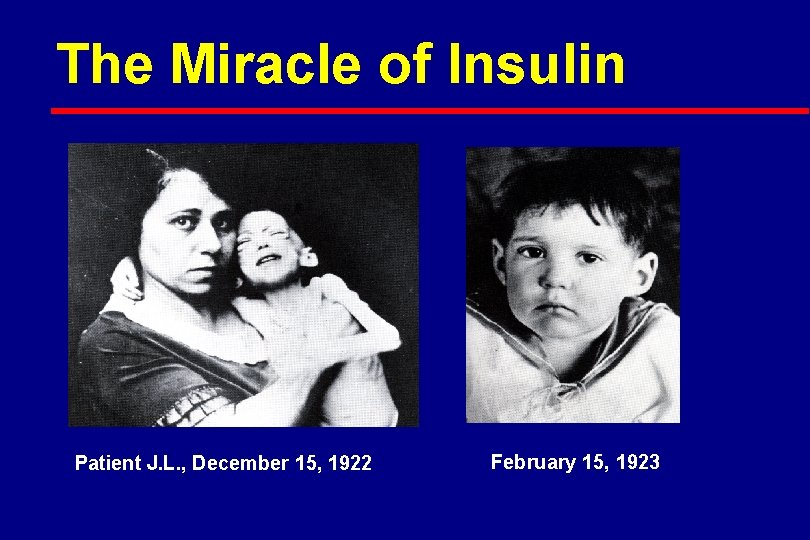
The Miracle of Insulin Patient J. L. , December 15, 1922 February 15, 1923
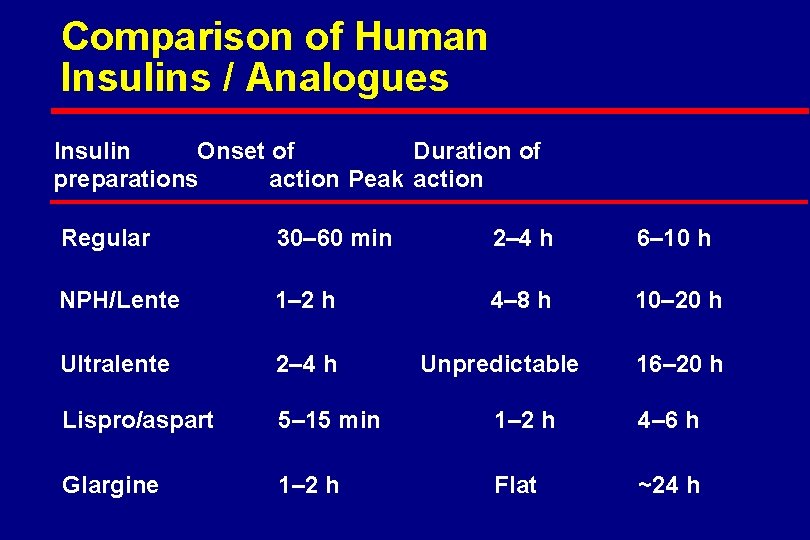
Comparison of Human Insulins / Analogues Insulin Onset of Duration of preparations action Peak action Regular 30– 60 min 2– 4 h 6– 10 h NPH/Lente 1– 2 h 4– 8 h 10– 20 h Ultralente 2– 4 h Lispro/aspart 5– 15 min 1– 2 h 4– 6 h Glargine 1– 2 h Flat ~24 h Unpredictable 16– 20 h

Rapid-acting Insulin Analogs: Medical Rationale l Administration at mealtime l Mimic physiological insulin profile l Improved postprandial glycemic control l Lower risk of late hypoglycemia 2/26/2021 7
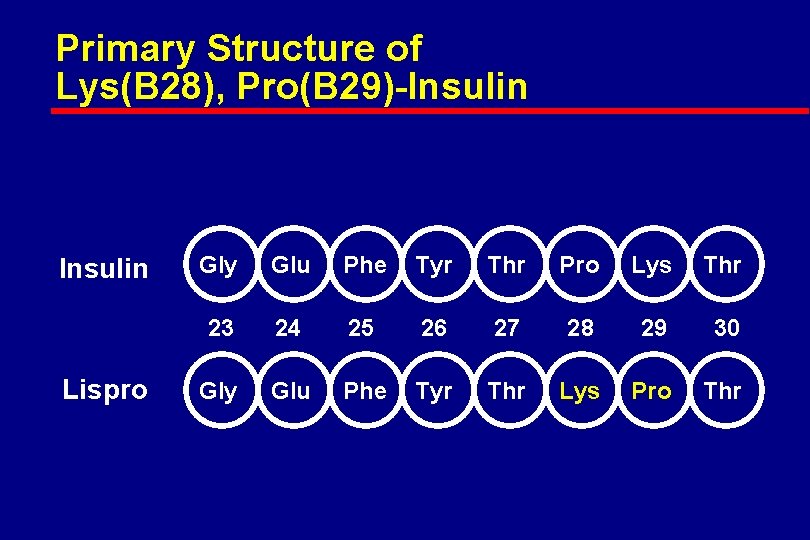
Primary Structure of Lys(B 28), Pro(B 29)-Insulin Lispro Gly Glu Phe Tyr Thr Pro Lys Thr 23 24 25 26 27 28 29 30 Gly Glu Phe Tyr Thr Lys Pro Thr
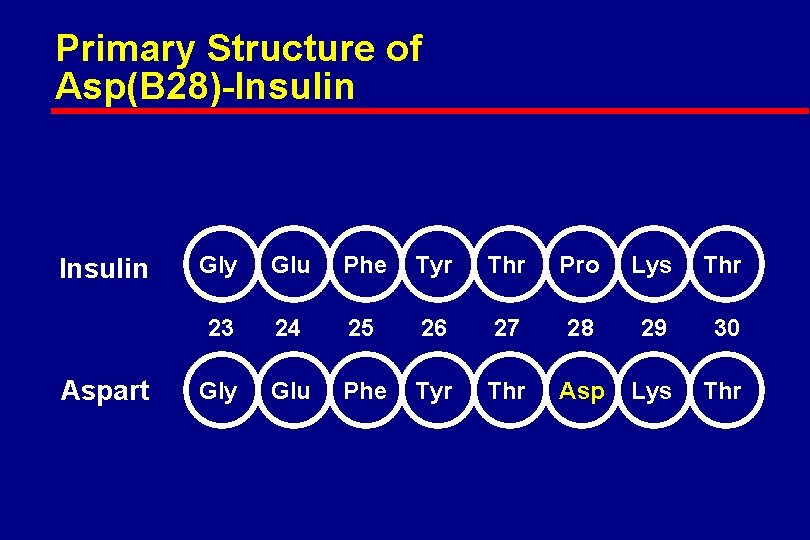
Primary Structure of Asp(B 28)-Insulin Aspart Gly Glu Phe Tyr Thr Pro Lys Thr 23 24 25 26 27 28 29 30 Gly Glu Phe Tyr Thr Asp Lys Thr
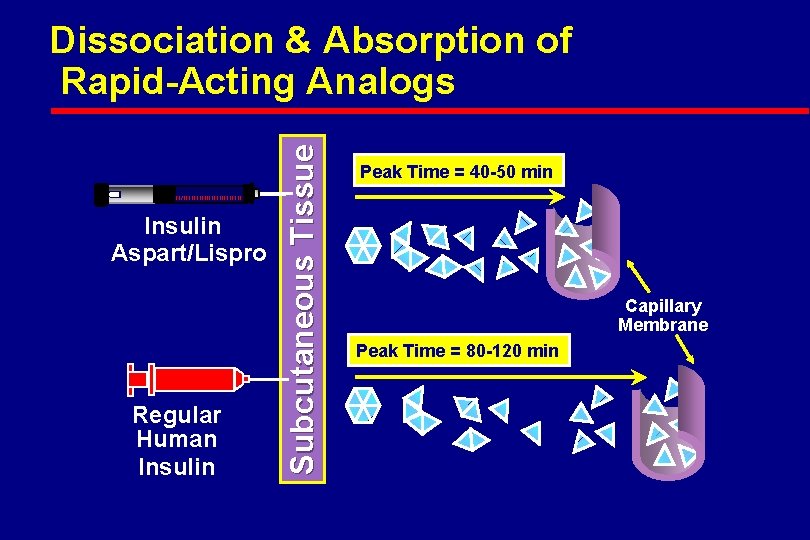
Insulin Aspart/Lispro Regular Human Insulin Subcutaneous Tissue Dissociation & Absorption of Rapid-Acting Analogs Peak Time = 40 -50 min Capillary Membrane Peak Time = 80 -120 min
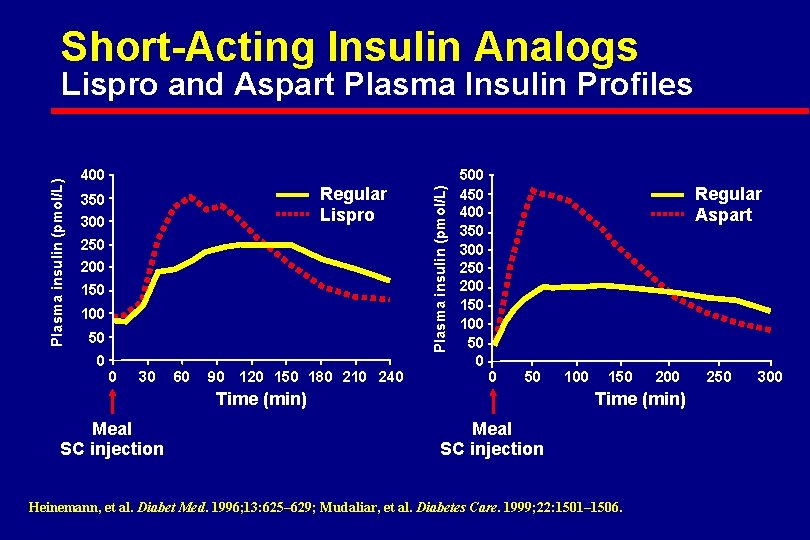
Short-Acting Insulin Analogs 400 Regular Lispro 350 300 250 200 150 100 50 0 0 30 60 90 120 150 180 210 240 Plasma insulin (pmol/L) Lispro and Aspart Plasma Insulin Profiles 500 450 400 350 300 250 200 150 100 50 0 Regular Aspart 0 50 Time (min) Meal SC injection 100 150 200 Time (min) Meal SC injection Heinemann, et al. Diabet Med. 1996; 13: 625– 629; Mudaliar, et al. Diabetes Care. 1999; 22: 1501– 1506. 250 300
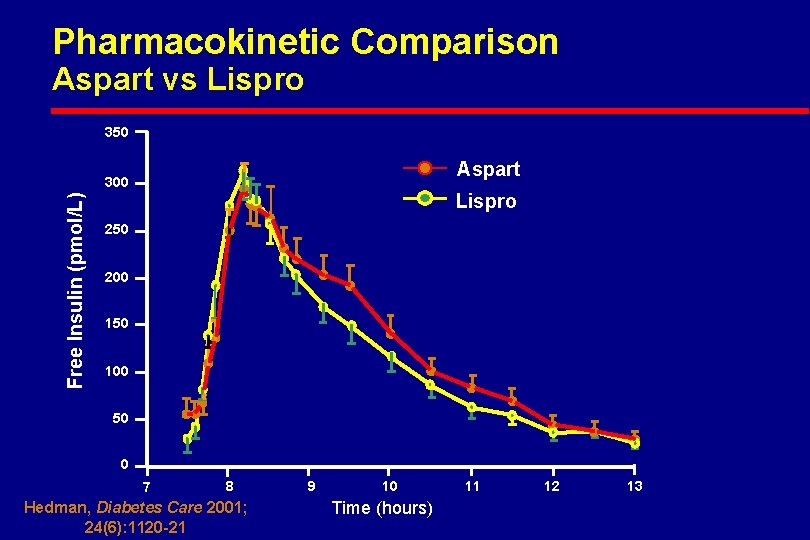
Pharmacokinetic Comparison Aspart vs Lispro 350 Aspart Free Insulin (pmol/L) 300 Lispro 250 200 150 100 50 0 7 8 Hedman, Diabetes Care 2001; 24(6): 1120 -21 9 10 Time (hours) 11 12 13
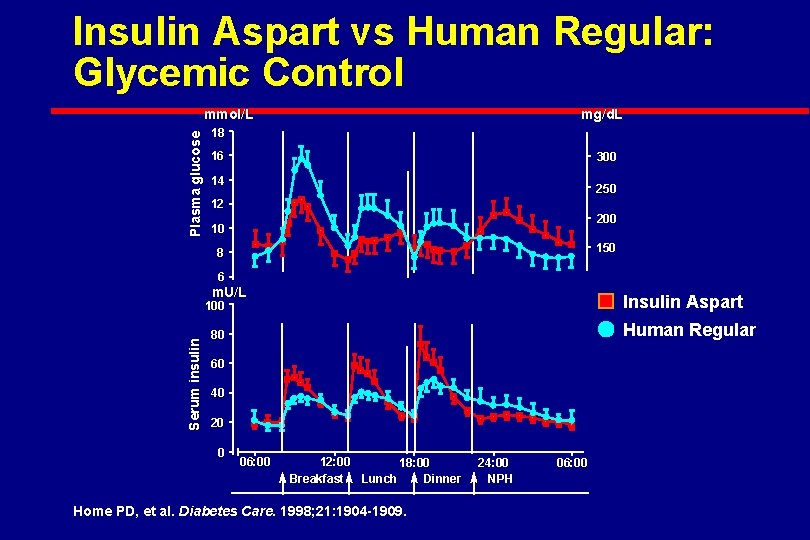
Insulin Aspart vs Human Regular: Glycemic Control Plasma glucose mmol/L mg/d. L 18 16 300 14 250 12 200 10 150 8 6 m. U/L Insulin Aspart Serum insulin 100 Human Regular 80 60 40 20 0 06: 00 12: 00 18: 00 Breakfast Lunch Dinner Home PD, et al. Diabetes Care. 1998; 21: 1904 -1909. 24: 00 NPH 06: 00
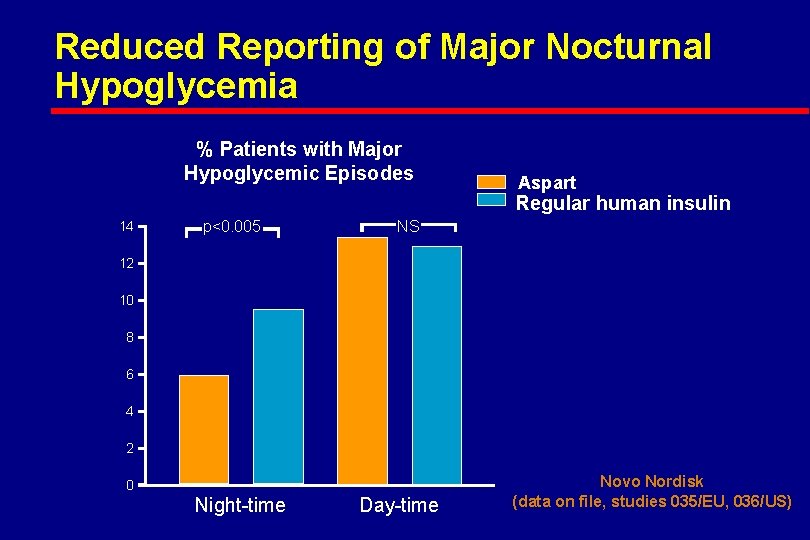
Reduced Reporting of Major Nocturnal Hypoglycemia % Patients with Major Hypoglycemic Episodes Aspart Regular human insulin 14 p<0. 005 NS 12 10 8 6 4 2 0 Night-time Day-time Novo Nordisk (data on file, studies 035/EU, 036/US)
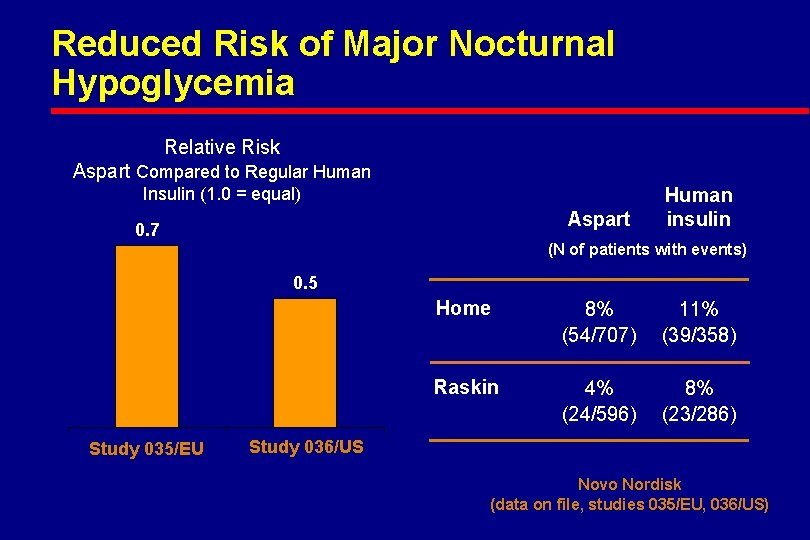
Reduced Risk of Major Nocturnal Hypoglycemia Relative Risk Aspart Compared to Regular Human Insulin (1. 0 = equal) Aspart 0. 7 Human insulin (N of patients with events) 0. 5 Study 035/EU Home 8% (54/707) 11% (39/358) Raskin 4% (24/596) 8% (23/286) Study 036/US Novo Nordisk (data on file, studies 035/EU, 036/US)
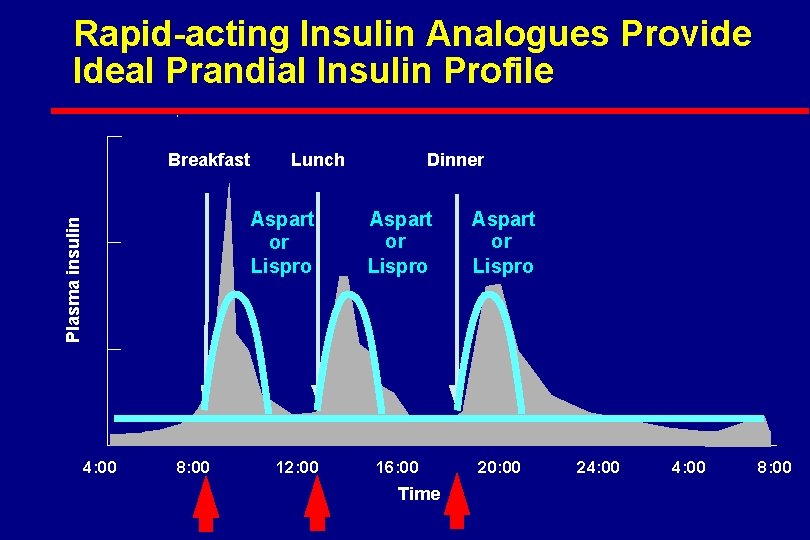
Rapid-acting Insulin Analogues Provide Ideal Prandial Insulin Profile Breakfast Lunch Plasma insulin Aspart or Lispro 4: 00 8: 00 12: 00 Dinner Aspart or Lispro 16: 00 20: 00 Time 24: 00 8: 00
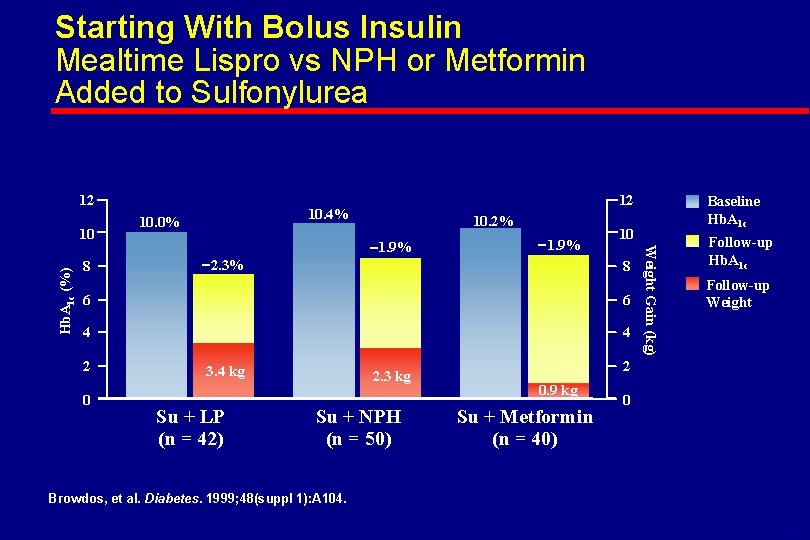
Starting With Bolus Insulin Mealtime Lispro vs NPH or Metformin Added to Sulfonylurea 12 8 10. 0% 10. 2% 1. 9% 2. 3% 1. 9% 10 8 6 6 4 4 2 0 3. 4 kg Su + LP (n = 42) 2. 3 kg Su + NPH (n = 50) Baseline Hb. A 1 c Weight Gain (kg) Hb. A 1 c (%) 10 12 10. 4% Follow-up Hb. A 1 c Follow-up Weight 2 0. 9 kg Su + Metformin (n = 40) 0 Browdos, et al. Diabetes. 1999; 48(suppl 1): A 104. 6 -47
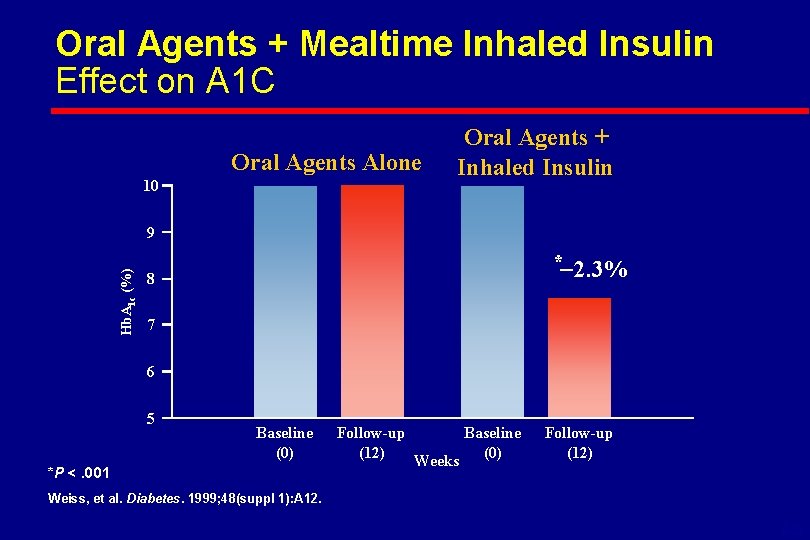
Oral Agents + Mealtime Inhaled Insulin Effect on A 1 C Oral Agents Alone 10 Oral Agents + Inhaled Insulin Hb. A 1 c (%) 9 * 2. 3% 8 7 6 5 Baseline (0) *P <. 001 Follow-up (12) Weeks Baseline (0) Follow-up (12) Weiss, et al. Diabetes. 1999; 48(suppl 1): A 12. 6 -55

Advancing Basal/Bolus Insulin l Indicated when FBG acceptable but – A 1 C > 7% or > 6. 5% and/or – SMBG before dinner > 140 mg/d. L l Insulin options – To glargine or NPH, add mealtime aspart / lispro – To suppertime 70/30, add morning 70/30 – Consider insulin pump therapy l Oral agent options – Usually stop sulfonylurea – Continue metformin for weight control – Continue glitazone for glycemic stability?
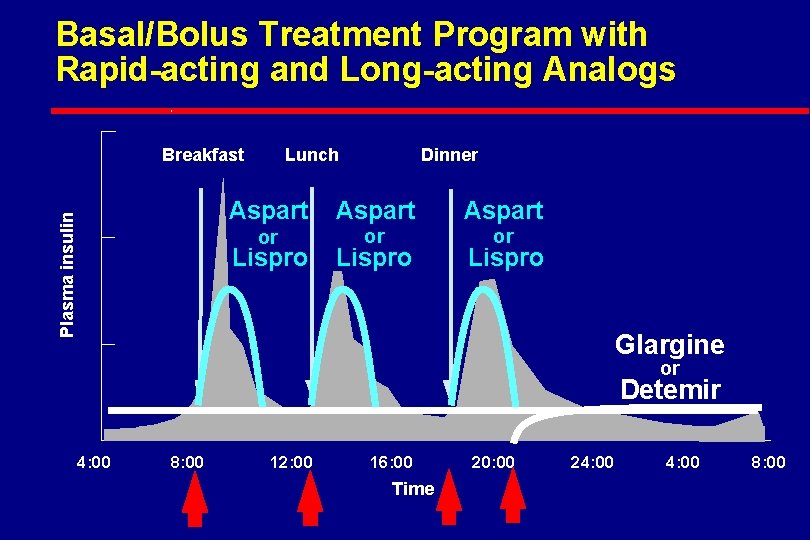
Basal/Bolus Treatment Program with Rapid-acting and Long-acting Analogs Plasma insulin Breakfast Lunch Dinner Aspart or or or Lispro Glargine or Detemir 4: 00 8: 00 12: 00 16: 00 Time 20: 00 24: 00 8: 00

The Basal/Bolus Insulin Concept l Basal insulin – Suppresses glucose production between meals and overnight – 40% to 50% of daily needs l Bolus insulin (mealtime) – Limits hyperglycemia after meals – Immediate rise and sharp peak at 1 hour – 10% to 20% of total daily insulin requirement at each meal
Insulin Pens First pen launched in 1985 Committed to developing one new insulin administration system per year.
Insulin Pens

Insulin Pens l 3 -m. L prefilled disposable pen offers precise dosing
Combined Insulin Pen and Meter Feature l Combined insulin doser and blood glucose monitor
Combined Insulin Pen and Meter Feature l Remembers amount of insulin delivered and time since last dose Benefit l Helps people inject the right amount of insulin at the right time

Starting MDI l Starting insulin dose is based on weight 0. 2 x wgt. in lbs. or 0. 45 x wgt. in kg l Bolus dose (aspart/lispro) = 20% of starting dose at each meal l Basal dose (glargine/NPH) = 40% of starting dose at bedtime

Starting MDI in 180 lb person l Starting dose = 0. 2 x wgt. in lbs. 0. 2 x 180 lbs. = 36 units l Bolus dose = 20% of starting dose at each meal 20% of 36 units = 7 units ac (tid) l Basal dose = 40% of starting dose at bedtime 40% of 36 units = 14 units at HS

Correction Bolus l Must determine how much glucose is lowered by 1 unit of short- or rapid-acting insulin l This number is known as the correction factor (CF) l Use the 1700 rule to estimate the CF l CF = 1700 divided by the total daily dose (TDD) ex: if TDD = 36 units, then CF = 1700/36 = ~50 meaning 1 unit will lower the BG ~50 mg/dl

Correction Bolus Formula Current BG - Ideal BG Glucose Correction factor Example: – Current BG: – Ideal BG: 220 mg/dl 100 mg/dl – Glucose Correction Factor: 50 mg/dl 220 - 100 =2. 4 u 50

Options to MDI l A Simpler Regimen l Insulin Pump l Premixed BID (DM 2 only)
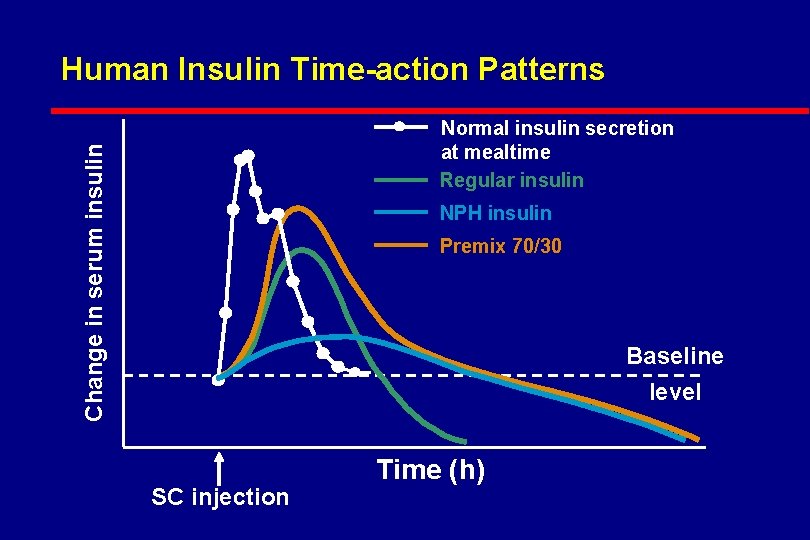
Human Insulin Time-action Patterns Change in serum insulin Normal insulin secretion at mealtime Regular insulin NPH insulin Premix 70/30 Baseline level SC injection Time (h)
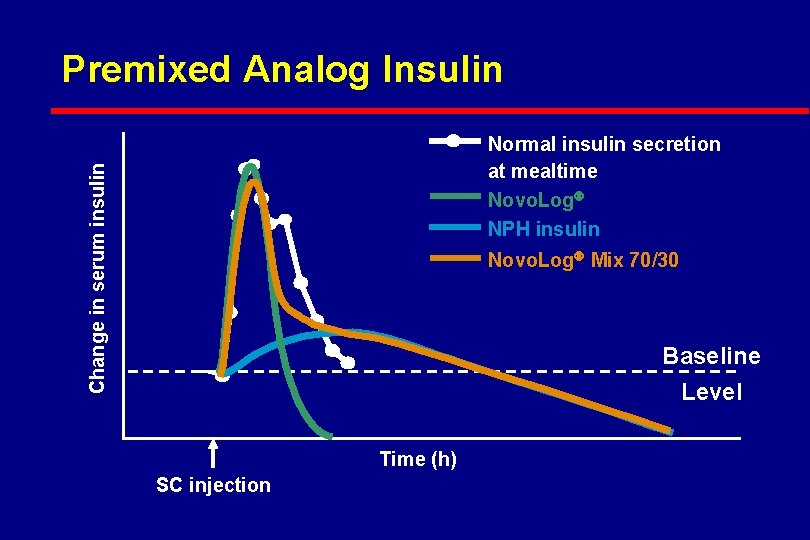
Premixed Analog Insulin Change in serum insulin Normal insulin secretion at mealtime Novo. Log NPH insulin Novo. Log Mix 70/30 Baseline Level Time (h) SC injection

Case #2: DM 2 on 70/30 l 60 year old black male l DM 2 age 56; Ht 69”; Wgt 180 l Failed oral agents l On 70/30 BID: 10 u am and pm l Hb. A 1 c 8. 4% SMBG 144 on 0. 8 tests/day l Increased 70/30, tried 3 xday, still not at goal

Case #2: DM 2 on 70/30 l Finally agrees to MDI l Starting dose: 0. 2 x wgt in # (36 u) l Bolus: 20% pre-meal (7 u ac tid) l Basal: 40% Bedtime or anytime (14 u HS) l Correction Factor: 1700 divided by TDD (50 mg/dl) l Does great - A 1 C 6. 4% l Current dose: 4 u am, 4 u noon, 10 u pm, 16 u Lantus HS
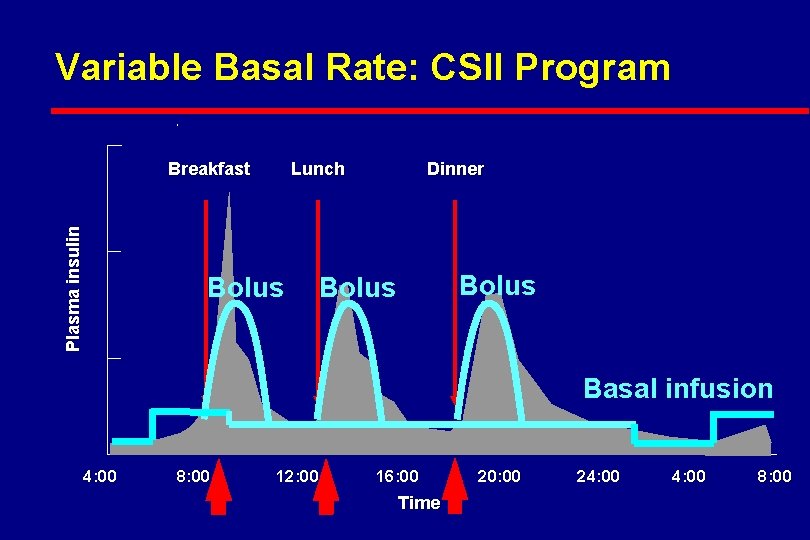
Variable Basal Rate: CSII Program Plasma insulin Breakfast Lunch Bolus Dinner Bolus Basal infusion 4: 00 8: 00 12: 00 16: 00 Time 20: 00 24: 00 8: 00

Pump Infusion Sets

Metabolic Advantages with CSII l Improved glycemic control l Better pharmacokinetic delivery of insulin – Less hypoglycemia – Less insulin required l Improved quality of life

CSII Factors Affecting A 1 C l Monitoring – A 1 C = 8. 3 - (0. 21 x BG per day) l Recording 7. 4 vs 7. 8 l Diet practiced – CHO: 7. 2 – Fixed: 7. 5 – WAG: 8. 0 l Insulin type (Aspart) Bode et al. Diabetes 1999; 48 Suppl 1: 264 Bode et al. Diabetes Care 2002; 25 439
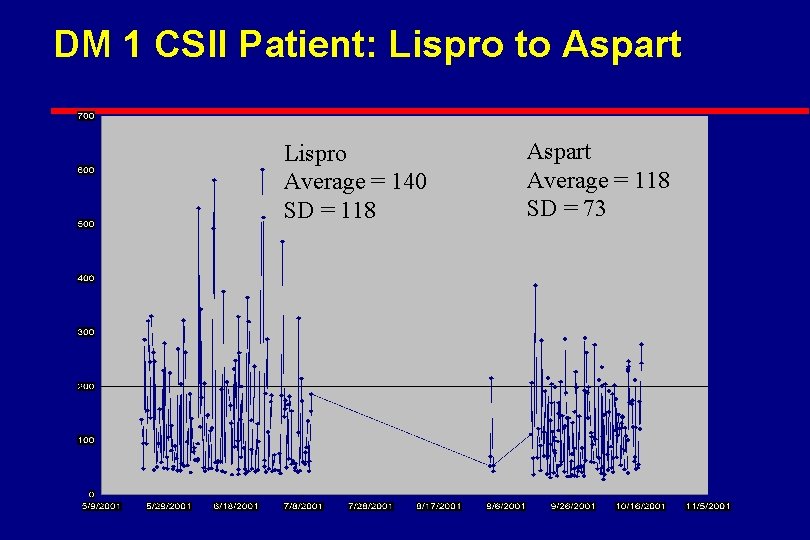
DM 1 CSII Patient: Lispro to Aspart Lispro Average = 140 SD = 118 Aspart Average = 118 SD = 73
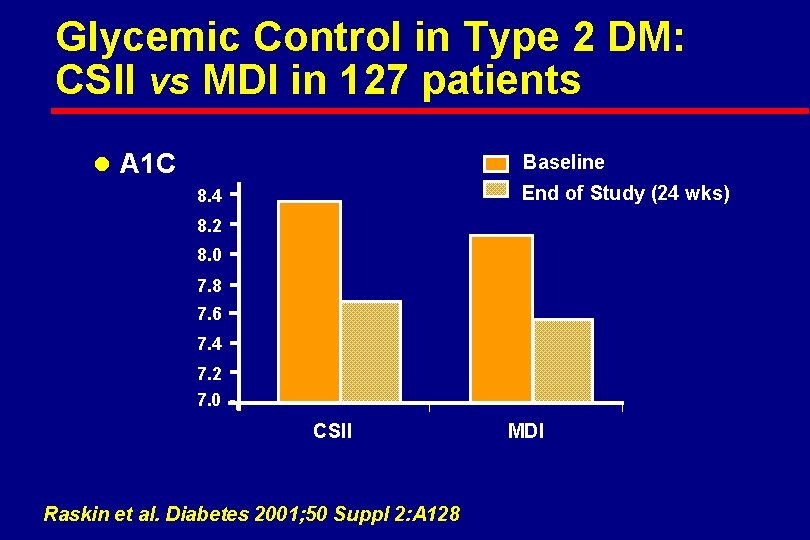
Glycemic Control in Type 2 DM: CSII vs MDI in 127 patients l A 1 C Baseline End of Study (24 wks) 8. 4 8. 2 8. 0 7. 8 7. 6 7. 4 7. 2 7. 0 CSII Raskin et al. Diabetes 2001; 50 Suppl 2: A 128 MDI
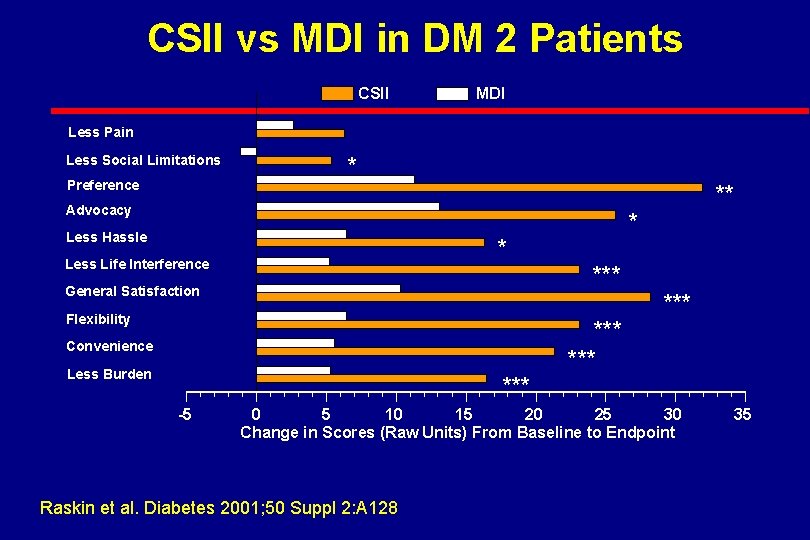
CSII vs MDI in DM 2 Patients CSII MDI Less Pain Less Social Limitations Preference * ** Advocacy Less Hassle * * Less Life Interference *** General Satisfaction Flexibility *** Convenience Less Burden *** -5 0 5 10 15 20 25 30 Change in Scores (Raw Units) From Baseline to Endpoint Raskin et al. Diabetes 2001; 50 Suppl 2: A 128 35

Case 3: DM 2 Poorly Controlled l 58 year old female presented with a 12 year history of poorly controlled, insulin treated diabetes l Ht 66’’, Wt 174#, BMI 28, C-peptide 2. 1 l A 1 C 10. 4% on 165 units per day (70/30 BID) l Added troglitazone, metformin, glimepiride to MDI insulin l A 1 C range 7. 7 to 12. 6% over 3 years

Case 3: DM 2 Poorly Controlled l Admitted twice for IV insulin and fasting with short lived success (A 1 C to 7. 6% but back up to 12. 6%) l Tried weight watchers and appetite suppressants; no help l Decided to try CSII
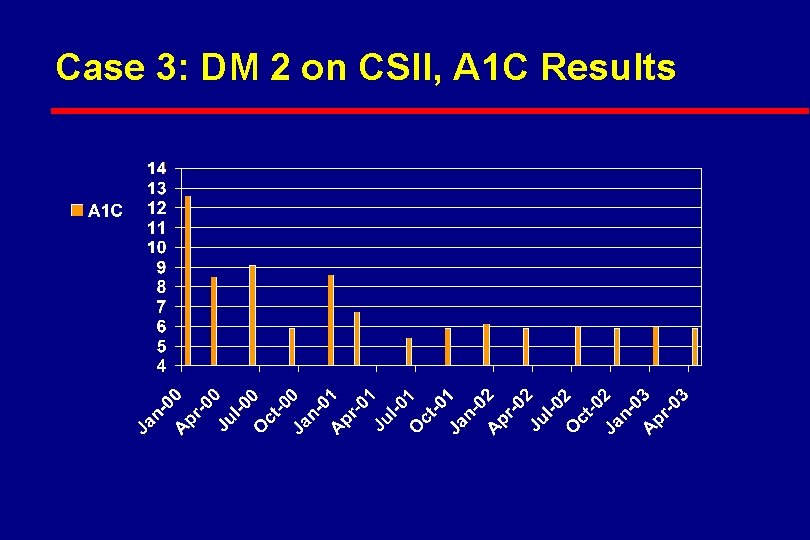
Case 3: DM 2 on CSII, A 1 C Results

Case 3: DM 2 Poorly Controlled l Patient loves the pump l On 110 units per day consuming 2 meals only per day (1. 4 units per kg or 0. 6 units per lbs) l Also on rosiglitazone 4 mg/day

Normalization of Lifestyle l Liberalization of diet — timing & amount l Increased control with exercise l Able to work shifts & through lunch l Less hassle with travel — time zones l Weight control l Less anxiety in trying to keep on schedule
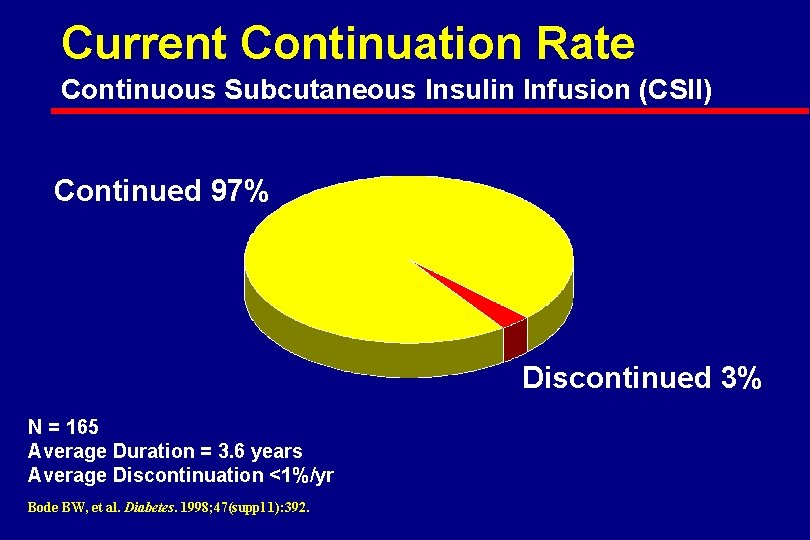
Current Continuation Rate Continuous Subcutaneous Insulin Infusion (CSII) Continued 97% Discontinued 3% N = 165 Average Duration = 3. 6 years Average Discontinuation <1%/yr Bode BW, et al. Diabetes. 1998; 47(suppl 1): 392.
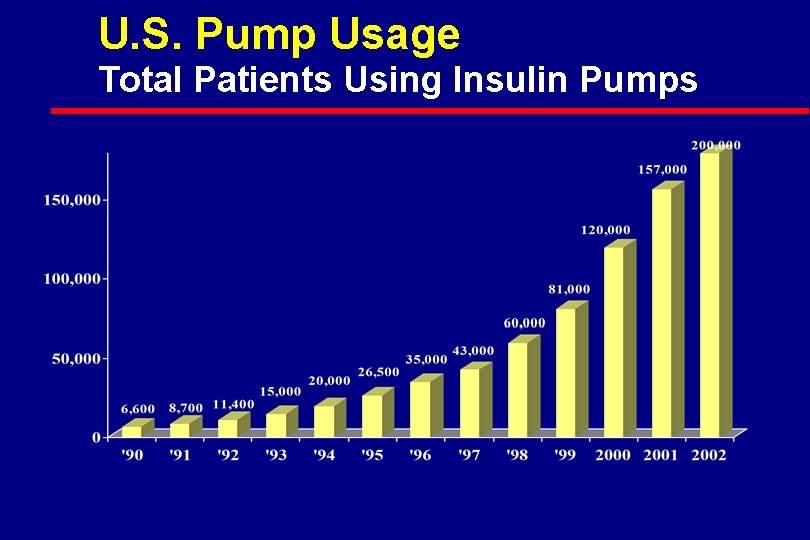
U. S. Pump Usage Total Patients Using Insulin Pumps

Current Pump Therapy Indications l Diagnosed with diabetes (even new onset DM 1) l Need to normalize blood glucose (BG) – A 1 C 7. 0% – Glycemic excursions l Hypoglycemia
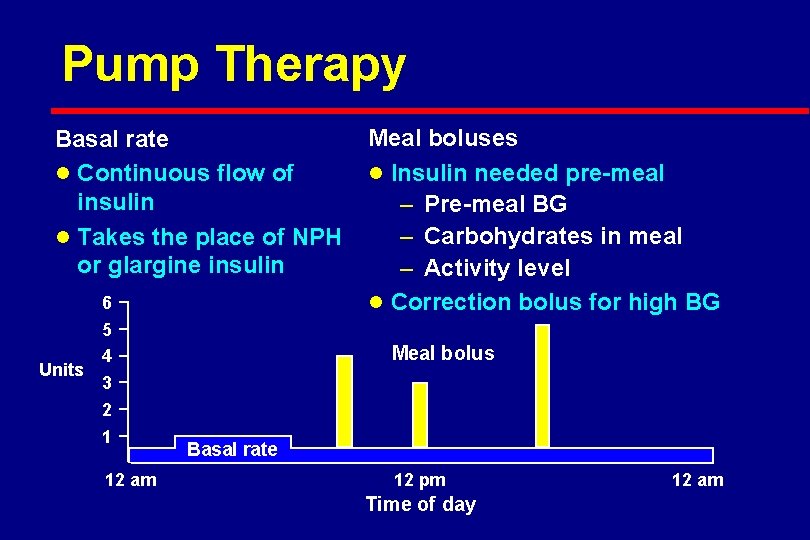
Pump Therapy Basal rate l Continuous flow of insulin l Takes the place of NPH or glargine insulin Units 6 5 4 3 2 1 12 am Meal boluses l Insulin needed pre-meal – Pre-meal BG – Carbohydrates in meal – Activity level l Correction bolus for high BG Meal bolus Basal rate 12 pm Time of day 12 am

Initial Adult Dosage Calculations Starting Doses – Based on pre-pump Total Daily Dose (TDD) Reduce TDD by 25 -30% for Pump TDD – Calculated based on weight 0. 24 x wgt in pounds (0. 5 x wgt in kg) Bode BW, et al. , Diabetes 1999, (Suppl 1): 84. Bell D and Ovalle F, Endocrine Practice 2000, 6: 357 -360. Crawford, LM, Endocrine Practice 2000, 6: 239 -43.

Initial Adult Dosage Calculations Basal Rate – 45 -50% of pump Total Daily Dose – Divide total basal by 24 hours to decide on hourly basal – Start with only one basal rate – See how it goes before adding additional basals

Estimating the Carbohydrate to Insulin Ratio (CIR) Individually determined CIR = (2. 8 x wgt in lbs) / TDD Anywhere from 5 to 25 g CHO is covered by 1 unit of insulin

What Type of Bolus Should You Give? Immediate vs Square vs Dual Wave l 9 DM 1 patients on CSII ate pizza and coke on four consecutive Saturdays l Dual wave bolus (70% at meal, 30% as 2 -h square): 9 mg/dl glucose rise l Single bolus: 32 mg/dl rise l Double bolus at -10 and 90 min: 66 m/dl rise l Square wave bolus over 2 hours: 79 m/dl rise Chase et al, Diabetes June 2001 #365

If A 1 C is Not to Goal Must look at: l SMBG frequency and recording l Infusion site areas – Are they in areas of lipohypertrophy? l Diet practiced – Do they know what they are eating? – Do they bolus for all food and snacks? l Other factors: – Fear of low BG – Overtreatment of low BG

If A 1 C Not to Goal and No Reason Identified l. Place on a continuous glucose monitoring system (CGMS by Medtronic Minimed, Glucowatch by Cygnus) to determine the cause

Summary l Insulin remains the most powerful agent we have to control diabetes l When used appropriately in a basal/bolus format, near-normal glycemia can be achieved l Newer insulins and insulin delivery devices along with glucose sensors will revolutionize our care of diabetes

Billing l Get paid for what you do l Use your codes and negotiate for coverage l Detailed visit: 99214 l Prolonged visit with contact plus above: 99354 or 99355 (insulin start or pump start) l Prolonged visit w/o contact plus above: 99358 or 59 (faxes, phone calls, emails)

Billing l Bill faxes as prolong visits with out contact or negotiate a separate charge l Bill meter download: 99091 l Bill CGMS: 95250 l Bill immediate A 1 C: 83036

Questions l For a copy or viewing of these slides, contact l WWW. adaendo. com
- Slides: 62