ECONOMIC EVALUATION OF HEALTHCARE INTERVENTIONS Kristian Bolin PRELIMINARIES

ECONOMIC EVALUATION OF HEALTH-CARE INTERVENTIONS Kristian Bolin

PRELIMINARIES • Why perform an economic evaluation? • We need information that can help us use resources efficiently

THERE IS A NEED FOR ECONOMIC EVALUATIONS IN THE AREA OF HEALTH CARE • Demand > Supply but rationing as in a free market not possible – or acceptable • Prioritisation – choices – via ‘administrative’ decisions; – lists with pharmaceuticals that may be used or interventions that are regarded as cost-effective • Economic evaluations used as support for decisions • The prioritisation problem is not trivial, i. e. substantial amount of resources spent on health care

PRELIMINARIES • Technological progress – new pharmaceuticals or new treatments – Improvements in survival and quality of life – Increased or decreased total healthcare costs – Changes in survival may influence productivity – Improved health may reduce work absenteeism and early pensions SHOULD THE NEW TECHNOLOGY BE IMPLEMENTED?

METHODS • The objective of an economic evaluation is to find out whether or not an intervention should be implemented or not by comparing benefits and costs • How do we perform an economic evaluation? • Methods: – Cost-benefit analysis (welfarist approach) – Cost-effectiveness analysis (non-welfarist approach) • Data: – Measurements - how, in practise can we collect information? – Some variables cannot be directly observed

COST-EFFECTIVENESS ANALYSIS (of health-care interventions) • The intervention can be a new or improved treatment for, for instance, cancer, CHD, or COPD (a pharmaceutical or treatment involving healthcare utilisation) • The intervention can also be more complex and involve the interaction between supplier and receiver, for instance, a new system for dental insurance
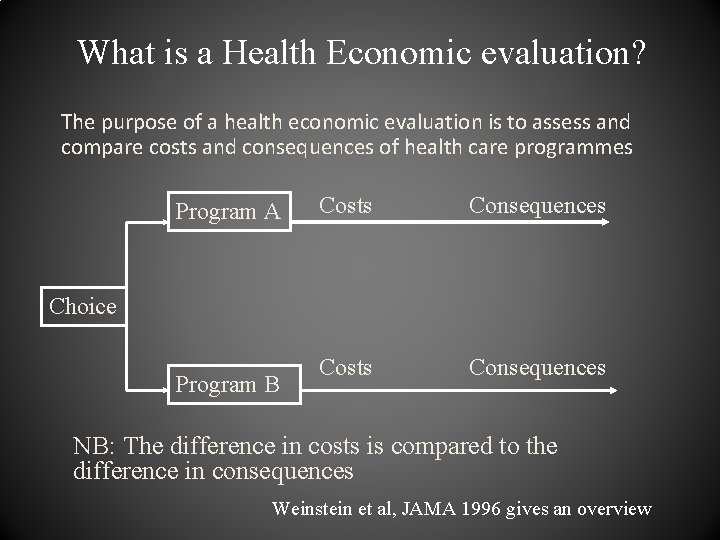
What is a Health Economic evaluation? The purpose of a health economic evaluation is to assess and compare costs and consequences of health care programmes Program A Costs Consequences Choice Program B NB: The difference in costs is compared to the difference in consequences Weinstein et al, JAMA 1996 gives an overview

COST-EFFECTIVENESS ANALYSIS • The basic outcome measure in a costeffectiveness analysis is the incremental costeffectiveness ratio (ICER): • Cost 1 and cost 2 are the costs involved in the treatment alternatives being compared • Similar for Effects • Actual marginal cost of implementation is often not taken into account

Cost and effect components in the ratio • US Panel argued that (Weinstein et al, JAMA 1996): – Net expenditure in the numerator • Costs of health care services • Costs of patient time expended for the intervention • Costs for care giving, travelling – Net improvement in health in the denominator • Effect on length and quality of life • HRQL should be captured in such a way that effects of morbidity on productive time (loss of income) and leisure are incorporated • Alternative and dominating view (Johannesson& Meltzer, Health Economics 1998): – Change/effect on leisure time can be assumed to be captured by the QALY – However, loss of productivity due to morbidity can not be assumed to be captured by the QALY • Individuals do not bear the full cost • Even when sick-leave is not fully paid, income and payroll taxes imply that the individual bear only a proportion of the cost – Furthermore, if QALYs were to capture loss of productivity, then why not also cost of health care, at least ‘out of pocket’ cost

Valuing productivity costs • Gross earnings lost – Changes in amount of time individuals can allocate to paid work (also, in principle, changes in productivity whilst at work) is valued by change in gross earnings (gross wage x time lost) – Gross wage reflects the value of the production at the margin – Rests firmly on neoclassic labour theory and theory of the firm • This assumes flexibility in prices and that all markets clear – Also known as the Human Capital approach : The value of an object (human capital) is determined by the owner’s financial loss from losing it (future income) – Critique: likely to result in overestimation i) marginal value of production often less than average value, ii) unemployment

Valuing productivity costs • The friction cost approach – Involuntary unemployment exist – can replace the sick worker; There will be a cost for identifying and training; loss of productivity during the friction period (until the replacement has taken place) – The value of lost production may be substantially less than with the human capital approach –especially for long-term sick-leave – Also, for short-term sick leave it has been argued that the worker may be able to ‘make up’ for the lost production on return to work, or work can be done by colleagues • Critique: – Not correct to assume that all vacancies can be filled by unemployed persons (country-specific data on length of friction period would not be enough, need data specific for location, industry, category of work) – Would imply that value of clinicians’ and other health care workers time also should be reduced – Assuming that workers can ‘make up’ upon their return is not in line with important elements of economic theory – someone “looses”

Guidelines’ views • Läkemedelsförmånsnämnden (The Pharmaceutical Benefits Board): – “All relevant costs associated with treatment and illness should be identified, quantified and evaluated. The production loss for treatment and sickness should also be included (estimated using the human capital method). ” • Guidelines for Pharmacoeconomic Research in the Netherlands (The Health Care Insurance Board): – “When indirect costs outside the health care system (also known as productivity costs) are involved, these need to be calculated using the friction cost method. ” • NICE: – “. . the appropriate reference case perspective on costs is that of the NHS and PSS. In non-reference case analyses, significant resource costs imposed outside the NHS may also be considered …. but will not normally include productivity costs. ”

COST-EFFECTIVENESS ANALYSIS • EXAMPLE 1: intervention for smoking-cessation: • BENEFITS (compared to no intervention): – Reduced morbidity (COPD, CHD, Cancer) – Reduced mortality (and increased production in the economy) – Improved quality of life – Reduced healthcare costs • COSTS (compared to no intervention): – Treatment cost – Increased healthcare costs due to increased survival – Increased consumption due to increased survival • The timing of benefits and costs

COST-EFFECTIVENESS ANALYSIS • The cost-effectiveness ratio must take all costs and benefits that are influenced by the intervention into account • How can we measure all the varaibles needed in order to calculate a cost-effectiveness ratio for a specific intervention (compared to an alternativ)

COST-EFFECTIVENESS ANALYSIS • The dominating effect measure in healtheconomic evaluation: the QALY • Definition of a QALY: Life time weighted by the quality of that time • Thus, it is possible that an intervention has a larger effect than a comparison even though expected life time is lower than without the intervention • Pharmaceuticals can alleviate pain but shorten the remaining life time

COST-EFFECTIVENESS ANALYSIS • • Variables that we need to measure: Effect on survival Effect on quality of life Not the same as treatment effect (or efficacy)!
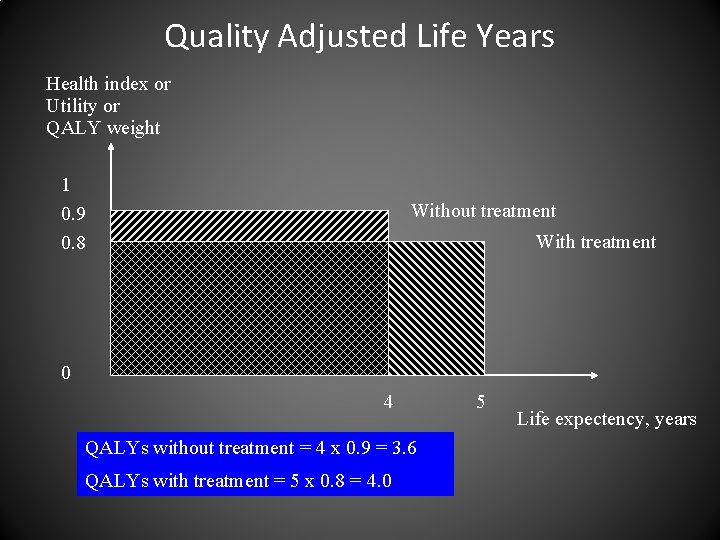
Quality Adjusted Life Years Health index or Utility or QALY weight 1 0. 9 0. 8 Without treatment With treatment 0 4 QALYs without treatment = 4 x 0. 9 = 3. 6 QALYs with treatment = 5 x 0. 8 = 4. 0 5 Life expectency, years

On QALY-weights • • • The QALY concept is grounded in decision science and expected utility theory It is assumed that individuals – and society - seek to maximize health – the value weighted time accumulated over the relevant time horizon Health states must be valued on a scale with 0 for being dead. By convention the upper end of the scale is defined as perfect health , with a value of 1 To permit aggregation of QALY changes, the scale should have interval scale properties; a gain from 0. 2 to 0. 4 is equally valuable as a gain from 0. 6 to 0. 8. States worse than death can exist, with a value below 0 An assumption of risk neutrality over life-years is also needed to ensure that the QALY is a useful representation of health state preferences See also Weinsten et al, Value in Health 2009

How to estimate QALY-weights • Rating Scale, Category Scaling, Visual Analogue Scale – Note; respondents are not faced with a ’choice’ • SG – Standard Gamble – A choice between a certain intermediate health state and a treatment with two possible outcomes, dead and healthy • TTO – Time Trade Off – A choice between living for a given time in a poor health state and living for a shorter time in full health

How to infer utilities STANDARD GAMBLE • Respondent choses probability p so that he or she is indifferent between alternatives p Full health Alt 1 1 -p Alt 2 Dead Health state (less than full health) Hi • If dead is assumed to correspond to utility=0, p will reflect the utility of the health state Hi

How to infer utilities TIME TRADE-OFF • Time in full health is related to time in health state Hi Health 1. 0 Hi Alt 1 Alt 2 x t Time • If x is chosen so that alt 1 and alt 2 are equally good, the utility of Hi is given by x/t
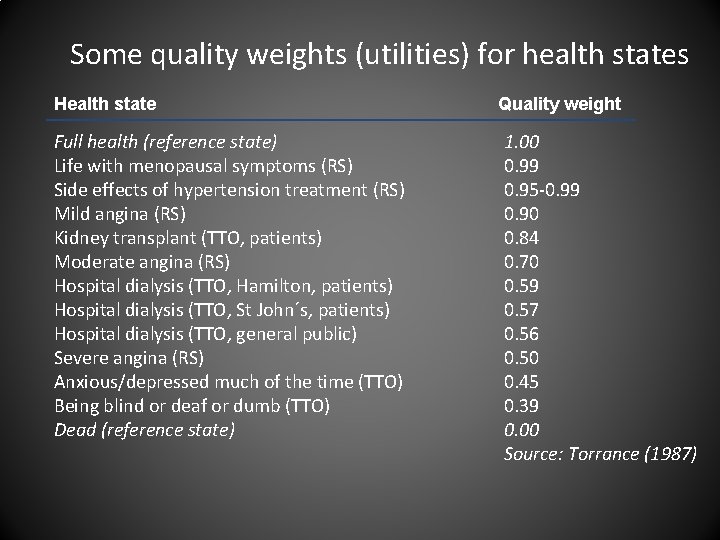

Some quality weights (utilities) for health states Health state Full health (reference state) Life with menopausal symptoms (RS) Side effects of hypertension treatment (RS) Mild angina (RS) Kidney transplant (TTO, patients) Moderate angina (RS) Hospital dialysis (TTO, Hamilton, patients) Hospital dialysis (TTO, St John´s, patients) Hospital dialysis (TTO, general public) Severe angina (RS) Anxious/depressed much of the time (TTO) Being blind or deaf or dumb (TTO) Dead (reference state) Quality weight 1. 00 0. 99 0. 95 -0. 99 0. 90 0. 84 0. 70 0. 59 0. 57 0. 56 0. 50 0. 45 0. 39 0. 00 Source: Torrance (1987)

COST-EFFECTIVENESS ANALYSIS • Definition of cost: – Opportunity cost: productivity given up when resources are used in a specific way. For instance, the number of patients not treated for condition X when resources instead are used for treating condition Y. – The opportunity cost is often valued in monetary terms, using a unit price for the forgone alternative.

How to calculate QALY in practise • First, we need a measure of utility • Common way to operationalise utility: – Utility is measured as a number – Normalisation so that utility can be between (and including) 0 and 1 • Second, when we have the utilities we multiply each time period’s utility by the lenght of the period

Modelling when relevant clinical trials do not exist • Synthesizing head-to-head comparisons – • Clinical trials sometimes compare new compound to placebo or – at least – omit some relevant active comparators Informing decisions in the absence of hard data – Clinical trials may not be feasible because of • • • Ethical considerations - for instance, when standard care is compared to less aggressive treatment Sample size requirements - screening Long follow-up – vaccination See also Brennan & Akehurst, Pharmacoeconomics , 2000

Modelling in economic evaluations alongside clinical trials • Combining several data sources to reflect all appropriate evidence – Resource use, unit costs, utilities etc. • Extrapolating from intermediate clinical endpoints to final outcomes – From, for instance, clinical events avoided to life years gained (or, preferably, QALYs gained) • Extrapolating beyond the period observed in a trial See also Brennan & Akehurst, Pharmacoeconomics , 2000
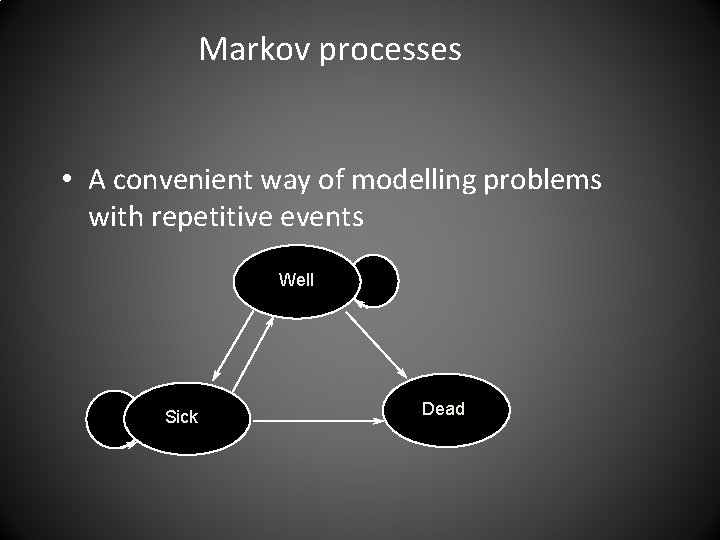
Markov processes • A convenient way of modelling problems with repetitive events Well Sick Dead

Markov processes • The patient is always in one of a finite number of states Markov states • The time horizon is divided into equal increments of time Markov cycles; the length of each cycle depends on the problem studied • During each cycle the patient may make a transition from one state to another - this is how events are modelled • States can be transient, temporary (just once) or absorbing • Transition probabilities can be constant or time-dependent (no. of cycles) – When the transition probability is constant the Markov models are referred to as Markov chains

Markov processes • Each state is assigned a cost and an effect, the contribution to the overall result depends on the time spent in the state • The Markovian assumption (a key limitation): – The transition probabilities depend only on the current health state – disease history is not taken into account • Can be circumvented by more health states
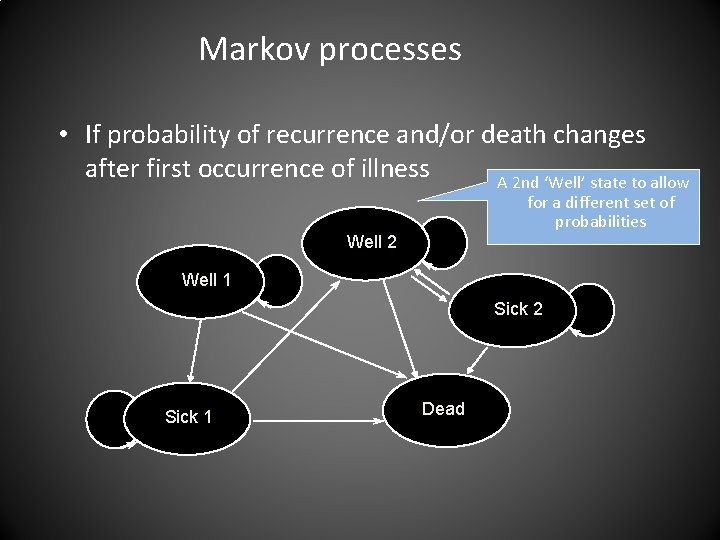
Markov processes • If probability of recurrence and/or death changes after first occurrence of illness A 2 nd ‘Well’ state to allow for a different set of probabilities Well 2 Well 1 Sick 2 Sick 1 Dead
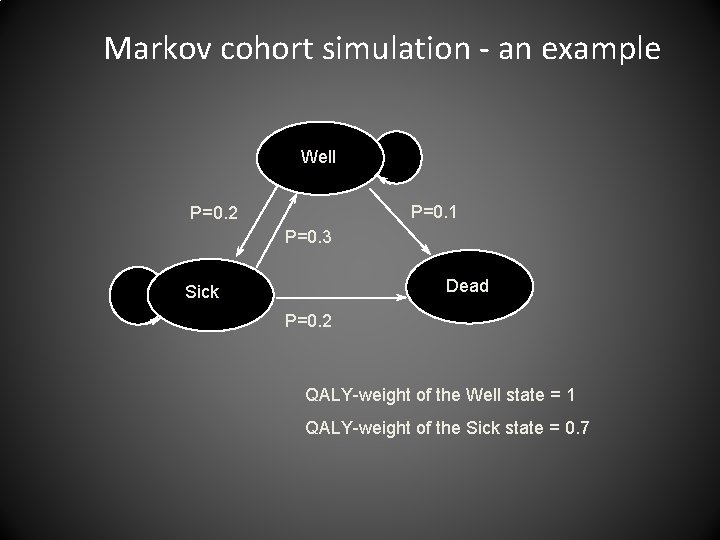
Markov cohort simulation - an example Well P=0. 1 P=0. 2 P=0. 3 Dead Sick P=0. 2 QALY-weight of the Well state = 1 QALY-weight of the Sick state = 0. 7
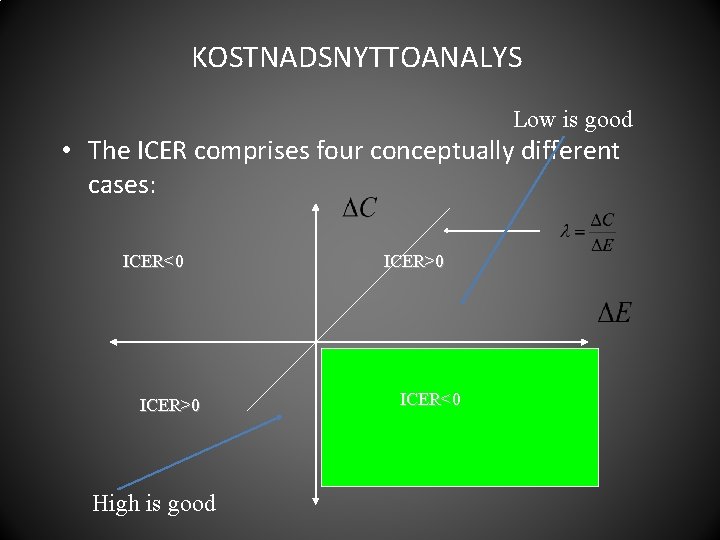
KOSTNADSNYTTOANALYS Low is good • The ICER comprises four conceptually different cases: ICER<0 ICER>0 High is good ICER>0 ICER<0

KRITERIUM FOR KOSTNADEFFEKTIVITET 2 • Problem med ICER: oklart hur värden i de olika kvadranterna skall tolkas • Alternativ: ”Nettomarginalnyttan” – NMB
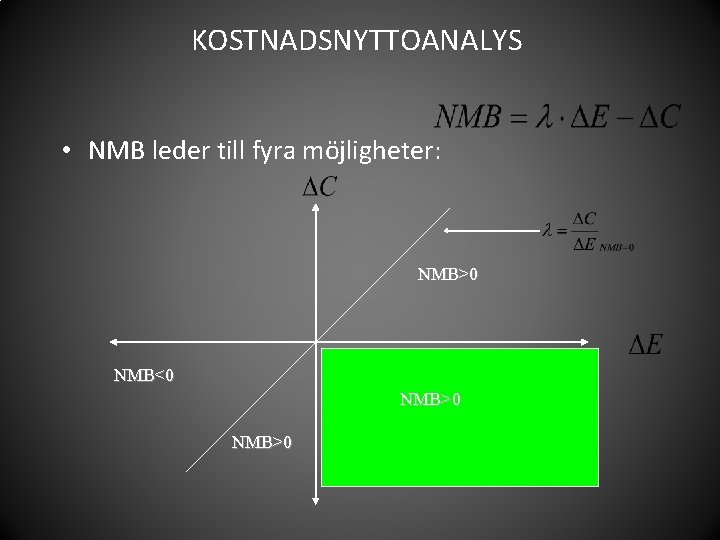
KOSTNADSNYTTOANALYS • NMB leder till fyra möjligheter: NMB>0 NMB<0 NMB>0
- Slides: 34