EAHP 16 LYWS217 BASEL Follicular lymphoma grade 3

EAHP 16 - LYWS-217 BASEL Follicular lymphoma grade 3 B with t(8; 14)

Ludmila Boudova* 1, Pavla Veselá 1, Michal Karas 2, Petr Grossmann 1, Jana Kuntscherova 1, Pavel Jindra 2, Tomas Vanecek 1, Petr Mukensnabl 1, David Slouka, Michal 1, Ivan Subrt 3, Marketa Stenova 3 1 Pathology, 2 Hematooncology, 3 Genetics, Charles University, Medical Faculty Hospital, Pilsen, Czech Republic

Clinical history A woman, 54 ys. Past history: ulcerous colitis (dg. 2011), mesalazine, no immunosuppression Presented with an abrupt onset of symptoms and a markedly aggressive course April 2014 - enlarged cervical LN and rapidly growing bulky abdominal tumours (9 cm in the diam), massive generalized lymphadenopathy pleural effusion, massive BM infiltration, high LDH, IPI 3, stage IV. B

Therapy and outcome Aggressive: R-Hyper. CVAD, R-HIDAC + MTX, BEAM with autologous PBSCT, CHOP, 2 complete remissions a relapse in the oral cavity (gingiva) in her second CR - allogenic PBSCT She died of pneumonia in December 2015.
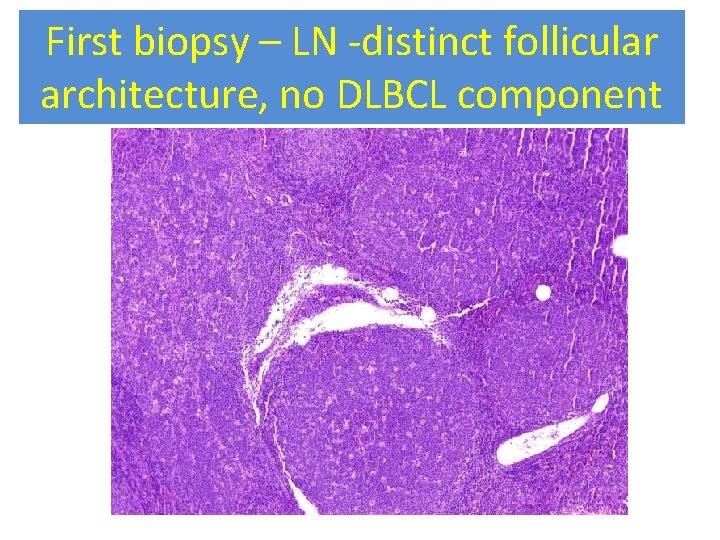
First biopsy – LN -distinct follicular architecture, no DLBCL component
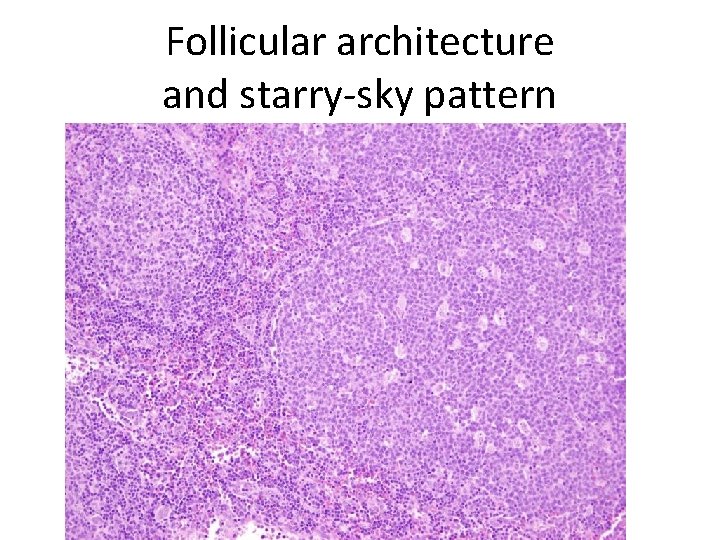
Follicular architecture and starry-sky pattern
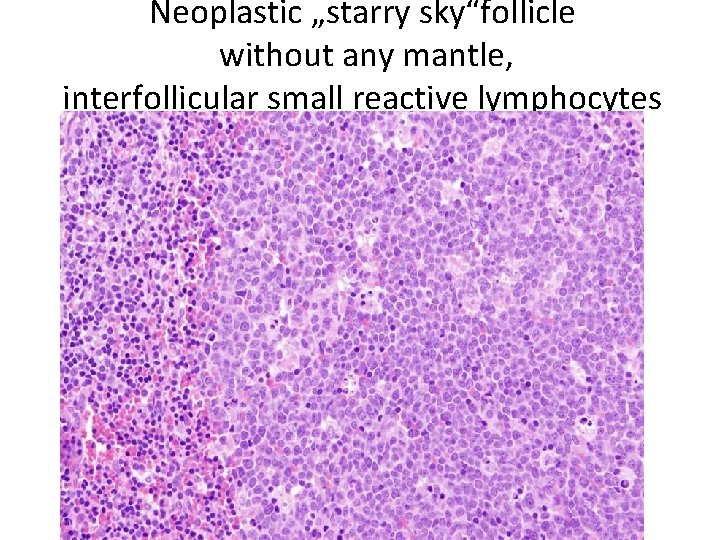
Neoplastic „starry sky“follicle without any mantle, interfollicular small reactive lymphocytes
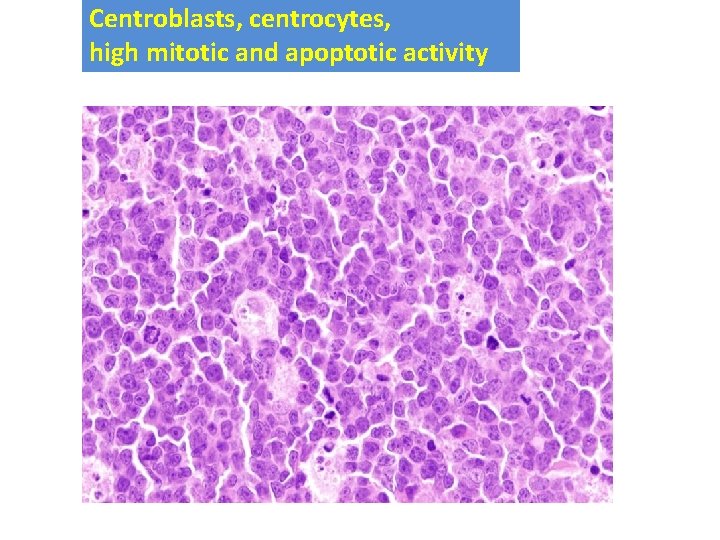
Centroblasts, centrocytes, high mitotic and apoptotic activity

Immunohistochemistry LN - neoplastic cells • Positive: CD 20, CD 79 a, PAX 5, CD 10, bcl 6, bcl 2, p 53, c-myc; Ki 67: approaching 100% • Negative: cyclin D 1, Td. T, MUM 1, CD 34, CD 30; Ig. L: slightly more kappa; polyclonal heavy chains • follicular dendritic meshworks retained only in few follicles(CD 23); a small admixture of T-cells, mainly around follicles (CD 3, CD 5) –helping make the follicular architecture very distinct
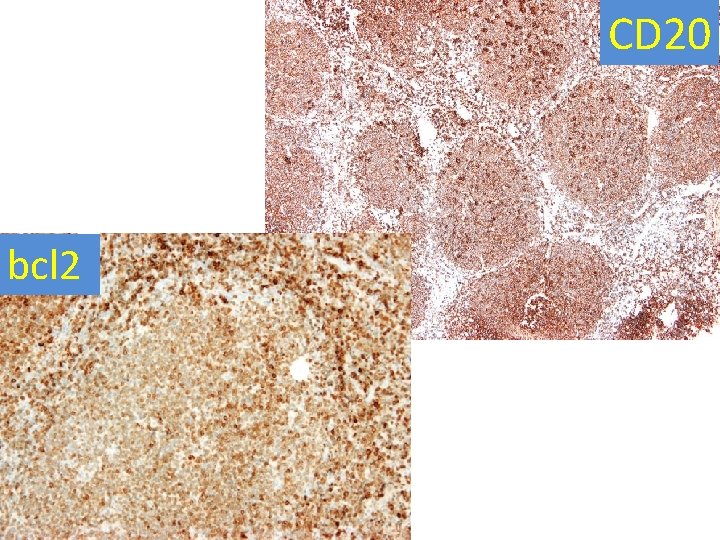
CD 20 bcl 2
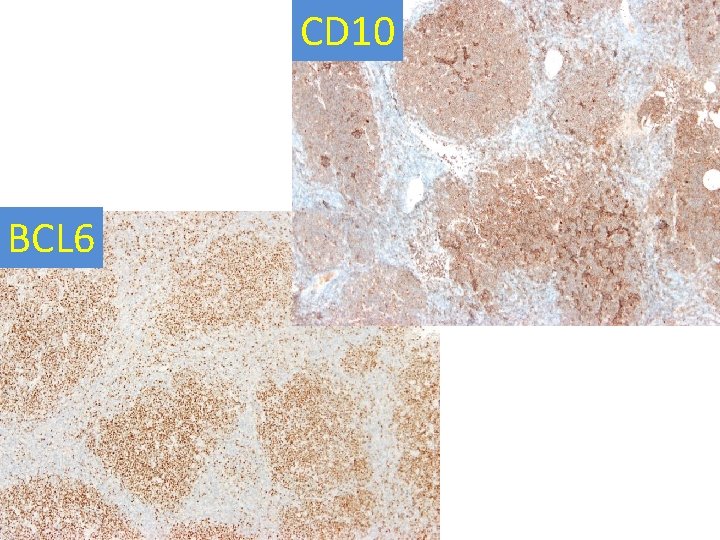
CD 10 BCL 6
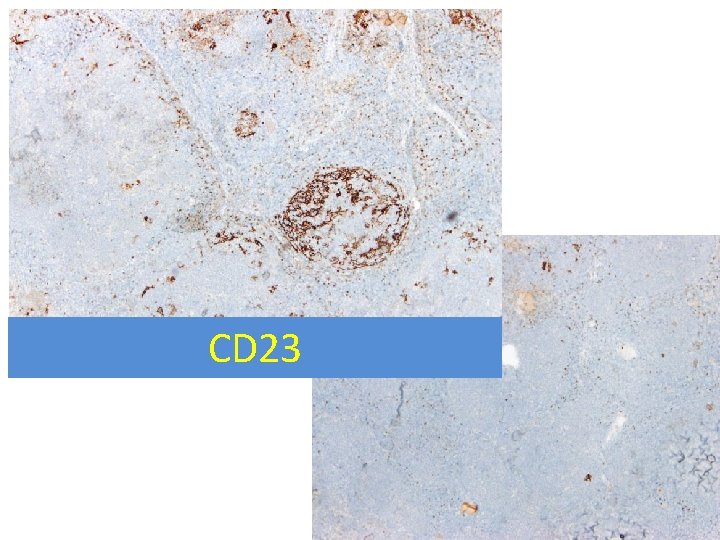
CD 23
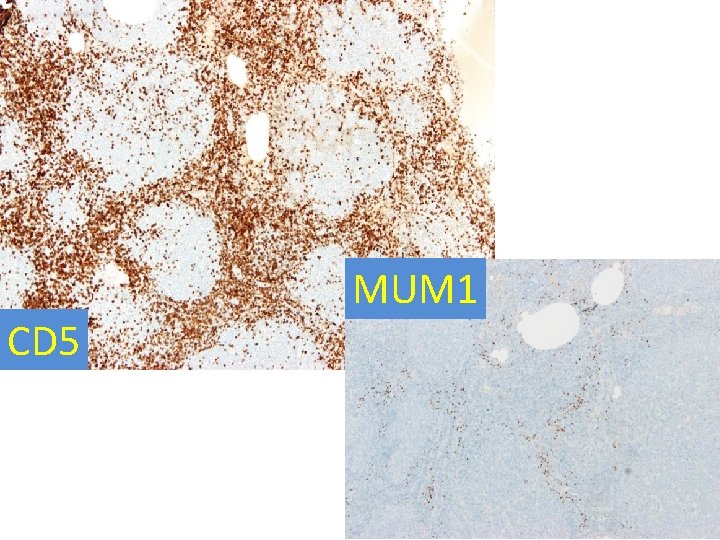
CD 5 MUM 1
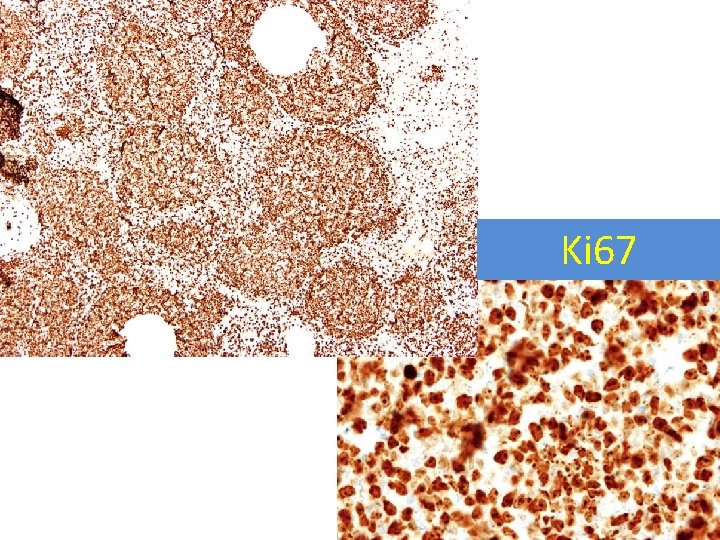
Ki 67
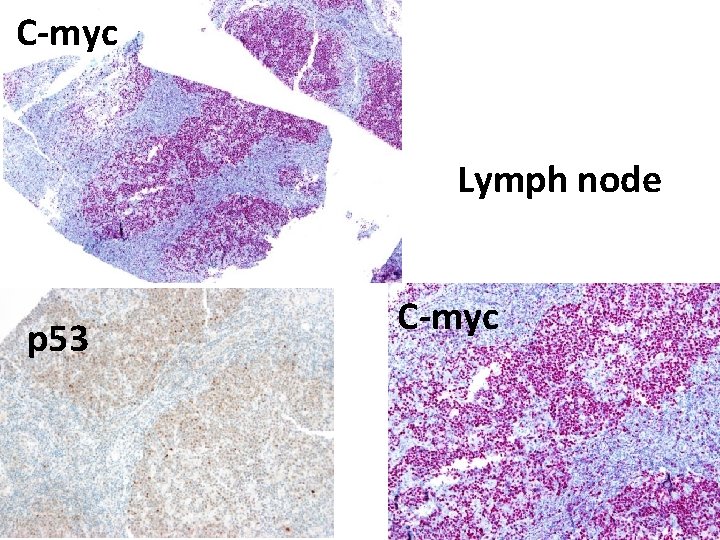
C-myc Lymph node p 53 C-myc
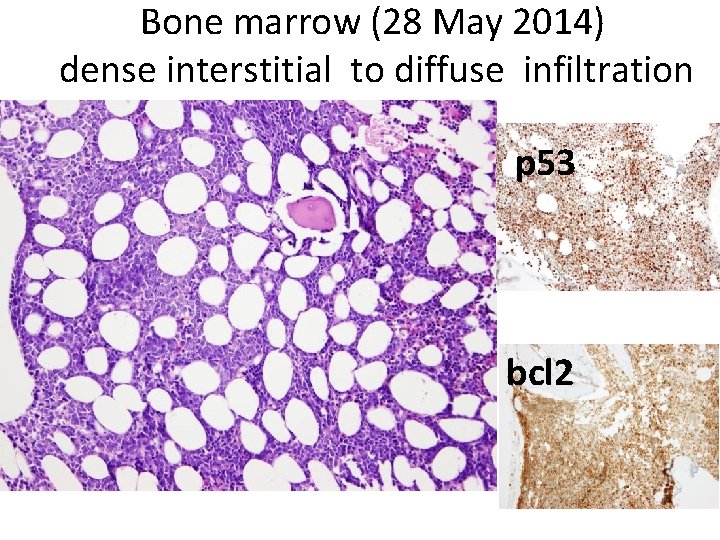
Bone marrow (28 May 2014) dense interstitial to diffuse infiltration p 53 bcl 2
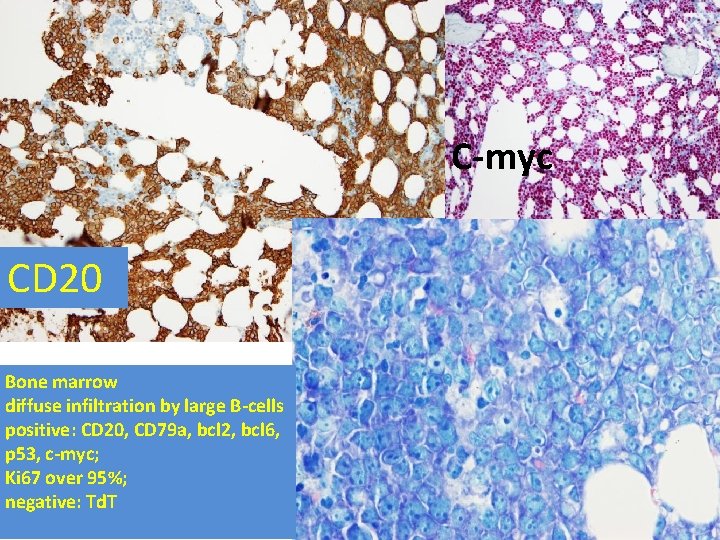
C-myc CD 20 Bone marrow diffuse infiltration by large B-cells positive: CD 20, CD 79 a, bcl 2, bcl 6, p 53, c-myc; Ki 67 over 95%; negative: Td. T
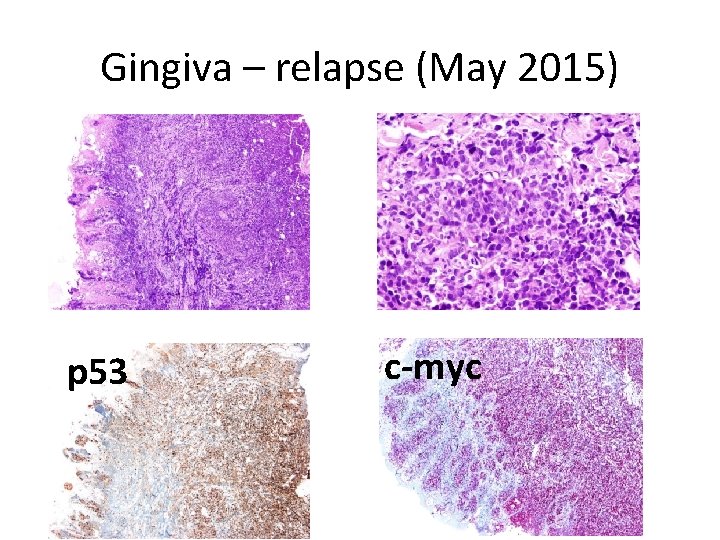
Gingiva – relapse (May 2015) p 53 c-myc

• • • Genetic studies Cytogenetics: lymph node (FFPE) - FISH - positive: t(8; 14); negative: t(11; 14); bcl 6; repeatedly not assessable (break apart, fusion probes): t(14; 18) similar: gingiva (FFPE) – relapse Bone marrow (fresh; examined in VI-VII/2014): G-banding and FISH: tumour cells: t(14; 18); t (8; 14); del TP 53, chrom. 7 trisomy Molecular studies: PCR BM - fresh - bcl 2/JHa : positive (mcr); Ig. H: clonal LN: bcl 2/Jha(mbr, mcr): negative; Ig. H: clonal Ig. H and Ig. K products – comparison same size in all three samples - Ig. K – 285 bp Ig. H – (FR 1 – 334 bp, FR 2 – 267 bp), FR 3 – 133 b • EBER ISH, EBV (PCR) – all negative (LN, BM, gingiva)

Proposed diagnosis: Lymph node: follicular lymphoma grade 3 B, with a follicular architecture - with t(8; 14); other translocations not detected possibly because of a poor technical quality of the FFPE sample Bone marrow: diffuse large B-cell lymphoma with t (8; 14), t(14; 18) del TP 53. chrom. 7 trisomy - transformation of FL Gingiva – relapse of DLBCL

Interesting feature(s) of submitted case: • Clinical: an abrupt onset of symptoms – • a very aggressive presentation, rapidly growing large tumours (“growing like a Burkitt lymphoma…“) • Pathological: follicular lymphoma grade 3 B without DLBCL – as found in the initial LN is relatively rare • t(8; 14) in FL g. 3 B is rare - found in 13 -20%; found in a similar percentage of FL of all grades • (Horn 2011, Bosga – Bouwer; Au, Mohamed; Offit)

• C-myc breaks in FL rare • 40% of lymphomas with dual myc/bcl 2 have a history of FL • 50% of lymphomas with c-myc rearrangement are DHL – DLBCL, Burkitt, to a lesser extent FL • c-myc - involved in transformation may be an adverse prognostic indicator. Differential diagnosis: • FL, blastoid and FL 3 B should differ in the cytology of tumour cells, but share some immunomorphological and genetic features (e. g. starry sky pattern, very high mitotic and proliferative rate, some genetic changes) • Burkitt lymphoma with a follicular growth pattern

Transformation – possible scenarios: 1. FL is usually known to have been present for years before it transforms to DLBCL. The transformation of FL occurs in 3% of cases per year over the first 15 ys of observation, most commonly to DLBCL 2. There may be patients who have LN with FL for some time and go undiagnosed until the transformation - which may draw attention by clinical worsening

Remark: • Our patient went to see her doctors frequently ( gastroenterologist; gymaecologist) years before the presentation of lymphoma The lymphoma probably started to grow very rapidly which is unusual but we cannot generally exclude that some lymph nodes with a lymphoma in an indolent phase may have escaped medical attention
- Slides: 24