Educational Workshops 2013 Bone and Joint Infections UTI

Educational Workshops 2013 Bone and Joint Infections UTI and prosthetic joint infections Andrea Guyot Consultant Microbiologist
77 y female patient: May 2011 L TKR insertion • • 1995 right TKR 3. 5. 2011 left TKR ASA 3, BMI 33, MRSA neg comorbidities: – Leg ulcers on shins with recurrent cellulitis – Recurrent UTIs (last UTI in April 2011 on preassessment with fully sensitive E. coli) – Chronic anaemia (Hb 10, iron 7)

WHAT ARE KNOWN RISK FACTORS FOR PROSTHETIC JOINT INFECTIONS?

Facilitator Slide Risk factors for PJI (Pulido et al Clin Orth Rel Res 2008; 466: 1710, Matthews et al. BMJ 2009; 338: 1378) • • ASA>2 BMI >35 Diabetes TKA Bilateral arthroplasty Duration of procedure >90 min Haematoma and oozing >5 d

20. 11. 2011 Admission for vertigo • Diagnosis of benign paroxymal positional vertigo treated with cinnarizine • Urine: 1450 WBC (culture isolates identified by Maldi. TOF): • Klebsiella – res amoxicilin only plus Enterobacter aerogenes – res: Augmentin, cefalexin – sens: cipro, trimethroprim, gentamicin, meropenem, cefpodoxime • Blood: iron deficiency anaemia with iron 3 umol/l and transferrin 2. 26 g/l Platelets 320, WBC 9. 9, Hb 8. 9, CRP 49

Home discharge • Discharge home on trimethroprim (to be taken until 26. 11. 2011) • On 13. 12. 2011 readmission for swollen hot L TKR • WBC 10, CRP 203, ESR 21, Hb 7. 5, platelets 23 • MSU: 94 WBC; Enterobacter aerogenes – res: Augmentin, cefalexin – sens: cipro, gent, cefpodoxime, trimethroprim
13. 12. 2011 • Synovial fluid 3720 WBC, 73% PMN • Citrobacter koseri (identified by Maldi. TOF) – res: Augmentin, cefuroxime – sens: cipro, gent , cefpodoxime

WHAT ARE THE SENSITIVITIES OF INVESTIGATIONS ON SYNOVIAL FLUID?
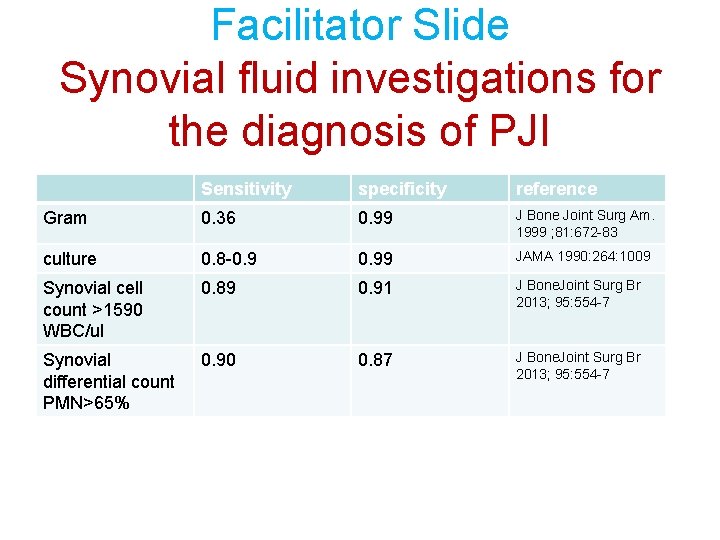
Facilitator Slide Synovial fluid investigations for the diagnosis of PJI Sensitivity specificity reference Gram 0. 36 0. 99 J Bone Joint Surg Am. 1999 ; 81: 672 -83 culture 0. 8 -0. 99 JAMA 1990: 264: 1009 Synovial cell count >1590 WBC/ul 0. 89 0. 91 J Bone. Joint Surg Br 2013; 95: 554 -7 Synovial differential count PMN>65% 0. 90 0. 87 J Bone. Joint Surg Br 2013; 95: 554 -7

Risk of UTI for PJI Maderazo E et al. Late infections of total joint prosthesis. Clin. Orthop Relat Res 1988; 229: 131 -142 Incidence of PJI=1% Risk for haematogenous seeding 1: 5= 0. 2% Risk for seeding from UTI = 13% of 0. 2%=0. 026%= 26: 100000 = approximately 1: 4000 arthroplasties get infected by haematogenous seeding from UTI
15. 12. 2011 1 st stage of revision • Removal of TKR and implantation of Vancogenx spacer with Palacos R&G (gentamicin) cement on prophylactic dose of teicoplanin 600 mg and 120 mg gentamicin • Meropenem 1 g tds started postop • 5 periprosthetic tissues grow Citrobacter kosei – sens: meropenem, gentamicin, ciprofloxacin

HOW MANY PERIPROSTHETIC TISSUES ARE REQUIRED FOR DIAGNOSIS OF PJI AND WHAT IS THE PERFORMANCE?

Facilitator Slide

WHICH ANTIBIOTIC WOULD YOU CHOOSE FOR CITROBACTER?

Facilitator Slide Antimicrobial therapy for Citrobacter

16. 12. 2011 post-op • Platelets 13, Hb 5. 6, prothrombin time 15 sec, PT ratio 1. 3 • Haematological diagnosis: – Thrombotic thrombocytopenic purpura • Transferred to a specialist hospital for Rituximab and plasma exchange • The features in the blood tests just prior to Christmas 2011 are absolutely classic with clear evidence of haemolysis, a grossly raised LDH of 1545 iu/L and no discernible ADAMS TS 13 evident in her peripheral bloods. The low platelet count was because of the inability of the enzyme ADAMS TS 13 to cut von Willebrand’s factor off her endothelial cells and therefore platelets were deposited in the vessel as a consequence. The most important thing in a patient like this is that you do not receive a platelet transfusion, which has been associated with fatal thrombotic stroke. • Fortunately she was transferred to the specialist hospital for plasmaphoresis with FFP, which acts as a source of the missing enzyme ADAMS TS 13 and also Rituximab therapy to destroy the B lymphocytes which produce the antibody in the first place.

25. 1. 2012 • Return from specialist hospital on meropenem 1 g tds: • MRSA in nose, not in groin • Mupirocin and chlorhexidine washes prescribed • CRP 7. 8, WBC 8, HB 10. 5, platelets 300 • going home on 26. 1. on oral ciprofloxacin 750 mg bd until 10. 3. 2012

HOW LONG SHOULD ANTIBIOTICS BE GIVEN BETWEEN 2 STAGES OF REVISION?

Facilitator Slide

26. 4. 2012 • Preassessment: MRSA neg, • CRP 4, ESR 6, WBC 3. 4, platelets 240, Hb 12. 4 • MSU 64 WBC, no growth
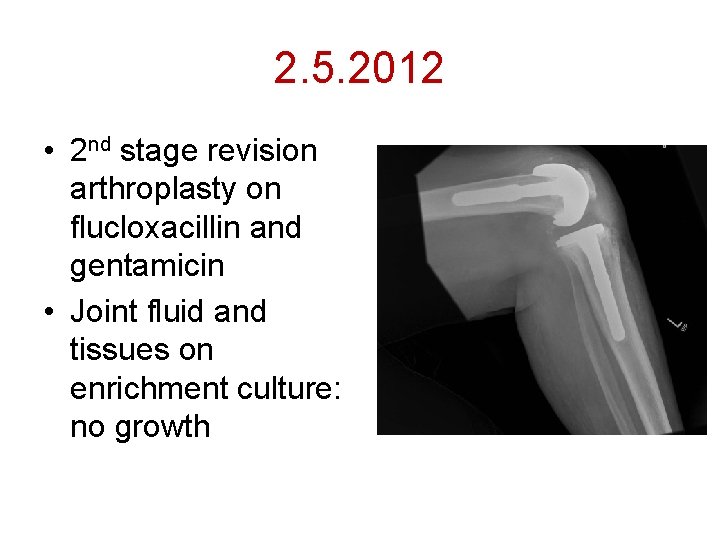
2. 5. 2012 • 2 nd stage revision arthroplasty on flucloxacillin and gentamicin • Joint fluid and tissues on enrichment culture: no growth
Follow up • Discharge home 21. 5. 2012 • ESR 21, CRP 5. 4, WBC 3. 4, platelets 208 • Platelets 360, Hb 10. 9 • • Follow up on 12. 3. 2013 (at 10 months after 2 nd stage) No sinus formation CRP <4, ESR 16, WBC 5. 7, Hb 11. 9 Oxford score 22 (max=50, good revision outcome >30) with pain score 1 (=mild) • ROM 120 C with lateral ligament laxity • Xray: no loosening
- Slides: 22