EENT Blueprint PANCE Blueprint Eye Disorders Blepharitis Blepharitis
EENT Blueprint PANCE Blueprint

Eye Disorders

Blepharitis • Blepharitis is characterized by inflammation of the eyelids • There is anterior and posterior blepharitis • Anterior is characterized by inflammation of the base of the eyelashes. Less common than posterior • Posterior is characterized by inflammation of the inner portion of the eyelid, at the level of the meibomian glands.

Blepharitis • Can cause colonization of staphylococcal organisms • Can be associated with Rosacea and Seborrheic Dermatitis • Typically patients will have red eyes, a gritty sensation, excessive tearing, eyes may burn, swollen erythematous eyelids, crusting, and photophobia. • Lid hygiene is important for treatment

Blepharitis • Warm compresses can be helpful • Topical antibiotics such azithromycin, erythromycin, or bacitracin may be helpful in reducing bacterial load of the lashes • Oral antibiotics such as tetracycline for severe cases of blepharitis
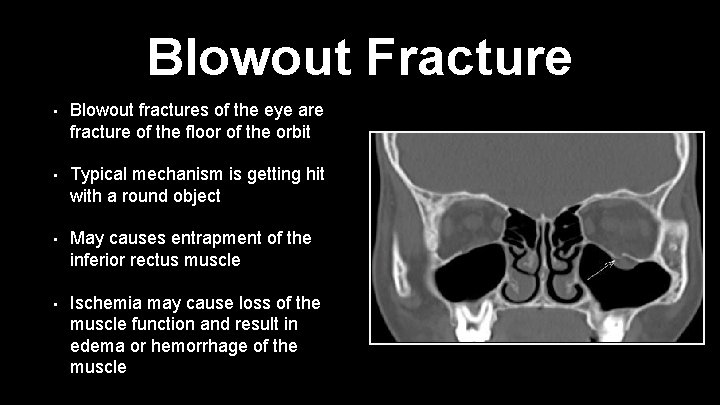
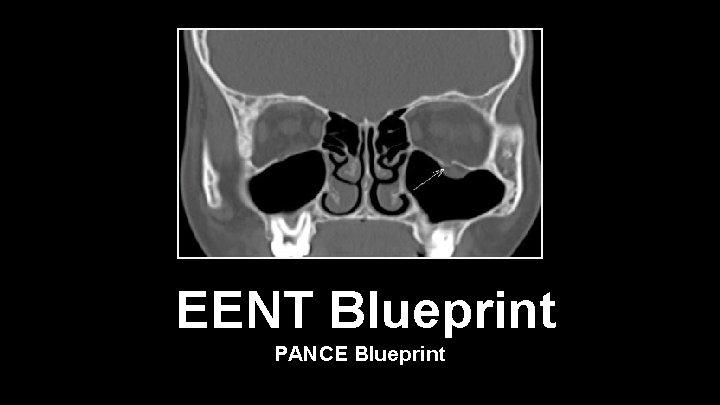
Blowout Fracture • Blowout fractures of the eye are fracture of the floor of the orbit • Typical mechanism is getting hit with a round object • May causes entrapment of the inferior rectus muscle • Ischemia may cause loss of the muscle function and result in edema or hemorrhage of the muscle
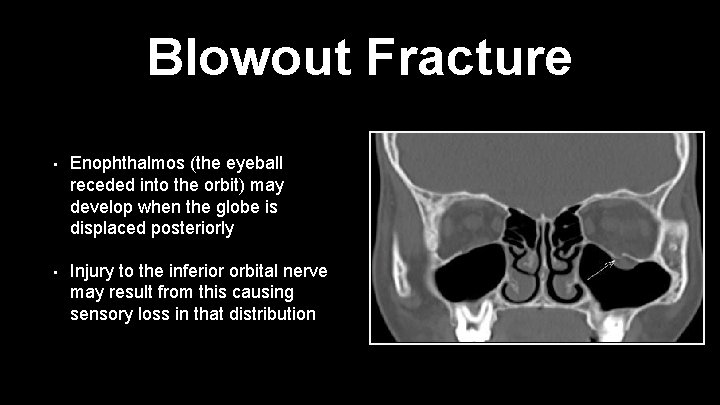
Blowout Fracture • Enophthalmos (the eyeball receded into the orbit) may develop when the globe is displaced posteriorly • Injury to the inferior orbital nerve may result from this causing sensory loss in that distribution

Cataract • Leading cause of blindness in the world • It is an opacity in the lens of the eye that can cause total or partial blindness • Embryonic development and lifelong growth of the lens produce a complex layering of cells • The lens does not shed its nonviable cells and this causes degenerative effects on its own cell structure leading some opacity problems
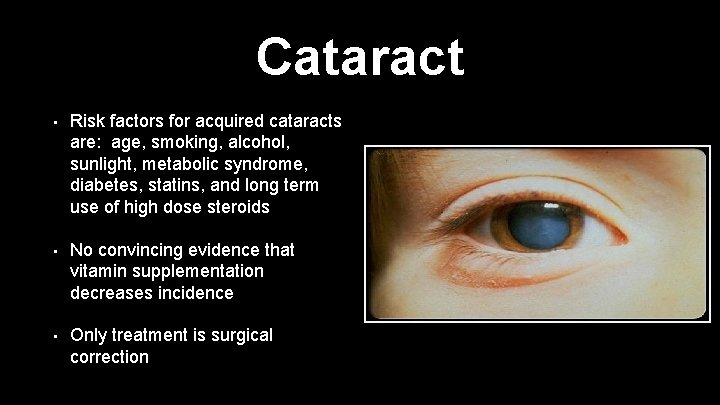
Cataract • Risk factors for acquired cataracts are: age, smoking, alcohol, sunlight, metabolic syndrome, diabetes, statins, and long term use of high dose steroids • No convincing evidence that vitamin supplementation decreases incidence • Only treatment is surgical correction
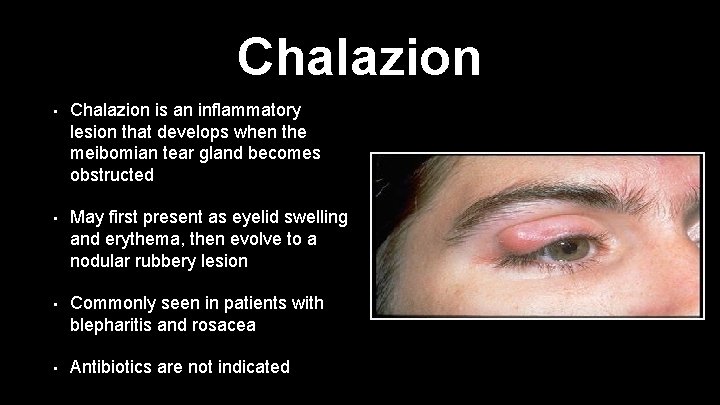
Chalazion • Chalazion is an inflammatory lesion that develops when the meibomian tear gland becomes obstructed • May first present as eyelid swelling and erythema, then evolve to a nodular rubbery lesion • Commonly seen in patients with blepharitis and rosacea • Antibiotics are not indicated
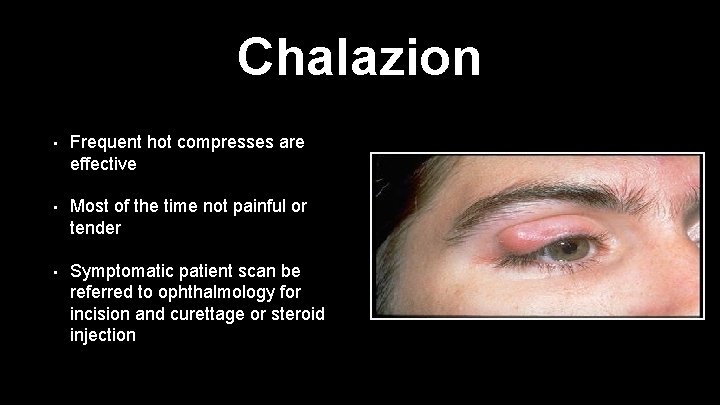
Chalazion • Frequent hot compresses are effective • Most of the time not painful or tender • Symptomatic patient scan be referred to ophthalmology for incision and curettage or steroid injection
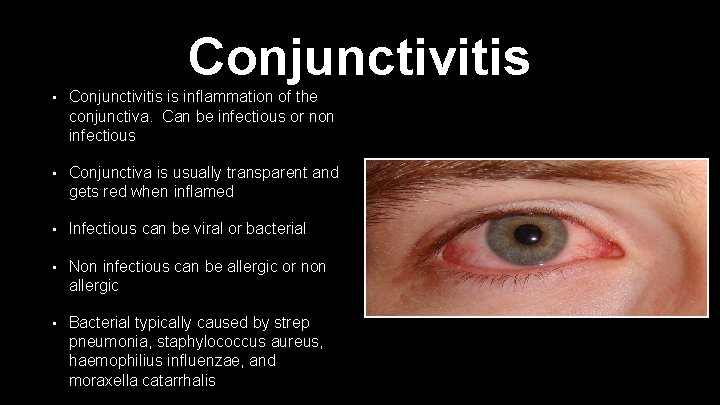
Conjunctivitis • Conjunctivitis is inflammation of the conjunctiva. Can be infectious or non infectious • Conjunctiva is usually transparent and gets red when inflamed • Infectious can be viral or bacterial • Non infectious can be allergic or non allergic • Bacterial typically caused by strep pneumonia, staphylococcus aureus, haemophilius influenzae, and moraxella catarrhalis

Conjunctivitis • Can be caused by neisseria gonorrheae and chlamydia • Viral is usually adenovirus • Allergic conjunctivitis is caused by airborne allergens contacting the eye that cause mast cell degranulation • Itching is the cardinal symptom for allergic conjunctivitis • Can be non allergic from chronic dry eye • Contact lens wearer need to throw away contacts and irrigation solution and case • Bacterial conjunctivitis include erythromycin ointment or polytrim drops.
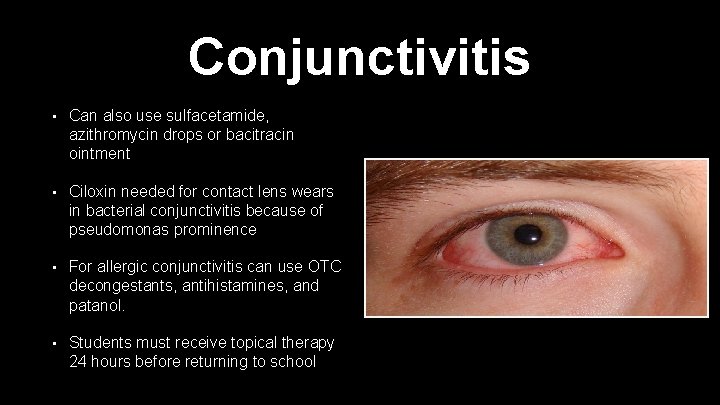
Conjunctivitis • Can also use sulfacetamide, azithromycin drops or bacitracin ointment • Ciloxin needed for contact lens wears in bacterial conjunctivitis because of pseudomonas prominence • For allergic conjunctivitis can use OTC decongestants, antihistamines, and patanol. • Students must receive topical therapy 24 hours before returning to school
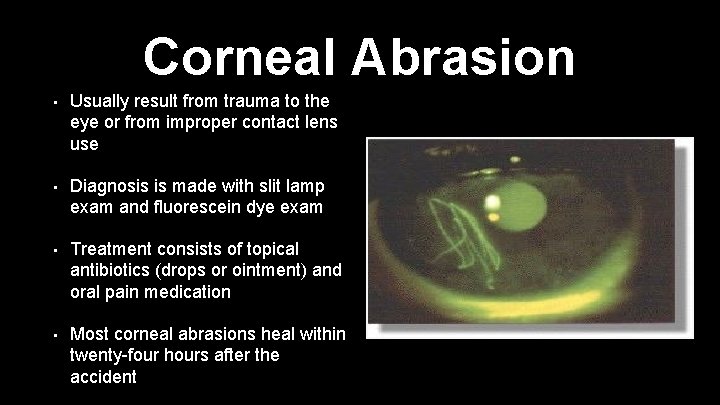
Corneal Abrasion • Usually result from trauma to the eye or from improper contact lens use • Diagnosis is made with slit lamp exam and fluorescein dye exam • Treatment consists of topical antibiotics (drops or ointment) and oral pain medication • Most corneal abrasions heal within twenty-four hours after the accident
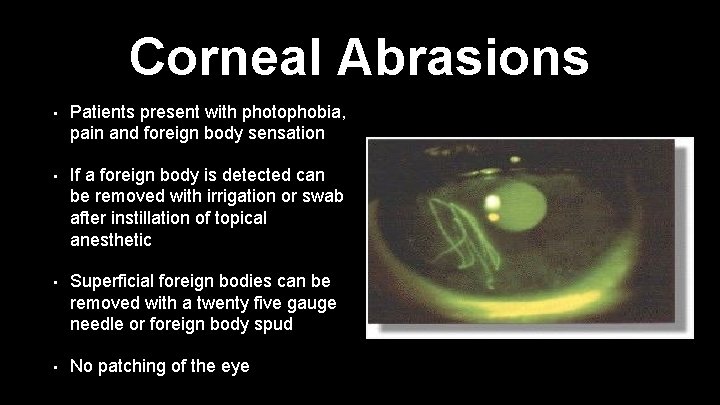
Corneal Abrasions • Patients present with photophobia, pain and foreign body sensation • If a foreign body is detected can be removed with irrigation or swab after instillation of topical anesthetic • Superficial foreign bodies can be removed with a twenty five gauge needle or foreign body spud • No patching of the eye
- Slides: 16