EBOLA VIRUS DISEASE Perspective of Both a Clinician

EBOLA VIRUS DISEASE: Perspective of Both a Clinician and a Suspect Case Lewis Rubinson MD, Ph. D Director, Critical Care Resuscitation Unit R Adams Cowley Shock Trauma Center Associate Professor of Medicine University of Maryland School of Medicine

RELEVANT DISCLAIMERS AND DISCLOSURES Site PI (Univ of MD) and Protocol Comm Co-Chair for a US DHHS FDA/BARDA contract for the United States Critical Illness and Injury Trials Group Program in Emergency Preparedness Scientific Advisory Board member for Glaxo. Smith. KLine and Phillips/Respironics Received honoraria and travel support from academic and public health professional societies. Subcontractor to ICF international for an Ebola preparedness effort for the US DHHS Office of the Assistant Secretary for Preparedness and Response World Health Organization consultant clinician in Sierra Leone. This talk has not been approved by the WHO and should not be considered to express any official policies or information releases. The details and opinions expressed are only my own.

EBOLA VIRUS HISTORY 20+ documented outbreaks after 1 st identified outbreak in 1976 – Largest previous outbreak in Gulu, Uganda (2000) with 425 documented human cases Public health and community-initiated measures controlled past outbreaks – Early case finding/ contact tracing, early isolation, case management (healthcare), and proper mgmt of dead bodies
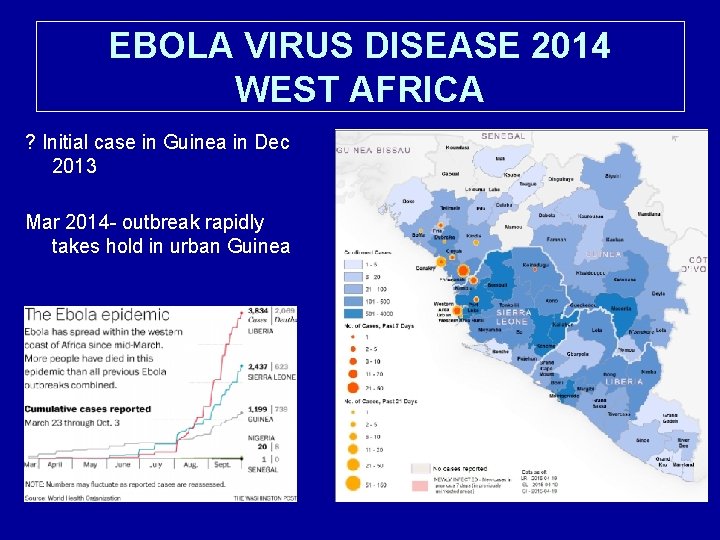
EBOLA VIRUS DISEASE 2014 WEST AFRICA ? Initial case in Guinea in Dec 2013 Mar 2014 - outbreak rapidly takes hold in urban Guinea

WHAT WAS PROVEN ABOUT EVD CLINICAL CARE BEFORE 2014? Prior clinical guidance based on limited data and care in very challenging environments Oral vs parenteral fluid resuscitation was opinion-based – Driven from cholera experience, but N/V and mental status issues may make different – Amount of fluid is controversial Addl supportive care regimens were opinion-derived and controversial when compared to modern critical care knowledgebase – Nutrition (? Importance, timing, amount)

SUMMER PRE-DEPLOYMENT DUE DILIGENCE • Responding to disasters for nearly 15 years (mostly US-based) – • Background in biosecurity – – – • Security, accountability, logistics, medical pre-screening, vaccinations and malaria proph, life/disability insurance Had served on VHF WGs over past decade Read everything I could about EVD and brushed up on trop med Reached out to USG, WHO and other colleagues with boots on ground clinical knowledge and situational awareness to better ready myself Self-directed crash course in Sierra Leone history, culture, politics, security situation and geography – Kenema Government Hospital
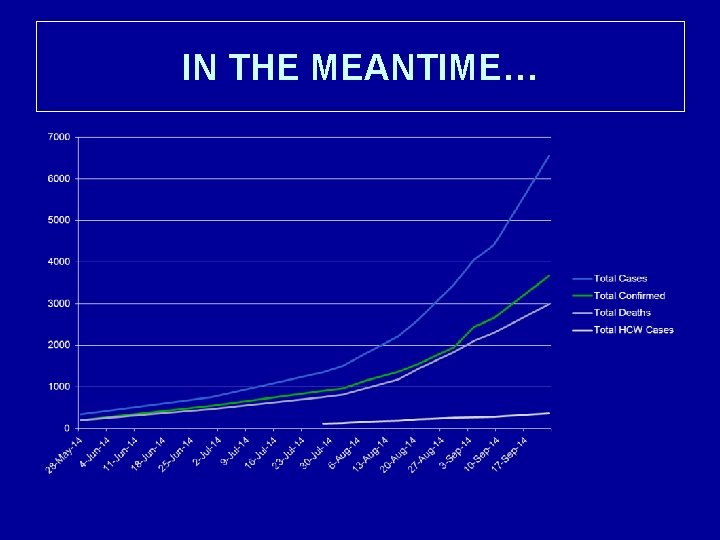
IN THE MEANTIME…
WHERE IS SIERRA LEONE?
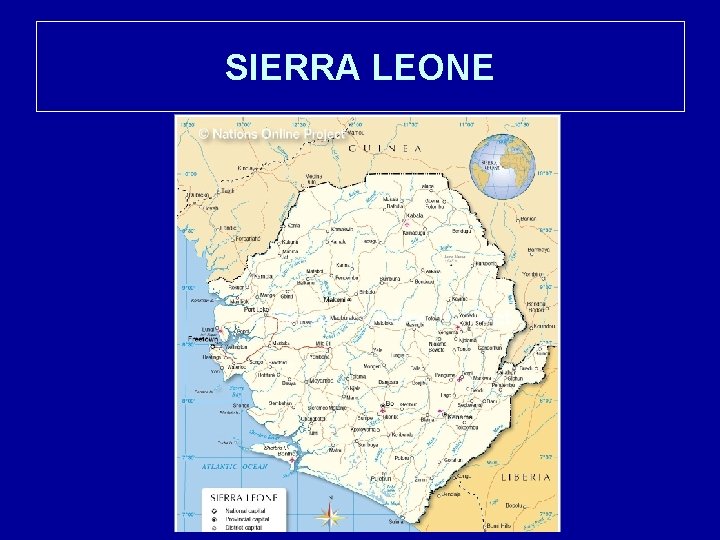
SIERRA LEONE

SIERRA LEONE Decade long civil war ended in 2002 GDP ~ $4 billion (2012) Approx 6 million people – – – > 40% 0 -14 years old Life expectancy < 50 y/o ~ 100 physicians for country prior to EVD Worst maternal mortality in world (2000) Literacy rate ~ 35% Minerals are major resources (diamonds, bauxite, gold)

TRAVELING TO KENEMA • • • Flights scheduled, cancelled and routes changed Baltimore to Phila, to Paris, to Nouakchott, Mauritania to Conakry, Guinea—UNHAS flight to Freetown, SL Due to flight changes no visa for Guinea – – – • In custody for several hours (language barrier) until Visa approved Luggage did not arrive At hotel, learned from email that MD I was to replace in Kenema has been med evac for EVD UNHAS flight following day, no water taxis running to Freetown since no commercial aircraft – 4 hr delay getting ground trans and 5+ hr drive to Freetown

STILL TRAVELING TO KENEMA • Promed and email traffic chatter that pts are stacking up at referring facilities since US MD was evacuated Kenema • UN security briefing, WHO mission brief, skipped the bank • Still no luggage. Given a bottle of hand sanitizer from WHO communications lead – “You’re going to Kenema, you will need it more than me” • 5 hr drive to Kenema

WEST AFRICA: BASELINE Courtesy CDR James Lawler

MAJOR PILLARS OF EVD CONTROL 1. Contact tracing and case finding 1. Early isolation 1. Clinical care 1. Safe treatment of the dead

ARRIVAL AT KENEMA GOVERNMENT HOSPITAL Only dedicated Lassa ward in the world ~30 + HCW infections, nearly 20 died ETU referral center for western/central SL No SL physicians working in ETU Since Dr. Crozier illness and evac, no clinical oversight in ETU Unknown census

LEARNING FROM THE EXPERTS I was clinical lead for KGH but team effort to make KGH function. WHO team responsible for elements of patient care when I arrived Frederique Jacquerioz (trop med, Lassa expert, EVD experience in Guinea) Suzanne Donovan (IC physician from LA, very thoughtful about PPE) Dario Gramuglia (logisitician, EVD experience with MSF) Rebecca Stretch (IC nurse, tons of EVD experience with month experience at KGH) Henry Kyobe Bosa (Ugandan physician with significant EVD outbreak experience) PLEASE SHOW ME HOW TO STAY SAFE!!

HOW IS AND WHEN IS EBOLA TRANSMITTED? EVD is transmitted from infectious body fluids entering your body (through mucus membranes or skin breaks) Sicker people with more symptoms have production of larger volumes of body fluids (emesis, diarrhea) ---typically more infectious – Most of these people are too symptomatic to be out and about – Close contacts at home who are caring for these people or sharing bathrooms, etc – Healthcare workers…in US especially ICU workers (intensity of exposure and duration of exposure) • 450 HCWs infected as of Oct 2014 Fomite transmission less likely but depends on ambient conditions Airborne transmission unconfirmed but aerosolization with projectile vomiting, therapeutic interventions, flushing of toilet with large infectious burden of stool all plausible
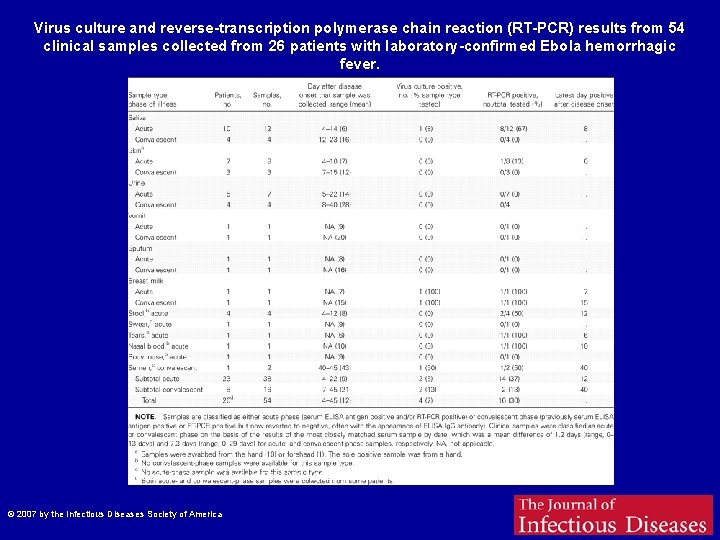
Virus culture and reverse-transcription polymerase chain reaction (RT-PCR) results from 54 clinical samples collected from 26 patients with laboratory-confirmed Ebola hemorrhagic fever. Bausch D G et al. J Infect Dis. 2007; 196: S 142 -S 147 © 2007 by the Infectious Diseases Society of America
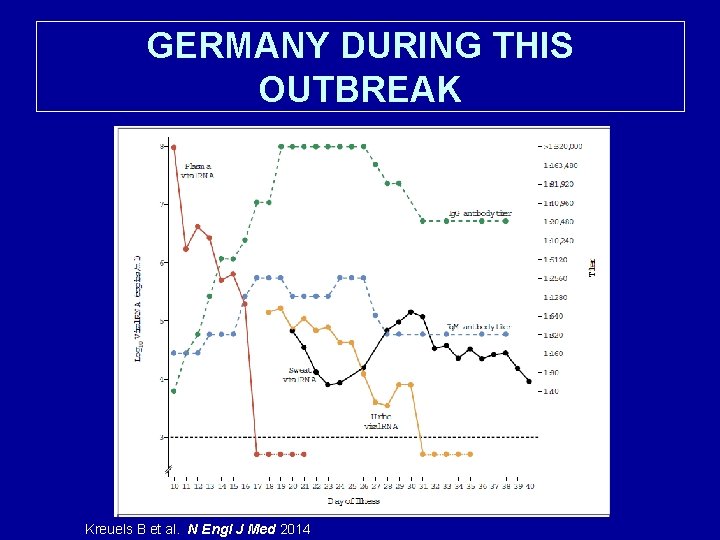
GERMANY DURING THIS OUTBREAK Kreuels B et al. N Engl J Med 2014
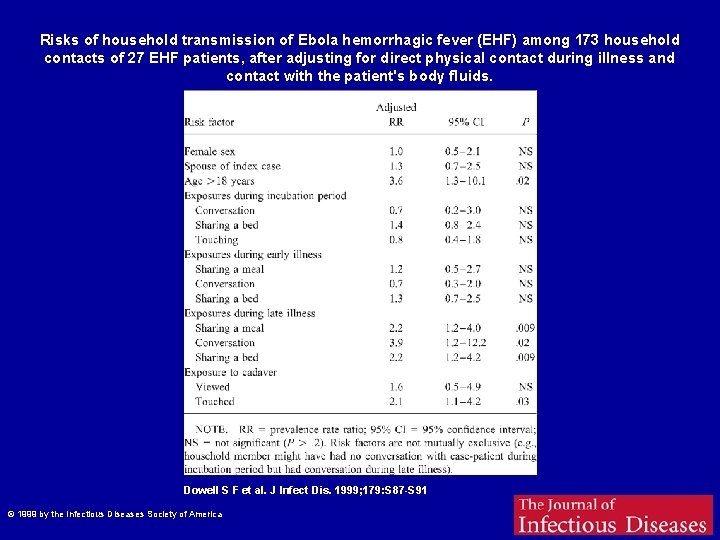
Risks of household transmission of Ebola hemorrhagic fever (EHF) among 173 household contacts of 27 EHF patients, after adjusting for direct physical contact during illness and contact with the patient's body fluids. Dowell S F et al. J Infect Dis. 1999; 179: S 87 -S 91 © 1999 by the Infectious Diseases Society of America
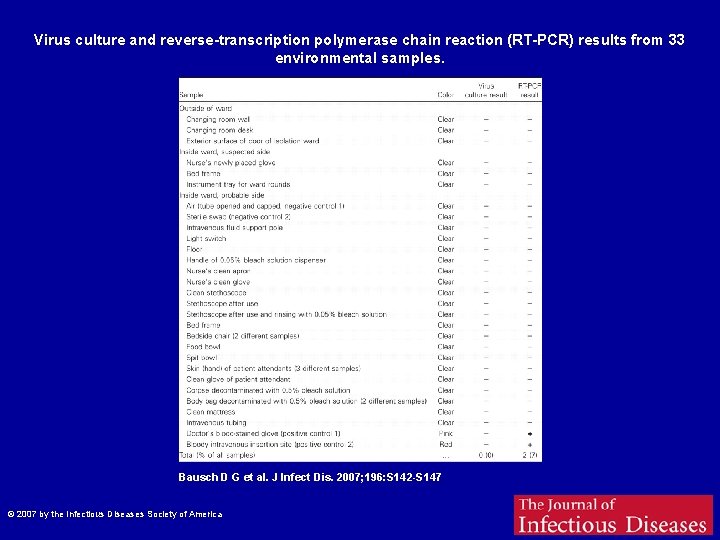
Virus culture and reverse-transcription polymerase chain reaction (RT-PCR) results from 33 environmental samples. Bausch D G et al. J Infect Dis. 2007; 196: S 142 -S 147 © 2007 by the Infectious Diseases Society of America



TRICKS OF THE TRADE


THE CLOCK STARTS…ITS ALREADY HOT

BUDDY CHECK

DISCIPLINED DOFFING

PPE FOR RESOURCE-RICH COUNTRIES West African transmission/ prevention is more similar than different for resource-rich countries. – No simple PPE widget to buy and you are protected (takes discipline and detailed process to minimize self-contamination) – Transmission in resource rich may have better environmental controls but impact on care interventions and disease transmission remains largely uncertain Airborne precautions are not unreasonable because interplay with modern therapeutics (oxygen delivery, etc) remains unknown Best means to disinfect during PPE doffing remains uncertain – Spray disinfectant (bleach, hydrogen peroxide) vs wipes

ORGANIZATION OF AN ETU Suspect ward- Annex at KGH – Pts who are triaged as suspect – Ambulance pts – Mixture of EVD and non-EVD pts Confirmed ward- Med/surg ward at KGH – “best” place to provide care Convalescent ward – Pts significantly improving w/o rebound sxs and awaiting neg PCR HCW flow should always go from Suspect ward to either Confirmed or Convalescent ward – ETU is “high risk”, outside of ETU must be protected. No one in PPE, once in ETU can leave without doffing/ disinfection. Materials which cannot be disinfected stay in ETU

GOING IN Dr. Henry and I were “clinical buddies” – Typically 2 hours in am and 2 hours in pm – Heat limitations for duration and times of day for ETU access – Unreliable electricity made night shifts too unsafe We established consensus amongst us and nurses about goals for particular shift – We kept each other on track because could be distracted off target by so many needs in ETU Final buddy check of PPE and hands go to apron (just like in OR when not actively involved in procedure) We start in the suspect ward

KGH STAFF

THE ANNEX

SUSPECT WARD We enter through the front gate and hop the trip hazard and pass the first few rooms to meet people outside – There are clearly sick people with probable EVD in ward but we bypass them to try to talk to lower suspicion folks first – Do not want to give someone EVD because they were incorrectly triaged to ETU Update the census and determine duration of sxs – PCR may be at detection threshold or below in early disease (need 72 hrs to r/o) – Census then matched to EVD PCR list (huge issue about pt id, sample matching integrity) Goals of suspect ward 1. Get low-med suspect pts PCR so can be d/cd rapidly 2. Identify very high suspicion pts and make sure they have PCR so can move to confirmed unit for more aggressive treatment 3. Keep all pts separated but really try to separate high prob from all others

CENSUS EXAMPLE

PERSONS UNDER INVESIGATION (PUI) FOR EVD • US CDC, state and local public health have criteria for screening • All US healthcare entities which must be able to screen/ temporarily isolate and protect HCWs from EVD – Can’t control where possible persons with EVD present • Timely travel from impacted areas or occupational exposure to EVD are best 1 st screening questions – Causes of fever and other symptoms are much more likely to be due to non-EVD etiologies • Even in West Africa, sick contact is best way to assess risk of EVD

SCREENING Screening criteria must be translated to make clinically operational Symptom duration is not part of criteria but useful (nausea/vomiting for weeks is not EVD) Diagnostics for alternate diagnosis may not be available at your institution
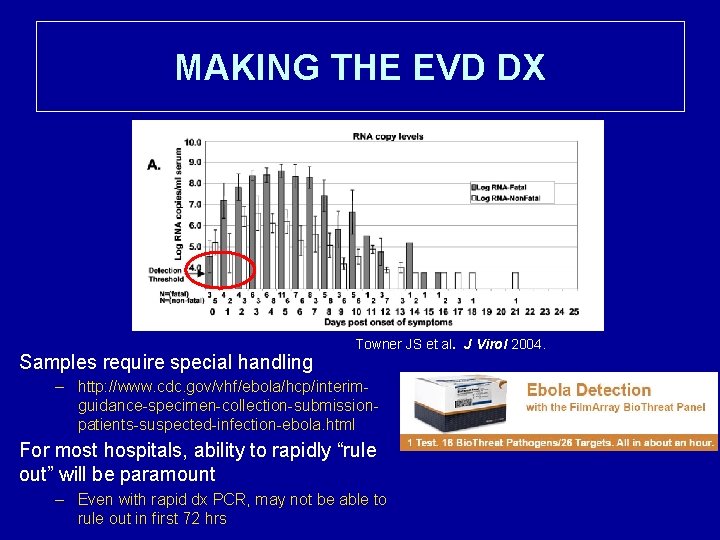
MAKING THE EVD DX Samples require special handling Towner JS et al. J Virol 2004. – http: //www. cdc. gov/vhf/ebola/hcp/interimguidance-specimen-collection-submissionpatients-suspected-infection-ebola. html For most hospitals, ability to rapidly “rule out” will be paramount – Even with rapid dx PCR, may not be able to rule out in first 72 hrs

RESOURCE-RICH GENERAL ISOLATION STRATEGIES Pt is cared for in dedicated space and not moved (except from ED depending on hosp plan) Diagnostics- most labs are only using POC tests – CDC guidance suggests can use general labs but most hospitals will not be doing so – Limited labs (will vary by equipment and process solutions) – Bedside ultrasound mainstay of imaging • Some facilities are using portable diag Xray as well • No CT, MR, cath lab, etc for suspected or confirmed EVD at most hospitals American College of Surgeons put out EVD guidance – Will require extensive training, planning and facilities commitment if any hospital chooses to operationalize

POSSIBLE ADVERSE CONSEQUENCES OF PUI PROCESS Person travels recently from impacted country – Has neurological signs/sxs suggestive of acute CVA Do you go immediately to CT scanner for possible TPA admin for CVA? How do you decide what is best for pt? How are facility and staff safety factored in? If there is a time sensitive window, what process is in place to optimize outcomes when EVD PCR from LRN cannot be turned around in necessary window?

RAPID EVD ASSESSMENT TEAM Must be able to rapidly assess likelihood of EVD Requires immediate activation of multi-disciplinary team Risk to pt if delayed dx or tx Public health, ID/inf control, clinicians, risk mgmt – Are there alternatives? Risk to HCWs or facility for proposed eval/tx – CT scan vs procedure Must have endorsement by hosp leadership to make decision or must make rapid rec and hospital leadership must make timely decision Should be formalized and tested prior to need

ANNEX CONTINUED Now we start assessing the pts who are high risk for EVD. Many are lying on the ground, prostrate. Some are near death. Most are in the same position as when they were brought in from the ambulances. – We provide water and Oral rehydration fluids (ORF) to those who everyone who can tolerate it as we assess them – We treat seriously ill with empiric ACT (for malaria), and ceftriaxone (or cipro) during severe GI dysfunction We have approx 60 -90 sec per pt and you learn how to assess pts in any position without breaching your PPE – We must move on as we still have the entire confirmed ward to see

ON TO THE CONFIRMED WARD 15 -20 pts are sitting outside of unit on open walkway – Many complain of myalgias, pruritus but generally “wellappearing” – We provide water, ORF, and paracetemol to each. We get their info, but we must move on Inside ward, numerous pts at various stages of illness – Initial screen for severe illness---walking, eating, under blankets, signs of bleeding (gingival, epistaxis, peri-IV)
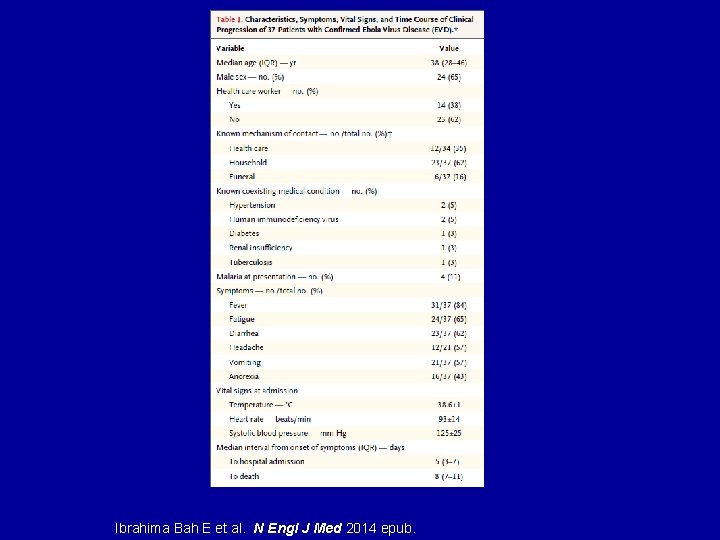

Ibrahima Bah E et al. N Engl J Med 2014 epub.
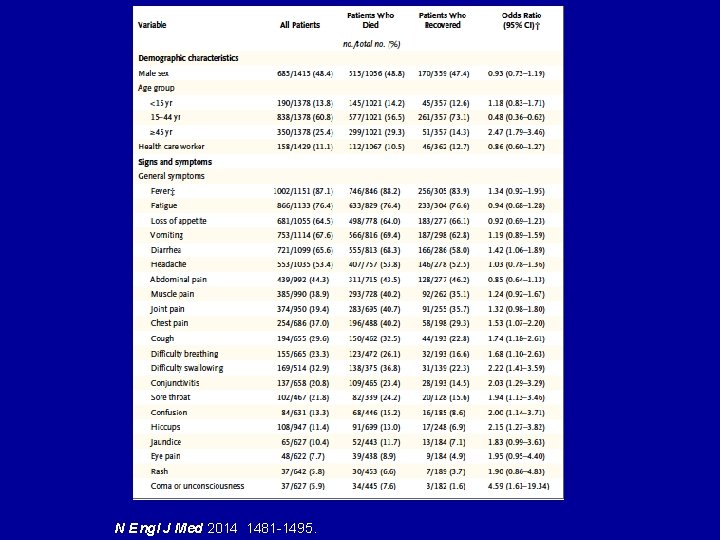
N Engl J Med 2014 1481 -1495.
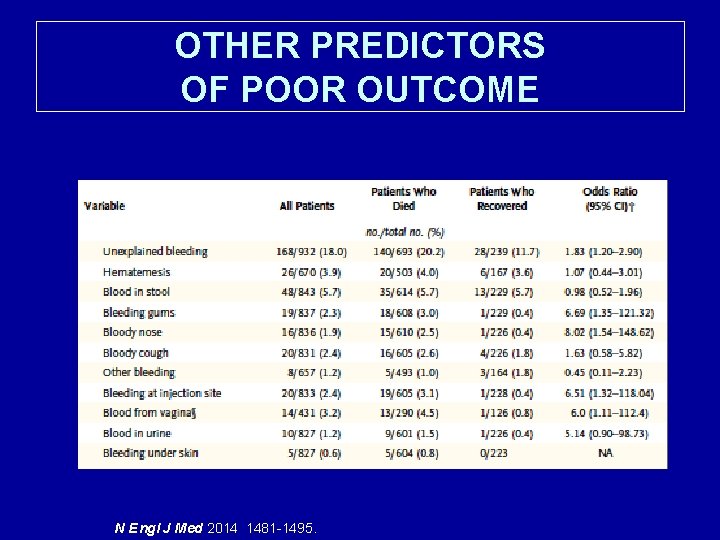
OTHER PREDICTORS OF POOR OUTCOME N Engl J Med 2014 1481 -1495.
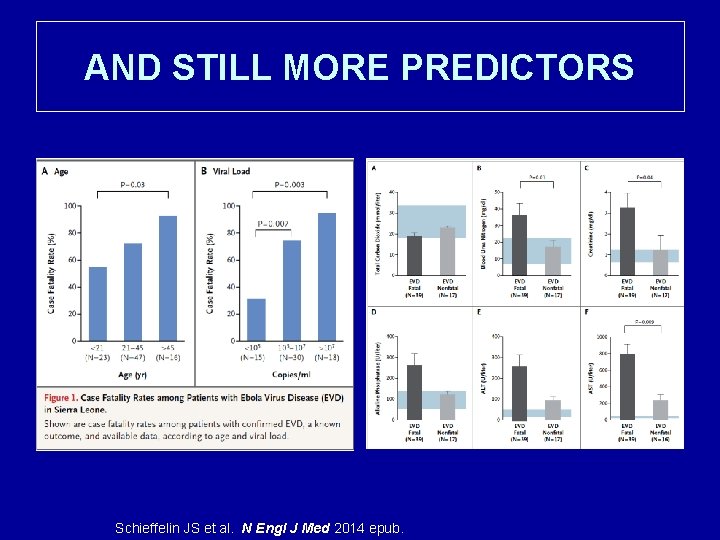
AND STILL MORE PREDICTORS Schieffelin JS et al. N Engl J Med 2014 epub.

SURVIVORS
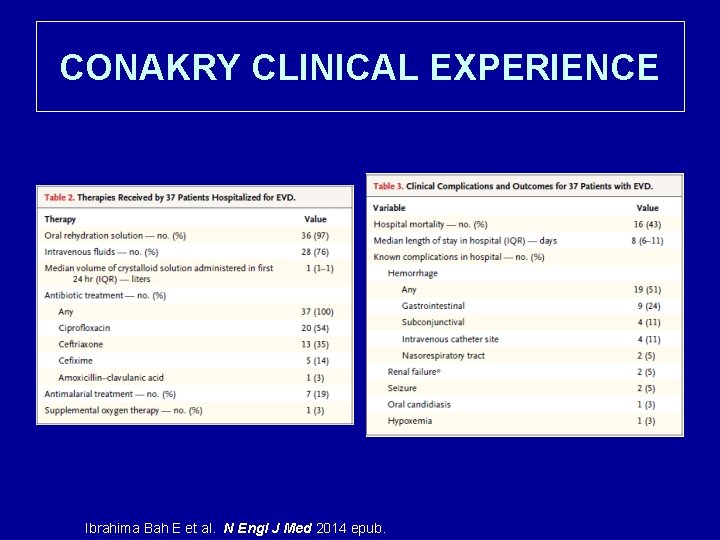
CONAKRY CLINICAL EXPERIENCE Ibrahima Bah E et al. N Engl J Med 2014 epub.

RUBINSON’S PRINCIPLES (= OPINIONS) FOR EVD CARE 1. Minimization of numbers of people in pt’s room 2. Minimization of exposure a) b) ? Role of routine exam and assessments Balancing pt needs with staff safety 3. There should be no emergencies 4. Procedures should be pre-briefed, choreographed and done by experienced, team-players a) PACE 5. Novel therapeutics should be used in clinical trial if possible 6. Limited organ support reasonable but many interventions/ diagnostics will put staff, institution at high risk

A BIT OF A PERSONAL MISHAP 1 day prior to finishing at KGH I stuck myself with an 18 G hollow bore needle through soiled gloves – Deep stick Determined by WHO and CDC to be high risk exposure and to be medically evacuated to NIH biocontainment center Elected to enroll in r. VSV vaccine PEP study

AN INTERESTING JOURNEY Most HCWs who become infected with EVD did not recognize exposure – I simply had to wait for the future – Long drive back to Freetown and flight to US

EVD FEAR TAKES OVER US Told not to open door of airplane in Azores – Considered dangerous and at time asymptomatic and only 48 hrs after exposure Large police escort moving at very fast speed to get me to NIH Had started to feel a bit ill at end of flight (anticipated timing for PEP sxs) Symptomatic at NIH and Mr. Jordan ill in Dallas
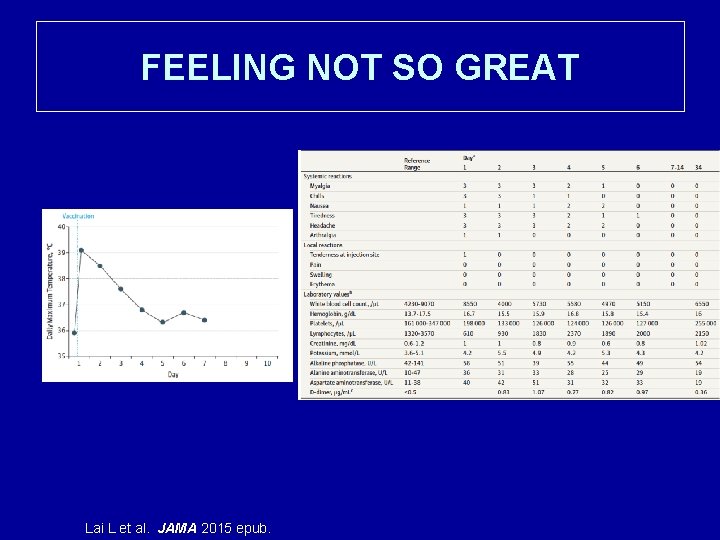
FEELING NOT SO GREAT Lai L et al. JAMA 2015 epub.

GREAT CARE BUT VERY ISOLATING

FEAR AND POLITICS OVER SCIENCE Dallas case and secondary case – Excessive public fear due to failed risk communication strategies Became clear my sxs were due to PEP and I was all better – Length of stay at NIH longer than sxs warranted and then placed under what was essentially home arrest Never would hurt anyone, but despite much more experience with EVD than any of the folks managing me, there was no place to appeal except in courts – Did not want to be identified to protect my daughter

PUBLIC HEALTH AND RESPONSE AGENCIES MUST BRING SENSIBILITY BACK TO RESPONSE: DON’T LET FEAR DEFEAT SCIENCE
- Slides: 57