Economic burden of NCDs and costeffective responses by

Economic burden of NCDs and costeffective responses by David B Evans, Director Department of Health Systems Financing 1| Department of Health Systems Financing: Better Financing for Better Health

Question Is there a tension between a clinical perspective and a population health perspective? Is there tension between a health systems perspective and a disease-specific perspective? 2| Department of Health Systems Financing: Better Financing for Better Health

Outline 1. The challenges of health financing from a system perspective 2. What are the synergies between questions of economic burden and costeffectiveness of NCDs and a health systems financing perspective? 3| Department of Health Systems Financing: Better Financing for Better Health

WHO Framework for Assessing Health Systems (World Health Report 2000; Everybody's Business 2006) I N P U T S 4| Department of Health Systems Financing: Better Financing for Better Health
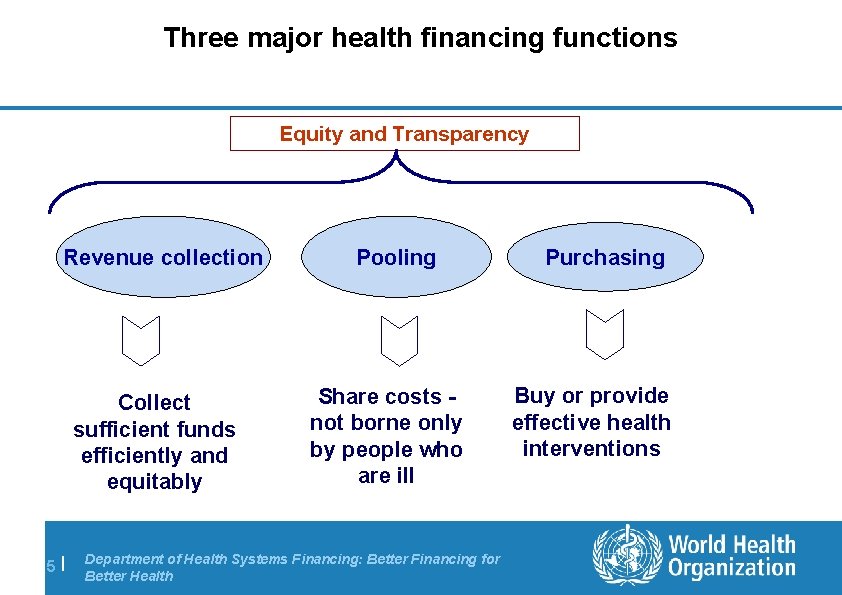
Three major health financing functions Equity and Transparency Revenue collection Collect sufficient funds efficiently and equitably 5| Pooling Share costs not borne only by people who are ill Department of Health Systems Financing: Better Financing for Better Health Purchasing Buy or provide effective health interventions
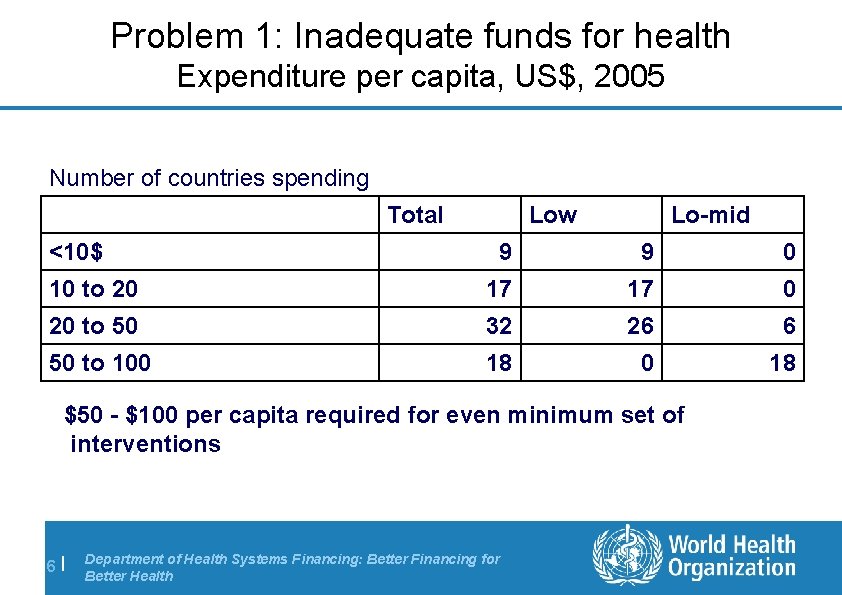
Problem 1: Inadequate funds for health Expenditure per capita, US$, 2005 Number of countries spending Total <10$ Low Lo-mid 9 9 0 10 to 20 17 17 0 20 to 50 32 26 6 50 to 100 18 $50 - $100 per capita required for even minimum set of interventions 6| Department of Health Systems Financing: Better Financing for Better Health
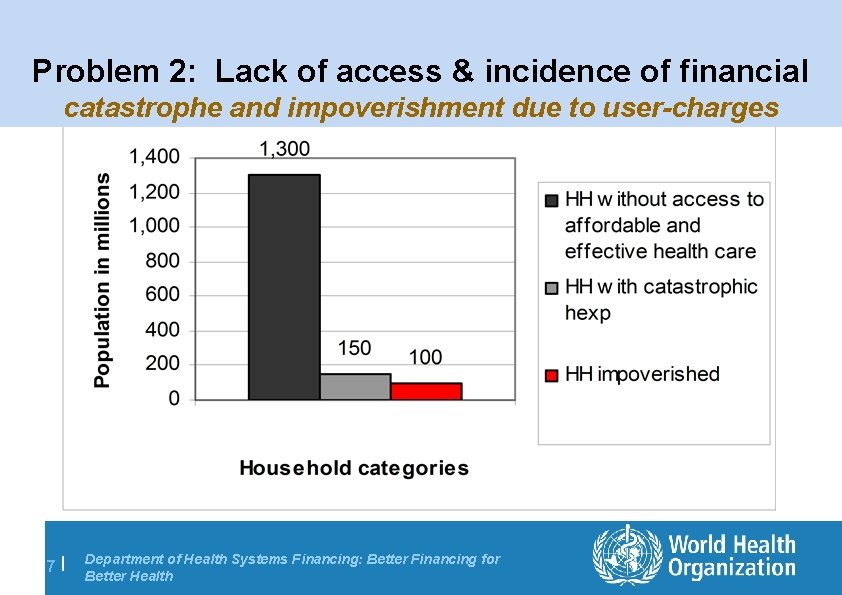
Problem 2: Lack of access & incidence of financial catastrophe and impoverishment due to user-charges 7| Department of Health Systems Financing: Better Financing for Better Health
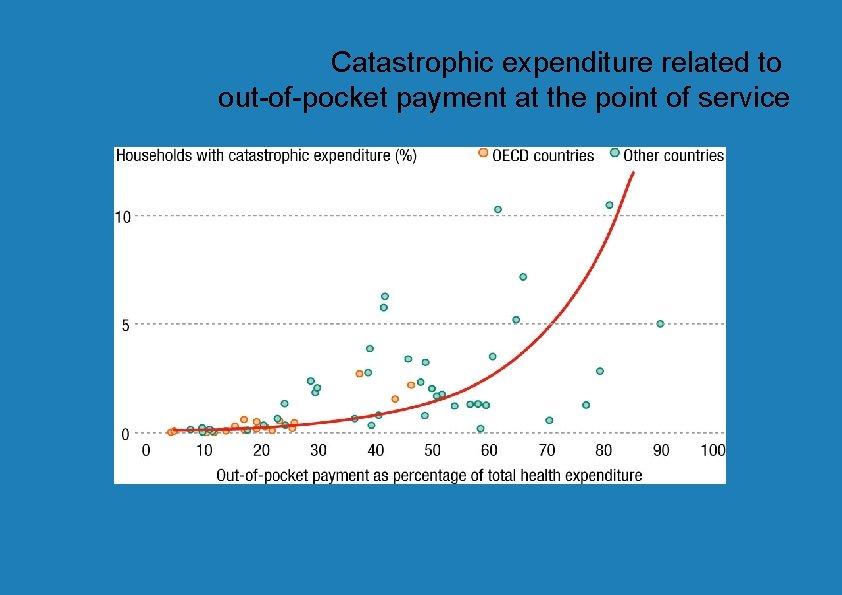
Catastrophic expenditure related to out-of-pocket payment at the point of service
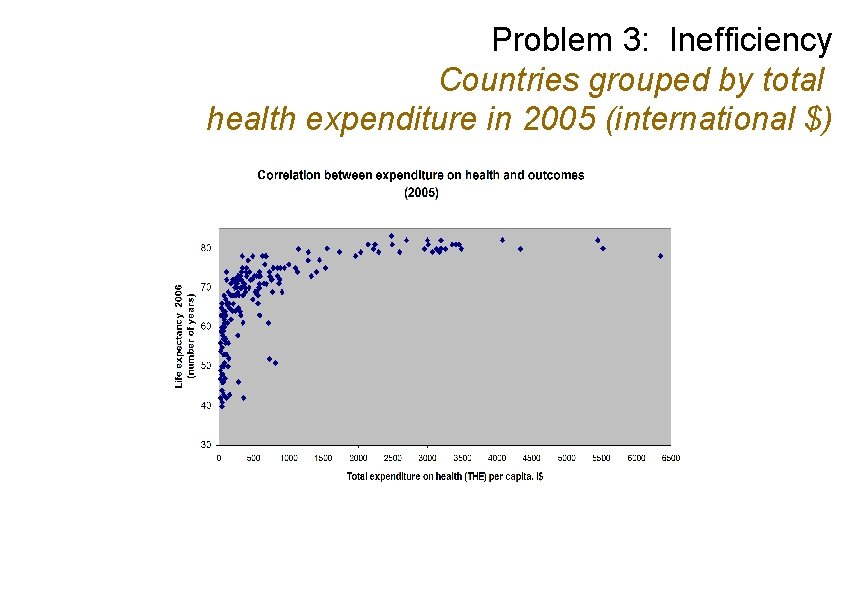
Problem 3: Inefficiency Countries grouped by total health expenditure in 2005 (international $)
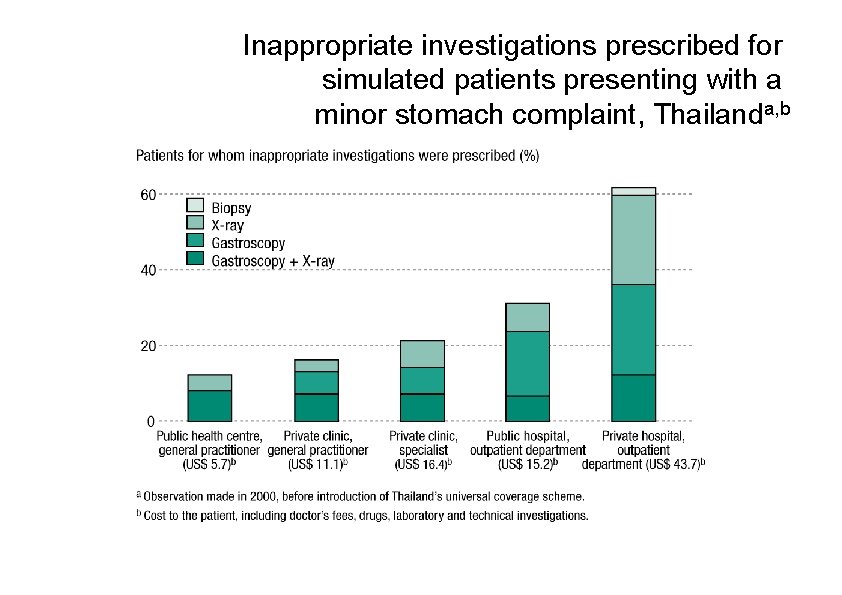
Inappropriate investigations prescribed for simulated patients presenting with a minor stomach complaint, Thailanda, b

Sources of Inefficiency 1. Technical inefficiency - waste 2. Allocative inefficiency - use of high cost, low effectiveness interventions when low cost, high effectiveness interventions are not (fully) implemented - "over spending" on hospitals versus other levels; high tech vs population based. 11 | Department of Health Systems Financing: Better Financing for Better Health
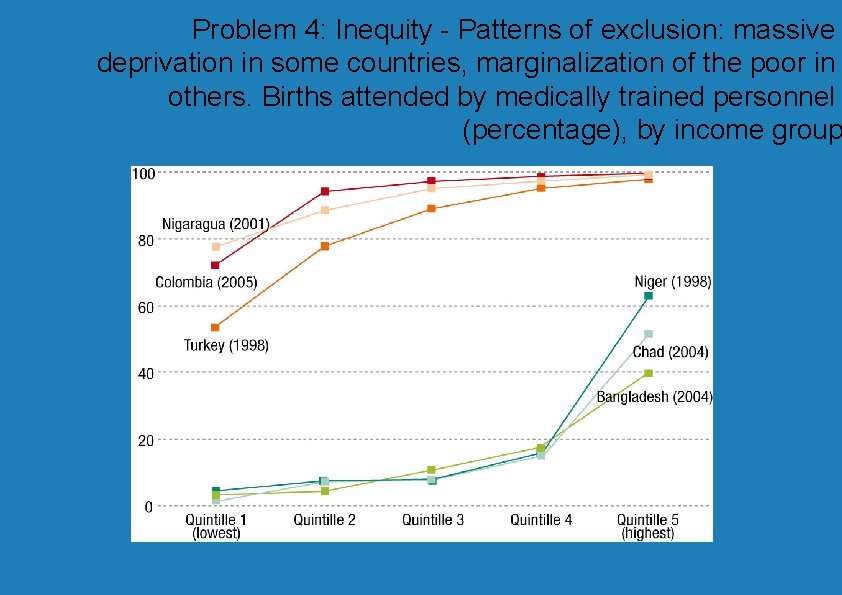
Problem 4: Inequity - Patterns of exclusion: massive deprivation in some countries, marginalization of the poor in others. Births attended by medically trained personnel (percentage), by income group

Responses v Raise more funds for health v Reduce reliance on out-of-pocket payments and increase pre-payment and pooling v Improve efficiency v Improve equity in raising and using resources 13 | Department of Health Systems Financing: Better Financing for Better Health

Link with NCDs? Some suggestions ü Raise money for health – how to position NCDs? Prevention? ü Ensure the "right interventions" are available to the population. When resources are scarce, which ones should be provided? 2 areas where economics can help in selection of interventions 1. Can interventions based on price incentives work? 2. What interventions should be given priority – economic consequences and cost-effectiveness 14 | Department of Health Systems Financing: Better Financing for Better Health

Economic Burden: What questions are we trying to answer? Level Question / topic Macro: Society 1. 2. 3. Micro: Households 1. 2. 15 | What impact does ill-health have on gross domestic product or its rate of growth? How much does society pay for medical and other expenses because of illness? What is the impact on social product (i. e. , both market and non-market consumption lost opportunities), or on social welfare more generally? What impact does ill-health have on a household's income or consumption patterns (over a single year, or for a longer period of time)? How much do households pay for medical or other expenses because of illness (for an episode, over a year, or over a lifetime)? Department of Health Systems Financing: Better Financing for Better Health

What questions are we trying to answer? (continued) Level Question / topic Micro (cont) 1. Firms 2. Government 1. 2. 16 | What impact does ill-health have on a firm's operating costs, output or profit? What is the impact of ill-health on productivity in the work place (including impaired performance while still at work, as well as absenteeism) ? What proportion of government expenditure could have been saved and directed to an alternative use in the absence of illness? (e. g. what social security payments could be avoided by the prevention of or cure for disease? ) What impact does ill-health have on the government workforce and on the government's ability to provide services? Department of Health Systems Financing: Better Financing for Better Health
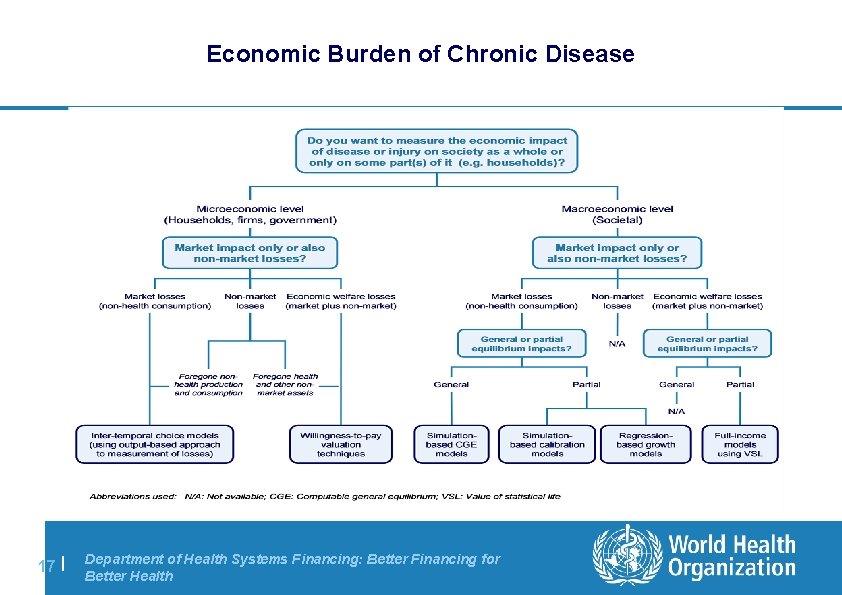
Economic Burden of Chronic Disease 17 | Department of Health Systems Financing: Better Financing for Better Health
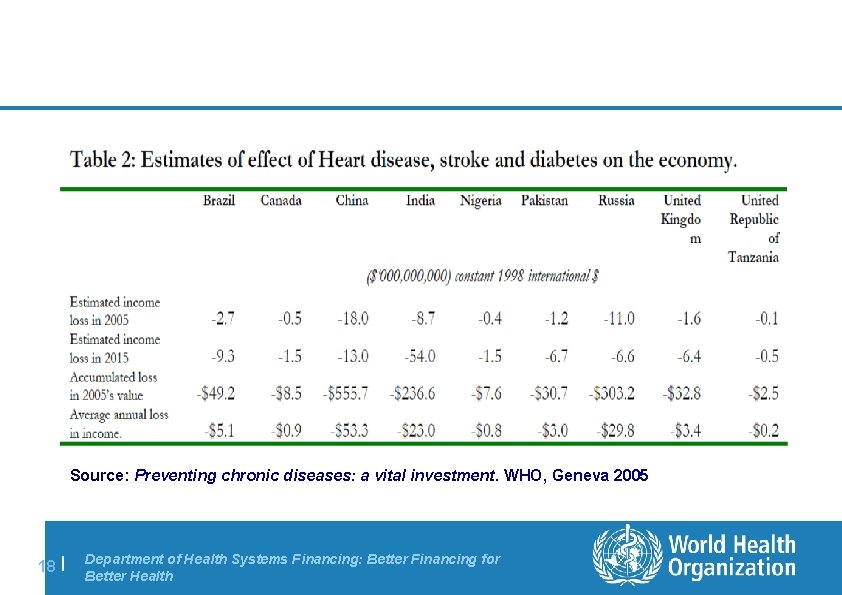
Source: Preventing chronic diseases: a vital investment. WHO, Geneva 2005 18 | Department of Health Systems Financing: Better Financing for Better Health
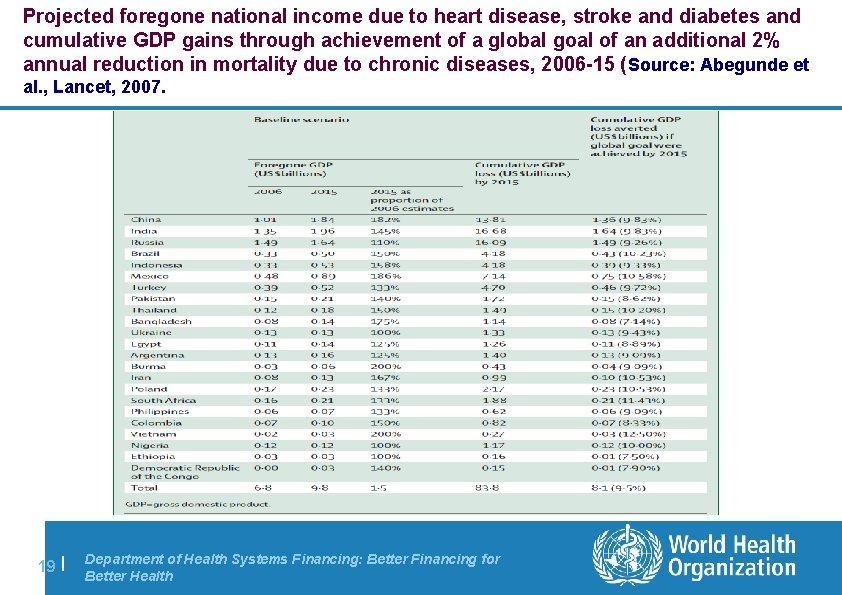
Projected foregone national income due to heart disease, stroke and diabetes and cumulative GDP gains through achievement of a global goal of an additional 2% annual reduction in mortality due to chronic diseases, 2006 -15 ( Source: Abegunde et al. , Lancet, 2007. 19 | Department of Health Systems Financing: Better Financing for Better Health
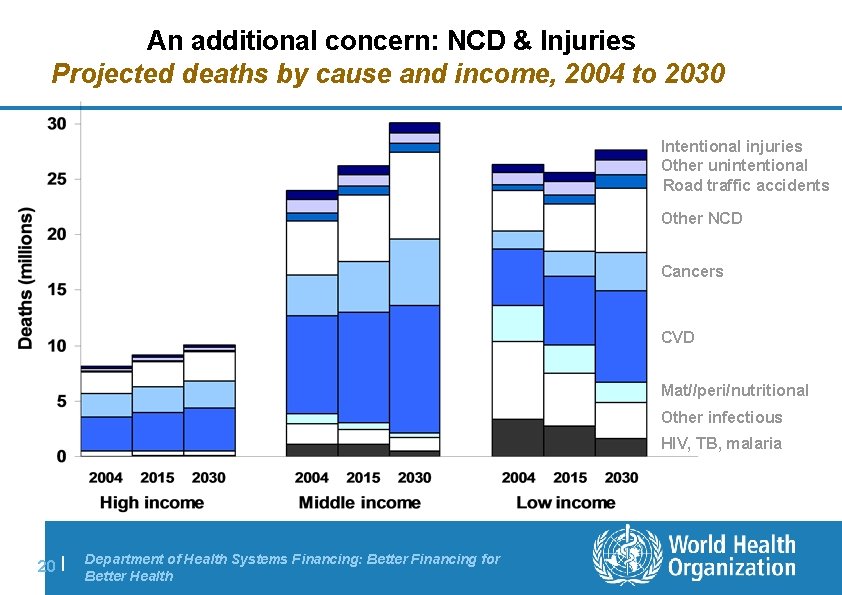
An additional concern: NCD & Injuries Projected deaths by cause and income, 2004 to 2030 Intentional injuries Other unintentional Road traffic accidents Other NCD Cancers CVD Mat//peri/nutritional Other infectious HIV, TB, malaria 20 | Department of Health Systems Financing: Better Financing for Better Health

Economic Burden of Chronic Disease: Examples 1. Abegunde D & A. Stanciole, "An estimation of the economic impact of chronic noncommunicable diseases in selected countries", WHO working paper, 2006 www. who. int/chp/working_paper_growth%20 model 29 may. pdf 2. Preventing chronic diseases: a vital investment. WHO, Geneva 2005 www. who. int/chp/chronic_disease_report/contents/en/index. html 3. D. O. Abegunde, C. D. Mathers, T. Adam, M. Ortegon, K. Strong. "The burden and costs of chronic diseases in low-income and middle-income countries", Lancet 370: 1921 -1938, 2007. 4. M. Suhrcke & D. Urban. "Are cardiovascular diseases bad for economic growth? ", Cesifo Working Paper No. 1845, November 2006. 21 | Department of Health Systems Financing: Better Financing for Better Health

Economic Burden of Chronic Disease: Methods 1. Evans, D. , T. Tan Torres Edejer, D. Chisholm, A. Stanciole. WHO Guide To Identifying the Economic Consequences of Disease and Injury, WHO, Geneva 2009. Published on line: http: //www. who. int/choice/publications/d_economic_impact_guide. pdf 2. Chisholm, D. , A. E. Stanciole, T. Tan Torres Edejer, D. B. Evans. "The economic impact of disease and injury: counting what matters", British Medical Journal (forthcoming). 22 | Department of Health Systems Financing: Better Financing for Better Health

WHO cost-effectiveness analysis of CVD prevention (Murray et al; Lancet, 2003) l Comparative, population-based, sector-wide approach, operationalised via the CHOICE project (CHOosing Interventions that are Cost-Effective; www. who. int/choice) – effectiveness: healthy years gained / DALYs averted over the lifetime of a population, with and without intervention(s) in place – resource costs: patient + programme level (international $) l Range of current and new/potential interventions assessed – personal: anti-hypertensive and ant-cholesterol drugs; poly-drug therapy / absolute risk approach – non-personal: salt (15 and 30% reduction); mass media to reduce cholesterol l Results summarised in WHO regional C-E databases – available for country-level adaptation / analysis 23 | Department of Health Systems Financing: Better Financing for Better Health
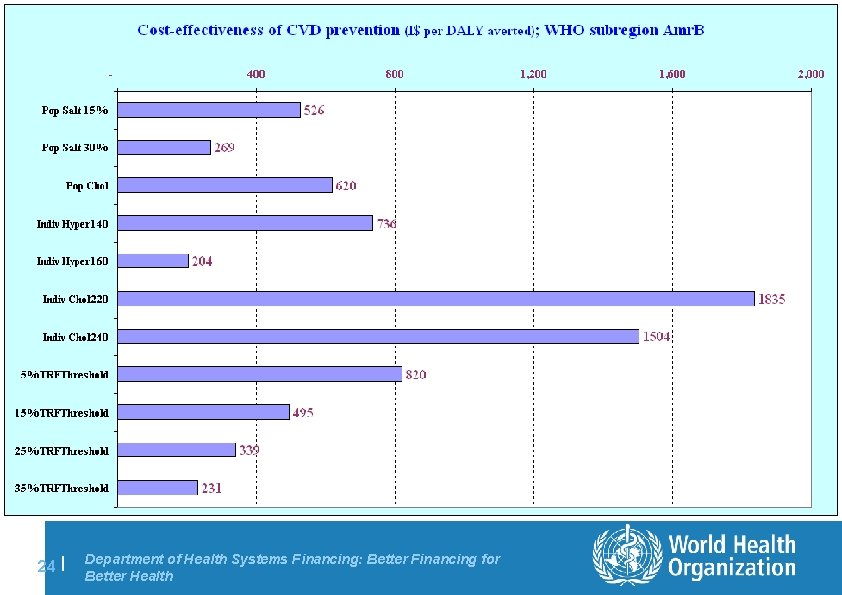
24 | Department of Health Systems Financing: Better Financing for Better Health
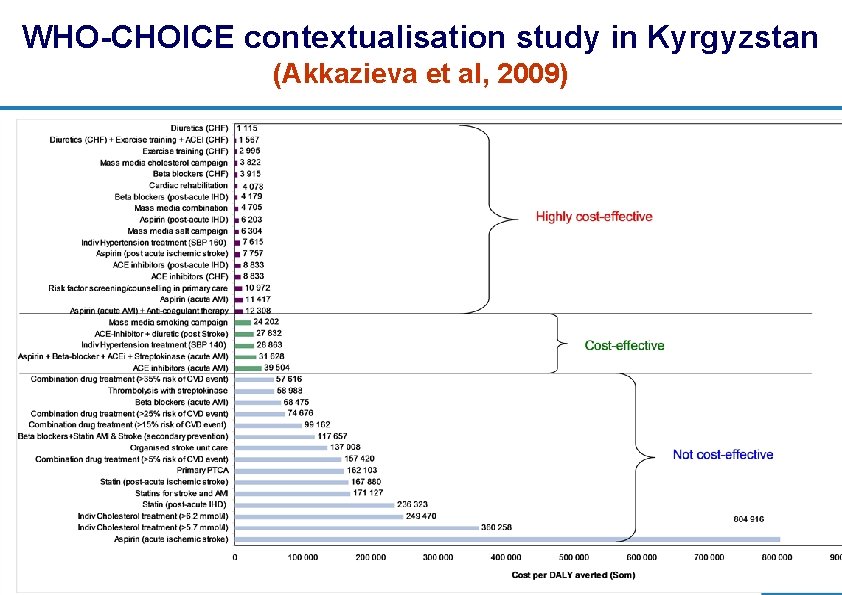
WHO-CHOICE contextualisation study in Kyrgyzstan (Akkazieva et al, 2009) 25 | Department of Health Systems Financing: Better Financing for Better Health
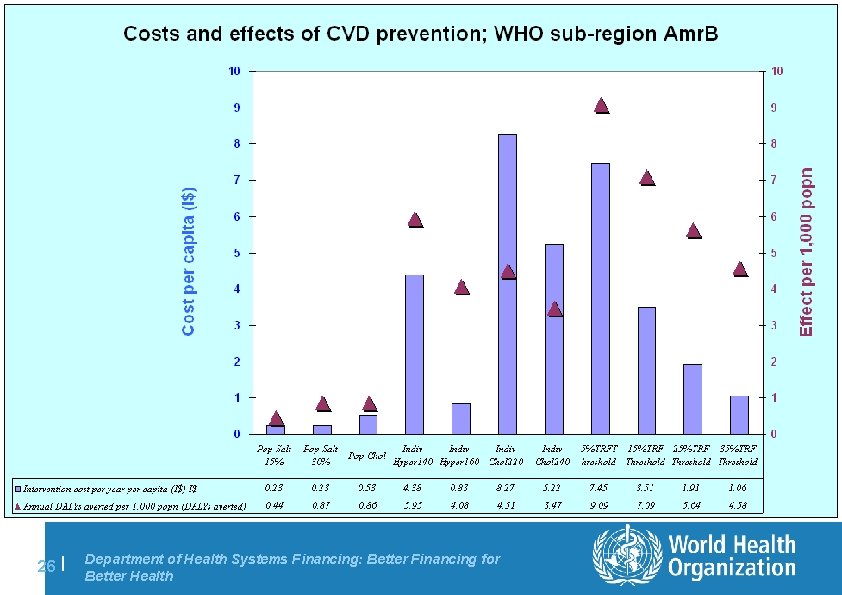
26 | Department of Health Systems Financing: Better Financing for Better Health
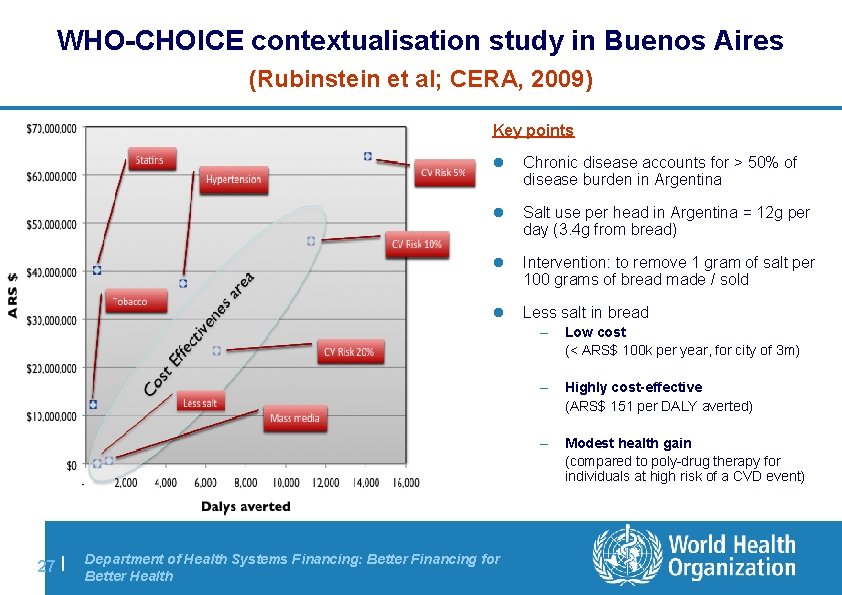
WHO-CHOICE contextualisation study in Buenos Aires (Rubinstein et al; CERA, 2009) Key points 27 | l Chronic disease accounts for > 50% of disease burden in Argentina l Salt use per head in Argentina = 12 g per day (3. 4 g from bread) l Intervention: to remove 1 gram of salt per 100 grams of bread made / sold l Less salt in bread Department of Health Systems Financing: Better Financing for Better Health – Low cost (< ARS$ 100 k per year, for city of 3 m) – Highly cost-effective (ARS$ 151 per DALY averted) – Modest health gain (compared to poly-drug therapy for individuals at high risk of a CVD event)
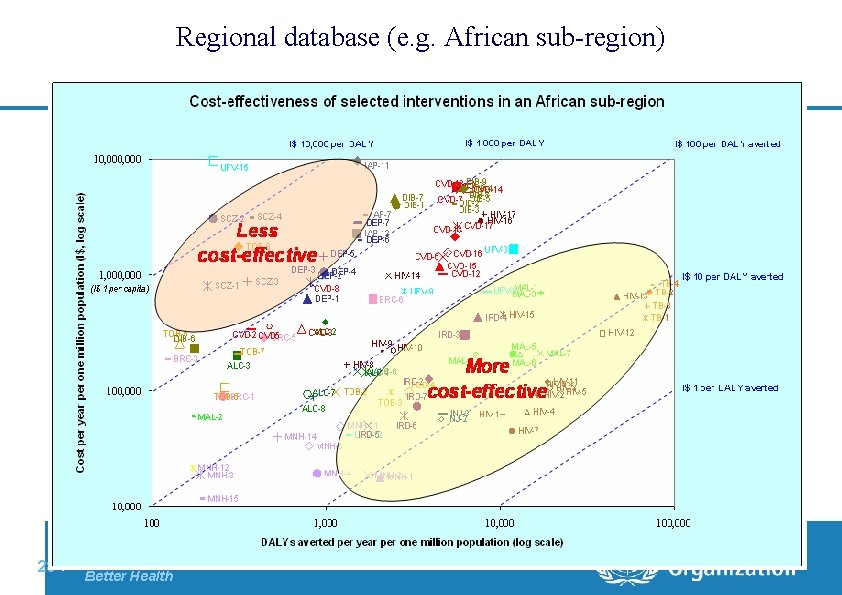
Regional database (e. g. African sub-region) 28 | Department of Health Systems Financing: Better Financing for Better Health
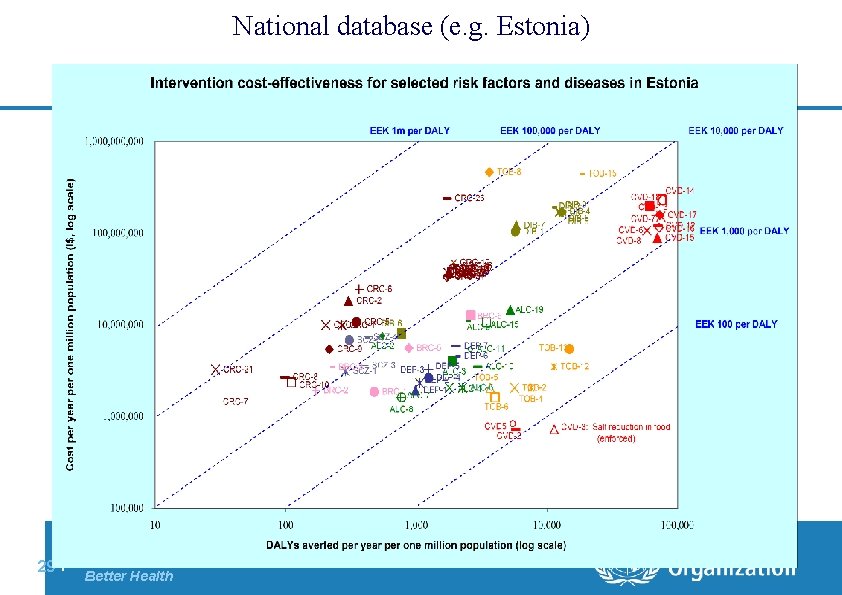
National database (e. g. Estonia) 29 | Department of Health Systems Financing: Better Financing for Better Health

Conclusions 30 | Department of Health Systems Financing: Better Financing for Better Health
Spare slides 31 | Department of Health Systems Financing: Better Financing for Better Health
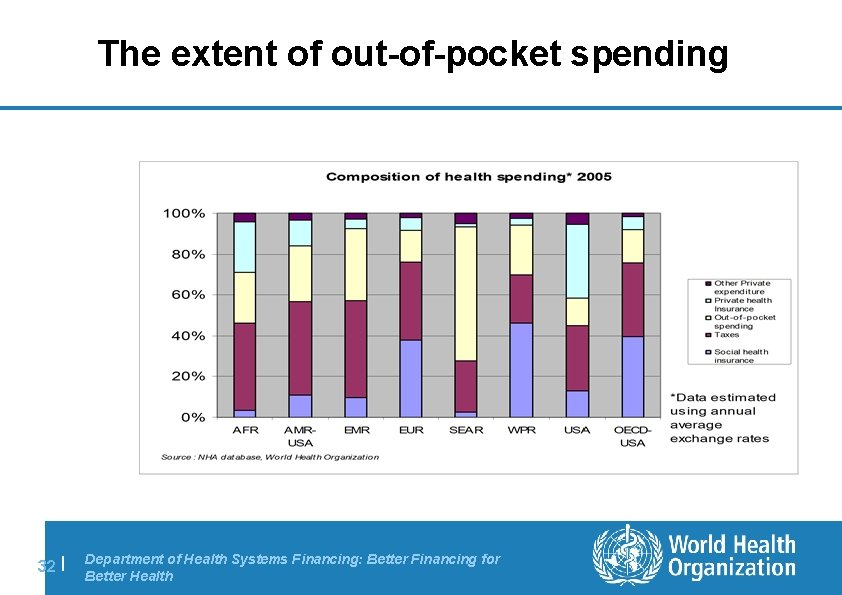
The extent of out-of-pocket spending 32 | Department of Health Systems Financing: Better Financing for Better Health

Strategy 4: Safety Net Review l Specific policies ð Conditional cash transfers subject to fulfilling certain conditions (e. g. vaccinations) ð Vouchers, e. g. to better access health services ð Waivers and exemptions l Policies integrating the poor ð Universal provision of health services (UK) ð Explicit inclusion of the poor in social health insurance (e. g. France, Mexico, Thailand, Colombia, Chile) 33 | Department of Health Systems Financing: Better Financing for Better Health
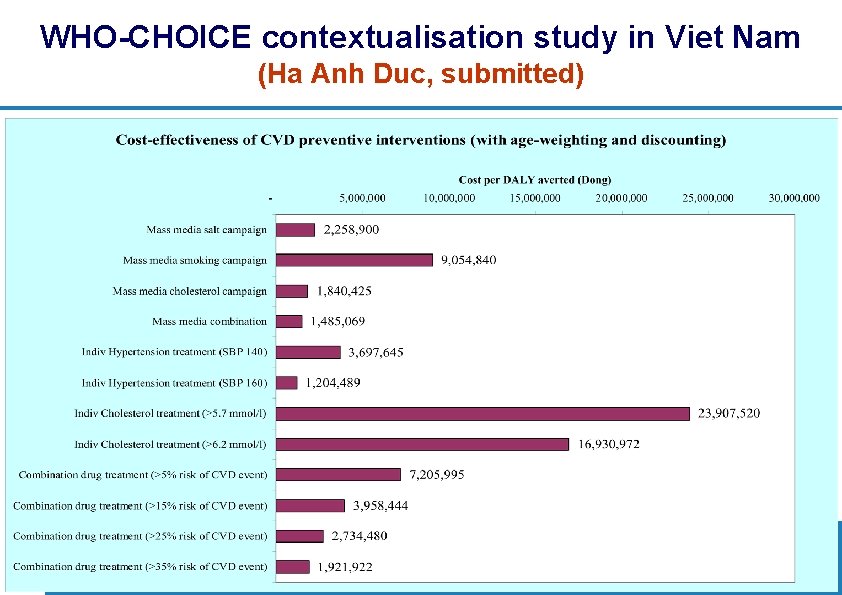
WHO-CHOICE contextualisation study in Viet Nam (Ha Anh Duc, submitted) 34 | Department of Health Systems Financing: Better Financing for Better Health
- Slides: 34