Effective Teaching and Learning Strategies in a Competencybased

Effective Teaching and Learning Strategies in a Competency-based Clinical Learning Environment April 21, 2017 Marcia Ditmyer, Ph. D Assistant Dean of Assessment and Instruction UNLV, School of Dental Medicine

All speakers agree that neither they nor members of their immediate family have any financial relationships with commercial entities that may be relevant to this presentation.

3 Marcia Ditmyer, Ph. D. , MS, MBA • Assistant Dean for Assessment and Instruction University of Nevada, Las Vegas School of Dental Medicine • AAL Senior Consultant • Education: • Ph. D. Public Health and Research/Measurement • MBA and MS Health Education • Experience: • 20 years Business and 17 years Higher Education • 31 of that in Healthcare Field

4 Learning Outcomes • Explain how the changing landscape of competency- based education has transformed instructional design and course planning strategies in a clinical environment. • Identify instructional techniques that are associated with high quality clinical teaching. • Examine practical applications for teaching and feedback styles effective with adult learners.

5 Learning Outcome 1

6 A Brief History Adopted by N. Chomsky in 1965, “…fundamental difference between the competence or knowledge of language and its application or actual use of language. ”

7 Competency-based ≠ Outcomes-based Competency-based education (CBE) is based on the broader concept of Outcomes-based education (OBE). Basically, know that a list of college credits and 1. Students we advance upon demonstrated competence. 2. Competencies include explicit, measurable, transferable grades on a transcript or even a diploma are poor learning outcomes empower students. can do. proxies that of what a student 3. Assessment is meaningful and a positive learning experience for students. 4. Students receive rapid, in differentiated supporta based Competencies, contrast, offer moreon their individual learning needs. of what a student both meaningful reflection 5. Learning outcomes emphasize competencies that include knows can of doknowledge with thatalong knowledge. application andand creation with the development of important skills and dispositions.
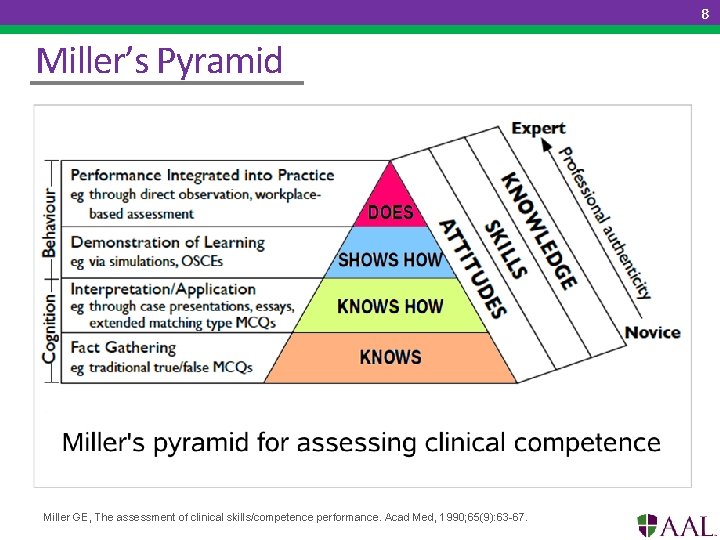
8 Miller’s Pyramid Miller GE, The assessment of clinical skills/competence performance. Acad Med, 1990; 65(9): 63 -67.
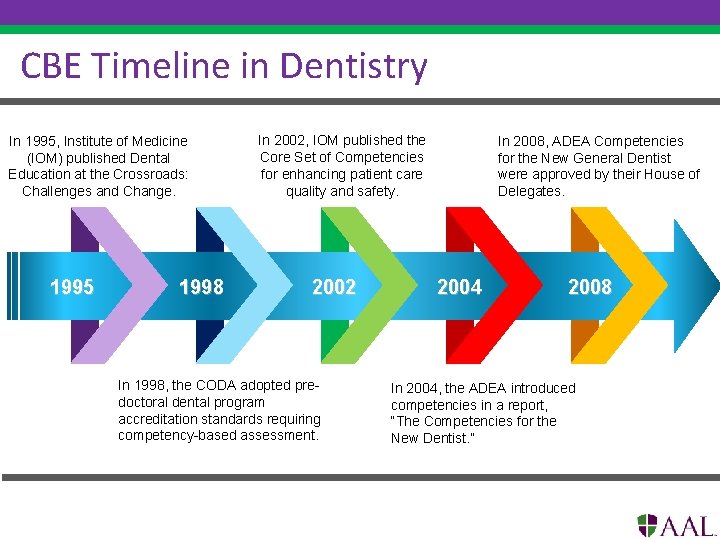
9 CBE Timeline in Dentistry In 1995, Institute of Medicine (IOM) published Dental Education at the Crossroads: Challenges and Change. 1995 1998 In 2002, IOM published the Core Set of Competencies for enhancing patient care quality and safety. 2002 In 1998, the CODA adopted predoctoral dental program accreditation standards requiring competency-based assessment. In 2008, ADEA Competencies for the New General Dentist were approved by their House of Delegates. 2004 2008 In 2004, the ADEA introduced competencies in a report, “The Competencies for the New Dentist. ”
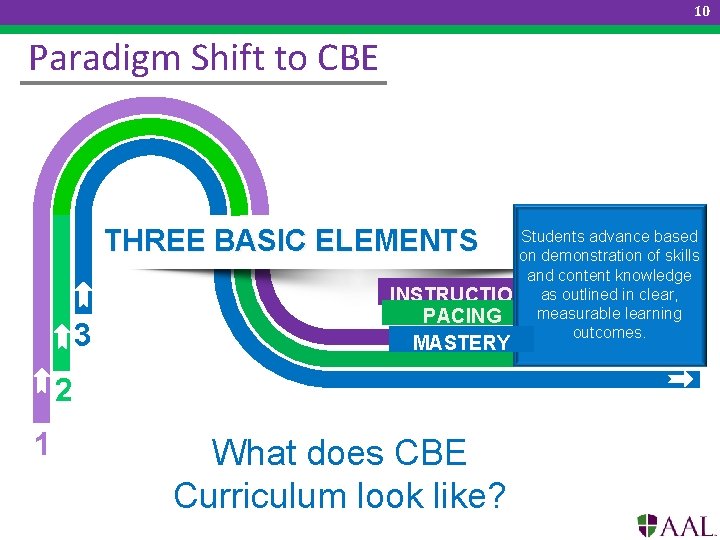
10 Paradigm Shift to CBE Students receive Students advance based Students progress at differential support to on demonstration of skills different ratesindividual in different match their and content knowledge areas, rather than learning needs; their as outlined in clear, INSTRUCTION knowledge teacher driven…it is and skills measurable learning PACING are increasingly learner driven. outcomes. challenged. THREE BASIC ELEMENTS 3 MASTERY 2 1 What does CBE Curriculum look like?
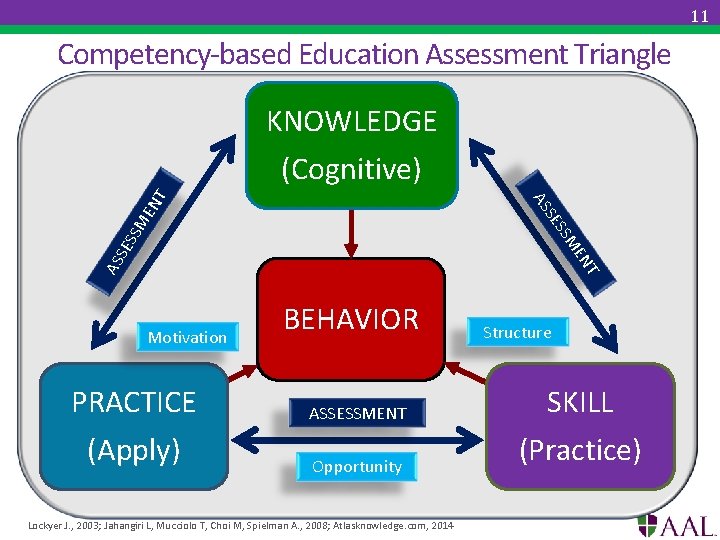
11 Competency-based Education Assessment Triangle KNOWLEDGE T AS EN SE SM S SE EN AS T (Cognitive) Motivation BEHAVIOR Structure PRACTICE ASSESSMENT SKILL (Apply) Opportunity (Practice) Lockyer J. , 2003; Jahangiri L, Mucciolo T, Choi M, Spielman A. , 2008; Atlasknowledge. com, 2014
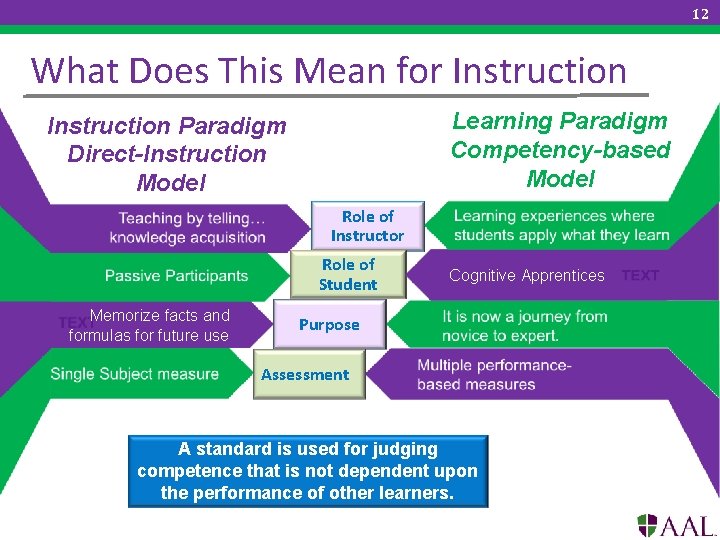
12 What Does This Mean for Instruction Learning Paradigm Competency-based Model Instruction Paradigm Direct-Instruction Model Role of Instructor Role of Student Memorize facts and formulas for future use Cognitive Apprentices Purpose Assessment A standard is used for judging competence that is not dependent upon the performance of other learners.
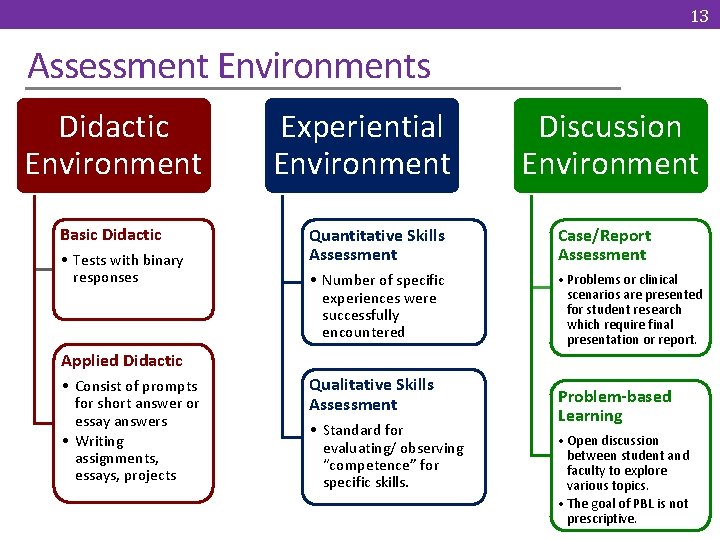
13 Assessment Environments Didactic Environment Basic Didactic • Tests with binary responses Experiential Environment Discussion Environment Quantitative Skills Assessment Case/Report Assessment • Number of specific experiences were successfully encountered • Problems or clinical scenarios are presented for student research which require final presentation or report. Applied Didactic • Consist of prompts for short answer or essay answers • Writing assignments, essays, projects Qualitative Skills Assessment • Standard for evaluating/ observing “competence” for specific skills. Problem-based Learning • Open discussion between student and faculty to explore various topics. • The goal of PBL is not prescriptive.

14 • Consider your program. How would you describe instructional design and course planning strategies? • • • Are you innovative? What is the educational culture? What barriers and challenges are you currently facing? What do you anticipate facing in the future?

15 Learning Outcome 2 Identify instructional techniques that are associated with high quality clinical teaching.

16 Teaching in Clinical Settings • Clinical learning can take place in almost all sites where patients are exposed to dental care. • Teaching in the clinical context can be unpredictable and dependent on the availability of sufficient clinical cases. • The clinical teacher plays a significant role in creating an environment that facilitates the learning of students. • The best way to achieve this is to create a positive learning environment and actively involve students in their learning.

17 Excellent Clinical Teachers: • share a passion for teaching; • are clear, organized, accessible, supportive and compassionate; • are able to establish rapport; provide direction and feedback; exhibit integrity and respect for others; • demonstrate clinical competence; • possess a broad repertoire of teaching methods; • engage in self-evaluation and reflection; • draw upon multiple forms of knowledge, target their teaching to the learners’ level of knowledge. Ramani S, Leinsteramee S. AMEE Guide 34, Medical Teacher, 2008; 30: 347– 364
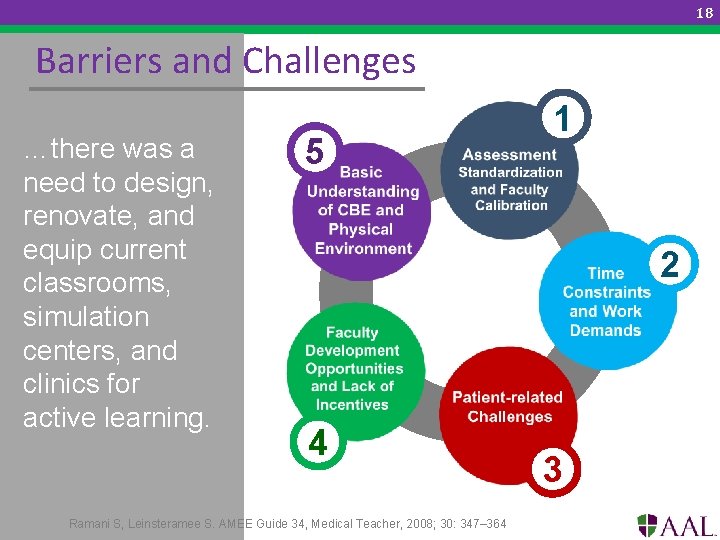
18 Barriers and Challenges …there was a need to design, renovate, and equip current classrooms, simulation centers, and clinics for active learning. 5 1 2 4 Ramani S, Leinsteramee S. AMEE Guide 34, Medical Teacher, 2008; 30: 347– 364 3
19 Consider 3 Factors RELEVANCE IMPORTANCE CONSEQUENCE OR HARM

20 Students Road to Discovery • To ask questions is to be on the road to discovery. • There are two questions to ask yourself: • 'Where am I going? ' • 'Who will go with me? ’ • If you ever get these questions in the wrong order, you are in trouble. ~ Sam Keen
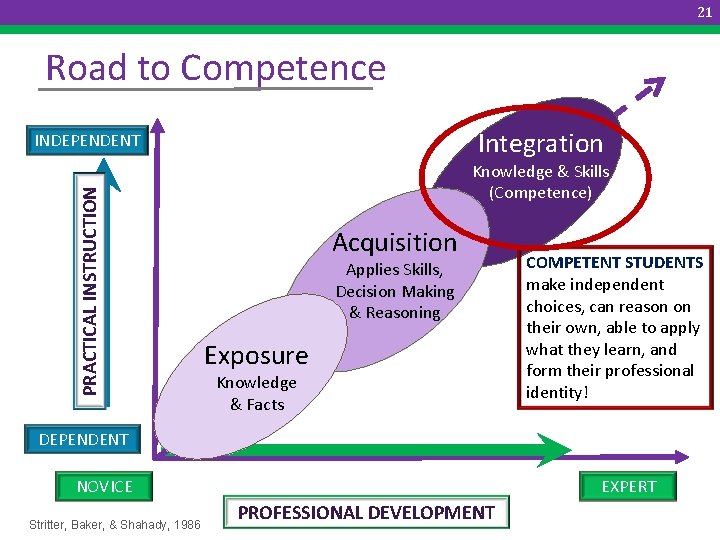
21 Road to Competence Integration INDEPENDENT PRACTICAL INSTRUCTION 2 Knowledge & Skills (Competence) Acquisition Applies Skills, Decision Making & Reasoning Exposure Knowledge & Facts COMPETENT STUDENTS make independent choices, can reason on their own, able to apply what they learn, and form their professional identity! DEPENDENT NOVICE Stritter, Baker, & Shahady, 1986 EXPERT PROFESSIONAL DEVELOPMENT

22 How Do We Move Students To Competence p, elo sed dev focu e. y to tay com bilit d s out …aate anelling cul mp arti a co re sa on tion ten her d in d ot r an ar ; vio tow ities eha cted ibil …b dire poss Answer: Outcome-Directed. Thinking! Highly effective people invest little energy on their existing problem situations, rather focus their attention and energy on their desired outcome. Fisher, 1981; Cashman, 1986; Bostrom, 1988

23 Outcome-Directed Thinking • Let’s do a short exercise… • Think of a problem that you have at work or home. For DO YOU HAVE YOUR PROBLEM? On an emotional scale of 1 -10, make the problem a 3 -5. purposes of this exercise, make the problem one that has been disconcerting, but not so overwhelming. • • Using the problem you selected above, answer the two sets of questions on the next slides either in your mind or on a sheet of paper. • Simply answer the questions and pay attention to how you feel as you answer each question.

24 Question Set 1 • Why do you have this problem? • Who caused this problem? • Who is to blame for this problem? • What are the roadblocks or obstacles to solving this problem? • How hopeful are you that this problem will be solved? • Now take a few seconds to remember what it felt like answering these questions.

25 Question Set 2 • What do you want instead of this problem? • What will you see, hear, and feel to know you have achieved this outcome? • Imagine it is sometime in the future and you have the outcome you want. What have you gained by achieving this outcome? • What resources will you have to activate or acquire to achieve this outcome? What are your first steps? • Now take a few seconds to remember what it felt like answering these questions.

26 Now that you had a moment to notice how you were feeling and thinking when answering these sets of questions. Compare your thinking process and think about how your feelings and behavior differed between question set I and II? Were you problem-directed or outcome-directed?
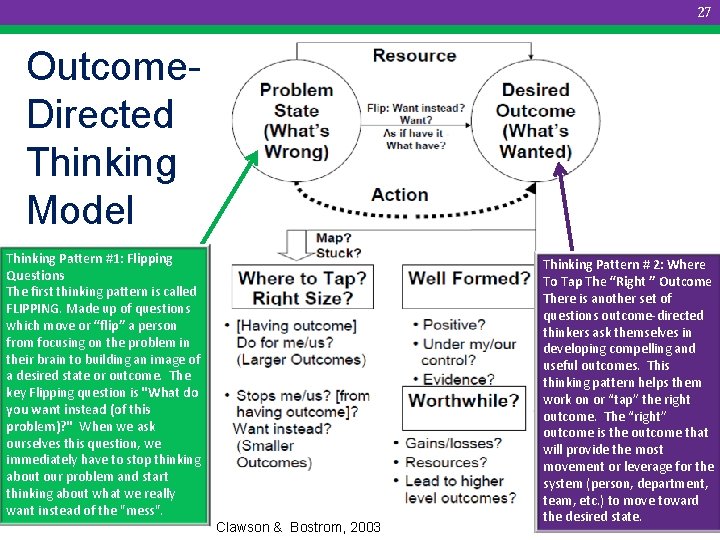
27 Outcome. Directed Thinking Model Thinking Pattern #1: Flipping Questions The first thinking pattern is called FLIPPING. Made up of questions which move or “flip” a person from focusing on the problem in their brain to building an image of a desired state or outcome. The key Flipping question is "What do you want instead (of this problem)? " When we ask ourselves this question, we immediately have to stop thinking about our problem and start thinking about what we really want instead of the "mess". Clawson & Bostrom, 2003 Thinking Pattern # 2: Where To Tap The “Right ” Outcome There is another set of questions outcome-directed thinkers ask themselves in developing compelling and useful outcomes. This thinking pattern helps them work on or “tap” the right outcome. The “right” outcome is the outcome that will provide the most movement or leverage for the system (person, department, team, etc. ) to move toward the desired state.

28 Shift from Pattern to Process of Thinking How aware you of your process of thinking? The “content” of our thinking is all the values, conclusions, ideas, beliefs, and other forms of “knowing” that you hold dear. Our curriculum and program has the content…it is how we want our students to process it that is important. Requires active learning.
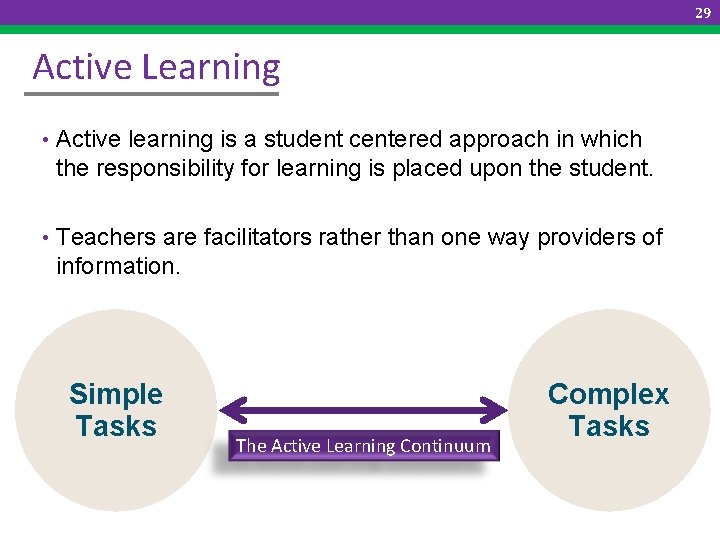
29 Active Learning • Active learning is a student centered approach in which the responsibility for learning is placed upon the student. • Teachers are facilitators rather than one way providers of information. Simple Tasks The Active Learning Continuum Complex Tasks

30 A. D. D. I. E. Active Learning Model A D D I E ANALYZE: Identify Performance Gaps and Needs DESIGN: Define Performance Outcomes; Deliver/Evaluate Strategies DEVELOP: Develop Training Materials, Lesson Plans, and Evaluation Methods IMPLEMENT: Deliver and Check for Understanding EVALUATE: Assess Effectiveness and Continuously Improve

31 Example Strategies in Clinical Settings One-Minute Microskills 1. Get a commitment 2. Probe for supporting evidence 3. Teach general rules 4. Reinforce what was done right 5. Correct mistakes Learner-Led Education 1. Summarize relevant history and physical findings 2. Narrow the differential: Likely? Relevant? 3. Analyze the differential 4. Probe the instructor 5. Plan patient management 6. Select a case-related learning issue
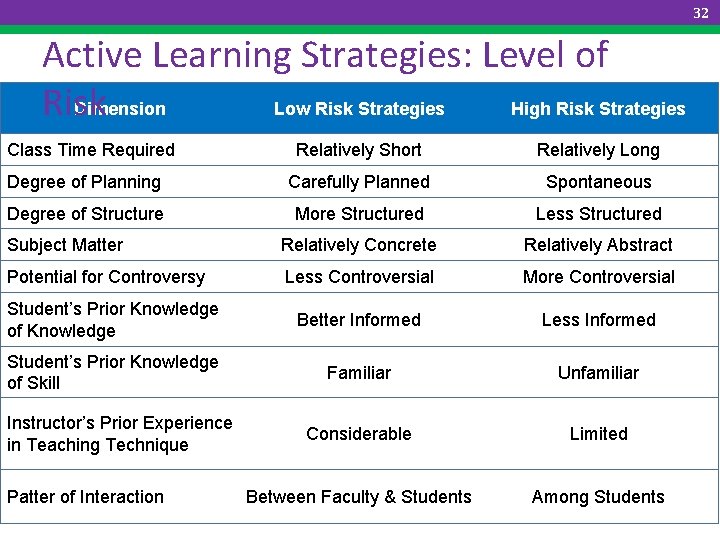
32 Active Learning Strategies: Level of Risk Dimension Low Risk Strategies High Risk Strategies Class Time Required Relatively Short Relatively Long Degree of Planning Carefully Planned Spontaneous Degree of Structure More Structured Less Structured Subject Matter Relatively Concrete Relatively Abstract Potential for Controversy Less Controversial More Controversial Student’s Prior Knowledge of Knowledge Better Informed Less Informed Student’s Prior Knowledge of Skill Familiar Unfamiliar Considerable Limited Between Faculty & Students Among Students Instructor’s Prior Experience in Teaching Technique Patter of Interaction

33 • Review the list of active learning strategies • Select a clinic (or didactic) course you teach (or plan to teach) • Consider which of these strategies would be useful in that course. Discuss at your tables

34 Learning Outcome 3

35 1 1 TAB ONE Add your own text here DO TEACHERS TEACH THE WAY THEY WERE TAUGHT? YES… It is more effective to design curriculum and clinical teaching to include multiple modes, so that there is a way for all learners of every learning style to engage with the topic. Stitt-Gohdes 2001, p. 136; Miller 2001; Stitt-Gohdes 2003; Spoon and Shell 1998; Delahoussaye 2002; Kolb, 1984, 1998

36 Learning Styles Why are we talking about learning styles in section on teaching and feedback? We spoke of patterns and process, now we need to talk about learning styles… …focusing on one’s learning style can sometimes harm learning rather than help. What is important is to focus on metalearning—being aware of and taking control of one's learning. Howard-Jones, P. A. (2014). Neuroscience and education: Myths and messages. Nature Reviews Neuroscience Nat Rev Neurosci, 15(12), 817824; Pashler, H. , Mcdaniel, M. , Rohrer, D. , & Bjork, R. (2008). Learning Styles: Concepts and Evidence. Psychological Science in the Public Interest, 9(3), 105 -119.

37 Meta-Learning Meta learning is the process by which learners become aware of and increasingly in control of habits of perception, inquiry, learning, and growth that they have internalized. Within this context, meta learning depends on the learner’s conceptions of learning, learning beliefs and processes, and academic skills. Donald B. Maudsley (1979)

38 38 Meta-Learning • A student with a high level of metalearning awareness is able to assess the effectiveness of her/his learning approach and regulate it based on the demands of the learning task. • A student with a low level of metalearning awareness will not be able to reflect on her/his learning approach or the nature of the learning task set. Donald B. Maudsley (1979)
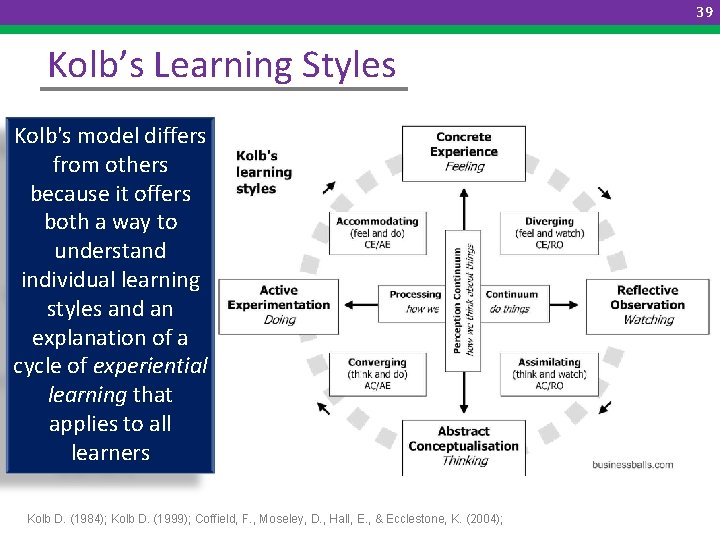
39 Kolb’s Learning Styles Kolb's model differs from others because it offers both a way to understand individual learning styles and an explanation of a cycle of experiential learning that applies to all learners Kolb D. (1984); Kolb D. (1999); Coffield, F. , Moseley, D. , Hall, E. , & Ecclestone, K. (2004);

40 Feedback Matrix POSITIVE Student usually has a good idea of what they are doing well. NEGATIVE EXPECTED FEEDBACK POSITIVE Student usually does not have a good idea of what they are doing well. This student feels they are not doing as well as they really are. Student usually has a good idea of what they are not doing well. NEGATIVE NOT EXPECTED FEEDBACK Student usually does not have a good idea of what they are not doing well. This student feels they are doing much better then they really are. The most common model used to describe the acquisition of skills is the consciouscompetence model. This model is widely used in management training but no-one is entirely clear where it originated.

41 The Acquisition of Skills Unconscious Incompetence • The subject is not aware of the skill in question Conscious Incompetence • The subject is aware of the skill and recognizes the need to acquire it Conscious Competence • The subject has acquired the skill but needs to focus their attention on its performance. Unconscious Competence • The subject has achieved mastery of the skill and can perform it without conscious thought, other tasks can be performed at the same time Ramani S, Leinsteramee S. AMEE Guide 34, Medical Teacher, 2008; 30: 347– 364

42 Faculty must identify and acknowledge these differences to include all learners in the process. In the clinical setting, it is common to have learners with different experiences and at different learning levels. Having different educational and clinical experiences/levels can provide a rich forum for discussion. SO LET’S BRAINSTORM THINK… About the BEST & WORST teacher you ever had TRAITS That made them the BEST/WORST?

43 How to Provide Feedback What is important about providing feedback? • Tangible/transparent • Owned/timely/ongoing • Balanced & specific • Actionable • Self-reflective • Written/documented • Verbal/non-verbal • User-friendly • Consistent • Formal/informal • Direct/indirect • Multiple sources

44 Challenges in Providing Feedback? What students are thinking… • Not descriptive = “good job today” • Not often/consistent • Not understood (vague) • Comes with emotion (disappointment/aggravation) • No cues for how to improve • Not conducive to the environment • Not about the activity, but something else

45 Clearly Established Criteria Students need to know what good work should look like, and have clear and specific success criteria against which they can assess their work. The test of good criteria is whether students can use them for effective self assessment. If they can’t, they need to be reworked.

46 Essential Communication Skills O. A. R. S. is a skills-based model of interactive techniques adapted from a patient-centered approach, using motivational interviewing principles. These skill-based techniques include verbal and non -verbal responses and behaviors. Both verbal and non-verbal techniques need to be adapted to be culturally sensitive and appropriate.
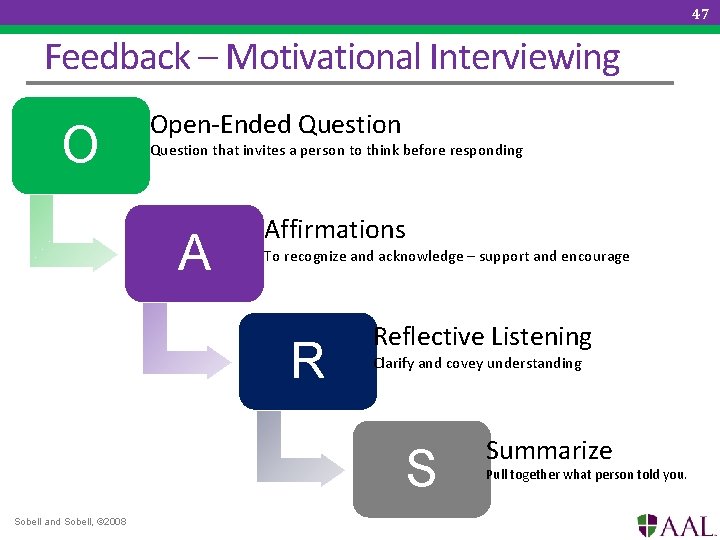
47 Feedback – Motivational Interviewing O Open-Ended Question that invites a person to think before responding A Affirmations To recognize and acknowledge – support and encourage R Reflective Listening Clarify and covey understanding S Sobell and Sobell, © 2008 Summarize Pull together what person told you.

48 Purpose of O. A. R. S 1. Provide us with a common language when teach communication skills. 2. Provide us with a “checklist” of skills as we do our on-going skills self-assessment. 3. Provide us with a format to help us be intentional when working with our patients/clients. Using skills intentionally helps us become more efficient and more effective in the work that we do.

49 Argumentative Students/Patients • When sense signs of an argument are present, stop the conversation and indicate that the intent is not to take sides but hat you are seeking understanding of his/her point of view. • Remember…argument, confrontation, lectures, and fear tactics lead to patient/student resistance. • This can be perceived as judging and typically breeds defensiveness.

50 Reframing Argument • When this happens, reframe the patient/student’s statement and offer a positive perspective on what they have already done. • During Reflective listening, turn the question back on the patient/student. • Develop Discrepancy – Develop between the patient/student’s behavior and broader goals and values. Most people are motivated to change when it comes from themselves rather than someone else.

51 Group Practice 1. Patient/Student: Focus on “something you feel two ways about” 2. Clinician: Focus on gaining a better UNDERSTANDING of the patient 3. Observer: Keep track of OARS on tracking sheet LET’S PRACTICE O. A. R. S

52 Let’s Discuss the Experience?

53 Practical strategies Teaching objectives • Do you establish teaching goals for different types of clinical encounters? • Did you communicate your teaching goals to the learners? • Did you elicit goals of the learners? Teaching methods • What teaching methods did you use and were they successful (demonstrating, observing, questioning, role-modelling)? • Do you use the same teaching strategies for all learners or do you change your methods for different learner levels and skills? Ramani S, Leinsteramee S. AMEE Guide 34, Medical Teacher, 2008; 30: 347– 364

54 Practical strategies Feedback • Did you give feedback? Did you ask for learners’ feedback on your teaching? • Planning for the next encounter • Have you used reflective critique of your teaching to change your teaching methods? Professional Development • Have you attended courses, studied educational literature or held discussions with other teachers to improve your teaching skills? • Are you planning to engage in the scholarship of teaching, study the impact of your interventions Ramani S, Leinsteramee S. AMEE Guide 34, Medical Teacher, 2008; 30: 347– 364

55 QUESTIONS
- Slides: 55