Elimination Basic Principles Wash Hands Wear Gloves Infection

Elimination

Basic Principles § Wash Hands & Wear Gloves § Infection control, your protection & your client’s protection § Privacy § Embarrassing § Positions for urination § Independence

Functions of Urinary System § Remove wastes from blood to form urine § Remove nitrogenous waste products of cellular metabolism § Regulates fluid and electrolyte balance The nephron = functional unit of the kidney and forms the urine

Goal of Urinary System § To maintain chemical homeostasis of the blood. § Filtration by the Nephrons § H 2 O, glucose, amino acids, urea, creatinine, major electrolytes § Not normally large proteins or blood cells § Proteinuria is a sign of glomerular injury § Normal adult 24 hr output = 1500 -1600 ml.

Overview of Urinary System § Kidneys § Bean shaped organs § Either side of vertebral columns T 12 – L 3 § Right kidney lower due to liver § Urine produced with filtration of blood through nephrons § Major role in fluid & electrolyte balance

§ Ureters § Connect kidneys to bladder § 10 -12 in length, ½ in diameter in adult § Peristaltic waves § Renal colic § Micturition

§ Bladder § Distensible, muscular sac § Reservoir for urine ( approx. capacity = 600 mls ) § Organ of excretion ( norm. voiding= 300 mls) § Lies in pelvic cavity behind symphysis pubis

§ Urethra § Short, muscular tube § Urine from bladder to meatus and from the body § Female 4 -6. 5 cm (1 ½ - 2 ½ in. ) length § Male 20 cms ( 8 in. ) § Urinary and reproductive systems

§ Meatus § External opening of the urethra, male & female § The need to void is a conscious awareness

Life Cycle Changes § Infants & children § Unable to concentrate urine b/c kidneys are immature § Urine is light yellow § Void frequently § Voluntary control @ 24 mos. when neuromuscular structures develop

§ Adult § 1500 – 1600 mls urine/24 hrs § Concentrates urine – normal is amber colored § Nocturia § Not usually § Decreased renal blood flow during rest § Ability to concentrate urine

§ Elderly § Micturition impaired § mobility § Diseases, alzheimer’s, CVA § Physiological age related changes § Bladder loses muscle tone and capacity § Kidneys lose ability to concentrate urine § Bladder loses muscle strength

Common Problems § Urinary Retention § Accumulation of urine in the bladder § Inability to empty § Pressure, discomfort and tenderness § Residual Urine = urine retained in the bladder after voiding

§ Incontinence § Loss of voluntary control to void § Infection, nerve damage to bladder or brain, spinal cord injury, or aging process § Total incontinence = no control § Stress incontinence = sm. amts. Urine excreted involuntarily with coughing or laughing At risk for skin breakdown related to acid urine next to skin. Adult Diapers or Attends

§ § Frequency & Urgency Nocturia Enuresis – involuntary discharge of urine Nocturnal Enuresis § During sleep § Bed-wetting children 5 yrs and older § Oliguria § 30 mls/hr or 720 mls/24 hrs
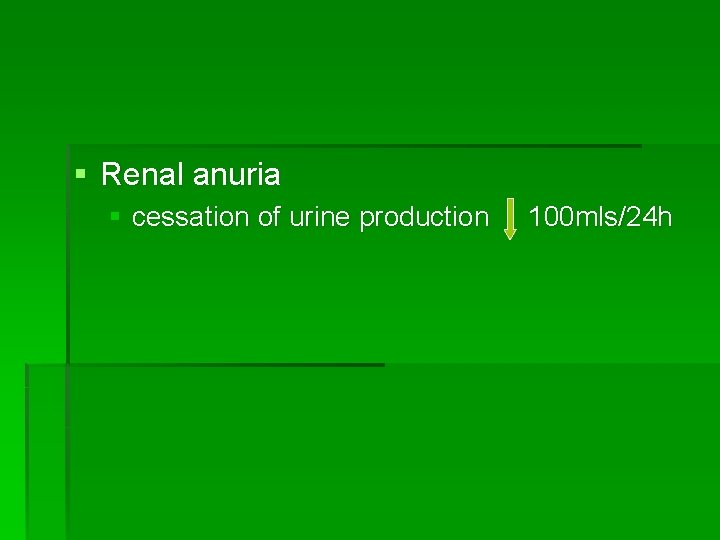
§ Renal anuria § cessation of urine production 100 mls/24 h

Promoting Healthy Urinary Elimination § Urinate as soon as the urge is felt § Avoids stasis and distention § Prevents urgency, infection, and incontinence § Drink about 2 liters fluid/day § Limit Na, caffeine, and alcohol

§ For people with Nocturia § § § fld. Intake in the p. m. caffiene and alcohol Void before bedtime § For Women § § Wipe perineum front to back Void soon after intercourse Wash hands Pelvic – floor strengthening exercises (Kegel Exercises)

Client Education § § S & S of infection Fluid intake ( if no restrictions 2 -5 L/day ) Perineal hygiene Meds. & side effects on urination, color, and volume

Facilitating Micturition § Nursing Measures to promote voiding in people who are having difficulty: 1. 2. 3. 4. 5. Privacy and natural position Providing commode or bathroom Running water Warm water to dangle fingers Warm water over perineum ( measure if on In/Out )

6. Gently stroking inner thighs or pressure to symphysis pubis 7. Pain relief Warmth to the bladder & perineum relaxes muscles & facilitates voiding. ( Sitz bath or warm tub ) If unsuccessful- urinary catheterization may be indicated

§ Promoting complete bladder emptying § Prevention of infection § Good perineal hygiene § Adequate fld. Intake § Dilutes urine & flushes urethra § Acidifying urine ( inhibits microorganisms) § Cranberry juice, whole grain breads, meats, eggs, prunes and plums.

Indwelling Catheter Care § Goal- prevent infection & maintain unobstructed flow of urine. Monitor for problems. § Perineal hygiene @ least 2 x/day and prn § Do not advance catheter further into urethra during perineal care

Catheter Care § § § Fld intake (3 L/day ) Handwashing and Gloves Positioning § Urine bag § Tubing

Bowel Elimination § Function- excrete/eliminate waste products of digestion. § Maintaining normal bowel elimination is essential to health and efficient body functions.

GI System § Small Intestine § Absorption nutrients & electrolytes § 20 ft length, 1 in. diameter § 3 sections § Duodenum § Jejunum § Ileum

GI § Large Intestine § Absorbs H 2 O and electrolytes § Temporarily stores waste products § Main function is elimination § 5 – 6 ft. length, 6 – 7 cm. diameter § Cecum § Ascending colon ( Right side ) § Transverse colon § Descending colon

Patterns through life cycle § Babies: 3 – 6 BM’s/day § Children: § Neuromuscular structures not developed until 15 – 18 mos. § Voluntary control 2 – 3 yrs. § Pregnant women prone to constipation § Pressure on abd. Organs § Iron supplements

§ Elderly prone to constipation § Slowing of peristalsis

Determinants affecting elimination § Dietary patterns & fld. Intake § 6 – 8 glasses H 2 O/day ( 1400 - 2000 mls ) § fld. Liquifies stool § Dietary fiber stimulates peristalsis § Soft stool

Factors affecting elimination § Fiber ( undigestible residue ) provides bulk § Absorbs fluid § Increases stool mass § Bowel wall stretches § Peristalsis stimulated § Defecation results

Factors affecting elimination § Personal habits § Busy schedule, postpone BM, constipation § Activity & exercise § Immobile activity in colon § Medications § Laxatives § Narcotics with codiene

Factors affecting elimination § Emotions § Anxiety peristalsis & diarrhea § Depression § Pain § Surgery § Anaesthetic causes temporary cessation of peristalsis § Direct manipulation of the bowel stops peristalsis

Common Problems 1. Constipation – difficult passage of hard, dry stool; infrequent movements 2. Fecal Impaction – unrelieved constipation, feces wedged in rectum, no BM usually 3 days, oozing of diarrheal stool develops 3. Diarrhea- # liquid stool 4. Flatulence – abd. Distention & pain

Common Problems § Incontinence – inability to control passage of stool § Hemorrhoids § Dilated engorged veins § Increased pressure when straining § Internal / external § Bleeding

§ § Daily BM Not essential. 2 / week a concern Defecation pattern BM, Stool, Feces, Defecate – all mean waste products expelled via the bowel
Promoting Healthy Bowel Elimination ü Privacy ü Squatting position ü Bedpan position ü Cathartics & laxatives ü Anti- diarrheal agents ü Enemas ü disimpaction

ü Bowel routine üDaily time clock üHot drinks üStool softeners üPrivavy üPosition and abdominal pressure üBearing down

Assissting with Elimination § Embarrassing & stressful § Usually urge to defecate 1 hr. Pc § Bedpans § Metal or plastic § Regular or fracture pan § Cleanliness § Urinals § Commode

Procedure § § § § Privacy- close door, Side rail as needed Recumbent with HOB Tissue Call bell Leave alone if possible Gloves Clean genitals

Procedure § § § § Remove pan and cover In & Out Specimens Clean pan Wash hands yours and client’s Lower bed Client comfort

Peri - Care § Cleaning of genitals , routine part of complete/ partial bed bath § Incontinence

Procedure for Peri Care § Regular patient § Simple explanation- layman’s terms § Privacy § Gloves § Dorsal recumbent position § Incontinent pad under buttocks § Warm soap and water § Female – separate labia

Procedure for Peri Care § Male – begin penile head move down along shaft, retract foreskin, rinse and dry.

Procedure for Peri Care § Catheter – § Q 8 hrs. § Clean perineum & 2 in. Of catheter § No powders / lotions § Avoid advancing catheter § Keep urine drainage bag off floor but below level of bladder § Empty bag Q 8 – 12 hrs or when bag is full, remember to mark amt. Emptied on In/Out sheet

§ Avoid use of baby powder/ cornstarch § No medicinal purpose § Can form clumps or will cake in creases § Use vaseline/ zincoxide as skin barrier for incontinent clients

Suppository Administration § § § Check physician’s order, protocol Left Lateral position Gloves Lubication Hold with thumb and index finger Insert with index finger (3 – 4”) never force § Deep breath = relaxes anal sphincter

§ Caution § Vagus nerve stimulation cause heart rate to slow – avoid excess manipulation

Enema Administration § Main purpose § Promotion of defecation, stimulate peristalsis § The fluid breaks up fecal mass, stretches the rectal wall & initiates the defecation reflex

Types of Enemas

Cleansing Enemas § Tap Water § Hypotonic § Used only once § Electrolyte imbalance § Water toxicity § Circulatory overload ( concentration gradient)

§ Normal Saline § Used when more than one enema is needed § Safest § Isotonic § Large volume to distend bowel

§ Hypertonic Solution § Smaller volume of fluid § Draws from surrounding tissue into bowel to soften stool and stimulate peristalsis § Fleets – sodium phosphate § Low volume, concentrated solution
§ Soap suds § Less common § Soap irritates the bowel § 5 – 15 mls. Castile soap in 1000 mls warm water

§ Oil Retention § Oil based solution § Lubricates the rectum and colon § Softens stool, easier to pass § Retain 1 – 2 hrs if possible § Follow with cleansing enema

§ Medicated § Instill meds. § Rectal mucosa absorption § Ex. – Kayexalate to K (potassium). Absorbs K from the intestinal tract

Volumes for Enemas § Large Volume § 500 – 1000 mls. § Container 12 – 18 in. above the bowel § Lg. Volume stimulates & causes evacuation of stool § Small Volume § 500 mls. § Container 12 in. above bowel

Volumes for Enemas § Pre packaged § Fleet 150 mls § Microlax 5 mls § Hypertonic solution § User friendly § Hold for 5 min. § Oral Fleet

§ Prepackaged used more than large volume because: § Works § Less risk for electrolyte imbalance § Rapid administration § Less discomfort and distention § Convenient and quick

§ Physician’s order reads “ enemas to clear” § No more than 3 total given § Return solution will be highly colored but no solid stool § Isotonic solution (normal saline) Excess enema use seriously depletes fluid and electrolytes

Procedure for Enema Administration § Confirm Dr’s order, prepare client, verbal consent, equipment, privacy § Left lateral position ( fld. Flows by gravity) § Drape, pad under buttocks § Warm solution- stimulates peristalsis § Hot sol’n burns mucosa § Cold sol’n causes cramping

Procedure for Enema Administration § § Prime tube Lubricate tip Glove Insert 7 – 10 cm. (3 -4 in) adult § Do not force § Deep breath § Guide toward umbilicus

Procedure for Enema Administration § Container at appropriate height § Lg. = 12 – 18 in § Sm. = 12 in § 1000 mls takes ~ 10 min to instill § Higher the bag – greater the pressure § C/O discomfort, lower bag, slow infusion, stop, then start again § Remain side lying to retain 5 – 10 min. or as long as possible

Procedure for Enema Administration § § § Assist to bathroom or give bedpan Evaluate results Document § Type & volume of enema § Color, amount, consistency of fecal return § Hygienic measures for client § Wash Hands

Ostomy Care

§ Certain diseases require surgical interventions to create an opening into the abdominal wall for fecal and urinary elimination § Enterostomy – the surgical procedure performed to produce the artificial stoma.

Definitions § Ostomy = opening made to allow passage of urine or stool § Piece of intestine is brought out onto the client’s abd. § Lacks nerve endings § Doesn’t hurt to touch but has other implications § Stoma = mouth like opening in the abdominal wall to drain urine or stool

§ Effluent – drainage from stoma § Bowel ostomies § Cancer ( Ca) § Drain fecal material § Consistency depends on location § Higher up = more liquid § Greater risk skin irritation b/c concentration of digestive enzymes

§ Ileostomy § End of small intestine § By passes lg. Intestine = freq. Liquid stools § Colostomy § Large intestine § More solid stool

§ Ostomies may be permanent § More common § temporary § Rest the bowel § Crohn’s

Urinary Ostomies § Provide drainage of urine that bypasses the bladder = Urinary Diversion § Ureterostomy § Ureter to abd. Wall § Lt. , Rt. , Bilateral

Ileal Conduit § § § 6 – 8 in. ileum 1 end for external opening Other end closed off Ureters implanted into this piece of bowel Pouch Urine will have shred of mucus b/c bowel still produces same

Concerns § Infection § Sterile ureters provide opening into system § Skin Breakdown § Continuous drainage § Moisture on skin § Replace urinary pouch q 2 -3 days

Pouching an Enterostomy § § Effluent ( drainage ) may begin immediately Collects all effluent Protects the skin Stoma should be moist and reddish pink (same as other mucus membranes) § Flush to skin or bud-like protrusion § Black, purple, dry = inadequate circulation

Pouch with Skin Barrier § § Comfortable fit Cover skin surrounding stoma Good seal Post-op pouch should allow for visibility of stoma

Types of pouches and skin barriers § One Piece Pouching System § Skin barriers preattached, precut, custom fit § Two Piece System § Skin barrier with flange ( plastic ring) § Corresponding size pouch § Assess stoma § § § Measure correct size Change q 3 -7 days Empty 1/3 to ½ full, expel flatus prn

Steps to Care for Ostomies § § § Supine position Wash hands, glove Remove pouch & skin barrier, push skin away from barrier § Cleanse peristomal skin gently with warm tap water and clean cloth § Do not scrub, Avoid soap ( residue- pouch won’t adher)

Steps to Care for Ostomies § § Correct sizing Cut opening 1/16 – 1/8 larger than stoma Remove backing Ileostomy- apply thin circle barrier paste around opening of pouch and allow to dry (if creases or bumps use barrier paste to even surface for pouch application)

Steps to Care for Ostomies § Pouch should point to client’s knees § Maintain gentle finger pressure around barrier for 1 -2 min. § Picture frame flange with non allergic paper tape § Ostomy deodorant for pouch § Tub bath or shower

Steps to Care for Ostomies § § Normal stoma oozes blood if rubbed Actual bleeding into pouch is abnormal Pouch covers are available The client will be watching the nurse during ostomy care to gage reaction. § Be conscious of facial expression & nonverbal cues

Steps to Care for Ostomies § Education § Counseling § Body image § Self care § Fear of rejection § Sexual function § Powerlessness over bowel regulation
- Slides: 81