Economic evidence for NCDs burden costeffectiveness the cost

Economic evidence for NCDs - burden, cost-effectiveness & the cost of scaling-up Dan Chisholm, Ph. D Noncommunicable diseases and Mental Health (formerly Dept of Health Systems Financing) 1| Department of Health Systems Financing Better Financing for Better Health

Overview 10: 30 -11: 15 -12: 00 2| Economic burden of NCDs Cost-effectiveness of clinical and public health interventions for NCD prevention and control Funding healthcare to maximise NCD prevention and control 1. Rationale for an economic perspective 2. Basic principles and methods of costeffectiveness analysis 3. Best buys for NCD prevention and control 1. The financial cost of scaling-up 2. The relative merits of different health insurance mechanisms 3. Key dimensions of health system financing and universal coverage Department of Health Systems Financing Better Financing for Better Health

Overview – economic burden / cost-effectiveness analysis l Economic impact (burden to health system and beyond) – costs to whom? - private households, public services, society – scope / range of costs? - health, welfare – implications for government (projections of future impact) l Cost-effectiveness (efficiency of care & prevention strategies) 3| – Comparative intervention cost-effectiveness (across diseases and age groups) – Identifying 'best buys' for key contributors to chronic disease burden Department of Health Systems Financing Better Financing for Better Health

What are the economic consequences of NCDs? Who do the costs fall on? 4| Department of Health Systems Financing Better Financing for Better Health
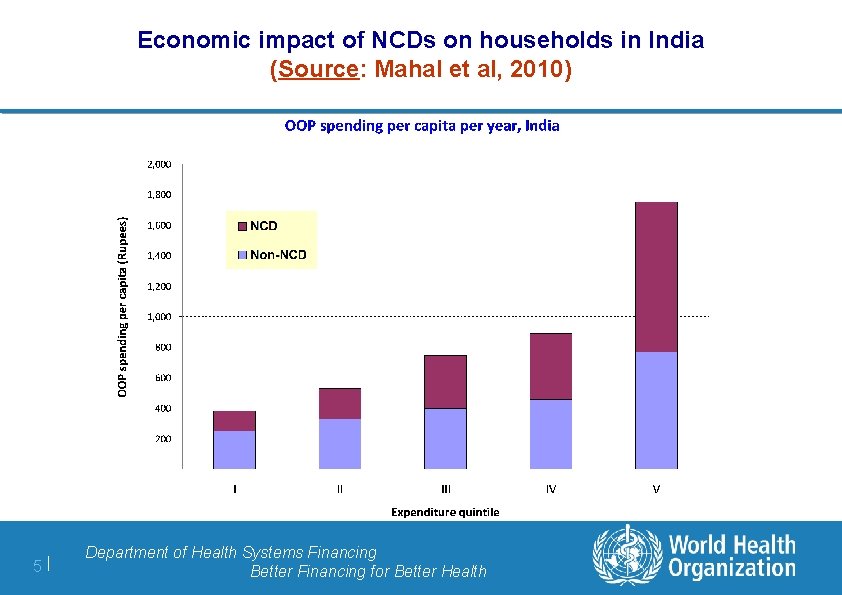
Economic impact of NCDs on households in India (Source: Mahal et al, 2010) 5| Department of Health Systems Financing Better Financing for Better Health
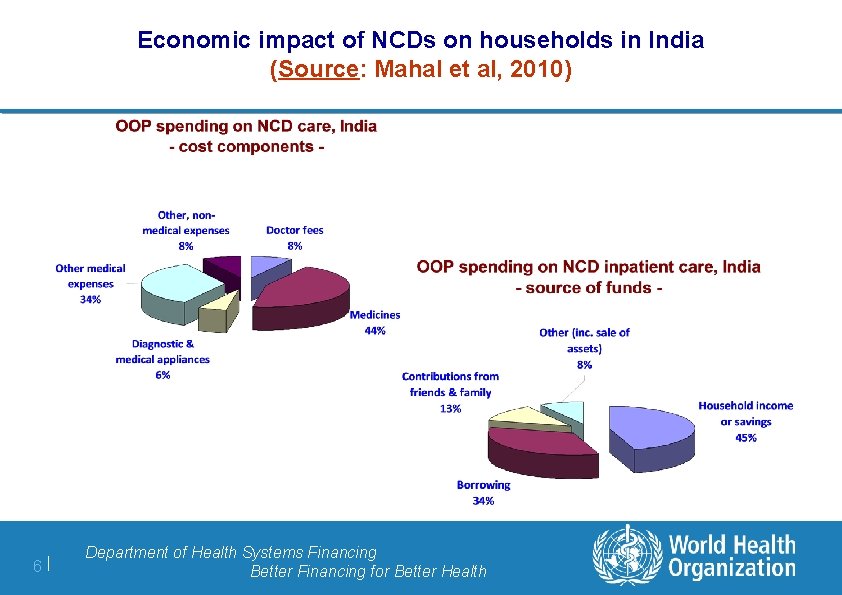
Economic impact of NCDs on households in India (Source: Mahal et al, 2010) 6| Department of Health Systems Financing Better Financing for Better Health

Macroeconomic / societal impact of NCDs 1. The cost-of-illness (COI) approach, a commonly used method that sets out to capture the societal economic impact of disease; it focuses mainly on foregone income and personal medical care costs associated with NCDs; 2. The economic growth approach, which estimates the projected impact of NCDs on aggregate economic output (GDP) by considering how these diseases deplete labour, capital and other factors to production levels in a country (see Figure below). 3. The value of statistical life (VSL) approach, which reflects a population’s willingness to pay to reduce the risk of disability or death associated with NCDs. By placing an economic value on the loss of health itself, this approach goes beyond the impact of NCDs on GDP alone. 7| Department of Health Systems Financing Better Financing for Better Health
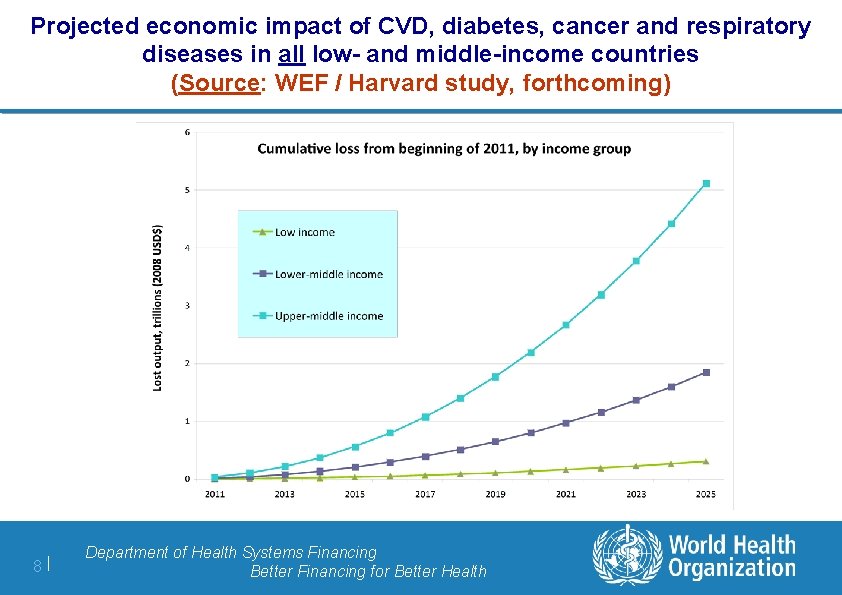
Projected economic impact of CVD, diabetes, cancer and respiratory diseases in all low- and middle-income countries (Source: WEF / Harvard study, forthcoming) 8| Department of Health Systems Financing Better Financing for Better Health

Cost-effectiveness analysis Costs Consequences Programme-level: • administrative staffing • training • drug supply / distribution Individual-level: • treatment (drugs, therapy) • inpatient care • outpatient & primary care Programme-level / intermediate: Intervention populations: (enhanced care or new treatment) • referral • treatment rates / quality vs Individual-level / final: Non-intervention populations: (usual care or no treatment) • ancillary care 9| • detection Department of Health Systems Financing Better Financing for Better Health • morbidity • mortality • QALY, DALY (composite indices)

Approaches to cost-effectiveness analysis § Alongside (long-term) prospective studies § observational § experimental § Modelling § decision analytic methods (e. g. 5 -year cohort incidence model) § population-based disease modelling (e. g. WHO-CHOICE) 10 | Department of Health Systems Financing Better Financing for Better Health

CHOosing Interventions that are Cost-Effective (www. who. int/choice) l CHOICE is WHO's work programme on cost-effectiveness l Use of a common set of tools and methods – enhances comparability between diseases / risk factors l Sectoral, population-level CEA – effectiveness: – resource costs: healthy years gained over the lifetime of a population, with / without intervention patient + programme level (intl $ or local units) l Results summarised in WHO regional C-E databases – available for country-level adaptation / analysis 11 | Department of Health Systems Financing Better Financing for Better Health

WHO-CHOICE series on NCDs and injury 12 | Department of Health Systems Financing Better Financing for Better Health
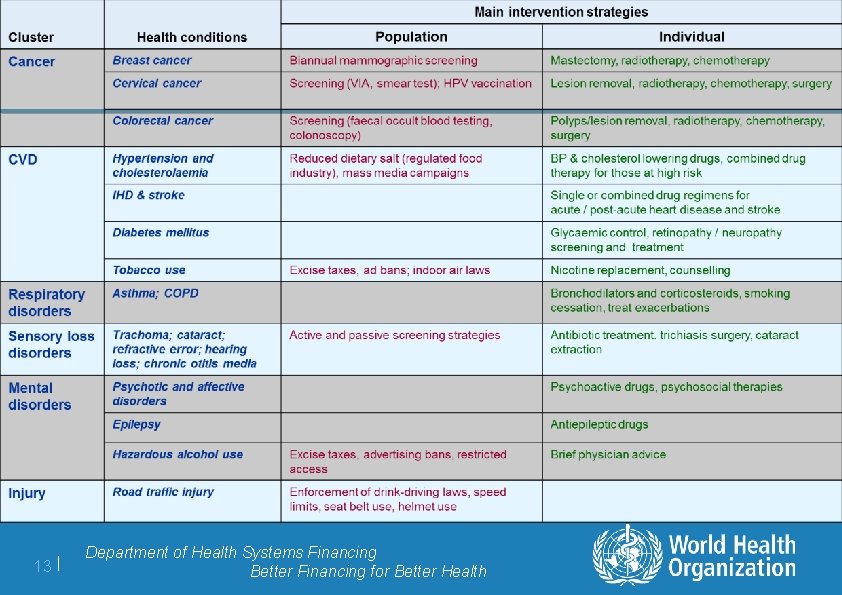
13 | Department of Health Systems Financing Better Financing for Better Health
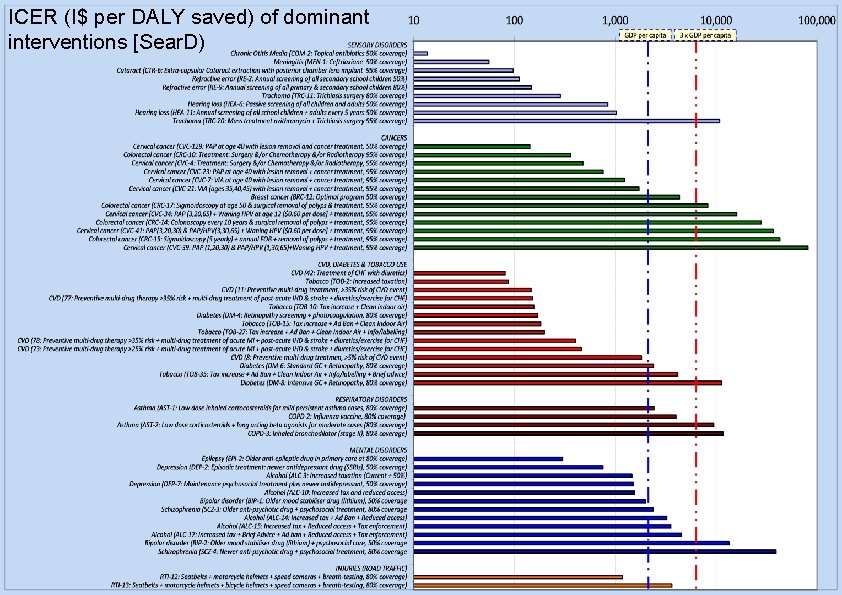
ICER (I$ per DALY saved) of dominant interventions [Sear. D) 14 | Department of Health Systems Financing Better Financing for Better Health

NCDs risk factors – identification of 'best buys' l 'Best buy' – an intervention that is: – very cost-effective – low cost – feasible, acceptable and appropriate l 'Good buy' – an intervention that does not meet all of 'best buy' criteria but which offers good value and has other attributes that recommends its use l Policy-makers can consider best buys as a core set of interventions for priority scale-up, and good buys as an expanded set of interventions to be made available when resources allow. 15 | Department of Health Systems Financing Better Financing for Better Health
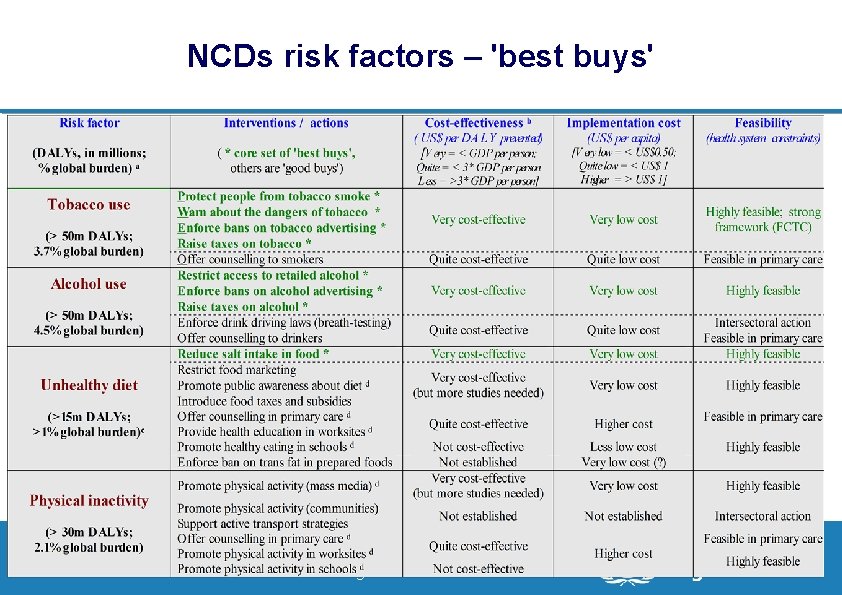
NCDs risk factors – 'best buys' 16 | Department of Health Systems Financing Better Financing for Better Health
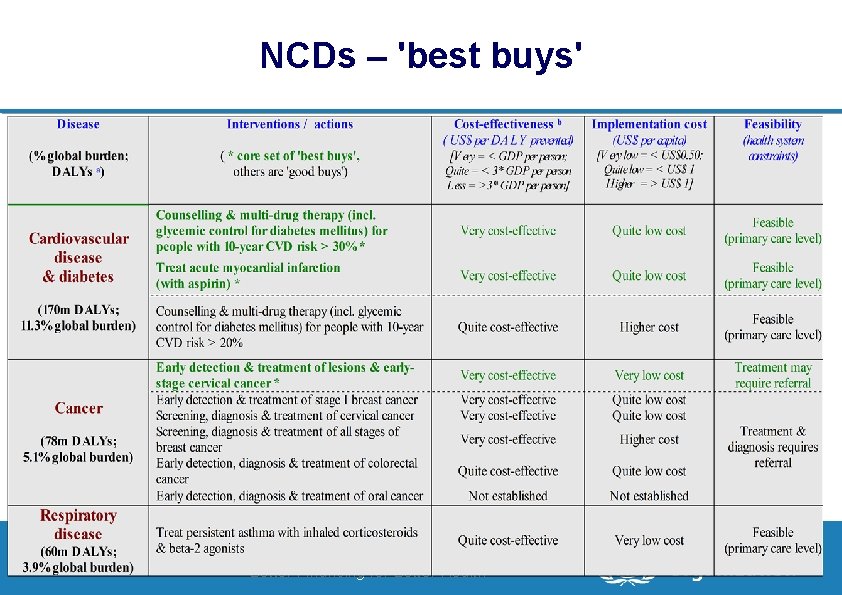
NCDs – 'best buys' 17 | Department of Health Systems Financing Better Financing for Better Health

Costs and cost-effectiveness - key points l Health & social welfare costs of chronic disease – already large and growing rapidly (ageing populations) – a major challenge for public health and for government policy – economic or financial impact studies can help make the investment case l Economic evidence for policies concerning chronic disease prevention & mgt – Paucity of studies in low- and middle-income countries – Largely a vertical disease approach (vs more horizontal, health platform approach) – Long time lags / slow returns on investment – how to convince ministries of finance – Being 'cost-effective' does not mean an intervention is going to be financially feasible – Implementation of NCD best buys is inexpensive and will produce dramatic health gains 18 | Department of Health Systems Financing Better Financing for Better Health

Funding healthcare to maximise NCD prevention and control Dan Chisholm, Ph. D Dept of Health Systems Financing, WHO Geneva 19 | Department of Health Systems Financing Better Financing for Better Health

Overview 11: 15 -12: 00 20 | Funding healthcare to maximise NCD prevention and control 1. The financial cost of scaling-up 2. The relative merits of different health insurance mechanisms 3. Key dimensions of health system financing and universal coverage Department of Health Systems Financing Better Financing for Better Health

Cost of scaling-up a cost-effective NCD package Analysis was performed on a group of 42 low- and middle-income countries (with populations in excess of 20 million) that account for 90% of the chronic disease burden in developing regions of the world. Upward adjustments were made from this set in order to derive estimates for all low- and middle-income countries. The period of scaling-up was set at 2011 -2025 to achieve desired levels of treatment coverage (80%). Full implementation of population-based strategies would occur more rapidly (after approximately 5 -6 years). Key data sources included UN Population Division statistics, WHO Global Burden of Disease and risk factor surveillance estimates, international treatment guidelines, and cost databases. 21 | Department of Health Systems Financing Better Financing for Better Health

What to scale up? NCD 'best buys' (Source: NCD Global Status Report; WHO, 2011) Condition Interventions Tobacco use Tax increases; smoke-free indoor workplaces & public places; health information / warnings; advertising/promotion bans Alcohol use Tax increases; restrict retail access; advertising bans Unhealthy diet & physical inactivity Reduced salt intake; replacement of trans fat; public awareness about diet & physical activity CVD & diabetes Counselling & multi-drug therapy (including glycaemic control for diabetes) for people with >30% CVD risk (including those with CVD); treatment of heart attacks with aspirin Cancer Hepatitis B immunization to prevent liver cancer; screening & treatment of pre -cancerous lesions to prevent cervical cancer 22 | Department of Health Systems Financing Better Financing for Better Health
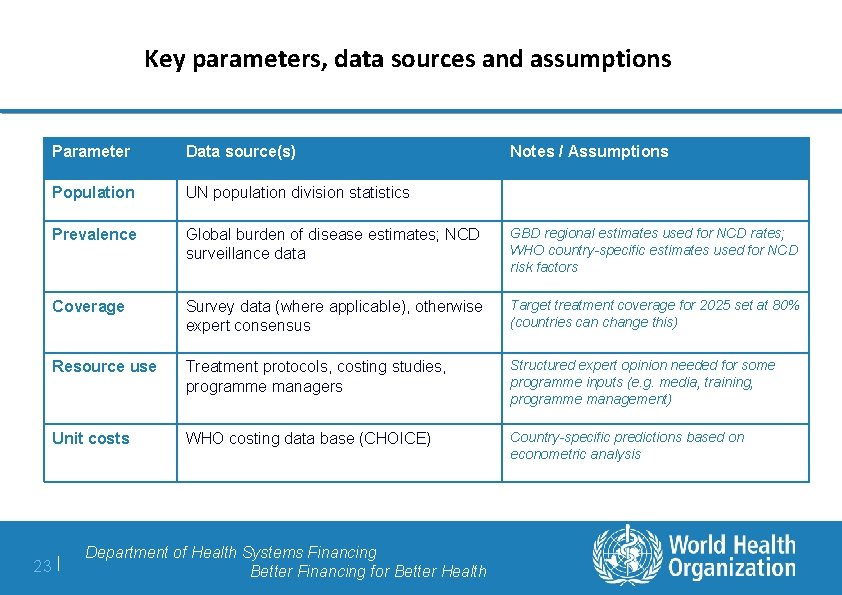

Key parameters, data sources and assumptions Parameter Data source(s) Population UN population division statistics Prevalence Global burden of disease estimates; NCD surveillance data GBD regional estimates used for NCD rates; WHO country-specific estimates used for NCD risk factors Coverage Survey data (where applicable), otherwise expert consensus Target treatment coverage for 2025 set at 80% (countries can change this) Resource use Treatment protocols, costing studies, programme managers Structured expert opinion needed for some programme inputs (e. g. media, training, programme management) Unit costs WHO costing data base (CHOICE) Country-specific predictions based on econometric analysis 23 | Department of Health Systems Financing Better Financing for Better Health Notes / Assumptions
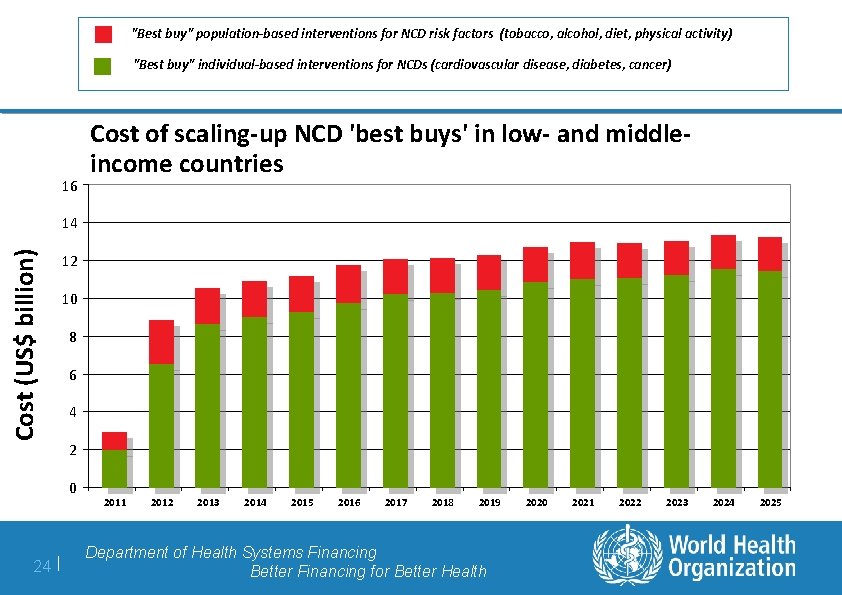
"Best buy" population-based interventions for NCD risk factors (tobacco, alcohol, diet, physical activity) "Best buy" individual-based interventions for NCDs (cardiovascular disease, diabetes, cancer) 16 Cost of scaling-up NCD 'best buys' in low- and middleincome countries Cost (US$ billion) 14 12 10 8 6 4 2 0 24 | 2011 2012 2013 2014 2015 2016 2017 2018 2019 Department of Health Systems Financing Better Financing for Better Health 2020 2021 2022 2023 2024 2025

So, how much will it cost to scale-up these NCD 'best buys'? Answer: for all LMIC, US$ 11. 4 billion per year on average • • 25 | Population-based measures: close to US$ 2 billion per year • Low- and lower-middle-income countries: < US$ 0. 20 per head • Upper-middle income countries: < US$ 0. 50 per head Individual-based measures: nearly US$ 10 billion per year • Low-income countries: < US$ 1. 00 per head • Lower middle-income countries: < US$ 1. 50 per head • Upper-middle income countries: ~ US$ 2. 50 per head Department of Health Systems Financing Better Financing for Better Health

Who is going to pay for all this? Health Financing Mechanisms Financing mechanisms Tax-based financing Health care services 1. General tax or other revenue Social health insurance 2. Payroll tax Other prepayment schemes 3. Contribution or premium Out-of-pocket payments 26 | Financing sources External resource Household 4. Direct payment Department of Health Systems Financing Better Financing for Better Health Natural resource revenue
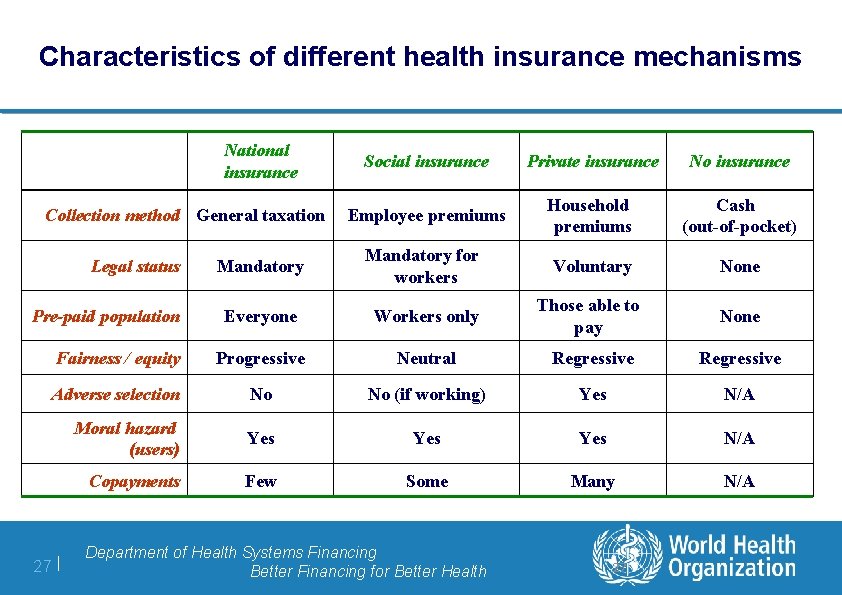
Characteristics of different health insurance mechanisms National insurance Social insurance Private insurance No insurance Employee premiums Household premiums Cash (out-of-pocket) Mandatory for workers Voluntary None Everyone Workers only Those able to pay None Fairness / equity Progressive Neutral Regressive Adverse selection No No (if working) Yes N/A Moral hazard (users) Yes Yes N/A Copayments Few Some Many N/A Collection method General taxation Legal status Pre-paid population 27 | Department of Health Systems Financing Better Financing for Better Health 27

Financing for universal health coverage - WHR 2010 1. What is meant by universal coverage? All people have access to needed health services - prevention, promotion, treatment and rehabilitation - without the risk of financial hardship associated with accessing services. 2. Where are we? In many LMIC, a long way away. . . service coverage for NCDs and many other disorders very low, while the extent of financial catastrophe and impoverishment worryingly high. Richer countries also moving further away from it either with increases in cost-sharing or as a result of financial crisis. 3. What can be done? Various options / actions available, including better protection for the worse off, better use of existing resources and raising new sources of funding for health. 28 | Department of Health Systems Financing Better Financing for Better Health
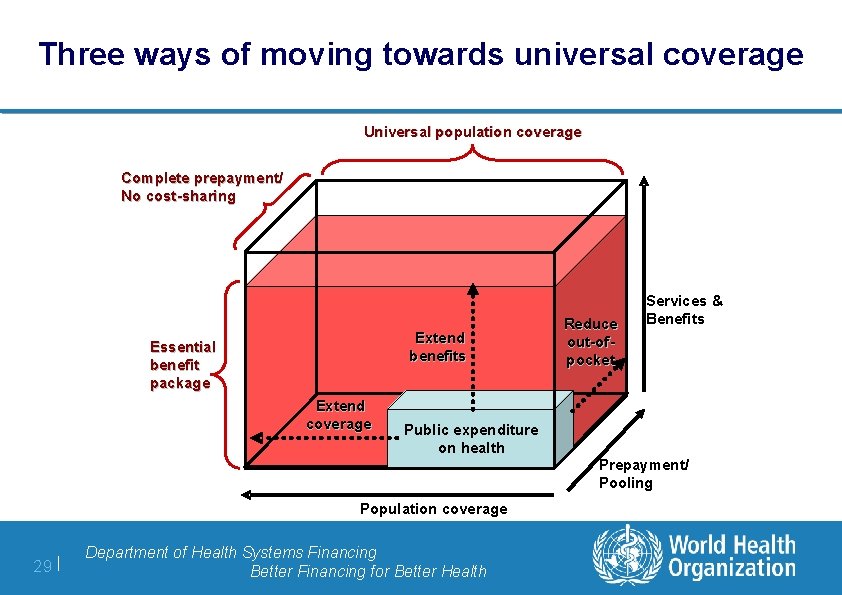
Three ways of moving towards universal coverage Universal population coverage Complete prepayment/ No cost-sharing Extend benefits Essential benefit package Extend coverage Reduce out-ofpocket Services & Benefits Public expenditure on health Prepayment/ Pooling Population coverage 29 | Department of Health Systems Financing Better Financing for Better Health

Where are we now? 1. Heavy reliance on out of pocket payments (OOPs) to finance health in many countries – prevents many from using services and results in financial catastrophe and impoverishment for many who do. – – – 150 million people face financial catastrophe 100 million people are pushed below the poverty line Millions of people do not have access to effective / affordable health care 2. Inefficient and inequitable use of the resources that are available. 3. Even if we get this right, simply insufficient funds in may countries, despite large increases in DAH since 2000. Even high income countries continually trying to find the resources necessary to keep their systems moving forward and to meet people's expectations. 30 | Department of Health Systems Financing Better Financing for Better Health
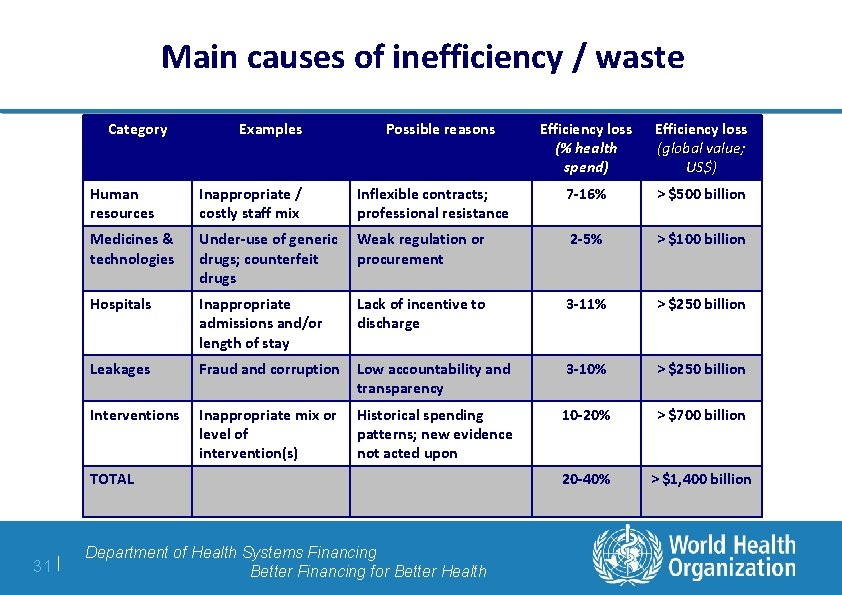

Main causes of inefficiency / waste Category Examples Possible reasons Efficiency loss (global value; US$) Human resources Inappropriate / costly staff mix Inflexible contracts; professional resistance 7 -16% > $500 billion Medicines & technologies Under-use of generic drugs; counterfeit drugs Weak regulation or procurement 2 -5% > $100 billion Hospitals Inappropriate admissions and/or length of stay Lack of incentive to discharge 3 -11% > $250 billion Leakages Fraud and corruption Low accountability and transparency 3 -10% > $250 billion Interventions Inappropriate mix or level of intervention(s) Historical spending patterns; new evidence not acted upon 10 -20% > $700 billion 20 -40% > $1, 400 billion TOTAL 31 | Efficiency loss (% health spend) Department of Health Systems Financing Better Financing for Better Health

What can be done? 1. Reducing financial barriers to coverage, and protecting people against financial risks of ill health – how to increase pooling, to protect people against financial catastrophe and impoverishment. How to maintain it and prevent reversals. 2. Use funds more efficiently and equitably: Analysis of the nature and extent of inefficiencies and inequalities, and what steps have and can be taken to improve them. This will have practical examples of how improvements can be made. 3. Raise sufficient funds for health – practical suggestions, mix of external (for low income countries) and domestic. 32 | Department of Health Systems Financing Better Financing for Better Health

Innovative Financing? l Low-income countries will be unable to finance the levels of spending required to scale up services from domestic sources for many years l Despite large increases in external financial assistance since 2000, it remains insufficient, and only a few donors are on track to meet their own international targets l Mobilizing additional traditional ODA funds when the global economy is in turmoil is a major challenge l Innovative financing mechanisms can complement traditional aid and help deliver urgently needed financing l Scope for design of more efficient, more effective funding and uses 33 | Department of Health Systems Financing Better Financing for Better Health
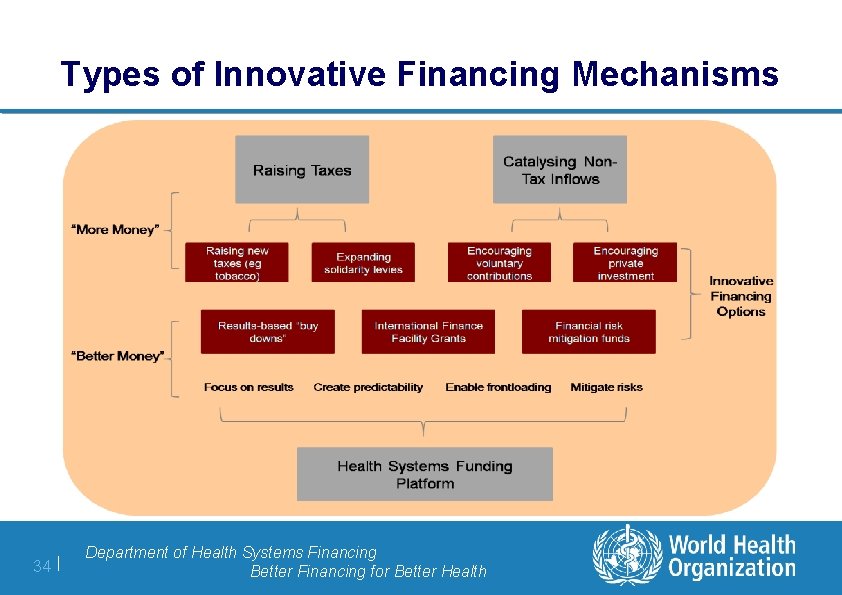
Types of Innovative Financing Mechanisms 34 | Department of Health Systems Financing Better Financing for Better Health

Health financing for NCDs – key points 1. Reduce OOPs / increase pre-payment § Systemic rather than disease-specific issue, however OOPs for chronic diseases / conditions particularly regressive and impoverishing because they endure over time (need more research showing the economic impact of NCDs on household budgets/incomes) 2. Use funds more efficiently and equitably: § Identify 'best buys' for prevention and opportunities for positive synergies re: treatment in PHC 3. Raise sufficient funds for health § § § 35 | Better articulation of and budgeting for core NCD packages / components Costing tool for scaling-up (evidence-based advocacy) Additional funding via sin taxes (e. g. alcohol, tobacco) Department of Health Systems Financing Better Financing for Better Health
- Slides: 35