Eating Disorder Ass Prof Heba Essawy Ain Shams

Eating Disorder Ass. Prof. Heba Essawy Ain Shams University

1 - General characteristic n Marked disturbance in eating behavior Including: § Anorexia nervosa. § Bulimia. § Obesity

2 - Anorexia nervosa: serious, characterize By: n Disturbed body image. n Self-imposed. n Severe dietary limitation n Serious malnutrition n Mortality is 5 -18%.

ANOREXIA NERVOSA Diagnosis (DSM-IV-TR): n Refusal to maintain body weight at or above a minimum normal weight for age and ht. (body wt 85% of that excepted) n Intense fear of gaining weight. n Amenorrhea (absence of 3 periods) Specify: n Restricting type n Purging type/Binge Eating.

CLINICAL FEATURES PHYSICAL SIGNS: n Hypothermia. n Dependent odema. n Bradicardia. n Hypotension. n Lanugo Hair. n ECG Changes: Flat or invert T wave Depressed ST Segment Lengthening of QT Interval.

LABORATORY EXAMINATION n n n n Serum Electrolyte. Renal Tests. Thyroid Function. Glucose Level. Cholesterol Level. CBC. ECG.

Epidemiology: n Life time prevalence n In Adolescent Girl n AN and BN n Death n Age: Sp. After stress n M: F ratio n In professions ballet dancers. 0. 5 - 3. 7% 0. 5 - 1% 30 - 50% 3 -8% 10 -30 years. 1: 20 modeling –

Etiology Biological: – Concordance in MZ than DZ – In familial depression – Eating disorders – Alcohol dependence. n n 3 Methoxy 4 hydroxy phenyl glycol( MHPG) in urine & CSF. norepinephrine turnover Endogenous opioid activity. Hypercortisolemia & non DST suppresion. MRI volume of gray matter during illness.

ETIOLOGY 2 - Psychological: n n n Reaction for independence. Lack of autonomy & selfhood. Over emphasis of thinness and exercise. Troubled parent relationship. Fear of pregnancy.

DIFERENTIAL DIAGNOSIS n Medical illness cancer, brain tumor. n Depressive disorder. n Somatization disorder. n Bulimia (wt. loss less than 15%)

ANOREXIA NERVOSA Prognosis: n 40% → recover. n 30% → improve. n 30% → chronic cases.

Treatment n Outpatient. Inpatient : depend on degree of dehydration, starvation, & electrolyte imbalance and weight loss. 1. Ensure weight gain 2. Treatment of metabolic condition n

ANOREXIA NERVOSA HOSPITALIZATION n - Recommended for patients who are 20 % below the expected. n - Require hospitalization if patients are 30% less than expected→ two to six months.

PLAN OF TREATMENT n Patient resists medication. n Antidepressant § SSRI Fluoxetine (Prozac) § Weight gain by cyproheptadine( periactin). § TCA → if nutritional status is ok. n Group therapy: § Education § Supportive § Inspirational n n n Individual psychodynamic Family therapy Cognitive therapy ( not effective)

BULIMIA NERVOSA n Uncontrolled , rapid ingestion n n Compulsive For short time Followed by n Self-induced vomiting n Use of laxatives n Use of diuretics n Fasting n Exercise Specify type n Purging n Non purging

Epidemiology n Life time prevalence 1 -4% n Age 16 -18 ys n M: F 1: 10. n Occur in normal weight or obese. Etiology 1. Biological n Norepinephrine n 5 -HT n Plasma endorphins after vomiting

PSYCHOLOGICAL n n Patient have difficulties with adolescent demands. Bulimics are impulsive, angry, Self destructive sexual relation. Emotional Lability and suicide are at Risk. Binge Eating is Egodystonic so seeking more help.

D. D: n Epileptic files. n CNS tumors n Borderline personality. n MD. D Course and Prognosis: n Electrolyte imbalance (Hypomagnesaemia and Hyperamylasemia). n Metabolic alkalosis. n Esophagitis, Salivary Gland Enlargement. n Dental caries. n 60% recover within 5 ys

Treatment 1. Hospitalization. n Electrolyte imbalance. Metabolic alkalosis. For suicide n n

2 - Pharmacological: n Imipramine (Tofranil) n Desipramine n Trazadonce n MAOI n SSRI Prozac 3 - Psychological n Motivation n Depression n Group therapy individual psychotherapy. cognitive therapy

EATING DISODER (NOS) n n n AN but with regular menses. AN with weight within normal range. BN occur less than twice a week , or less than 3 months. Repeated chewing or spiting out lerge amount of food. Binge Eating Disorder in absence of compensatory behavior.

Obesity: Def: Ch. By excessive accumulation of fat in the body Diagnosis: when the body wt. exceeds by 20% the standard wt. listed in ht-wt tables or according BMI, healthful BMI is range of 20 to 25. Epidemiology: § More in female by 6 times esp in lower social class § More in female than male Etiology: 1 - Biological § Impaired metabolic signal to the receptors in the hypothalamus after eating remaining sense of hunger § Leptin abnormality, act as a fat thermostat. Patient level leptin is more full in consumed. § Baseline set patient (food in relation to energy to keep baseline fat store).

Genetic: – 80% of patient have +ve family history. Psychological: – No Specific mental illness – Stress produces hyperphgia – Strong dependence needs produce overeating as compensation. D. D: – Metabolic: Cushing's disease – Myxedema – SRI wt gain – Anti-psychotic.

Treatment: n Diet: Balanced diet of 1. 100 to 1. 200 calories/day n Supplemented iron, folic acid , Zn, vit B 6. n Side effect of modified fasting n Orthostatic hypotension n Impaired nitrogen balance. Exercise: Drug n Orlistal (xenical) 260 mg/d n Sibutramine (Meridia) 10 -20 mg/d n Mazindal (Anorex) 3 -9 mg/d
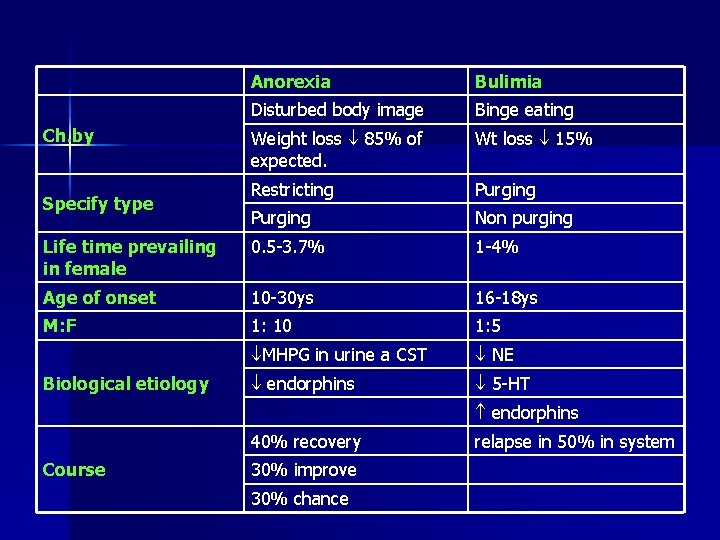
Anorexia Bulimia Disturbed body image Binge eating Weight loss 85% of expected. Wt loss 15% Restricting Purging Non purging Life time prevailing in female 0. 5 -3. 7% 1 -4% Age of onset 10 -30 ys 16 -18 ys M: F 1: 10 1: 5 MHPG in urine a CST NE endorphins 5 -HT Ch. by Specify type Biological etiology endorphins 40% recovery Course 30% improve 30% chance relapse in 50% in system
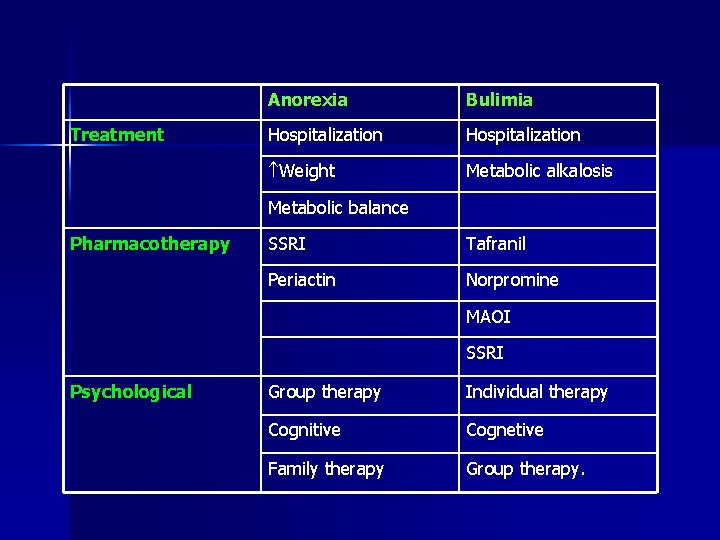
Treatment Anorexia Bulimia Hospitalization Weight Metabolic alkalosis Metabolic balance Pharmacotherapy SSRI Tafranil Periactin Norpromine MAOI SSRI Psychological Group therapy Individual therapy Cognitive Cognetive Family therapy Group therapy.
- Slides: 26