Educators Without Borders Teaching psychiatry in Ethiopia John

Educators Without Borders Teaching psychiatry in Ethiopia John Teshima Staff Psychiatrist Division of Youth Psychiatry

Learning Objectives At the end of this presentation, participants will be able to: • describe some of the distinctive features of mental health care in Ethiopia • debate the role that educational institutions in developed countries can play in the training of health professionals in developing countries • reflect on the challenges and rewards of teaching psychiatry in Ethiopia
Ethiopia • population 81 million • half of the population is under 18 years old • one of the world’s poorest countries – gross national income per capita is 1190 international dollars (WHO, 2008)

Prevalence of mental health problems • 12 -18. 7% for all disorders – 0. 9% for schizophrenia – 1. 8% for bipolar disorder – 10. 8% somatoform disorders – 2. 7 -3. 7% problem drinking – suicide rate 7. 8 per 100, 000 (Alem, 2001)

Mental health beliefs • most Ethiopians believe that psychiatric symptoms are due to spiritual causes • they first seek out traditional healers – typical treatments: herbal remedies, holy water, exorcisms • only when such methods fail, do families seek modern psychiatric treatment (Alem et al. , 1999), (Alem, 2001)

Mental health services • 54 outpatient clinics – staffed by psychiatric nurses • 6 inpatient wards in general hospitals – only in 4 out of 9 federal regions • one psychiatric hospital – Amanuel Hospital in Addis Ababa (Desta, 2008)

Mental health services • in 2002, there were 9 psychiatrists • all practicing in Addis Ababa • all foreign-trained

How to increase Ethiopia’s psychiatrists? • continue to send medical graduates abroad for training • establish a training program locally with Ethiopian faculty • import a curriculum and faculty from an existing training program

Problems with sending graduates abroad • they don’t come back “…there were more Malawian doctors practicing in Manchester than in the whole of Malawi. ” (Broadhead & Muula, 2002) – roughly 80% of Ethiopian medical school graduates leave to work in other countries (Araya, personal communication, 2008) • they come back with knowledge and skills that are not specific/relevant to the local context

Problems with establishing a local training program • not enough faculty to teach and supervise • challenging for a small number of faculty to create a curriculum

Problems with importing a curriculum and faculty • curriculum is usually the same as for the original institution (Harden, 2006) – thus can be insensitive or irrelevant to the local context • focus tends to be revenue generating – e. g. , Cornell University in Qatar, Duke University in Singapore (Harden, 2006) – not feasible in a poor country such as Ethiopia

TAAPP’s solution • in 2002, the Toronto Addis Ababa Psychiatry Project was created – a collaboration between the Departments of Psychiatry at U of T and Addis Ababa U • combines the numbers and strengths of U of T faculty with the local experience of Addis Ababa U faculty – U of T faculty providing their services pro bono

Format of TAAPP • teams of two psychiatrists and one resident from U of T spend 1 month each in Ethiopia • each team collaborates with the Addis Ababa faculty to develop a curriculum • 3 trips per year initially – trips focus on a specific theme, e. g. , Psychotic Disorders, Child Psychiatry

Teaching duties of TAAPP • formal seminars and workshops 3 afternoons per week • clinical supervision: – inpatient wards – outpatient clinics – emergency department

My TAAPP experience • in the summer of 2007, my wife and I agreed to go on a TAAPP trip in 2008 • after months of meetings and many hours of preparation, we left for Addis Ababa on March 8 th

Formal teaching challenges: the content

Formal teaching challenges: the content • some mental health problems have very different prevalence rates in Ethiopia – e. g. , 1. 5% for ADHD (Ashenafi et al. , 2001) • only 14 psychiatric medications are available in Ethiopia – a few typical antipsychotics, a few TCAs, lithium, valproic acid, a few benzodiazepines, fluoxetine

Formal teaching challenges: the process

Formal teaching challenges: the process • engaging the residents in interactive teaching methods was initially slow going – teaching in Ethiopia is almost exclusively didactic • limitations to the classroom environment

Clinical supervision challenges
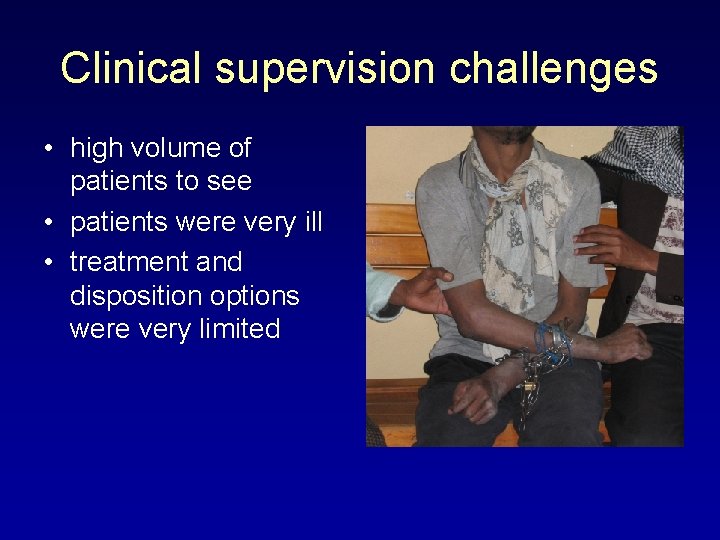
Clinical supervision challenges • high volume of patients to see • patients were very ill • treatment and disposition options were very limited

Teaching rewards • after a warm-up period, the residents did engage well in interactive teaching • the residents were very quick to implement new knowledge or feedback on their performance

Conclusions • Ethiopia desperately needs more mental health professionals • international collaboration is a feasible approach to developing training programs • teaching can cross borders, languages, and cultures

- Slides: 24