Ecological Correlates of Obesity and Related Health Behaviors


Ecological Correlates of Obesity and Related Health Behaviors among Adults Living in Rural Areas of South Carolina Demetrius Abshire Ph. D, RN Abbas Tavakoli Dr. PH

What is the biggest barrier to promoting weight loss for people who live in rural areas?

“When environmental conditions exercise powerful constraints on behavior, they emerge as the overriding determinants. ” Albert Bandura Sallis. 2018. Health Education & Behavior, 45(5), 661 -7.
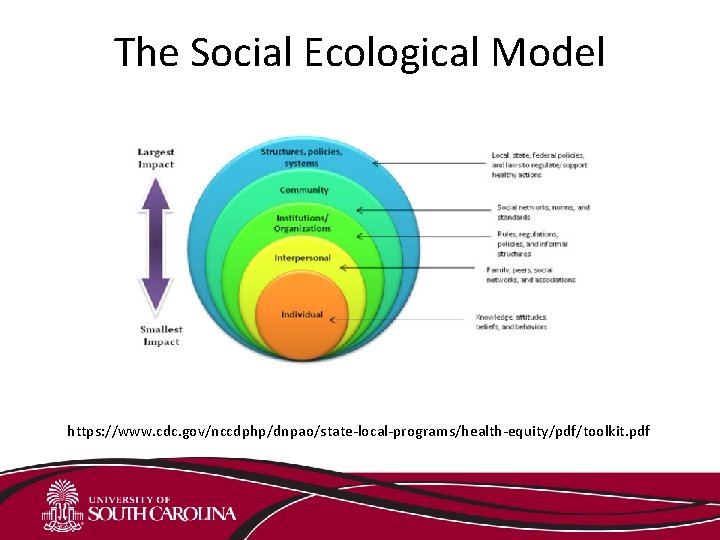
The Social Ecological Model https: //www. cdc. gov/nccdphp/dnpao/state-local-programs/health-equity/pdf/toolkit. pdf

Promoting Healthy Behaviors in Rural Areas • Environmental Constraints 1 -3 • Limited/poor public transportation • Limited options for healthier foods • Physical activity infrastructure lacking • Safety concerns • “Positive Deviants” 4 • Engaging in healthy behaviors despite constraints • The home environment and motivation are key 1. 2. 3. 4. Morgan et al. 2016. BMC Public Health, 16, 305. Bolin et al. 2015. J Rural Health, 31(3), 326 -33. Frost et al. 2010. Am J Health Promot, 24, 267 -83. Kegler et al. 2013. J Primary Prevent, 34, 5 -15.

The Social Ecological Model in Rural Areas • Healthy Rural Communities 2 (Home & Neighborhood) • Only perceived neighborhood access to healthy food had a direct effect on BMI • Factors positively associated with F/V and fat intake – Household inventory of FVs, family support for FV intake, household inventory of fatty foods • Factors associated with PA – More PA equipment, higher family support, higher selfefficacy • No direct effect between fat and FV intake with BMI Kegler et al. 2014. Prev Sci, 15, 1 -11
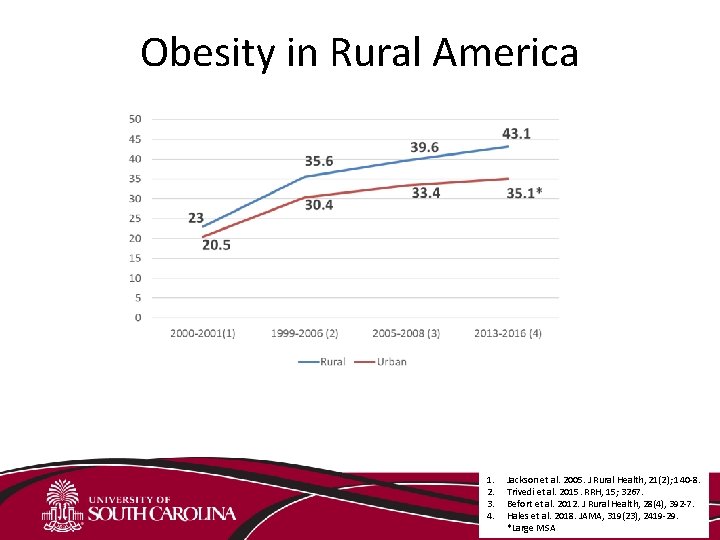
Obesity in Rural America 1. 2. 3. 4. Jackson et al. 2005. J Rural Health, 21(2); 140 -8. Trivedi et al. 2015. RRH, 15; 3267. Befort et al. 2012. J Rural Health, 28(4), 392 -7. Hales et al. 2018. JAMA, 319(23), 2419 -29. *Large MSA

Methods • Cross-sectional survey of rural (n=201) and urban (n=228) dwelling South Carolina adults • Survey Sampling International • Self-reported height and weight • Environmental perceptions for PA, self-efficacy, social support, beliefs regarding diet and exercise – http: //sallis. ucsd. edu/ University of Wisconsin Population Health Institute. County Health Rankings & Roadmaps 2018. www. countyhealthrankings. org.
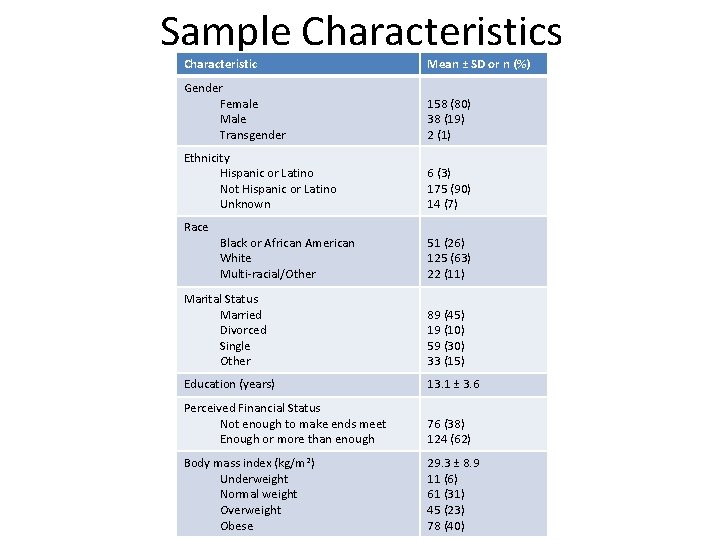
Sample Characteristics Characteristic Mean ± SD or n (%) Gender Female Male Transgender 158 (80) 38 (19) 2 (1) Ethnicity Hispanic or Latino Not Hispanic or Latino Unknown 6 (3) 175 (90) 14 (7) Race Black or African American White Multi-racial/Other 51 (26) 125 (63) 22 (11) Marital Status Married Divorced Single Other 89 (45) 19 (10) 59 (30) 33 (15) Education (years) 13. 1 ± 3. 6 Perceived Financial Status Not enough to make ends meet Enough or more than enough 76 (38) 124 (62) Body mass index (kg/m 2) Underweight Normal weight Overweight Obese 29. 3 ± 8. 9 11 (6) 61 (31) 45 (23) 78 (40)

Results Hierarchical linear regression for predictors of BMI (coefficients shown for Step 4) Step Variable B (SE) t-value p-value R 2 1 Intercept 34. 79 (5. 82) 5. 98 <. 01 0. 04 Education -0. 41 (0. 24) -1. 71 0. 09 Age 0. 11 (0. 06) 1. 96 0. 05 Gender 1. 98 (1. 90) 1. 04 0. 30 Black 3. 31 (1. 74) 1. 90 0. 06 Multi-racial 3. 48 (2. 65) 1. 31 0. 19 2 Self-efficacy (sticking to diet) -0. 18 (0. 12) -1. 42 0. 16 0. 08 3 Seeing others walk or jog -0. 82 (0. 63) -1. 30 0. 20 0. 10 4 Home environment PA supports -0. 33 (0. 19) -1. 74 0. 08 0. 12
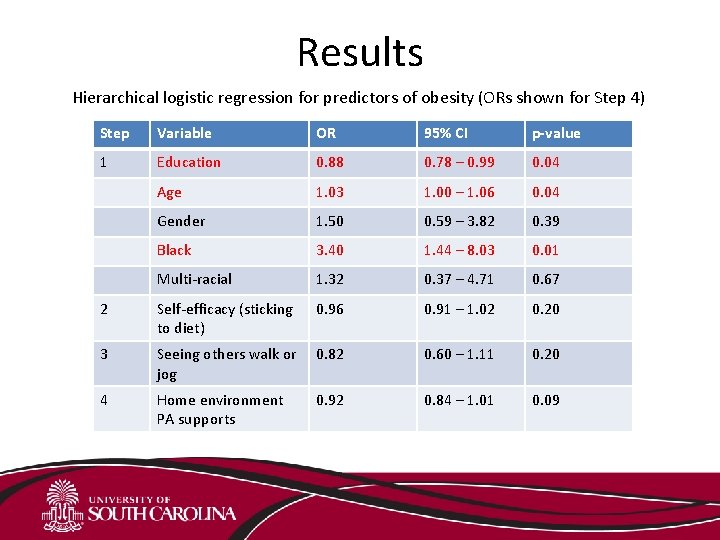
Results Hierarchical logistic regression for predictors of obesity (ORs shown for Step 4) Step Variable OR 95% CI p-value 1 Education 0. 88 0. 78 – 0. 99 0. 04 Age 1. 03 1. 00 – 1. 06 0. 04 Gender 1. 50 0. 59 – 3. 82 0. 39 Black 3. 40 1. 44 – 8. 03 0. 01 Multi-racial 1. 32 0. 37 – 4. 71 0. 67 2 Self-efficacy (sticking to diet) 0. 96 0. 91 – 1. 02 0. 20 3 Seeing others walk or jog 0. 82 0. 60 – 1. 11 0. 20 4 Home environment PA supports 0. 92 0. 84 – 1. 01 0. 09

Discussion/Conclusion • Individual, social, and environmental factors correlated with BMI were not predictive of BMI/obesity in multivariable models. • Sociodemographic factors have a significant influence on BMI/obesity. • Next steps: Ecological correlates of behavior • Limitation: Small sample size (interpret findings with caution)

THANK YOU! QUESTIONS, COMMENTS, AND DISCUSSION Demetrius Abshire, Ph. D, RN abshired@mailbox. sc. edu 803 -576 -6262
- Slides: 14