Embryogenesis The human thyroid gland develops from a

Embryogenesis The human thyroid gland develops from @ a median anlage derived from the primitive pharyngeal floor @ paired lateral anlagen from the 4 pharyngo-bronchial pouch. These structures are visible by days 16 to 17 of gestation. Gestation 1 st 2 nd 3 rd By 50 days, the median and lateral anlagen have fused and the thyroid gland has migrated to its definitive location in the anterior neck. By 2 months of fetal life [70 days of gestation], iodide concentration, TSH receptors, thyroglobulin and thyroid peroxidase messenger RNA (m. RNA), and protein can be demonstrated within the thyroid gland. By 4 months of fetal life [late 2 nd trimester ] the thyroid is well formed , has full axis and able to produce thyroid hormones

What control Thyroid embryo genesis ? Thyroid embryogenesis is dependent on production of a programmed sequence of homeobox and transcription factors : @ TTF-1 , 2 [thyroid transcription factors 1 and 2} @ PAX-8. Targeted mutation in mice TTF-1 ------Thyroid gland aplasia TTF-2 ----- Ectopic, sublingual thyroid gland. PAX-8 ---- Hypolasia (very small thyroid gland ) Mutations in these genes, however, account for only approximately 2% of human thyroid dysgenesis.

1 Congenital hypothyroidism Prevalence o Worldwide 1: 4, 000 infants o Hispanics /Native Americans 1 : 2, 000 o Black Americans 1 : 32, 000 Male : Female 1: 2
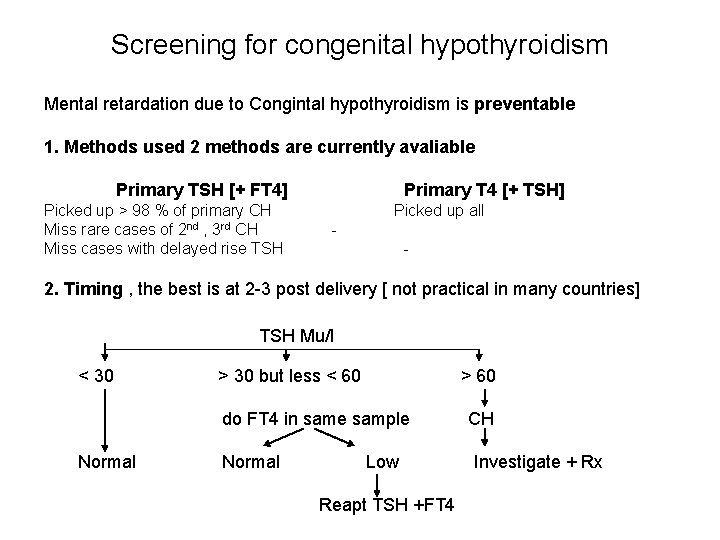
Screening for congenital hypothyroidism Mental retardation due to Congintal hypothyroidism is preventable 1. Methods used 2 methods are currently avaliable Primary TSH [+ FT 4] Picked up > 98 % of primary CH Miss rare cases of 2 nd , 3 rd CH Miss cases with delayed rise TSH Primary T 4 [+ TSH] Picked up all 2. Timing , the best is at 2 3 post delivery [ not practical in many countries] TSH Mu/l < 30 > 30 but less < 60 > 60 do FT 4 in same sample Normal Low Reapt TSH +FT 4 CH Investigate + Rx

Primary Hypothyroidism A. Defect of fetal thyroid development Aplasia, ectopia (dysgenesis) B. Defect in thyroid hormone synthesis (e. g. , goitrous hypothyroidism) 1. Thyroid oxidase mutations: Permanent (homozygotic) Transient (heterozygotic) 2. Iodide transport defect 3. Thyroid peroxidase defect 4. Thyroglobulin synthesis defect 5. Deiodination defect C. Iodine deficiency (endemic goiter) Neurologic type Myxedematous type D. Maternal Factors 1. antibodies TSH receptor blocking antibody (TRBAb) Other name TSH binding inhibitor immunoglobulin) 2. Maternal medications Propylthiouracil Methimazole Amiodarone 3. Radioiodine, iodides dyshermogensis
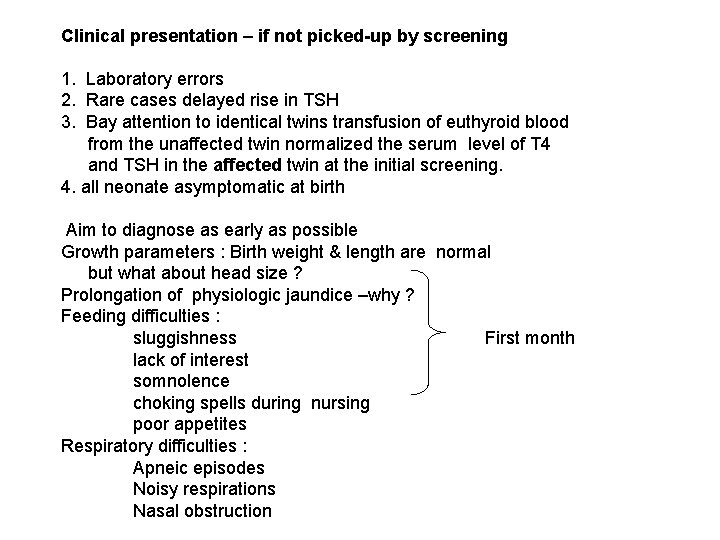
Clinical presentation – if not picked-up by screening 1. Laboratory errors 2. Rare cases delayed rise in TSH 3. Bay attention to identical twins transfusion of euthyroid blood from the unaffected twin normalized the serum level of T 4 and TSH in the affected twin at the initial screening. 4. all neonate asymptomatic at birth Aim to diagnose as early as possible Growth parameters : Birth weight & length are normal but what about head size ? Prolongation of physiologic jaundice –why ? Feeding difficulties : First month sluggishness lack of interest somnolence choking spells during nursing poor appetites Respiratory difficulties : Apneic episodes Noisy respirations Nasal obstruction

Constipation (Difficult to treatment). Anemia is often present and is refractory to treatment with iron What type of anemia ? Physical Examinations : IF early can be essentially normal In long standing untreated The temperature is subnormal, often less than 35°C The face may suggest diagnosis protruded tongue (minimal initially) The abdomen is large Umbilical hernia is usually present. Skin of limbs cold & mottled. Edema of the limbs & genitals CVS examinations may show : The pulse is slow Heart murmurs Common finding Cardiomegaly But commonly Asymptomatic pericardial effusion overlooked. Because symptoms appear gradually, the diagnosis is often delayed.
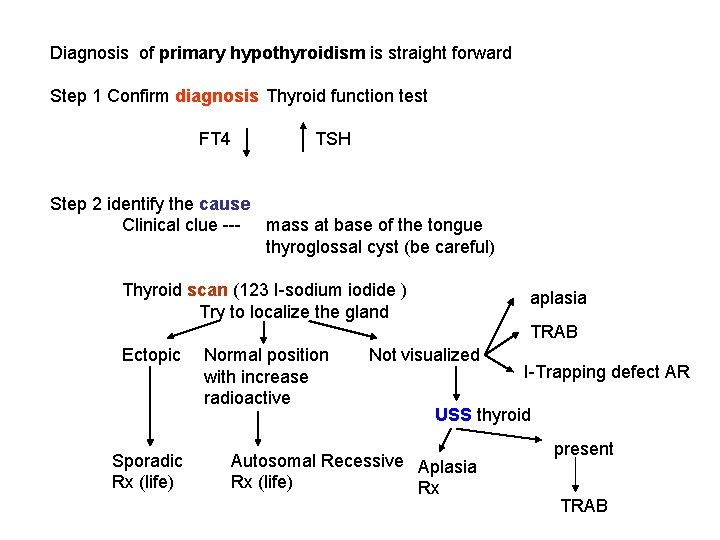
Diagnosis of primary hypothyroidism is straight forward Step 1 Confirm diagnosis Thyroid function test FT 4 TSH Step 2 identify the cause Clinical clue mass at base of the tongue thyroglossal cyst (be careful) Thyroid scan (123 I sodium iodide ) Try to localize the gland aplasia TRAB Ectopic Sporadic Rx (life) Normal position with increase radioactive Not visualized I Trapping defect AR USS thyroid Autosomal Recessive Aplasia Rx (life) Rx present TRAB

Treatment Guide lines Start treatment as possible early mean Idealy < 2 weeks but < 6 week is ok Start 8 micg/kg/dose [once dialy] l thyroxine is tablet thus embrically use 37. 5 micg l thyroxine once daily or embrically use 50 micgs Reapt the TFT after 2 weeks where most infant normalize FT 4 Aim to keep FT 4 at the upper half of normal. TSH may still elevated , ignore as far FT 4 is in the target range Follow-up : At 2 , 4 weeks of start Every month for frist 6 months Every 2 months for the rest of year Every 3 month till age 3 years Every 4 month till growth & puberty completed Every 2 weeks if you change the dose More frequents if there is concern about the compliance

Infant treated at age < 6 weeks and maintained normal FT 4 in first 3 years of age their IQ=Normal

Thyroid in older children and Adults 1 -Symptoms & Signs Thyroid hormone disturbance - due to deficiency or excess circulating thyroid hormone Over-secretion (Hyper-) ( ) Symptoms ) General Environment Sleep Bowel habit Skin Lethargic “cool” Cold intolerance Excessive Constipation Cold, dry skin “Fatigue” due to irritability , Nervousness Heat intolerance little sleep “Insomnia” Diarrhoea “Increased bowel movements” Warm , moist skin Signs Under-Secretion-Hypo- ( Face Weight CVS Pulse Hands Lower Limbs Muscle strength peri orbital puffiness Gain ? Slow H. R weak , small volume Cold , dry Cold Dry Weakness (proximal) Exophalmos , Lid lag Loss Rapid Heart Rate ! Palpitations Rapid bounding Moist , Trembling hands pre tibial myxoedema Weakness (proximal)

2 -Neck Mass and its effect – Thyroid enlargement (goitre) • It can be diffuse (generalised) and involve both thyroid lobes, or it can be more focal, as in nodular thyroid disease. • Patients and/or their relatives often notice a goitre as the first of a thyroid problem swallowing problems (dysphagia) 3 - Extreme presentation Myxoedema coma Thyroid storm

Examine the Eyes Look for * Proptosis (exophthalmia) examine from lateral view Hyperthyroidism * Lid retraction – if you can see the upper part of sclera Hyperthyroidism * Lid lag by examination Move you finger from up to down Observe for upper lid lags behind Hyperthyroidism Additional examinations A Hand examination Examine the palmar Skin : Moist Hyper Dray skin Hypo Palmer erythema Hyper Examine the Nails clubbing acropathy Grave’s (hyperthyroidism) Graves’ acropachy there is digital clubbing, thickening of the skin of the digits Examine for tremor – extend the hands / Paper Examine the Pulse Low pulse hypo bradycardia Rapid pulse hyper tachycardia Irregular (atrial fibrillation) not in exam) B Muscle (upper /lower) examination looking for proximal myopathy for upper limp ask patient to rise his both arms above head for lower limp ask patient to stand up C. Examination lower limp for pretibial myxoedema (Graves' dermopathy, thyroid dermopathy) 1 5%. Examination reflexes Slow / absent reflex Hypothyroidism Hyper reflexes Hyperthyroidism

Overall Approach to thyroid a thyroid problem can be rationally determined and subsequently managed by combining: • the history • clinical thyroid assessment • measurements of blood thyroid hormone levels • antibody studies; Anti microsmal antibodies anti thymoglobulin antibodies • thyroid imaging – thyroid technetium nuclear medicine scan – thyroid ultrasound • Fine needle biopsy
- Slides: 14