Effectiveness of a medication discharge plan to reduce















- Slides: 24

Effectiveness of a medication discharge plan to reduce discrepancies between hospital and ambulatory settings: a pragmatic randomized controlled trial MC Vanier, L Lalonde, AM Lampron, P Levasseur, R Khaddag, N Chaar Faculty of pharmacy, Université de Montréal Cité de la Santé Hospital Marie-claude. vanier@umontreal. ca

INTRODUCTION • About 10% of patients will experience adverse drug events after discharge 1 – 42% of life-threatening and serious adverse events preventable 2 • 42% to 82% of patients have at least one medication discrepancy after discharge – 10% of these discrepancies are considered serious • Rehospitalisation rate higher when discrepancies observed (14, 3% vs. 6, 1%) 1 - Forster AJ et al. CMAJ 2006; 174(7)921 -2. 2 - Bates DW wt al. JAMA 1995; 274(1): 29 -34.

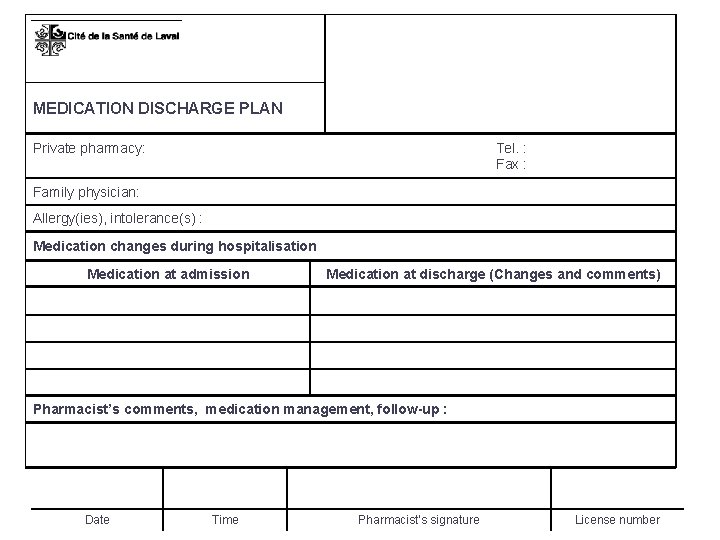
INTRODUCTION • Medication discharge plan (MDP) is medication related written information transferred from hospital to community pharmacist and family physician – Completed by hospital pharmacist – Information transferred: • medication at admission • medication changes during hospitalisation • additional clinical comments on medication issues important for seamless care

INTRODUCTION • Many studies assessed acceptability and feasibility of MDP • Only one assessed specifically MDP related outcomes – Integrated MDP/discharge prescription – Decrease in the rate of discrepancies between discharge prescription and pharmacy chart (60% vs 18% of patients with at least one discrepancy) – Not randomized controlled – Did not compare with patient self-reported medication use

OBJECTIVES • Evaluate impact of sending MDP to family physician and community pharmacy on medication discrepancies: 1) with pharmacy chart 2) with patient self-reported medication use few days after discharge

Study design and patients • Open, randomised controlled trial • Inclusion criteria: – ≥ 18 years old – Discharged from a geriatric, family medicine or psychiatry ward – At least 2 medication changes during hospitalisation – Medication history by hospital pharmacist during hospitalisation

Study design and patients • Exclusion criteria – – – Not French or English speaking Transferred to another hospital or a rehabilitation center Not available for phone interview following discharge No identified community pharmacy Already recruited in this study in a prior hospitalisation

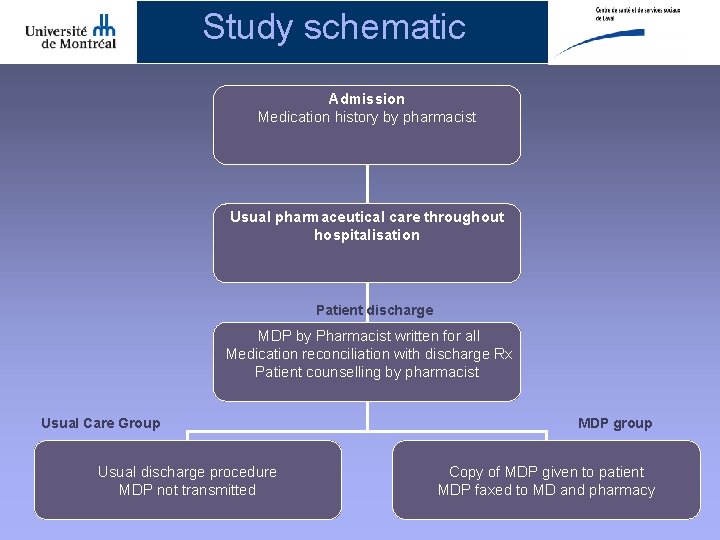
Study schematic Admission Medication history by pharmacist Usual pharmaceutical care throughout hospitalisation Patient discharge MDP by Pharmacist written for all Medication reconciliation with discharge Rx Patient counselling by pharmacist Usual Care Group Usual discharge procedure MDP not transmitted MDP group Copy of MDP given to patient MDP faxed to MD and pharmacy

MEDICATION DISCHARGE PLAN Private pharmacy: Tel. : Fax : Family physician: Allergy(ies), intolerance(s) : Medication changes during hospitalisation Medication at admission Medication at discharge (Changes and comments) Pharmacist’s comments, medication management, follow-up : Date Time Pharmacist’s signature License number

Discrepancies evaluation • MDP compared with three sources – Discharge prescription – Patient’s pharmacy chart • Obtained approximately one week after discharge – Self-reported medication use by patient • Systematic phone interview by research pharmacist approximately one week after discharge

Severity of discordances • Clinical impact of discordances blindly assessed individually by a clinical pharmacist and a family physician – If divergence, solved by consensus • Severity levels – Not clinically significant – Clinically significant but not life threatening – Serious: life-threatening or may cause important clinical problem or hospitalisation – Not enough information to make a decision – Not applicable

Statistical analyses • • All done with intent-to-treat approach Patient used as unit of analysis Proportion of patients with at least one discrepancy Percentage of discordant medication computed for each patient and each source of information • Difference between mean percentage of discordant medications was compared with Student t-test • Calculated sample size n=34 per group to detect a 40% difference – assuming a type I error of 5% and a power of 90%

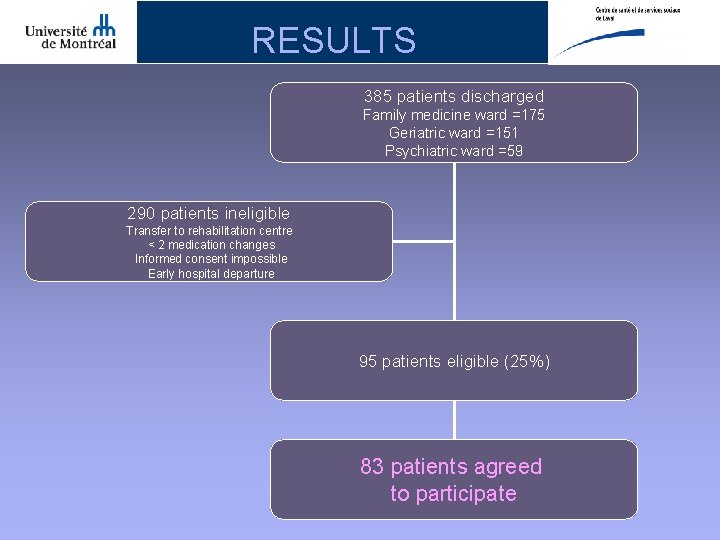
RESULTS 385 patients discharged Family medicine ward =175 Geriatric ward =151 Psychiatric ward =59 290 patients ineligible Transfer to rehabilitation centre < 2 medication changes Informed consent impossible Early hospital departure 95 patients eligible (25%) 83 patients agreed to participate

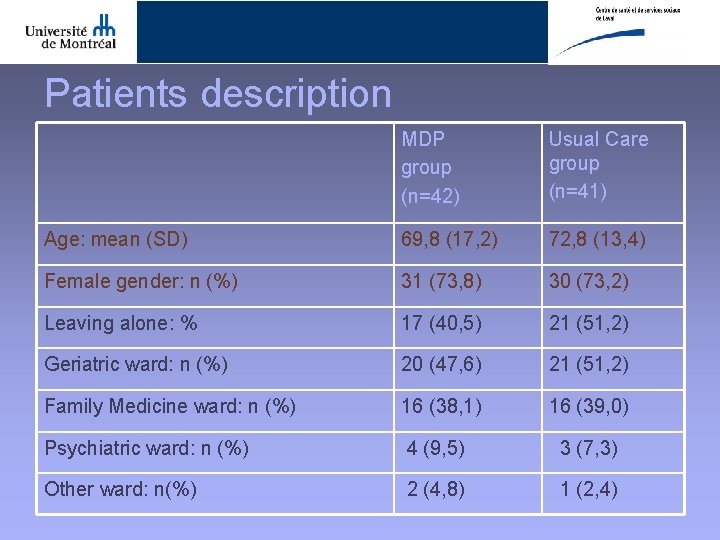
Patients description MDP group (n=42) Usual Care group (n=41) Age: mean (SD) 69, 8 (17, 2) 72, 8 (13, 4) Female gender: n (%) 31 (73, 8) 30 (73, 2) Leaving alone: % 17 (40, 5) 21 (51, 2) Geriatric ward: n (%) 20 (47, 6) 21 (51, 2) Family Medicine ward: n (%) 16 (38, 1) 16 (39, 0) Psychiatric ward: n (%) 4 (9, 5) 3 (7, 3) Other ward: n(%) 2 (4, 8) 1 (2, 4)

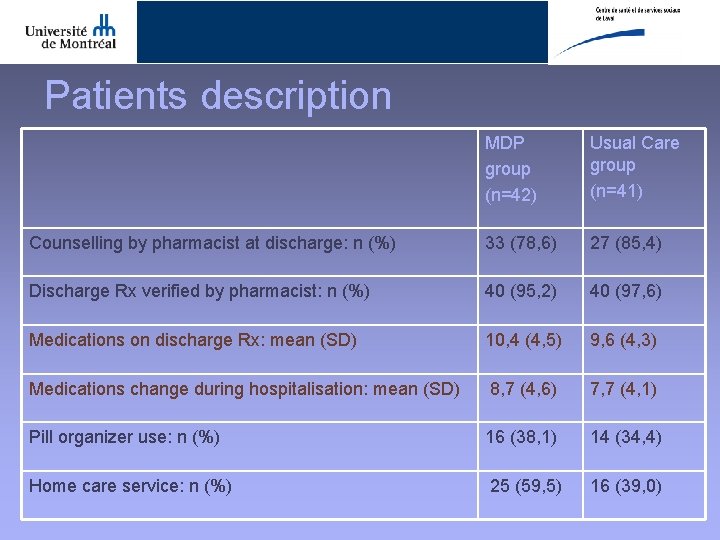
Patients description MDP group (n=42) Usual Care group (n=41) Counselling by pharmacist at discharge: n (%) 33 (78, 6) 27 (85, 4) Discharge Rx verified by pharmacist: n (%) 40 (95, 2) 40 (97, 6) Medications on discharge Rx: mean (SD) 10, 4 (4, 5) 9, 6 (4, 3) Medications change during hospitalisation: mean (SD) 8, 7 (4, 6) 7, 7 (4, 1) Pill organizer use: n (%) 16 (38, 1) 14 (34, 4) Home care service: n (%) 25 (59, 5) 16 (39, 0)

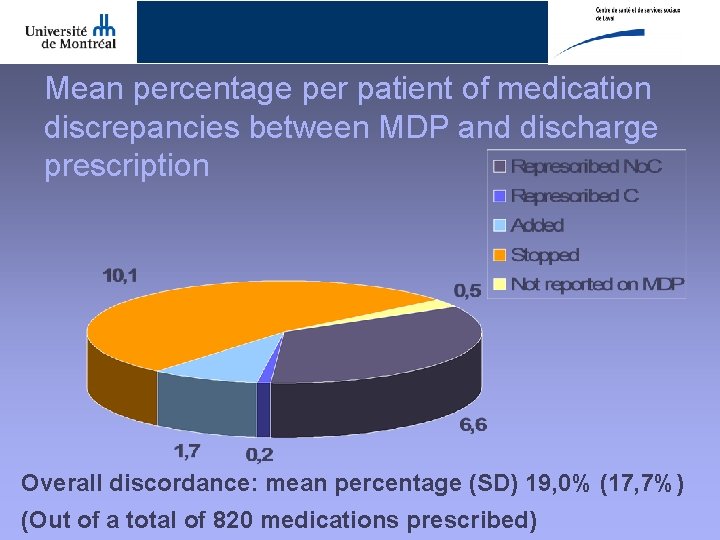
Mean percentage per patient of medication discrepancies between MDP and discharge prescription Overall discordance: mean percentage (SD) 19, 0% (17, 7%) (Out of a total of 820 medications prescribed)

Proportions of patients with at least one medication discrepancy between MDP and pharmacy chart • MDP patients: 66% • UC patients: 68%

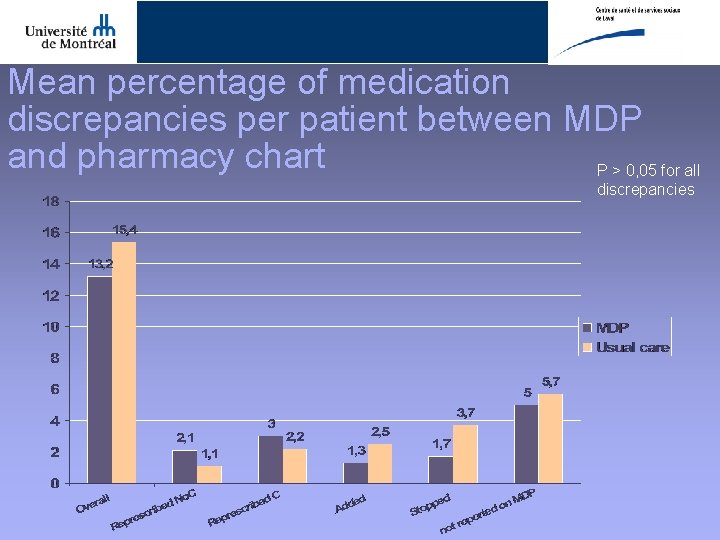
Mean percentage of medication discrepancies per patient between MDP and pharmacy chart P > 0, 05 for all discrepancies

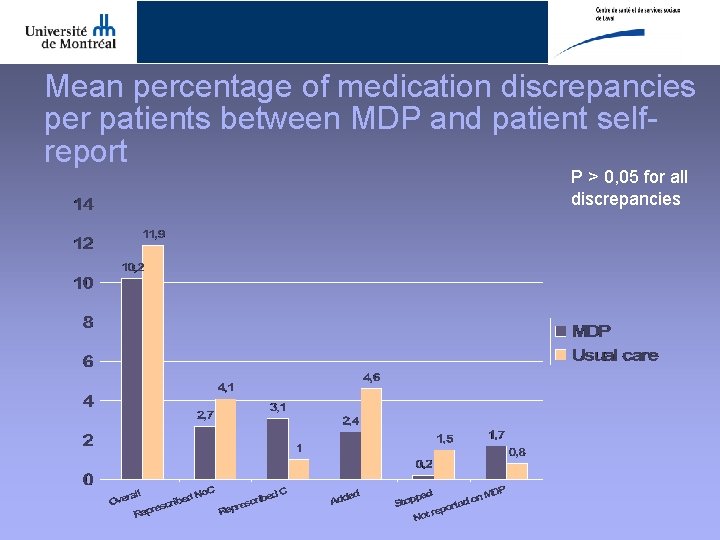
Mean percentage of medication discrepancies per patients between MDP and patient selfreport P > 0, 05 for all discrepancies

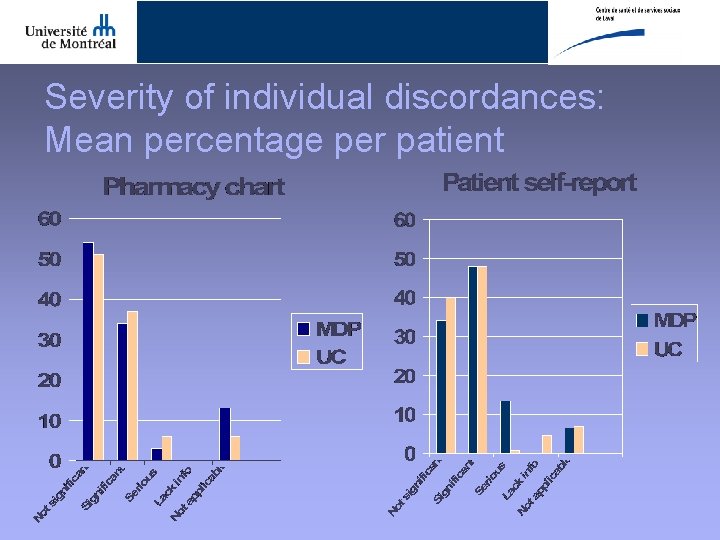
Severity of individual discordances: Mean percentage per patient

Examples of severity level of discrepancies • Not significant – PRN topical cream – PRN laxatives (stimulants, stool softeners) • Significant not life threatening – Antihypertensive agent stopped during hospitalisation due to hypotension but still active on pharmacy chart • Serious – Potassium supplements stopped during hospitalisation due to hyperkalemia on ACE but still active on pharmacy chart

CONCLUSION • High prevalence of medication discrepancies between hospital and ambulatory settings under real-life conditions – Pharmacy chart 13, 3% (MDP) 15, 4%(UC) – Patient self-report 10, 2% (MDP) 11, 9% (UC) • High rate of clinically significant discrepancies – About half of discrepancies with patient self-report are clinically significant or serious • Transmission of a MDP to community pharmacy and treating physician did not reduce medication discrepancies

SUGGESTIONS TO REDUCE MEDICATION DISCREPANCIES • Rigorous medication reconciliation process THROUGHOUT hospitalisation • Electronic medication information transfer tool interfaced with hospital patient information system • Integrated MDP/medication discharge prescription • Training of hospital and community pharmacists • Seamless care pharmacist to resolve medication discrepancies after discharge

DISCUSSION • Strengths of the study – Real life conditions • 52 pharmacies • Different ward pharmacists • Limitations of the study – – No prior training of community pharmacists No implementation phase of MDP prior to assessment Timing of information transfer Incomplete medication reconciliation • During hospitalisation • With ambulatory care settings