EAR PAIN Auricle 4 Hematoma 4 Cellulitis 4


































- Slides: 39

EAR PAIN

Auricle 4 Hematoma 4 Cellulitis 4 Relapsing Polychondritis

Hematoma 4 A localized mass of extravasated blood within the auricle- “bruise”

Hematoma 4 Must be drained to prevent significant cosmetic deformity 4 dissolution of supporting cartilagecauliflower ear

Cellulitis 4 Inflammation of the cellular tissue 4 May include lobule 4 Treat with Augmentin or Keflex 4 Complications- perichondritis and its resultant deformity

Relapsing Polychondritis 4 Auricular erythema and edema 4 Recurrent, frequently bilateral, painful 4 Does not include lobule- no cartilage 4 Systematic- may progress to involvement of the tracheobronchial tree 4 Treat- Corticosteroids might forestall cartilage dissolution

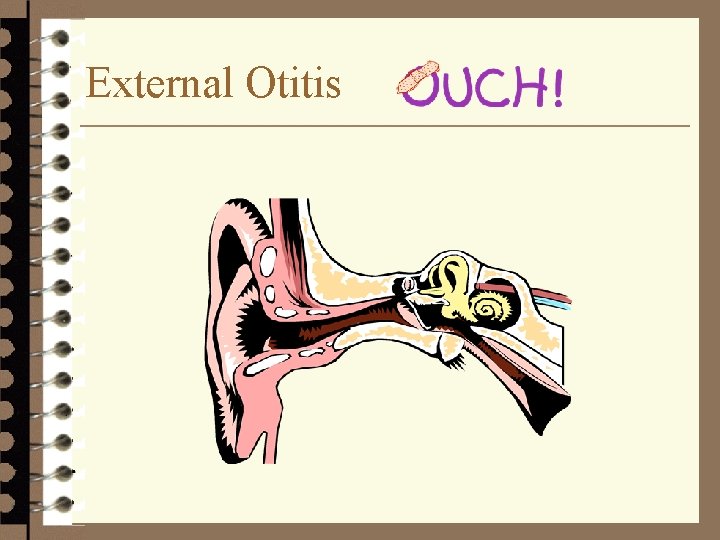
External Otitis

Otitis Externa 4 Otalgia 4 Pruritus 4 Purulent discharge 4 Often recent water exposure or mechanical trauma

Examination 4 Erythema 4 Edema 4 Purulent exudate 4 Auricular pain with manipulation 4 TM- moves normally with pneumatic otoscopy

Treatment 4 Avoid moisture 4 Otic drops containing aminoglycoside antibiotic and anti-inflammatory corticosteroid--neomycin sulfate, polymyxin B sulfate, and hydrocortisone 4 Ear wick

Auricular Pruritis 4 Common site- meatus 4 usually self induced – excoriation – overly zealous ear cleaning 4 Otitis Externa? ? 4 Dermatologic condition – seborrheic dermatitis – psoriasis

Treatment 4 Regeneration of Cerumen “blanket” 4 Avoid drying agents- soap & water, swabs 4 Mineral oil 4 0. 1% Triamcinolone- topical corticosteroid 4 Oral antihistamine 4 Stop messing with it!!!!

Malignant External Otitis 4 Persistent external otitis 4 Evolves into Osteomyelitis of the skull base – Diabetic or Immunocompromised 4 Pseudomonas aeruginosa

Clinical Findings 4 Persistent foul aural discharge 4 Granulation in the ear canal 4 Deep otalgia 4 Progressive cranial nerve palsies – (VI, VII, IX, X, XII) 4 Diagnosis confirmed with CT – osseous erosion

Treatment 4 Prolonged (antipseudomonal) ATB therapy – IV or Oral ciprofloxacin 4 Occasional surgical debridement

Serous Otitis Media 4 Caused by negative pressure – Blocked auditory tube – Transudation of fluid • children- tubes more narrow, more horizontal • common after URI • adults- persistent--think cancer

Clinical Findings 4 Dull, hypomobile TM 4 Air bubbles in middle ear 4 Conductive hearing loss

Treatment 4 Autoinflation 4 Oral corticosteroids 4 Oral ATB 4 All else fails, ventilating tubes

Barotrauma 4 Negative pressure tends to collapse and lock the auditory tube – Rapid altitudinal change • Air travel • Scuba diving

Treatment 4 Swallow, yawn, autoinflate 4 Systemic or topical decongestants – pseudoephedrine – phenylephrine nasal spray 4 If persists on ground after treatments listed above… – Myringotomy provides immediate relief – Ventilating tubes- frequent flyer

Acute Otitis Media 4 Bacterial infection of the mucosally lined air -containing spaces of the temporal bone. – Usually precipitated by viral URI which causes auditory tube edema…accumulation of fluid that becomes secondarily infected with bacteria – Streptococcus pneumoniae (49%), Haemophilus influenzae (14%), Moraxella catarrhalis (14%)

H&P Findings 4 Otalgia 4 Aural pressure 4 Decreased hearing 4 Fever 4 erythema 4 Decreased mobility of TM 4 TM bulge – perforation eminent

Treatment 4 ATB – amoxicillin – erythromycin – sulfonamides 4 Decongestants 4 Tympanocentesis 4 Ventilating tubes 4 ppx – sulfamethoxazole – amoxicillin

Chronic Otitis Media 4 Chronic infection 4 Perforation of TM usually present 4 Mucosal changes 4 P. aeruginosa, Proteus, Staphylococcus aureus

Clinical Findings 4 Hallmark- purulent aural discharge 4 Pain- on/off 4 Conductive hearing loss

Treatment 4 Removal of debris 4 earplugs to protect against water exposure 4 ATB drops for exacerbations 4 Definitive- surgical TM repair – eliminate infection – reconstruction of TM

Cholesteatoma* 4 Special variety of chronic otitis media 4 Most common cause is prolonged auditory tube dysfunction, with resultant chronic negative middle ear pressure that draws inward the upper flaccid portion of the tympanic membrane. *see picture

Cholesteatoma 4 Creates a squamous epithelium-lined sac 4 Becomes obstructed and fills with desquamated keratin and becomes chronically infected 4 Typically erodes bone, causes destruction of nerves, may spread intracranially

Cholesteatoma 4 Physical examination – epitympanic retraction pocket or marginal tympanic membrane perforation that exudes keratin debris 4 Treatment – surgical marsupialization of the sac or its complete removal

Mastoiditis- complication of OM 4 Postauricular pain and erythema 4 Spiking fever 4 X-ray reveals coalescence of the mastoid air cells due to destruction of their bony septa 4 IV ATB and myringotomy for culture and drainage 4 Mastoidectomy if other fails. . .

Petrous apicitis- complication of OM 4 Medial portion of the petrous bone between the inner ear and clivus may become a site of persistent infection 4 Foul discharge, deep ear and retro-orbital pain, and sixth nerve palsy 4 Prolonged ATB therapy and surgical drainage

Otogenic skull base osteomylitiscomplication of OM 4 Osteomyelitis of the skull base 4 Usually due to P aeruginosa

Facial paralysis- complication of OM 4 Acute– Results from inflammation of the nerve in its middle ear segment, perhaps through bacterially secreted neurotoxins • Myringotomy for drainage and culture • IV ATB • prognosis excellent

4 Chronic – Evolves slowly due to chronic pressure on the nerve in the middle ear or mastoid by cholesteatoma – surgical correction of the underlying disease – prognosis less favorable

Sigmoid sinus thrombosis complication of OM 4 Trapped infection within the mastoid air cells adjacent to the sigmoid sinus may cause septic thrombophlebitis 4 Systemic sepsis- spiking fevers, chills 4 Increased intracranial pressure- HA, lethargy, nausea and vomiting, papilledema 4 Diagnosis- MR venography 4 Tx- IV ATB, surgical drainage

Central Nervous System Infection - complication of OM 4 Otogenic meningitis- most common intracranial complication of ear infection

Non-auditory causes of earache 4 Temporomandibular joint dysfunction – chewing (soft foods, massage) – psychogenic – dental malocclusion (dental referral) 4 Glossopharyngeal neuralgia – refractory to medical management, may respond to decompression of ninth nerve

Non-auditory causes of earache 4 Infections and neoplasia that involve the oropharynx, hypopharynx, and larynx – persistent earache demands specialty referral to exclude cancer of the upper aerodigestive tract
