Educational Workshops 2013 Bone and Joint Infections An

Educational Workshops 2013 Bone and Joint Infections An oozy wound Dr Savita Gossain Heart of England NHS Foundation Trust

Case History • 77 Y F with background of Type II diabetes; Hypertension; Previous SVT & Osteoporosis • March 2008: Fractured Left NOF, Dynamic hip screw • Oct 2009: Pain in Left hip; at rest & on walking • Nov 2009: DHS revised to gamma nail, satisfactory recovery • 12 Dec 2009: Left total hip replacement following failed gamma nail; post-operative anaemia, otherwise uneventful recovery. [ASA 2/3, BMI ~ 35 ]

Day 15 post-op THR • 27 Dec 2009: Readmission – Pain & erythema hip wound – Wound oozing serous fluid – Systemically well – WCC 7. 5; CRP 16 – X-ray hip : NAD

WHAT WOULD YOU ADVISE?

• 1 Jan 2010: Discharged home 4/7 later on oral Flucloxacillin 7 days (No micro/ID consult) • 4 Jan 2010: T&O clinic review (D 23 post-op) – Wound erythematous & indurated with mucky discharge – Temp 380 C but otherwise well – CRP 91

WHAT WOULD YOU ADVISE NOW?

• Commenced on IV Benzylpenicillin +Flucloxacillin • 5 Jan 2010 (Day 24): Open washout – 30 -40 ml purulent fluid oozed from joint – Samples sent for micro (fluid & tissue) – Wound packed – layers not closed as plan to take back to theatre in 48 hrs

7 Jan 2010 (Day 26) • E. coli grown from fluid samples x 2 • Tissue not received (!) • Changed to iv ciprofloxacin + stat gentamicin in theatre (Microbiology advice) Back to theatre “most tissues appeared healthy & viable. Three tissue samples taken (superficial, deep & capsule). Further debridement to healthy tissue. Washout of hip joint, 6 litres saline with pulsed lavage”

• 9 Jan 2010: All tissue samples from 7/1/10 grew E. coli as previously, ciprofloxacin continued. • E. coli = fully sensitive (Ampicillin, Gentamicin, Ciprofloxacin, Cefuroxime, Meropenem. . )

What would you advise for further management ?

Antibiotic treatment • Picc line inserted 11/1/10 & Ceftriaxone 2 g od commenced by ID Consultant. Plan for 4 -6/52 iv to be continued as OPAT and then prolonged oral course of antibiotics (Ciprofloxacin) to eradicate the infection.
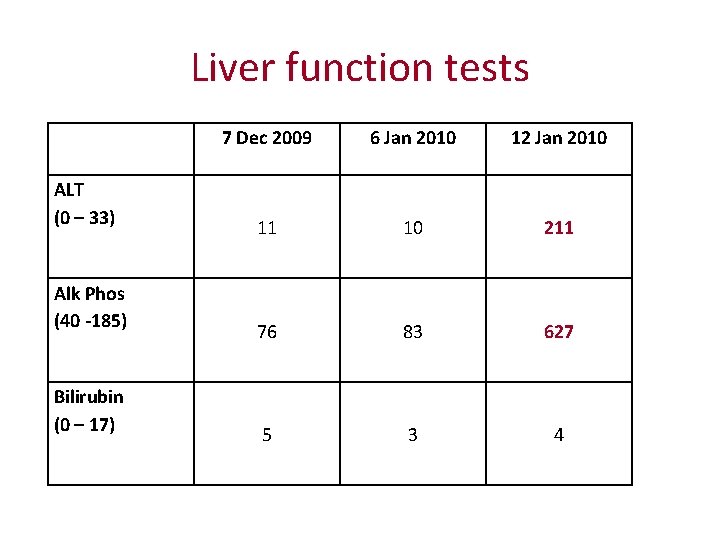
Liver function tests ALT (0 – 33) Alk Phos (40 -185) Bilirubin (0 – 17) 7 Dec 2009 6 Jan 2010 12 Jan 2010 11 10 211 76 83 627 5 3 4

Cause of deranged LFTs? What would you advise?

• It was thought that rise may be related to ciprofloxacin as raised 12 hours after switch to ceftriaxone. • However liver SEs much more common with ceftriaxone so planned to closely watch LFTs over next few days. .
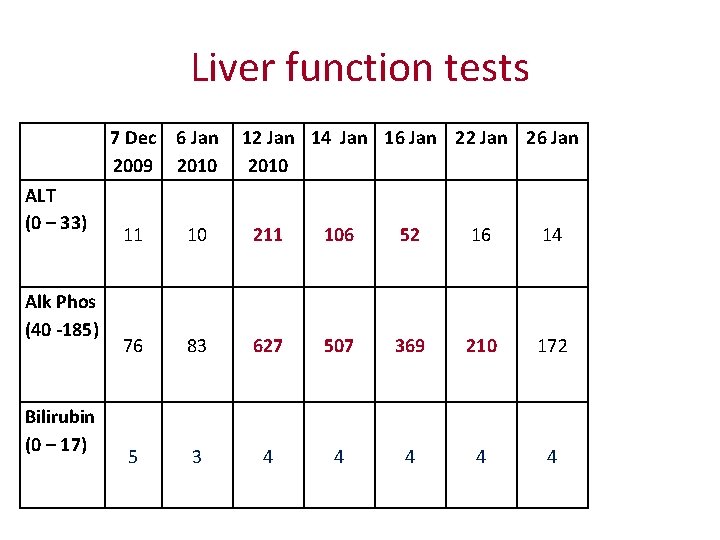
Liver function tests ALT (0 – 33) Alk Phos (40 -185) Bilirubin (0 – 17) 7 Dec 2009 6 Jan 2010 12 Jan 14 Jan 16 Jan 22 Jan 26 Jan 2010 11 10 211 106 52 16 14 76 83 627 507 369 210 172 5 3 4 4 4

Further progress • Following debridement & washout – wound oozing serous fluid for few days. Clips were removed 20/1/10 (Day 13 post debridement) • 22/1/10: temperature spike and ? rigors. Septic screen and paired BC advised & to remove line if further spike temperature. Wound ooze settling.

• • • Cultures: W/S mixed skin flora MSU : 13 WBC, 15 RBC, culture not indicated BC x 2: Negative CRP 15 • However, continuing ooze from wound (serous)and few spikes of temperature over next few days (still on ceftriaxone)

WHAT WOULD YOU ADVISE?

ID consult • Wound not settled post debridement although inflammatory markers down • Wound not cellulitic. Continued ooze suggests sinus tract • Consider USS to see if superficial collection • If joint secure – further w/o & debridement, excision sinus tract & and replacement of any exchangeable components • If joint loose – 2 stage revision • Alternative of long term suppression with antibiotics less useful with E. coli as more resistant strains may emerge during treatment

• USS on 4/2/10 (D 28 post debridement): No collection, no effusion in joint. • Temperature settling, mobilising, pain better • T & O consultant: “as improving and CRP coming down and no collection on USS, does not want to do 2 stage revision at this time” • Wound continued to ooze : no cellulitis, small discharging sinus middle wound

WHAT ARE THE OPTIONS?

19/2/10 Completed 6/52 IV Ceftriaxone ? Unsuccessful attempt at cure by DAIR Discharging chronic sinus No plan for revision Discharged home on po Amoxycillin 500 mg qds & review in 1 month whether to continue • If deterioration hip function , may require revision • Discharged home 1/3/10 (D 53 post debridement) • • •

• April 2010: Clinic Review – Systemically well – No cellulitis over wound – Sinus over the wound healed – Normal WCC & CRP 10 – Continued Amoxicillin 500 mg tds, suppressive treatment – Patient made aware of CDI risk, chronicity of infection.

• July 2011 & July 2012: – No problems with the hip. – Xray hip: NAD – Wound healed. – Continuing suppressive Amoxycillin

SUMMARY • Case of early infection THR (<30 d post surgery) • Delayed wound healing/ ooze may represent early infection +/- systemic symptoms • Managed as DAIR initially – IDSA guidelines (A-II recommendation for early infection, well fixed prosthesis) • ? Failed DAIR – sinus developed , but no further surgery planned • Suppressive antibiotics continuing
- Slides: 25