Educating Pediatric and Family Medicine residents about Transition

Educating Pediatric and Family Medicine residents about Transition to adult subspecialty care for Congenital Heart Disease

Consent Within this training module you will review slides and videos about transition of pediatric cardiac patients. If you consent to complete this module you will be required to answer pre- and post-test questions to assess your knowledge. • By checking the YES box you consent to participating in this training module and answering all the pre- and post-test questions Yes No

• • Name: Gender: Residency Program: Type of Residency (Peds / IM or FP): Year graduated Medical School: Medical School E-mail address:

• The focus of this module is Congenital Heart Disease (CHD) • The principles discussed can be applied to all healthy pediatric patients and those with other chronic conditions or special health care needs.

Objectives • By the completion of this module, residents should have a clear understanding of: • The importance of transition of cardiac patients • The importance of life-long cardiac care • How to encourage patient-centered care • How to develop strategies to incorporate transitional care into practice

What is transition? • Transition is the purposeful planned process that supports adolescents and young adults with chronic health conditions and allows them to move from a pediatric practice to an adult-oriented health -care practice, providers, and facilities • To be successful, the process attends to the medical, psychosocial, educational and vocational needs

Transition ≠ Transfer • Transition is not synonymous with the transfer of medical care • Transition refers to a gradual shift in the responsibility of health care management from the family to the patient • Transfer of care refers to the movement of patient care to adult centered providers

12 minute video • Intro • 0 to 29 seconds

Transition • The goal of transition is to “provide uninterrupted health care that is patientcentered, age and developmentally appropriate, flexible, and comprehensive. ” • Although this module is focused on CHD, the principles are applicable to all patients with special health care needs
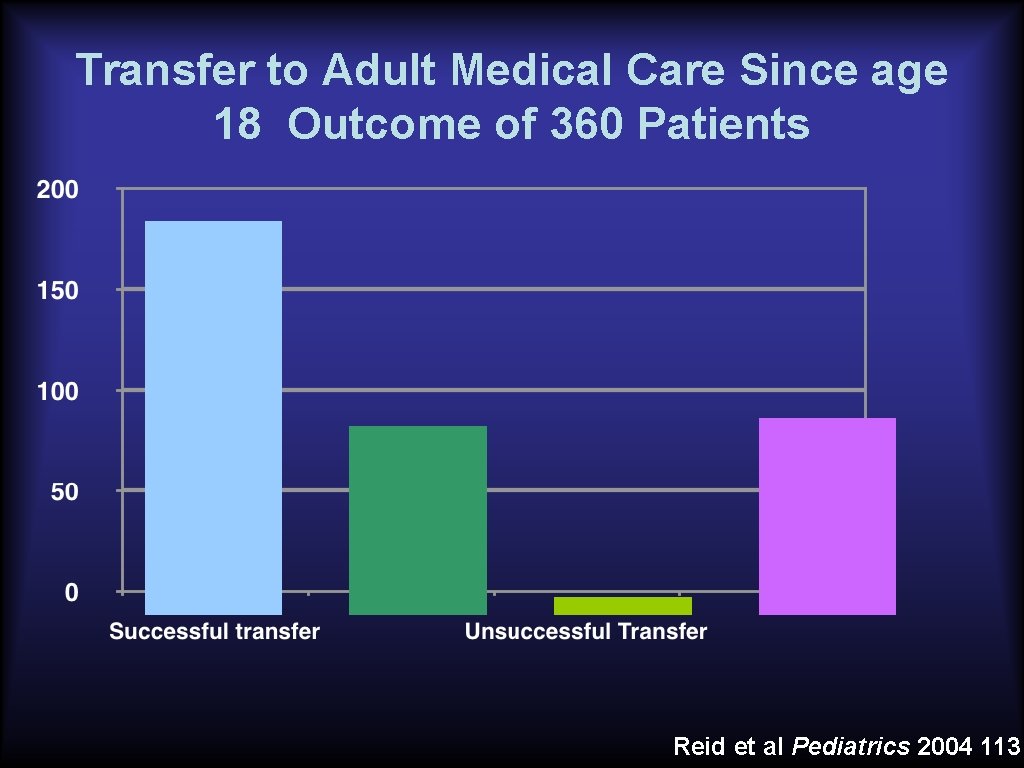
Transfer to Adult Medical Care Since age 18 Outcome of 360 Patients Reid et al Pediatrics 2004 113

Children with Special Health Care Needs • 50% of adolescents recalled provider who discussed how needs might change in adulthood • 30% had plans for changing health care needs • 21% had plan for transferring to adult care National CSHCN Survey 2000 -2001

Barriers to Transition

Barriers to Transition • There are many obstacles to the process of transition: • • • Patient Family Pediatric cardiology Adult Congenital Heart Disease (ACHD) providers

Barriers to Transition: Patients • Transfer experienced as rejection • May remain under parent’s insurance • Overwhelmed by new responsibilities: self-care, medical decision making, self-advocacy • Need to unlearn successful pediatric adaptive strategies and learn new “adult system” behaviors • Confronted with “realities” of morbidity and death • Timing of transfer coincides with other stresses • Regionalization of ACHD care and travel

Barriers to Transition: Parents • • Ensured children were compliant Concerned that adolescent is less vigilant Required to provide informed consent Parents become attached to pediatric providers • Parents feel alienated • 30% parents resisted children being seen alone but this decreased to 15% following education

Barriers to Transition: Pediatric cardiologists • May be reluctant to transition and transfer patients to ACHD care because of close relationship • May lack confidence in adult providers • Requires a shift in professional attitude to begin treating adolescents like young adults • Must unlearn behaviors and promote “closure”

Barriers to Transition: Adult Providers • Because of inadequate number of ACHD clinics, difficult to establish ACHD cardiac care • Many internists report inadequate training in the care of adults with childhood onset conditions • Adult care providers may be less prepared to meet ongoing transitional educational needs

Barriers to Transition: Insurance • Transition to adult care occurs at the time many young adults lose or change medical insurance • Insurance may be declined or offered at high premiums and may prevent continued care • Insured patients may be referred to a general cardiologist instead of out-ofnetwork ACHD cardiologist

Why Transition Congenital Heart Disease Patients?

AAP/ AAFP and ACP Guidelines • Transition “to maximize lifelong functioning and potential through the provision of high-quality, developmentally appropriate health care services that continue uninterrupted as the individual moves from adolescence to adulthood”
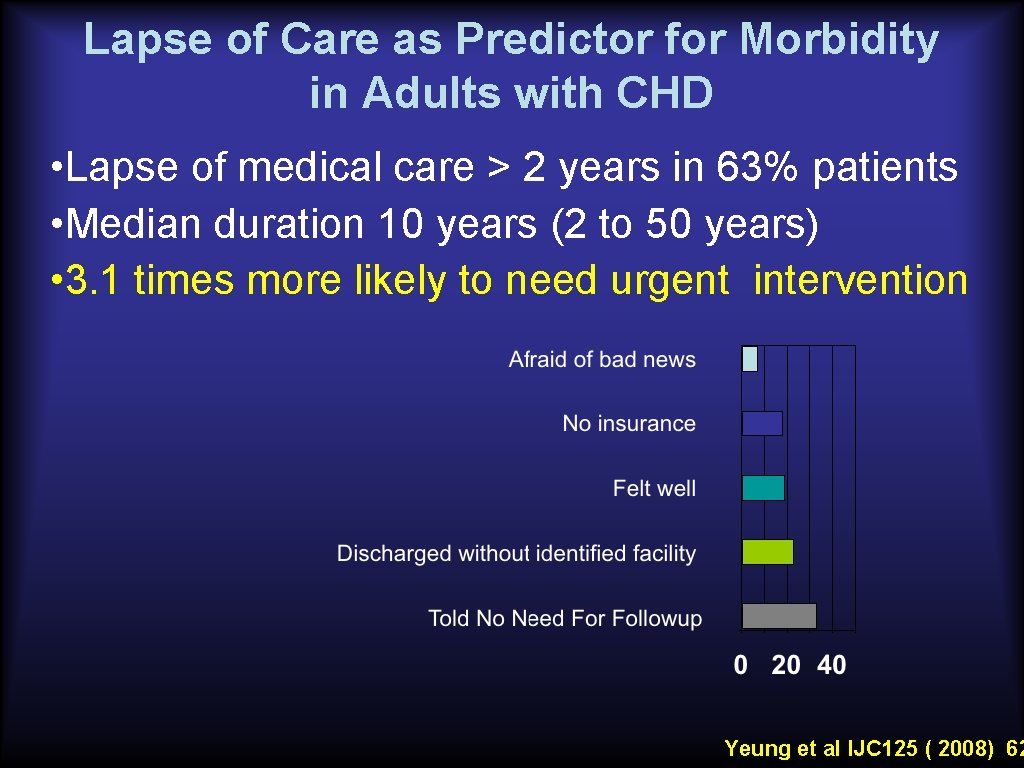
Lapse of Care as Predictor for Morbidity in Adults with CHD • Lapse of medical care > 2 years in 63% patients • Median duration 10 years (2 to 50 years) • 3. 1 times more likely to need urgent intervention Yeung et al IJC 125 ( 2008) 62

Inadequate transition • Inadequate transition leads to: • • Poor understanding of health status Loss of follow up Delayed care Potential serious consequences Late presentation to ER Emotional stress Financial stress

Why is transition important in CHD? • Young patients with CHD should: • • Take greater responsibility for their health care Become comfortable making medical decisions Optimize health through consistent medical care At a minimum, young patients with moderate or great complexity defects must be informed of the need for regular long term cardiac care

Goals for Optimizing Transition • Educate about medical condition • Establish comfort in communication • Encourage decision making • Provide uninterrupted health care • Optimize quality of life

Video • Make stronger • 30 seconds to 1. 02

When to Transition Congenital Heart Disease Patients?
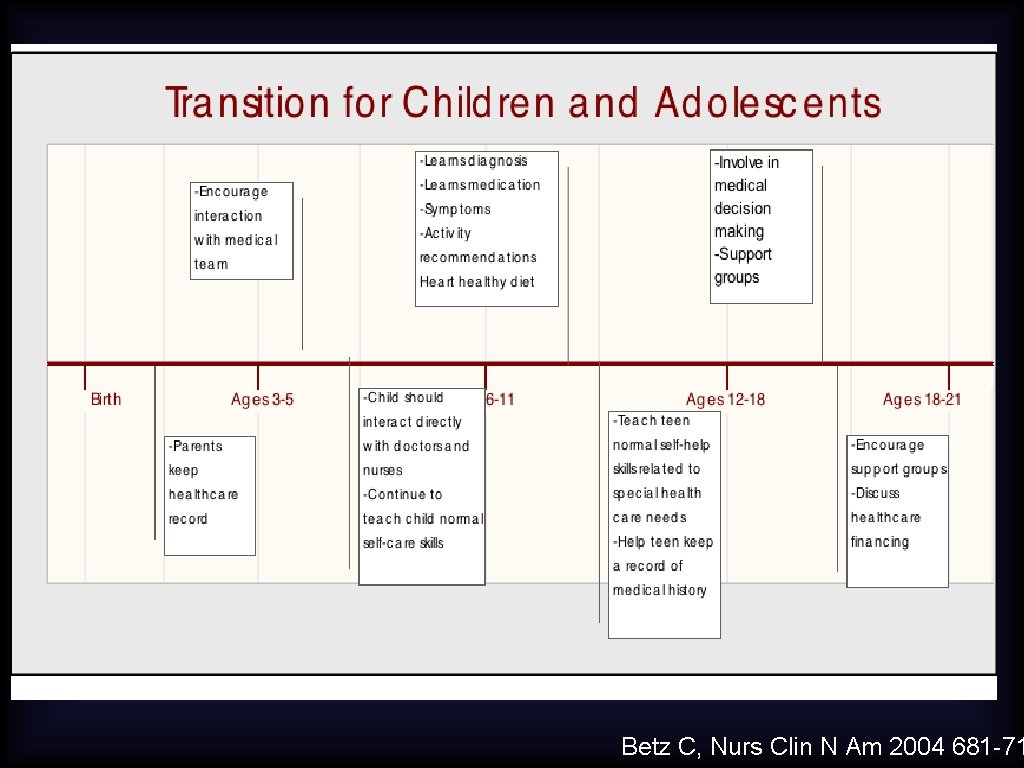
Betz C, Nurs Clin N Am 2004 681 -71

AAP Consensus Statement 2002 • Create a written health care transition plan by age 14 with young person and family. This plan should be reviewed and updated annually and before transfer of care.

How to Transition Congenital Heart Disease Patients Patient Considerations

Patient Challenges • Overwhelmed by new responsibilities: selfcare, medical decision making, self-advocacy • Confronted with “realities” of increasing morbidity • Need to unlearn pediatric adaptive behaviors • Need to learn new “adult system” behaviors • Our goal is to: • increase self-responsibility • provide support

Goal: Increase Self-Responsibility • • In coordination with general development Engage the patient Patients seen alone for part of clinic after 12 yrs Provide opportunities for control and decisions Encourage self care Modify to individual needs Involve family as desired by patient

Goal: Provide Support • • Planned and sensitive within constraints Patients in control within limits Dealing with self image Gradual process that begins at 12 years until adulthood and after care is transferred to ACHD team • Family are as involved as the patient wants

How to Transition Congenital Heart Disease Patients Provider Considerations

Specific CHD Issues • Anatomy • Previous surgeries • Hemodynamics • Arrhythmias • Medications • Endocarditis • Anticipated surgeries • Education/career plan • Contraception/pregna ncy • Genetics • Non cardiac surgery • Lifestyle issues • Communication skills • Self care “Repaired” does not mean fixed

How to transition • An ongoing process • 3 - 5 years: encourage discussion about activity level and symptoms • 7 -10 years: diagnosis, medication, exercise limitation, SBE discussed directly with patient • Teenagers: heart healthy behaviors, smoking, alcohol , illicit drugs, birth control, pregnancy risks, relevant genetic aspects

How to transition • Provide patients with accurate knowledge regarding their cardiac defects and treatment • Promote the concept of self care • Direct patients to transition internet sites • To avoid overlooking important educational topics, an “educational checklist” can be placed in all outpatient charts

A helpful mnemonic to remember issues • T Tattoos, piercings and antibiotic prophylaxis • E Education • E Exercise • N Need life long care • A Access to care and insurance • G General health • E Employment • R Relationships • S Smoking, alcohol and drugs

How to transition • Make a habit of speaking to young patients on their own • Review gradually and regularly during teenage years • Encourage patient to communicate their concerns • Encourage teenagers to contact office • Include patients in decision-making

How to transition • Develop a written transition plan with patient and family: • Display a public commitment to transition • Establish education as a priority • Consider referring patients to a regional “medical home” • Transfer of care letter with relevant medical and psychosocial information and care plan • Transfer to ACHD clinic

Medical Home • AAP: primary care that is accessible, continuous, comprehensive, family-centered, coordinated, compassionate, and culturally effective • Partnership between family and primary health care provider • Ideal place to educate patient with chronic health care needs and prepare for transfer to adult care

Video Participate 9: 48 to 11: 00

Transition Resources • Formal transition clinic for 14 to 16 year old • Group classes • Regional patient and family conferences • One-on-one nurse education • Generic transition services • Camp and mentorship

Transition Visits • Invitation to visit the ACHD clinic • Meet members of the adult team • Tour of the clinic area ± hospital • physical or virtual • Provide resource materials

After Transfer • No further appointments in pediatric services • Patient and pediatric provider contact • should be discouraged • only if agreed to by ACHD clinic • Communication between medical or nursing teams

Conclusion • Transition highlighted by AAP, ACP and AAFP • Transition is a purposeful and planned process that begins in early adolescence • Effective transition programs must address the needs of patients, family members, and health care providers • Improving transition process may reduce the number of patients lost to follow-up

Conclusion • Although this module is focused on CHD, the principles are applicable to all patients with special health care needs

Question 11 • According to the American Academy of Pediatrics, at what age should you have a written transition plan with patient and family? A. 10 years B. 12 years C. 14 years D. 16 years E. 18 years

Question 12 • A medical care home is a: A. Foster home for teenagers requiring medical supervision B. Partnership between family and primary health care provider C. Home health care for chronically ill patients D. Patient-centered access to care

Question 13 • Are the following statements true or false? A. Transition of care is the same as transfer of care B. You should always see 10 year old patients alone without their parents C. If you see adult patients you do not need to provide education about transition D. Transition refers to a shift in responsibility of health care management from the family to the patient E. The insurance companies are the main barrier to transition

Question 14 A 15 -year-old boy comes to your office for a sports physical examination. Compared with when you saw him at his 10 -year-old health supervision visit, he has progressed from Sexual Maturity Rating 1 to 4. Of the following, the laboratory value that is MOST likely to have changed is: A. Calcium B. Hemoglobin C. Platelet count D. Serum albumin E. White blood cell count

Question 15 According to the American Academy of Pediatrics (AAP), transition is: A. An alteration in discussion with young adults B. A change in the management of teenagers with chronic disease C. The purposeful planned process that supports adolescents with chronic health conditions and allows them to move from a pediatric practice to an adult-oriented healthcare practice D. The way we treat adolescents in clinic

Question 16 Which of the following statements about transition is most likely? A. Teenagers know about recommendations for health care but they do not want to follow the guidelines B. You should not repeat information and recommendations with teenagers after you have discussed them C. Transition should continue after the patient reaches 21 years D. Start talking with teenagers about lifelong care needs when they become 16 years

Question 17 A 16 -year-old girl who attends boarding school in your community comes to your office because she is feeling depressed. You see her alone for the visit, and she relates that she feels suicidal at this time and has a plan to kill herself. Of the following, the BEST description of your obligation to alert her parents to her situation is that: A. No parental notification is necessary because she is a mature minor B. No parental notification is necessary because she is an emancipated minor C. Parental notification is necessary due to billing issues D. Parental notification is necessary due to her serious threats of self-harm E. Parental notification is prohibited by the Health Insurance Portability and Accountability Act

Question 18 Which of the following is a significant barrier to transitioning an adolescent with congenital heart disease? A. Parents inability to let go B. Unfamiliarity of treating adult issues C. Insurance coverage D. Learned pediatric adaptive behaviors E. All of the above

Question 19 A community group asks you to speak at a forum on teenage pregnancy. O f the following, the MOST appropriate statement to include is that: A. Adolescent fathers do not have increased school drop-out rates B. Adolescents who become pregnant have the same vocational opportunities as their non-pregnant female peers C. Most adolescent pregnancies occur in 14 - to 16 -year-old young women D. Poverty is correlated significantly with adolescent pregnancy E. The adolescent pregnancy rate is increasing in the United States

Question 20 Young patients with chronic illness should: A. Not be compliant with medication B. Not participate in making any medical decisions C. Answer all the questions without assistance D. Take greater responsibility for their health care E. Never be seen alone by a medical provider

Question 21 • Next time you see a 7 year old patient with tetralogy of Fallot what would you do differently?

Question 22 • Next time you see a teenage patient with coarctation of the aorta what would you do differently?

Question 23 • List issues that you should discuss with teenager with CHD

Thank you
- Slides: 60