Elective Stenting versus Balloon Angioplasty with Bailout Stenting

Elective Stenting versus Balloon Angioplasty with Bail-out Stenting for Small Vessel Coronary Artery Disease: Evidence from a Meta-analysis of Randomized Trials TCT, Washington, 30 September 2004

There are no conflicts of interest nor funding to declare Pierfrancesco Agostoni on behalf of all co-authors

INTRODUCTION Bare-metal stents have been shown to reduce angiographic restenosis and repeat revascularization in discrete lesions in large vessels. 1, 2 The use of stents has increased radically also for “non-STRESS/BENESTENT” lesions, despite the lack of evidence of benefit. 1. Serruys PW, et al. BENESTENT Trial. NEJM, 1994 2. Fishman DL, et al. STRESS Trial. NEJM, 1994

INTRODUCTION Small vessels (with RVD < 3 mm) account for 40 -50% of all coronary stenoses. 3 Several recent randomized trials have compared bare-metal stenting vs. PTCA in small vessels, with conflicting and overall inconclusive results. 3. Wong P, et al. Catheter Cardiovasc Interv, 2000

INTRODUCTION As systematic overviews and meta-analytic techniques may provide more precise effect estimates with greater statistical power, leading to more robust and generalized conclusions. . .

AIM OF OUR REVIEW * Research * Retrieve * Evaluate * Combine in a systematic way all the randomized trials comparing bare-metal stenting vs. PTCA for the treatment of atherosclerotic lesions in small coronary vessels.

METHODS Systematic Research MEDLINE, CENTRAL AHA, ACC, ESC, TCT 2000 -2004 abstracts Inclusion criteria Prospective comparison Randomized allocation Intention-to-treat Follow-up 6 months Exclusion criteria Non-mandatory angiographic follow-up Use of DES or other devices stents Antithrombotic drugs ASA and thienopyridines

METHODS Primary End-points Death Myocardial infarction Repeat revascularization (TVR/TLR) MACE Secondary end-points Restenosis, RVD, MLD pre-, post-PCI and at follow-up, DS pre-, post-PCI and at follow-up, acute gain, late loss

METHODS Binary outcomes Odds Ratios (95% Confidence Intervals) Random effect model Heterogeneity Cochran Q 2 test

METHODS Pre-specified sub-group analysis 1, 2 Trials with mean DS post-PTCA < 20% (optimal) and Trials with mean DS post-PTCA > 20% (sub-optimal) 1. ACC Expert consensus Document JACC, 1998 2. Kastrati et al. JACC, 2001

Included Studies
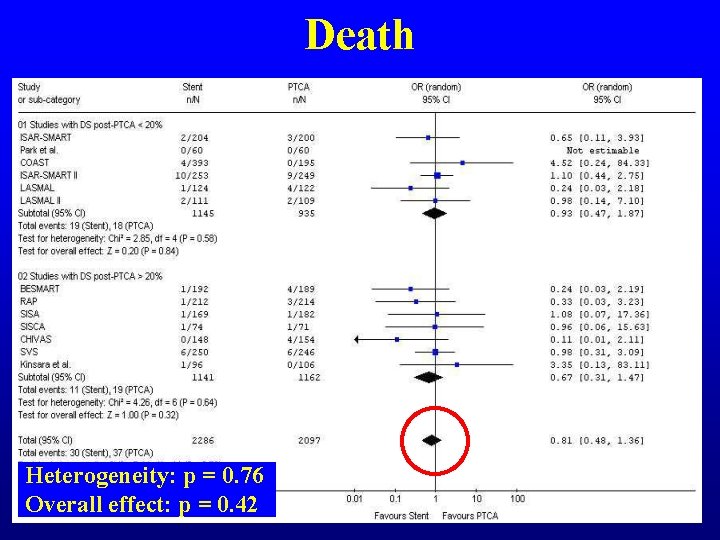
Death Heterogeneity: p = 0. 76 Overall effect: p = 0. 42
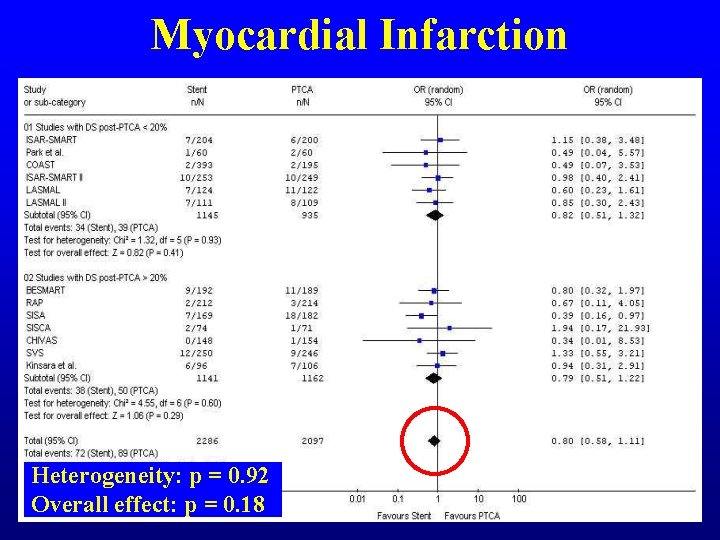
Myocardial Infarction Heterogeneity: p = 0. 92 Overall effect: p = 0. 18
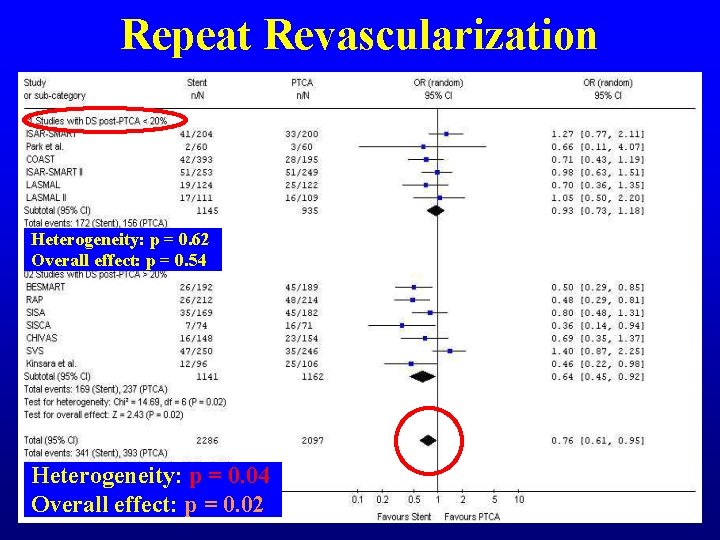
Repeat Revascularization Heterogeneity: p = 0. 62 Overall effect: p = 0. 54 Heterogeneity: p = 0. 04 Overall effect: p = 0. 02
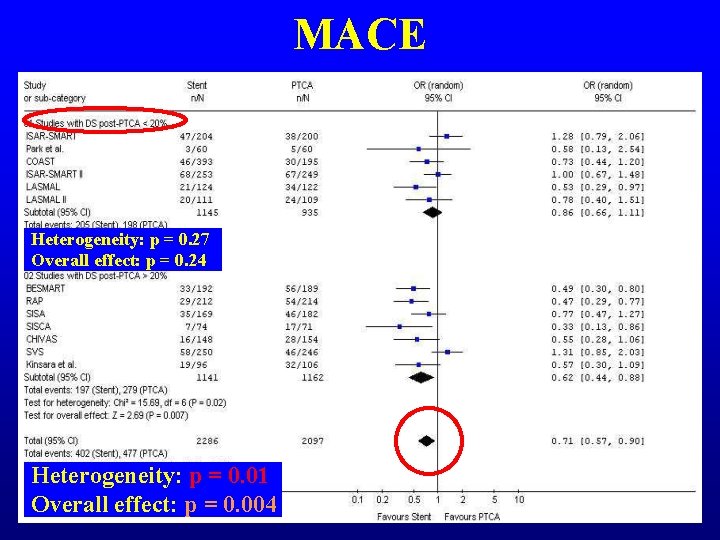
MACE Heterogeneity: p = 0. 27 Overall effect: p = 0. 24 Heterogeneity: p = 0. 01 Overall effect: p = 0. 004

CONCLUSIONS Bare-metal stenting is clinically superior to PTCA for the treatment of small vessels, in particular when compared to a sub-optimal PTCA result. The finding of significant heterogeneity casts a light of caution on the comprehensive pooled effect estimates. A strategy based on “optimal” PTCA with provisional stenting may be a valid alternative to systematic stenting.

CONCLUSIONS In any case, the rates of MACE (17%) and repeat revascularization (15%) remain high after stenting, unfavorably comparing with the MACE and revascularization rates in vessels with RVD > 3 mm ( 10%). 4, 5 4. Weaver WD, et al. OPUS-1 Trial. Lancet, 2001 5. Serruys PW, et al. JACC, 1999

Future Strategies As drug-eluting stents have been proved to be effective both in randomized trials 6 -8 and The use of DES should be considered the 8 in observational registries … first-line therapy for 6. the treatment of vessels with RVD < 3 mm. Schofer J, et al. E-SIRIUS Trial. Lancet, 2003 7. Schampaert E, et al. C-SIRIUS Trial. JACC, 2004 8. Ardissino D. SES-SMART Trial. ACC meeting, 2003 8. Lemos PA, et al. RESEARCH Registry. AJC, 2004

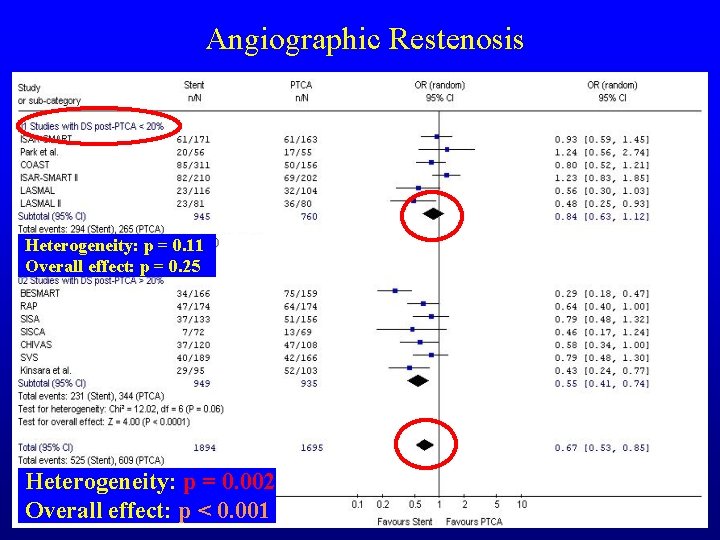
Angiographic Restenosis Heterogeneity: p = 0. 11 Overall effect: p = 0. 25 Heterogeneity: p = 0. 002 Overall effect: p < 0. 001



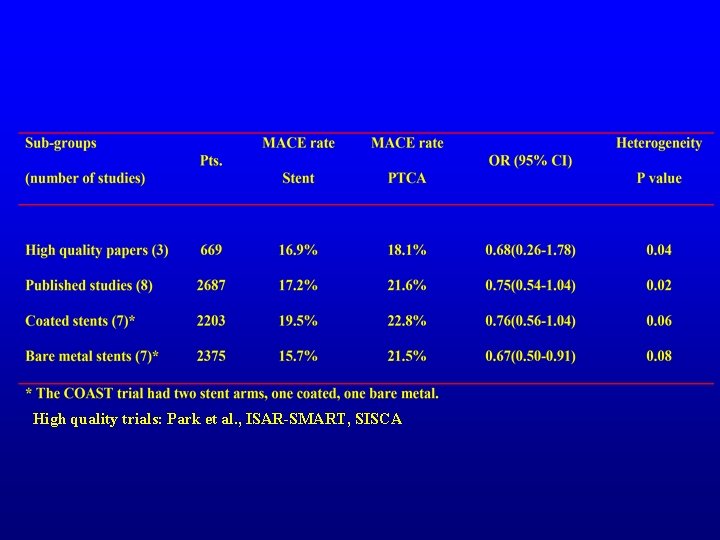
High quality trials: Park et al. , ISAR-SMART, SISCA

Quality Assessment Jadad’s Score (0 -5 points) • Study defined as randomized (1 point) – if randomization was correct 1 point more – if not correct 1 point less – if not mentioned no points • Study defined as blinded (1 point) – it is impossible in “interventional” trials! Stent is visible! • Clear description of drop-outs and withdrawals (1 point)

For further slides on these topics please feel free to visit the metcardio. org website: http: //www. metcardio. org/slides. html
- Slides: 26