Educational Workshops 2013 Bone and Joint Infections Osteomyelitis

Educational Workshops 2013 Bone and Joint Infections Osteomyelitis Martin Dedicoat Itisha Gupta Heart of England NHS Foundation Trust

22 year old female self referred to ED June 2012 � Recurrent abscess over her back. � History since a depot contraceptive injection in February over the left buttock. � Done at a Sexual Health clinic. � Developed pain a day after injection � Increasing pain for 4/12 ---

Past history � Known IDDM since 2006 � Been under investigation for PR bleed under Gastroenterologists in 2011 � In May 2012 diagnosed as ? Crohn’s proctitis. � Started on Mesalazine � A nurse by profession

What additional information you would like to know in history?

Antibiotic history � Flucloxacillin 500 mgqds in May for 1 week � Co-amoxiclav � No response for 5 d about 2 weeks back

Examination � History of fever, however apyrexial on admission. Examination � Soft tender left sided swelling lateral to the spine over renal area � No spinal tenderness Referred back to GP as scan booked
Investigation � WCC 12 and CRP 27 � US scan booked by GPnormal abdomen. A swelling on left renal area with subcutaneous collection with no vascular flow ? Haematoma ? seroma � GP referred back to hospital

What would you suggest be the next steps?

Surgical drainages 1) Drainage of 8 x 4 cm collection discharged on Co-amox for 7 days Sample- Microbiology No growth 2) Re-presented 4 d later with warm tender fluctuant swelling- re-accumulation 100 mls of haemo-purulent fluid drained

Surgical drainages continued Returned 2 days later � ↑ in pain and size � No fever � 6 x 4 cm hard swelling, warm, no erythema What further action?
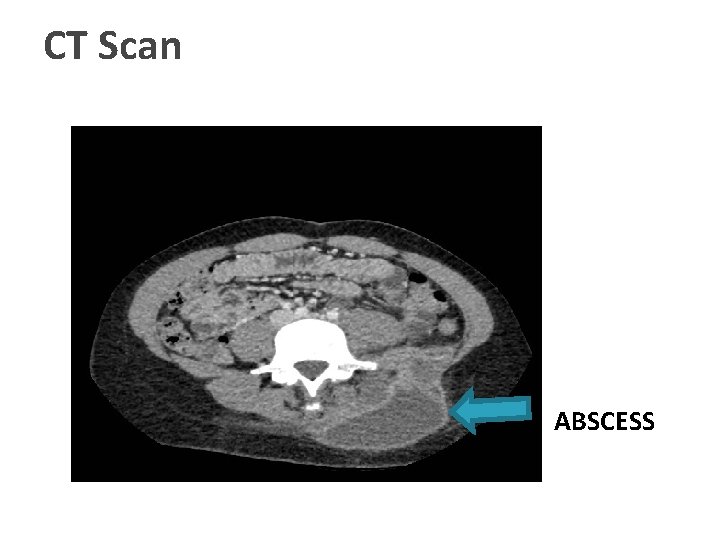
CT Scan ABSCESS

CT report � Paraspinal fluid collection with bony destruction of left iliac bone and small involucrum � An abscess in iliacus muscle � Small collections between iliacus and psoas muscle

What further management?

3) Surgical Drainage after CT report � I&D drainage under GA 20 ml of loculated cavity and erosion of iliac bone � Started � Pus on high dose of IV fluclox 2 gqds sent for culture- No growth

� What � Any management to consider now? further history?

More History � Born and brought-up in UK � Grandparents from Jamaica � Lives with mum and dad � No known history of TB � BCG vaccinated

Antibiotics � Fluclox high dose ↓ 3 days � Rifampicin 450 mg BD added to fluclox ↓ 7 days � Both changed to Ceftriaxone 2 g. OD ↓ 3 days Sent Home on IV therapy – Ceftriaxone for total 6 weeks
�Is that the whole story?
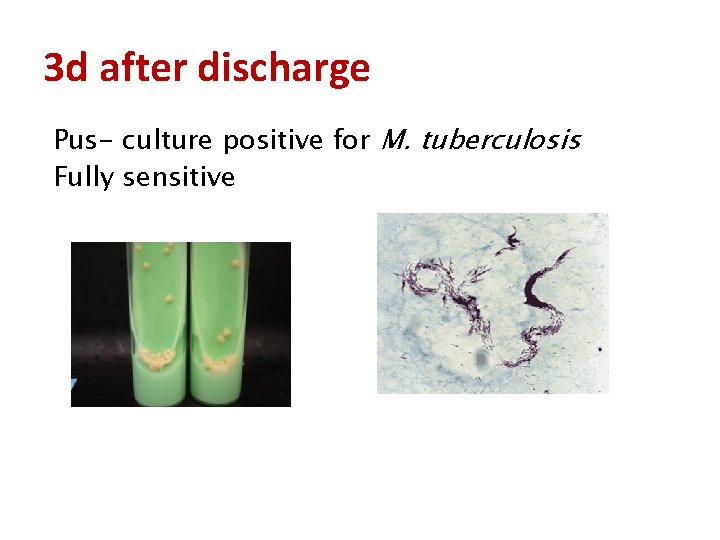
3 d after discharge Pus- culture positive for M. tuberculosis Fully sensitive

Treatment considerations

Treatment of Bone and Joint TB � Extrapulmonary foci usually respond to treatment rapidly than cavitary pulmonary TB � Drug sensitive TB 4 drug regimens ( INH, RMP, PZA and EMB) for 2 months followed by INH and RMP for 69 months � Surgery can be needed for diagnosis

ATT Started on Rifater plus Ethambutol Rifampicin and INH 2 months continuation phase 9 months Recent MRI much improved Treatment stopped in July 2013

� Risk assessment for adherence to treatment � Surgical therapy not recommended unless chemotherapy has failed and serious joint instability � Consider alternative non-hormonal methods of contraception throughout treatment and 1 month subsequently

Been in Bay �What actions to take? �What additional investigations needed?

Been in Bay � IPC precautions and actions List of all patients in the bay Inform District nurses for Vac dressing To wear masks at time of wound care and dressings � HIV negative
CXR normal

Infectiousness of patients with TB correlates with number of organisms expelled 1) Presence of cough 2) Cavitation on CXR 3) Positive AFB in smear 4) Respiratory tract disease with involvement of lung, pleura and larynx 5) Cough inducing procedures or aerosol generating procedures

Extrapulmonary TB ? Infectious 1) 2) 3) If have concomitant pulmonary TB, laryngeal TB Open abscess and drainage Aerosolisation of drainage fluid Globally extra-pulmonary without pulmonary involvement comprises of 14% of notified cases

Case – Extended typing of Mtb available � SIRU and MIRU typing shows identical 24 loci match to another nurse in the workplace with smear positive pulmonary TB few years back. � Patient was not contact screened at the time of the incident.

Slides for information � Further slides are for information only

Active case finding Human to human transmission prevention Screening * Household contacts irrespective of site of infection * For sputum smear-positive other close contacts should be assesses e. g. frequent visitors and workplace * Casual contacts should not normally be assessed

Contact tracing and IPC implication of active TB NICE Guidelines 2011 Diagnosis Offer Mantoux test to diagnose latent TB ( LTB) � Household contacts � Non household close contacts- e. g. Workplace Consider IFN-gamma if Mantoux is positive or if it is unreliable i. e. Previous BCG vaccination � Assessment for presence of active TB

For HCWs � Mantoux to new NHS employees who will be in contact are not new entrants not had BCG vaccination � Offer IFN gamma recent arrival from high incidence countries

Management of latent TB About 5 -10% of LTBI will develop active disease Considered if active TB excluded by CXR and examination � 35 years or younger � Any age with HIV � Any age and HCW and are either →Mantoux positive and without BCG vaccination →Strong Mantoux positive (>15 mm), IFN-γ pos and prior BCG
- Slides: 34