Early Detection of Possible Psychosis in Young People

Early Detection of Possible Psychosis in Young People: Is Stigma Linked with Symptoms or the At Risk Identification R 01 MH 096027 -01 National Institutes of Mental Health LAWRENCE YANG, PH. D. ASSOCIATE PROFESSOR DEPARTMENT OF SOCIAL AND BEHAVIORAL SCIENCES NEW YORK UNIVERSITY ADJUNCT ASSOCIATE PROFESSOR DEPARTMENT OF EPIDEMIOLOGY COLUMBIA UNIVERSITY

Click to edit. DISCLOSURES Master title style • Click to edit Master text styles • None 1

Click to edit Master title style RESEARCH BACKGROUND • Click to edit Master text styles • I) Social Factors that influence course of SCZ • II) Training in clinical psychology, anthropology and psychiatric epidemiology • III) Fieldwork in China • IV) Current NIH funding-- R 01– Stigma associated with prodromal psychosis; R 21– Stigma of genetic attributions in prodromal psychosis • R 01– Cognition of Untreated Psychosis in China – R 21 - Stigma Intervention for HIV in Botswana – U 19 - Global Hub- South America 2

Click to edit Master title style OVERVIEW • Click to edit Master text styles • I: Stigma’s Effects on Mental Health – Public stigma – Experienced Discrimination & Self stigma – Structural stigma – II: Stigma and the Clinical High Risk State for Psychosis – Initial Quantitative Findings (R 01) – Qualitative Findings 3

Click to edit Master style Definition of title Stigma • Click to edit Master text styles Stigma - set of interrelated social processes. Including: labeling, stereotyping, cognitive separating, emotional reactions, status loss and discrimination, and power (Link and Phelan, 2001) Leads to: poorer symptomatic and social outcomes (Link et al, 1989, Corrigan, 2006) 4

Click to edit Master. STIGMA title style PUBLIC • Click to edit Master text styles The process in which the general public stigmatizes individuals with mental illness and which consists of processes of stereotyping, prejudice, and discrimination 5

Click. STIGMA to edit Master title style PUBLIC GLOBALLY • Click to edit Master text styles Cross-National Study of “Backbone” of Public Stigma of Mental Illness (Pescosolido et al. , 2013) – 16 countries-- nationally representative samples – DSM-IV Case vignettes (MDD & SCZ) – Sample= 13, 081 community members – core sentiments that represent consistent, salient public health intervention targets – 5 items endorsed by >65% of respondents • • • Unwilling to care for children Unwilling to have marry into family Shouldn’t teach children Likely to be violent to self Unpredictable 6

Click to edit Master title style EXPERIENCED DISCRIMINATION • Click to edit Master text styles Experienced discrimination is when an individual is unfairly treated by another individual based on their status of having mental illness 7

Click to edit Master. Globally title style Discrimination • Click to edit Master text styles Cross-National Study of Stigma of Mental Illness (Thornicroft et al. , 2009) – 732 individuals with SCZ – 27 Countries (Europe; N. America; Asia; S. America) – 47% Negatively affected in Keeping Friends; 43% Treated differently by family *Greater discrimination associated with greater number of years ill (>5 years; >15 years) --Also increases with: Anticipated stigma and compulsory treatment 8

Click to edit Master. STIGMA title style INTERNALIZED • Click to edit Master text styles Internalized stigma takes place through stigmatized individuals themselves once they become aware of stereotypes and apply stereotypes to themselves. 9

Click to edit Master. Globally title style Anticipated Stigma • Click to edit Master text styles Cross-National Study of Stigma of Mental Illness (Thornicroft et al. , 2009) – 64% anticipated stigma in finding work – 55% anticipated stigma in intimate relationships – 72% felt need to “Conceal Diagnosis” 10
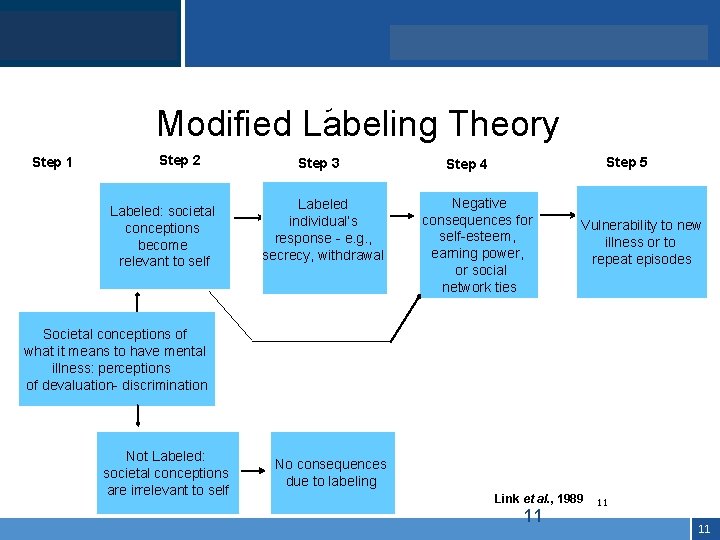
Click to edit Master title style • Click to edit Master text styles Modified Labeling Theory Step 1 Step 2 Labeled: societal conceptions become relevant to self Step 3 Labeled individual’s response - e. g. , secrecy, withdrawal Step 5 Step 4 Negative consequences for self-esteem, earning power, or social network ties Vulnerability to new illness or to repeat episodes Societal conceptions of what it means to have mental illness: perceptions of devaluation- discrimination Not Labeled: societal conceptions are irrelevant to self No consequences due to labeling Link et al. , 1989 11 11 11
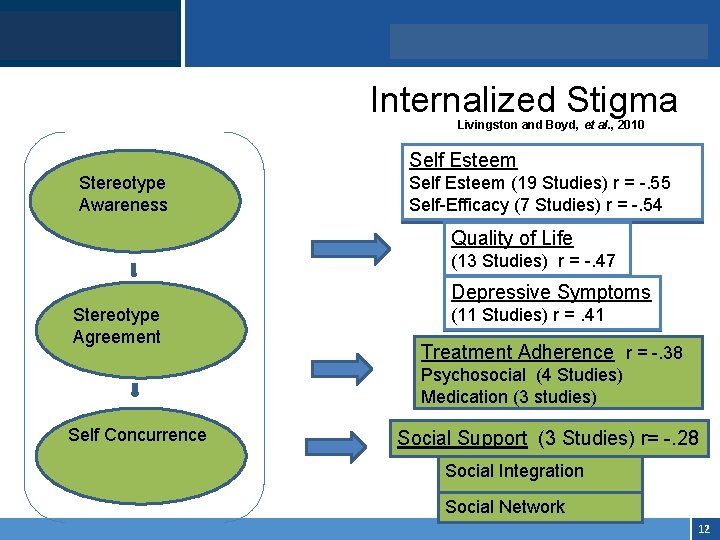
Click to edit Master title style • Internalized Stigma Click to edit Master text styles Livingston and Boyd, et al. , 2010 Self Esteem Stereotype Awareness Self Esteem (19 Studies) r = -. 55 Self-Efficacy (7 Studies) r = -. 54 Quality of Life (13 Studies) r = -. 47 Depressive Symptoms Stereotype Agreement (11 Studies) r =. 41 Treatment Adherence r = -. 38 Psychosocial (4 Studies) Medication (3 studies) Self Concurrence Social Support (3 Studies) r= -. 28 Social Integration Social Network 12

Click to edit Master. STIGMA title style STRUCTURAL • Click to edit Master text styles Institutional practices that work to the disadvantage of the stigmatized group or person 13

Click to edit Master. STIGMA title style STRUCTURAL • Click to edit Master text styles Common Forms – Countries spending far less Gross Domestic Product on mental health than physical health – Countries forbidding people with mental illness rights and privileges 14

BACKGROUND: STIGMA & CHR • ‘Clinical High Risk State for Psychosis’ (CHR)–Category to identify youth (12 -25 years old) who may develop psychosis • Earliest Identification of Pre-psychotic Signs; 29% transition to psychosis within 2 years • Stigma that may be associated with identification >70% ‘False Positives’ (Carpenter, 2010) – Public stigma (Yang, 2013) and Self-Stigma (Rusch, 2014; Rusch, 2015, Gronholm, Thornicroft, Laurens, Evans-Lacko, 2017) have been identified as salient for CHR – Stigma effects help-seeking and service contact for CHR (Gronholm, Thornicroft, Laurens, Evans-Lacko, 2017) 15

BACKGROUND • Unresolved question: “At-Risk Identification” vs. “Symptom” Stigma Why this matters: • CHR youth are identified when they are help-seeking for problematic symptoms/experiences • Earliest identification and treatment is intended to mitigate symptoms, which may avert significant stigma (e. g. , psychiatric hospitalization of a 1 st episode) • If symptom stigma is primary correlate of outcomes at baseline, may be somewhat less concerning • Stigma of at-risk identification (labeling stigma) may be initiated by CHR service – May be more concerning to field 16

BACKGROUND • No consensus on a standardized way of communicating the CHR status for all participants in CHR programs • Specialized CHR program clinicians are typically trained to give individualized feedback based on a wide range of factors, including: – – the individual and family’s concerns treatment engagement cultural background estimated risk within the CHR classification • CHR feedback might be adapted according to relatively lowerlevel symptoms indicating reduced risk (Cannon et al. , 2016). 17

STIGMA – “LABELING” “About being told I am at-risk for or developing psychosis…” (Yang, Link, Corcoran et al, 2015, SCZ Research) 1) ‘Negative emotions (shame)’ • “[X], I have felt ashamed. ” (3 items) 2) ‘Secrecy’ • “I have told no one that [X]. ” (5 items) 3) ‘Experienced Discrimination’ • “[X], people are a little afraid of me. ” (5 items) 18
![STIGMA – “Symptoms” “About my symptoms and experiences…” 1) ‘Negative emotions (shame)’ • “[X], STIGMA – “Symptoms” “About my symptoms and experiences…” 1) ‘Negative emotions (shame)’ • “[X],](http://slidetodoc.com/presentation_image_h/02dec875f126e16142efbd88dabf4d01/image-20.jpg)
STIGMA – “Symptoms” “About my symptoms and experiences…” 1) ‘Negative emotions (shame)’ • “[X], I have felt ashamed. ” (3 items) 2) ‘Secrecy’ • “I have told no one about [X]. ” (5 items) 3) ‘Experienced Discrimination’ • “[X], people are a little afraid of me. ” (5 items) 19

HYPOTHESES Main Hypotheses: #1) Compare Labeling vs. Symptom-related stigma #2) Assess to what extent labeling vs. symptom stigma are associated with psychological (self-esteem, quality of life) and social (social functioning, social networks) outcomes in CHR youth 20

SAMPLE 169 ‘Clinical High Risk (CHR)’ individuals given stigma assessment at CHR identification and then 6 month follow-up at Harvard, Maine, and Columbia University Medical Centers Study Period: 2012 -2017 Baseline Data Only presented (those who meet COPS criteria) Help seeking participants who met ≥ 1 SIPS/SOPS criteria: (1) attenuated positive symptom syndrome (2) genetic risk and deterioration syndrome (3) brief intermittent psychotic syndrome. (Miller, 2003) Included those CHR individuals who perceived psychosis risk; excluded those who were not aware of any or did not endorse psychosis-risk 21
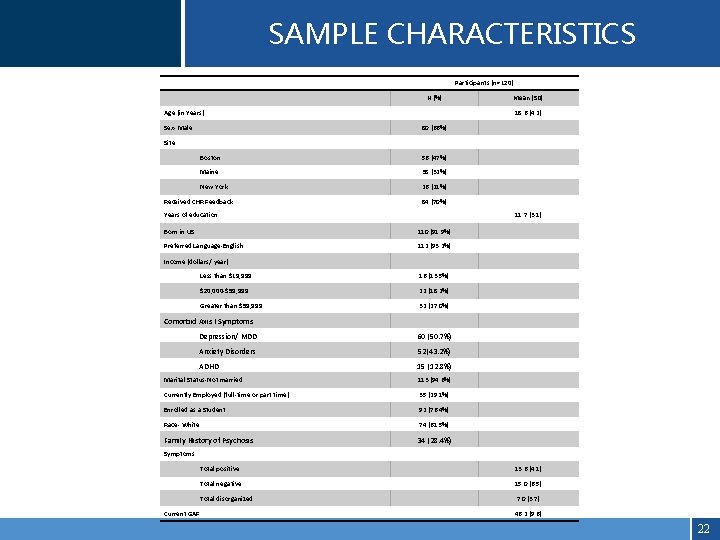
SAMPLE CHARACTERISTICS Participants (n=120) Age (in Years) Sex- Male Site N (%) Mean (SD) 18. 6 (4. 2) 80 (66%) Boston 56 (47%) Maine 38 (32%) New York 26 (21%) 84 (70%) 11. 7 (3. 1) Born in US 110 (91. 9%) Preferred Language-English 112 (93. 2%) Less than $19, 999 16 (13. 5%) $20, 000 -$59, 999 22 (18. 2%) Greater than $59, 999 32 (27. 0%) Received CHR Feedback Years of education Income (dollars/ year) Comorbid Axis I Symptoms Depression/ MDD 60 (50. 7%) Anxiety Disorders 52(43. 2%) ADHD 15 (12. 8%) Marital Status-Not married 113 (94. 6%) Currently Employed (full-time or part time) 35 (29. 1%) Enrolled as a Student 92 (76. 4%) Race- White+ 74 (61. 5%) Family History of Psychosis 34 (28. 4%) Symptoms Current GAF Total positive 13. 6 (4. 1) Total negative 15. 0 (6. 5) Total disorganized 7. 0 (3. 7) 46. 2 (9. 6) 22

Outcomes Psychological • Self-Esteem (Rosenberg Self-Esteem, 1965) • Quality of Life (WHO Quality of Life Scale- BREF, 1994) Social • Global Functioning: Social Scale (Cornblatt et al, 2007) • Loss of Social Networks (Norbeck Social Support Questionnaire; Total “loss of relationships/support” due to stigma) 23
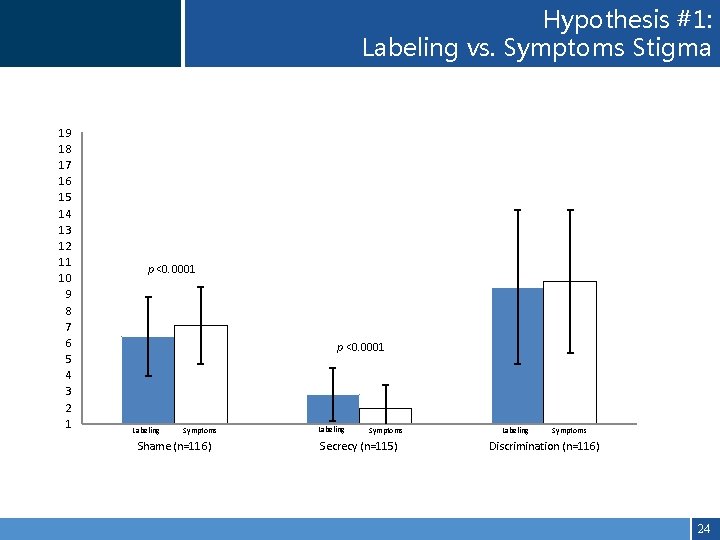
Hypothesis #1: Labeling vs. Symptoms Stigma 19 18 17 16 15 14 13 12 11 10 9 8 7 6 5 4 3 2 1 p <0. 0001 Labeling Symptoms Shame (n=116) Labeling Symptoms Secrecy (n=115) Labeling Symptoms Discrimination (n=116) 24
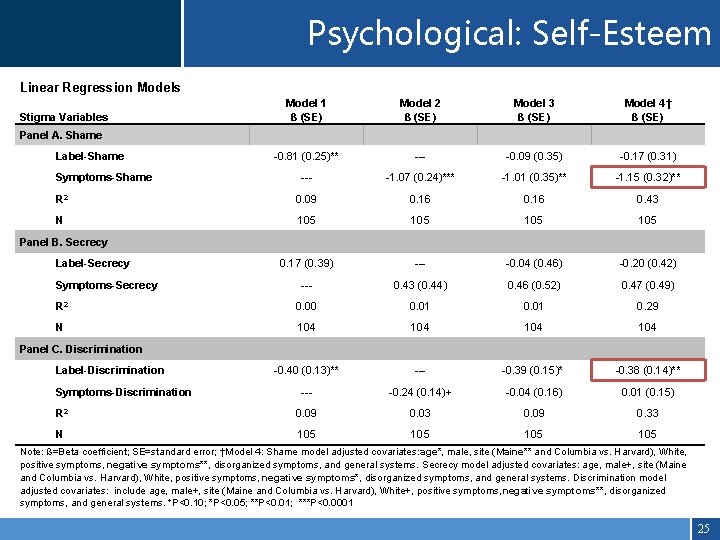
Psychological: Self-Esteem Linear Regression Models Stigma Variables Model 1 ß (SE) Model 2 ß (SE) Model 3 ß (SE) Model 4† ß (SE) Panel A. Shame -0. 81 (0. 25)** --- -0. 09 (0. 35) -0. 17 (0. 31) --- -1. 07 (0. 24)*** -1. 01 (0. 35)** -1. 15 (0. 32)** R 2 0. 09 0. 16 0. 43 N 105 105 0. 17 (0. 39) --- -0. 04 (0. 46) -0. 20 (0. 42) --- 0. 43 (0. 44) 0. 46 (0. 52) 0. 47 (0. 49) R 2 0. 00 0. 01 0. 29 N 104 104 -0. 40 (0. 13)** --- -0. 39 (0. 15)* -0. 38 (0. 14)** --- -0. 24 (0. 14)+ -0. 04 (0. 16) 0. 01 (0. 15) R 2 0. 09 0. 03 0. 09 0. 33 N 105 105 Label-Shame Symptoms-Shame Panel B. Secrecy Label-Secrecy Symptoms-Secrecy Panel C. Discrimination Label-Discrimination Symptoms-Discrimination Note: ß=Beta coefficient; SE=standard error; †Model 4: Shame model adjusted covariates: age*, male, site (Maine** and Columbia vs. Harvard), White, positive symptoms, negative symptoms**, disorganized symptoms, and general systems. Secrecy model adjusted covariates: age, male+, site (Maine and Columbia vs. Harvard), White, positive symptoms, negative symptoms*, disorganized symptoms, and general systems. Discrimination model adjusted covariates: include age, male+, site (Maine and Columbia vs. Harvard), White+, positive symptoms, negative symptoms**, disorganized symptoms, and general systems. +P<0. 10; *P<0. 05; **P<0. 01; ***P<0. 0001 25
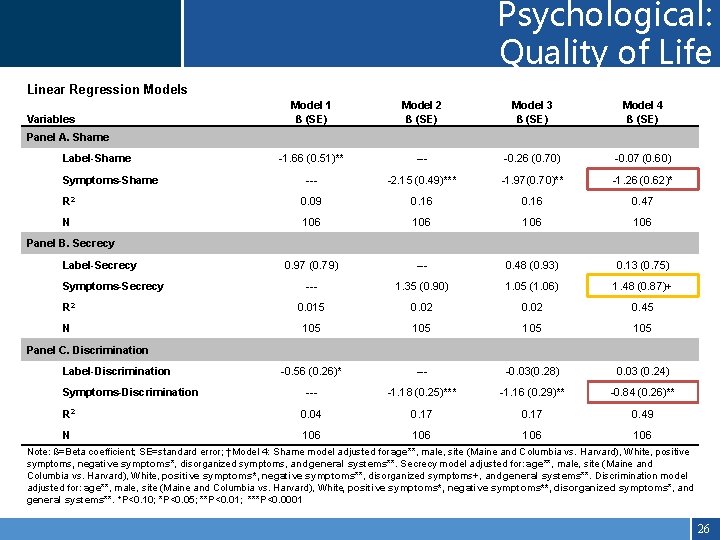
Psychological: Quality of Life Linear Regression Models Variables Model 1 ß (SE) Model 2 ß (SE) Model 3 ß (SE) Model 4 ß (SE) -1. 66 (0. 51)** --- -0. 26 (0. 70) -0. 07 (0. 60) --- -2. 15 (0. 49)*** -1. 97(0. 70)** -1. 26 (0. 62)* R 2 0. 09 0. 16 0. 47 N 106 106 0. 97 (0. 79) --- 0. 48 (0. 93) 0. 13 (0. 75) --- 1. 35 (0. 90) 1. 05 (1. 06) 1. 48 (0. 87)+ R 2 0. 015 0. 02 0. 45 N 105 105 -0. 56 (0. 26)* --- -0. 03(0. 28) 0. 03 (0. 24) --- -1. 18 (0. 25)*** -1. 16 (0. 29)** -0. 84 (0. 26)** R 2 0. 04 0. 17 0. 49 N 106 106 Panel A. Shame Label-Shame Symptoms-Shame Panel B. Secrecy Label-Secrecy Symptoms-Secrecy Panel C. Discrimination Label-Discrimination Symptoms-Discrimination Note: ß=Beta coefficient; SE=standard error; †Model 4: Shame model adjusted for age**, male, site (Maine and Columbia vs. Harvard), White, positive symptoms, negative symptoms*, disorganized symptoms, and general systems**. Secrecy model adjusted for: age**, male, site (Maine and Columbia vs. Harvard), White, positive symptoms*, negative symptoms**, disorganized symptoms+, and general systems**. Discrimination model adjusted for: age**, male, site (Maine and Columbia vs. Harvard), White, positive symptoms*, negative symptoms**, disorganized symptoms*, and general systems**. +P<0. 10; *P<0. 05; **P<0. 01; ***P<0. 0001 26

Social Scale Linear Regression Models Variables Model 1 ß (SE) Model 2 ß (SE) Model 3 ß (SE) Model 4 ß (SE) -0. 04 (0. 06) --- 0. 03 (0. 09) 0. 02 (0. 07) --- -0. 07 (0. 06) -0. 09 (0. 09) -0. 08 (0. 07) R 2 0. 00 0. 01 0. 47 N 109 109 -0. 23 (0. 09)* --- -0. 18 (0. 10)+ -0. 13 (0. 08) --- -0. 22 (0. 10)* -0. 12 (0. 12) -0. 06 (0. 09) R 2 0. 06 0. 04 0. 07 0. 49 N 108 108 -0. 02 (0. 03) --- 0. 01 (0. 03) 0. 02 (0. 03) --- -0. 08 (0. 03)* -0. 07 (0. 04)* -0. 05 (0. 03)+ R 2 0. 01 0. 06 0. 48 N 109 109 Panel A. Shame Label-Shame Symptoms-Shame Panel B. Secrecy Label-Secrecy Symptoms-Secrecy Panel C. Discrimination Label-Discrimination Symptoms-Discrimination Note: ß=Beta coefficient; SE=standard error; †Model 4: Shame model adjusted for: age, male+, site (Maine+ and Columbia* vs. Harvard), White, positive symptoms, negative symptoms***, disorganized symptoms**, and general systems. Secrecy model adjusted for: age, male, site (Maine+ and Columbia** vs. Harvard), White, positive symptoms, negative symptoms***, disorganized symptoms**, and general systems. Discrimination model adjusted for age, male+, site (Maine* and Columbia* vs. Harvard), White, positive symptoms, negative symptoms***, disorganized symptoms**, and general systems. +P<0. 10; *P<0. 05; **P<0. 01; ***P<0. 0001 27

Social Network Loss Linear Regression Models Variables Model 1 ß (SE) Model 2 ß (SE) Model 3 ß (SE) Model 4 ß (SE) 0. 18 (0. 03)*** --- 0. 11 (0. 04)** --- 0. 17 (0. 03)*** 0. 09 (0. 04) R 2 0. 26 0. 24 0. 29 0. 32 N 107 107 0. 08 (0. 05) --- 0. 08 (0. 06) 0. 11 (0. 06)+ --- 0. 03 (0. 06) -0. 02 (0. 07) R 2 0. 0023 0. 02 0. 13 N 106 106 0. 02 (0. 02) --- -0. 02 (0. 02) --- 0. 07 (0. 02)*** 0. 08 (0. 02)** R 2 0. 01 0. 15 0. 16 0. 22 N 107 107 Panel A. Shame Label-Shame Symptoms-Shame Panel B. Secrecy Label-Secrecy Symptoms-Secrecy Panel C. Discrimination Label-Discrimination Symptoms-Discrimination Note: ß=Beta coefficient; SE=standard error; †Model 4: Shame model adjusted for: age, male, site (Maine and Columbia vs. Harvard), White, positive symptoms, negative symptoms, disorganized symptoms, and general systems. Secrecy model adjusted for: age, male*, site (Maine and Columbia vs. Harvard), White, positive symptoms, negative symptoms, disorganized symptoms, and general systems. Discrimination model adjusted for: age, male+, site (Maine and Columbia vs. Harvard), White, positive symptoms, negative symptoms, disorganized symptoms, and general systems. +P<0. 10; *P<0. 05; **P<0. 01; ***P<0. 0001 28
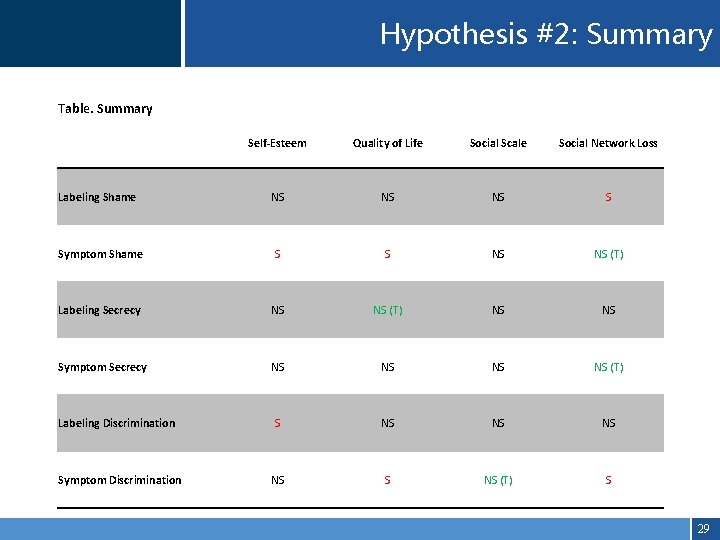
Hypothesis #2: Summary Table. Summary Self-Esteem Quality of Life Social Scale Social Network Loss Labeling Shame NS NS NS S Symptom Shame S S NS NS (T) Labeling Secrecy NS NS (T) NS NS Symptom Secrecy NS NS (T) Labeling Discrimination S NS NS NS Symptom Discrimination NS S NS (T) S 29

Qualitative: ‘Most Impacted’ By Psychosis • Purpose: To examine the nature of labeling- related stigma • Subjective Experience of being told at CHR (Yang et al, in press, SCZ Research) • Qualitatively examine processes including • --Positive effects (i. e. , operating through direct interaction with specialized CHR clinicians) • --Negative effects (i. e. , operating as anticipated stigma through CHR individuals themselves). • --Co-occurrence of these 30

Sample • Sample: Thirty-eight (n=38) semi-structured qualitative interviews (2009 -2010) to examine the meaning of being told they are at CHR • Were conducted after CHR identification, on average 11. 5 (SD=11. 7) months after entering the Columbia site. 31

Qualitative Questions • #1) Any direct treatment from others related to the CHR identification: – “Is there anything that happened to you in terms of how people treated you, good or bad, as a result of being in this (CHR) program? ” • Probes: – “Can you give me an example of when you were treated this way? ”, – “Who treated you this way? Where/when? ”, – “How did it make you feel? How did you respond to it? 32

Qualitative Questions • #2) Any potential effects via internalized processes that were related to CHR identification: – “In being in this program, you were told you have ‘an increased risk of psychosis compared to your peers. ’ How has this affected how you see yourself and how others see you? ” – Probes: • “Did being told you are ‘at-risk’ for psychosis change the way you thought about yourself? If so, how? ” • “Are you concerned about how others might react to knowing your at-risk status? ”, “Would others treat you any differently? ” 33

Qualitative Analyses NVivo software (V. 11. 0) utilized: -- Methodological advantage of quantifying overlap between major codes • Focused on the intersection between: 1) Positive and; 2) Negative Labeling Experiences • Jaccard’s similarity index (j-index), a measure of similarity indicating percentage overlap (range = 0% - 100%) of selected themes. 34

RESULTS Theme Definition Examples Endorsed a positive experience from being identified as CHR Reflects any one of the below positive code categories Accurate 0. 59 Understanding of CHR Risk Demonstrates a correct understanding of what it means to have a CHR status using specific language about risk after formal identification “It’s (being identified as at “psychosis-risk” is) like having a sore throat. You don’t know it will lead to strep throat, you have something indicating something is wrong but it might not develop into strep throat. ” Interpersonal Benefits of Disclosure of the CHR identification leads to a closer or more supportive relationship “Other people (participant’s friends and family ) are more aware of what I am thinking and feeling because of my CHR status. It is something like they may be more sensitive to me (about)…They are more supportive. ” Overall Positive J 0. 93 0. 50 35
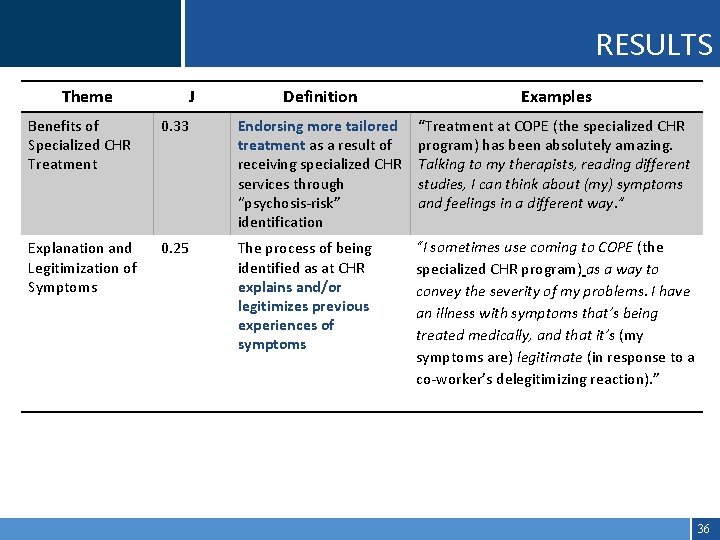
RESULTS Theme J Definition Examples Benefits of Specialized CHR Treatment 0. 33 Endorsing more tailored treatment as a result of receiving specialized CHR services through “psychosis-risk” identification “Treatment at COPE (the specialized CHR program) has been absolutely amazing. Talking to my therapists, reading different studies, I can think about (my) symptoms and feelings in a different way. ” Explanation and Legitimization of Symptoms 0. 25 The process of being identified as at CHR explains and/or legitimizes previous experiences of symptoms “I sometimes use coming to COPE (the specialized CHR program) as a way to convey the severity of my problems. I have an illness with symptoms that’s being treated medically, and that it’s (my symptoms are) legitimate (in response to a co-worker’s delegitimizing reaction). ” 36
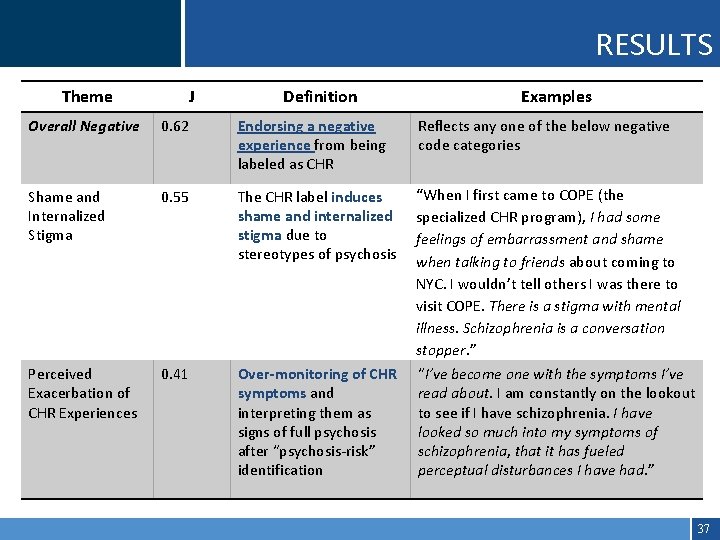
RESULTS Theme J Definition Examples Overall Negative 0. 62 Endorsing a negative experience from being labeled as CHR Reflects any one of the below negative code categories Shame and Internalized Stigma 0. 55 The CHR label induces shame and internalized stigma due to stereotypes of psychosis “When I first came to COPE (the specialized CHR program), I had some feelings of embarrassment and shame when talking to friends about coming to NYC. I wouldn’t tell others I was there to visit COPE. There is a stigma with mental illness. Schizophrenia is a conversation stopper. ” Perceived Exacerbation of CHR Experiences 0. 41 Over-monitoring of CHR symptoms and interpreting them as signs of full psychosis after “psychosis-risk” identification “I’ve become one with the symptoms I’ve read about. I am constantly on the lookout to see if I have schizophrenia. I have looked so much into my symptoms of schizophrenia, that it has fueled perceptual disturbances I have had. ” 37
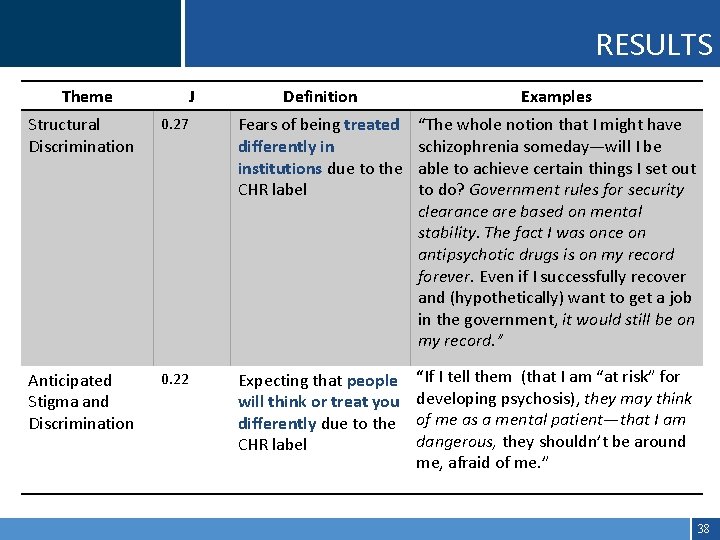
RESULTS Theme J Definition Examples Structural Discrimination 0. 27 Fears of being treated differently in institutions due to the CHR label “The whole notion that I might have schizophrenia someday—will I be able to achieve certain things I set out to do? Government rules for security clearance are based on mental stability. The fact I was once on antipsychotic drugs is on my record forever. Even if I successfully recover and (hypothetically) want to get a job in the government, it would still be on my record. ” Anticipated Stigma and Discrimination 0. 22 Expecting that people will think or treat you differently due to the CHR label “If I tell them (that I am “at risk” for developing psychosis), they may think of me as a mental patient—that I am dangerous, they shouldn’t be around me, afraid of me. ” 38

RESULTS Co-Occurring Positive and Negative Themes: Over half of the transcripts expressed overlap between positive and negative themes (Jaccards Coefficient=0. 55). --“Interpersonal Benefits of Disclosure” co-occurring with “Altered Perception and/or Negative Treatment from Others” (J=0. 5). --Individuals perceived interpersonal benefits of disclosing their mental health status, which was joined by a threat of being negatively treated or perceived by others, upon disclosure. “To talk about my at-risk status, there was stigma I had; growing up there was family embarrassment about my family’s mental illnesses. . . Having this new status (getting the CHR label by COPE) also scared my mom as well. My mom has a schizophrenic sister. . . Being identified as ‘at risk’ equals people thinking you are really developing something…. I sometimes use coming to COPE as a way to convey the severity of my problems. People try to be supportive. People make extra efforts, they would check in on me more. ” 39

RESULTS --“Accurate Understanding of Risk Status” Co-occurring with “Perceived Exacerbation of CHR Experiences” (J=0. 4). --Individuals with an accurate understanding of their risk status were likely to benefit from specialized CHR treatment through accurate understanding; however, this increase in monitoring may contribute to developing anxiety over their experiences. “[I now know that] Being CHR conveys a slightly greater risk for a disease. But it is a very complicated concept to explain to people…Dr. Kelly (psychiatrist at the CHR program) asks me about perceptual difficulties. I worry that these might be signs of psychosis, but now I can talk about it. At first identification, I was more worried because I thought it meant I was psychotic, and that there was an increase in the possibility that it’s (psychosis) really happening. …. ” 40

discussion Main Findings (Quantitative): Which form of stigma is higher? : Mixed Findings: Symptom Shame higher; but Labeling Secrecy higher Which form of stigma is more strongly associated? : Of 6 positive associations with outcomes, 4 have symptom stigma as more powerful correlate - Adds to findings that stigma matters for CHR - On balance, symptom stigma appears to be more salient at baseline; may be a target for CHR treatment - However, labeling stigma is present and might grow as youth become more familiar with identification status 41

discussion Qualitative Findings: Being told that one is “at risk for psychosis” is most likely linked with positive and negative experiences, which commonly overlap • -- Goal: Minimize negative effects while accentuating the positive benefits of CHR identification 42

discussion Implications for clinical care: Specialized CHR programs could be careful to avoid a singular focus on “psychosis-risk” and make it a point to attend to what is most distressing to each individual (e. g. , nonpsychotic disorders) (Yang et al, in press, SCZ Research) Help youth see their insight into their CHR symptoms as a strength, enabling them to effectively engage in treatments that can reduce their risk + receive support from others While important to engagement, recognize that being identified as “at risk for psychosis” may adversely impact individuals’ sense of self + anticipated treatment from others • CHR stigma intervention (Lucksted, “Ending 43

acknowledgements Collaborators: Larry J Seidman, Kristen Woodberry (m. PI’s), Caitlin Bryant, Emily Kline, Dan Shapir, Leda Kennedy Beth Israel Deaconess/ Harvard Medical School William Mc. Farlane (m. PI), Donna Downing, Anna Cloutier– Maine Medical Center Cheryl Corcoran– Mt Sinai School of Medicine Bruce Link– UC Riverside Ragy Girgis, Gary Brucato– NY State Psychiatric Institute/ Columbia University 44

RESULTS -- “Explanation and Legitimization of Symptoms” co-occurring with “Anticipated Stigma and Discrimination” (J=0. 375). --While the CHR identification provided an explanation for and legitimized symptoms, individuals could simultaneously anticipate stigma and discrimination due to this newfound knowledge. “The label and description has been positive for me because now I know that it’s “something. ” There have been things or symptoms that people have said ‘oh, you should have that checked. ’ …It’s good to know that it’s “something”, a real thing. I worry how being in COPE would affect my life in the future if anyone ever found out. I wonder if people would decide that I’m unfit to be a mother. I’m participating in COPE for my children in case they discover that this is genetic. But I worry that it’s in my records and that [my records] will come back even if I get better. ” 45
- Slides: 46