EBOLA VIRUS DISEASE Presented By Dr Zahra Doosti

EBOLA VIRUS DISEASE Presented By: Dr. Zahra Doosti


Ebola virus disease confined to well-defined geographic areas: Guinea, Liberia, Sierra Leone, Nigeria (Lagos and Port Harcourt only), Democratic Republic of Congo (Equateur province)

Ebolavirus species: • Zaire ebolavirus: 1976, Democratic Republic of Congo. • Sudan ebolavirus: 1976, Sudan. • Bundibugyo ebolavirus: 2007, Uganda. • Taї Forest ebolavirus (formerly Côte d’Ivoire ebolavirus): 1994, Ivory Coast. • Single case, veterinary worker handling primate. • Reston ebolavirus: 1989, Philippines. • Macaques, swine. • Human laboratory workers seropositive but no clinical disease.
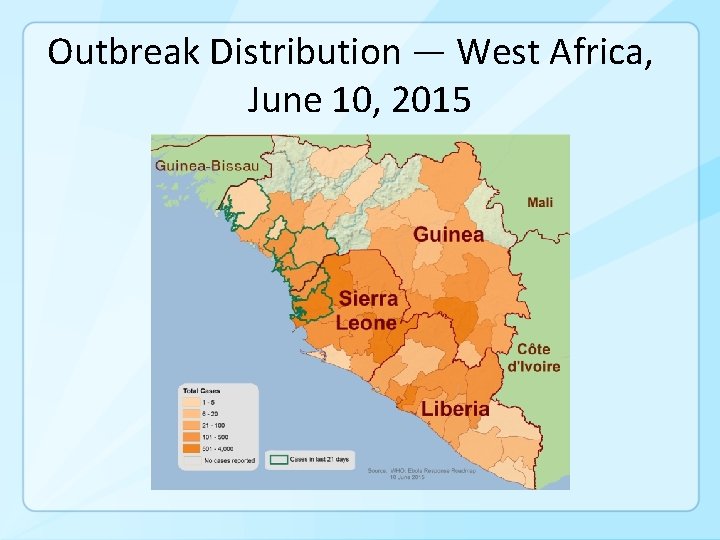
Outbreak Distribution — West Africa, June 10, 2015

Ebolavirus virion • Genome 19 kb long. • Diameter 80 nm; length 960 nm to 1200 nm. • Four viral proteins: polymerase (L), nucleoprotein (NP), and proteins VP 35 and VP 30. • Spikes formed by GP 1/GP 2 complexes (envelope glycoprotein) • VP 24 (membrane protein) associated with envelope • Secretory GP: binds to antibody, possible antineutrophil activity.


Reservoir and transmission to humans: • Fruit bats reservoir of virus - Drop partially eaten fruits • Bats infect chimpanzees, gorillas, forest antelopes, porcupines • Humans handle and eat bush meat (bats, chimpanzees, gorillas) • Infected human passes from person to person • Centers for Disease Control and Prevention; Virus Ecology Graphic (http: //www. cdc. gov/vhf/ebola/resources/virusecology. html )
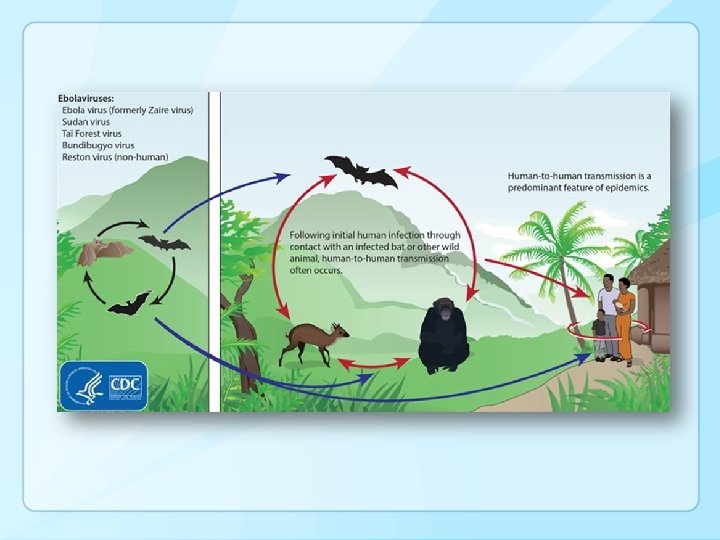

Pathogenesis of Ebola - transmission • Among 173 household contacts of 27 patients with confirmed Ebola, the transmission rate was only 16% despite none of the standard infection control precautions routinely employed in U. S. hospitals being used • Of 78 contacts who reported no physical contact with the infected patient, none became infected • Among those who did have physical contact, risk for Ebola was highest after contact with the patients’ blood • Large HCW transmission in Sierra Leone associated with infected woman in labour

Pathogenesis - transmission • Fastest incubation period has been reported associated with needle stick injury. • Viral load may correlate with disease severity and survival • This is NOT an airborne disease. Thus the pulmonary disease is hemorrhage and ARDS associated with severe sepsis.

Pathogenesis - how does Ebola cause disease? • Virus enters the body via infected blood/body fluid in contact with a mucosal surface or a break in intact skin. • Virus replicates preferentially in monocytes/macrophages and dendritic cells which facilitate dissemination of the virus throughout the body via lymphatic system. • Other cells are secondarily infected and there is rapid viral growth in hepatocytes, endothelial and epithelial tissues. • There is strong cytokine/inflammatory mediator release of TNF-a and inflammatory cascade.

Pathogenesis - inflammatory response • Leads to endothelial damage, increased vascular permeability and shock. • This results in the end organ damage and multiorgan dysfunction • Diffuse intravascular coagulopathy(DIC) with platelet and coagulation factor consumption which leads to hemorrhage. • Ig. M starts forming in 2 day and Ig. G in 5 -8 days post infection. Immunologic response correlates with survival. • Thus the observation that those who live >1 week are more likely to survive.
Clinical Manifestations: • Incubation period 8 -10 days (range 2 -21) • Sudden onset of Fever >38. 6 • Flu-like symptoms: chills, myalgias, and malaise, sore throat • Nausea, vomiting , abdominal pain, diarrhea • Respiratory symptoms of chest pain, shortness of breath and cough • CNS symptoms: Headache, confusion and coma

Clinical Manifestations: • Rash occurs around day 5 • Hypotension, peripheral edema • Bleeding manifestations develop in >50% (internal/external) • Can vary from petechiae& easy bruising, to mucosal hemorrhage, uncontrolled bleeding and massive GI blood loss • Multi-organ dysfunction : kidneys and Liver • Laboratory abnormalities • Thrombocytopenia and leukopenia • Elevated transaminases (AST > ALT), amylase, D-dimer • Reduced albumin



Other possible infectious causes of symptoms: - Malaria - typhoid fever - Meningococcemia - Lassa fever - other bacterial infections (e. g. , pneumonia) – all very common in Africa

Laboratory Findings • Thrombocytopenia (50, 000– 100, 000/m. L range) • Leukopenia followed by neutrophilia • Transaminase elevation: elevation serum aspartate amino-transferase (AST) > alanine transferase (ALT) • Electrolyte abnormalities from fluid shifts • Coagulation: PT and PTT prolonged • Renal: proteinuria, increased creatinine

Immunity and Survival • Treatment is supportive care • Ig. G response appears to be protective • Survivors may have persistent high antibody titres and associated sequelae of hepatitis, uveitis, muscle weakness etc. • Previous observation was that serum from an Ebola survivor was therapeutic • Anecdotal reports of Mab therapy being successful • Caution, in a disease with 50% survival, any anecdotal observation can be a chance event • It does support the potential role of vaccination


Screening tools: • Screening for travel to affected country/area and presence of symptoms Recommended action for: • Primary health care providers • Emergency departments – algorithm • Community laboratories • Dental and allied health care professional offices • Emergency medical services • Communications to post-secondary schools

For EVD: Droplet + Contact Precautions: Patient accommodation: • Single room with dedicated bathroom (minimum requirement); door closed • Consider use of an isolation room that has an anteroom for donning or doffing PPE for all staff entering the room: • fluid-resistant, long-sleeved, cuffed gown • gloves • full face protection (face shield) • surgical or procedure mask • Maintain log of all individuals entering the room; only essential people should enter the room.

Risk Assessment for EVD • Use risk assessment to determine the need for additional PPE; as the patient’s condition changes, the risk to HCPs may change. • The procedure being performed and the presence of clinical symptoms impacts the decision of what PPE to wear. Clinical risks may include: • Large amounts of blood/body fluids: foot/leg coverings, head coverings, waterproof gowns, or biohazard suits • Aerosol generating procedures: N 95 respirators • Phlebotomy: double gloves • Ensure adequate training before adding unfamiliar PPE

Diagnostic tests: Reverse Transcriptase PCR (RT-PCR) • Used to diagnose acute infection • More sensitive than antigen detection ELISA • Identification of specific viral genetic fragments • Performed in select CLIA-certified laboratories RT-PCR sample collection Volume: minimum volume of 4 m. L whole blood Plastic collection tubes (not glass or heparinized tubes) Whole blood preserved with EDTA is preferred Whole blood preserved with sodium polyanethol sulfonate (SPS), citrate, or with clot activator is acceptable

Virus isolation • Requires Biosafety Level 4 laboratory; • Can take several days Immunohistochemical staining and histopathology • On collected tissue or dead wild animals; localizes viral antigen Serologic testing for Ig. M and Ig. G antibodies (ELISA) • Detection of viral antibodies in specimens, such as blood, serum, or tissue suspensions • Monitor the immune response in confirmed EVD patients

** Repeat laboratory testing on day 4 of fever **

Some Important points: • Ebola virus is only present in blood after onset of fever. • It may take up to 4 days after fever onset for Ebola virus PCR to be positive, So Repeat laboratory testing on day 4 of fever. • If initial testing was done within 4 days of onset of fever, testing should be repeated on day 4 if clinical suspicion is still present.


Post-exposures prophylaxis / treatment Zmapp: Three monoclonal antibodies against parts of the glycoprotein • Grown in tobacco plants • Suppress viremia and viral spread • Effective in non-human primates – 3 doses starting on day 3 to 5 • Post-exposure, used in seven people - 2 of 7 died

Post-exposure prophylaxis Tekmira Small interfering RNAs • Formulated in stable nucleic acid lipid particle (SNALP) • Inhibits the replications of the virus • Post-exposure prophylaxis in non-human primates given in multiple doses (30 minutes after infection and then either day 1, 3 and 5 or daily for 6 days) • Tested in humans, put on hold then released • Also a Marburg variety

Post-exposure prophylaxis / treatment BCX-4430 – Bio. Cryst Pharmaceuticals • Small molecule • Adenosine analogue, inhibits viral RNA polymerase function • Broad antiviral inhibitor 20 viruses • Within 48 hours after exposure and then twice daily for 14 days Favipiravir - Fujifilm • Small molecule, nucleotide analogue • Targets the polymerase to stop viral replication; Effective 6 days post infection • Approved to treat influenza in Japan • Sarepta • Binds to viral RNA and stops replication

Vaccines VSV-EBOV 1 - Public Health Agency of Canada • Recombinant vesicular stomatitis virus • Replace glycoprotein with Ebola – Zaire , Ebola - Sudan or Marburg • Live vaccine; single dose • Pre-exposure and possibly post-exposure – used in one laboratory worker • Canada donating 800 -1000 doses • Glaxo. Smith. Kline/National Institute of Allergy and Immunology 2 • Combined with chimp adenovirus 3 • Bivalent – Zaire and Sudan, Univalent – Zaire • Inactivated vaccine; single dose ? ?

Patients who survive often have signs of clinical improvement by the second week of illness … • Associated with the development of virus-specific antibodies • Antibody with neutralizing activity against Ebola persists greater than 12 years after infection Prolonged convalescence: • Includes arthralgia, myalgia, abdominal pain, extreme fatigue, and anorexia; many symptoms resolve by 21 months • Significant arthralgia and myalgia may persist for >21 months • Skin sloughing and hair loss has also been reported

Transmission by semen: • Up to 82 days after disease onset. • At least 7 weeks after recovery • Consensus: safe sex for at least 3 months after recovery. (in some references up to 6 months)



Key Ebola Virus Disease Facts • Only spread by direct contact with blood and body fluids; not airborne • Incubation 2 -21 days; usually 8 -10 days • Only infectious when symptomatic • Increasingly infectious as get sicker

Perspectives on risk assessment: • Ebola virus disease confined to well-defined geographic areas: Guinea, Liberia, Sierra Leone, Nigeria (Lagos and Port Harcourt only), Democratic Republic of Congo (Equateur province) • Most infected individuals likely to have known exposures (not unrecognized exposures) • Most infected individuals, other than aid and health care workers, not likely to travel to Ontario • Common things are common: Malaria, typhoid fever, influenza, meningococcal, much more likely diagnoses

Thanks for attention
- Slides: 40