e Ed E60 Spectrum of Cavernous Malformations Anthony




- Slides: 31

e. Ed. E-60 Spectrum of Cavernous Malformations Anthony Abou Karam MD, Nassim Akle MD, Luis Ramos MD, Jose Gavito MD, Bryan Foley MD Department of Radiology, Texas Tech University Health Sciences Center El Paso, TX

Disclosures: None

OBJECTIVES: This educational exhibit will present common and uncommon cavernous malformations to better understand their appearance, locations, and clinical issues when encountered. Cases will be presented as an interactive learning session with images, description, key facts, and differential diagnosis when applicable.

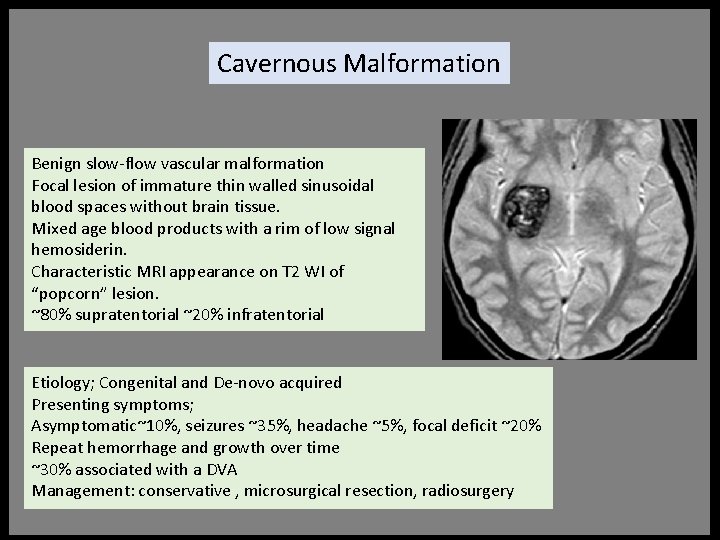
Cavernous Malformation Benign slow-flow vascular malformation Focal lesion of immature thin walled sinusoidal blood spaces without brain tissue. Mixed age blood products with a rim of low signal hemosiderin. Characteristic MRI appearance on T 2 WI of “popcorn” lesion. ~80% supratentorial ~20% infratentorial Etiology; Congenital and De-novo acquired Presenting symptoms; Asymptomatic~10%, seizures ~35%, headache ~5%, focal deficit ~20% Repeat hemorrhage and growth over time ~30% associated with a DVA Management: conservative , microsurgical resection, radiosurgery

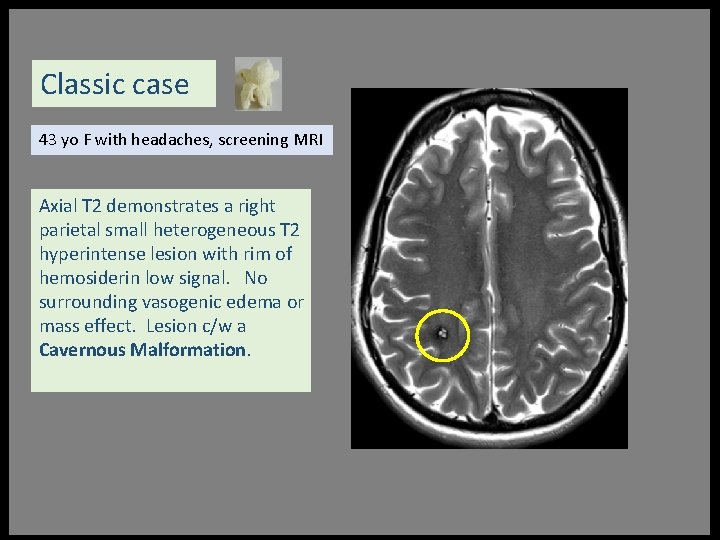
Classic case 43 yo F with headaches, screening MRI Axial T 2 demonstrates a right parietal small heterogeneous T 2 hyperintense lesion with rim of hemosiderin low signal. No surrounding vasogenic edema or mass effect. Lesion c/w a Cavernous Malformation.

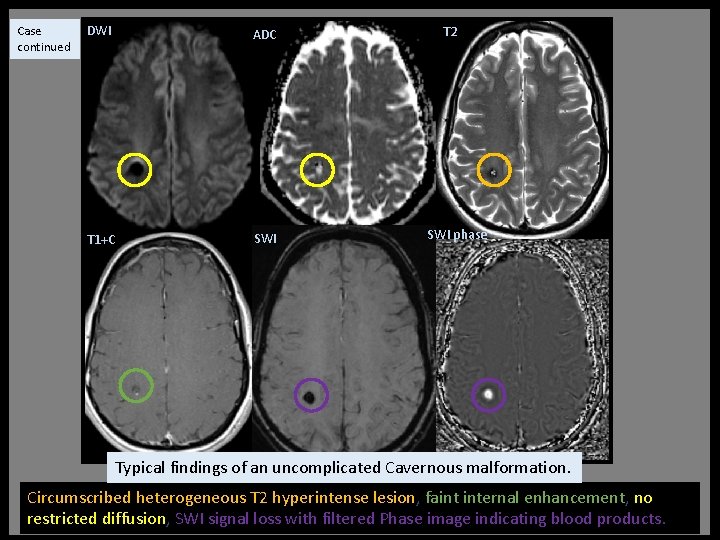
Case continued DWI ADC T 1+C SWI T 2 SWI phase Typical findings of an uncomplicated Cavernous malformation. Circumscribed heterogeneous T 2 hyperintense lesion, faint internal enhancement, no restricted diffusion, SWI signal loss with filtered Phase image indicating blood products.

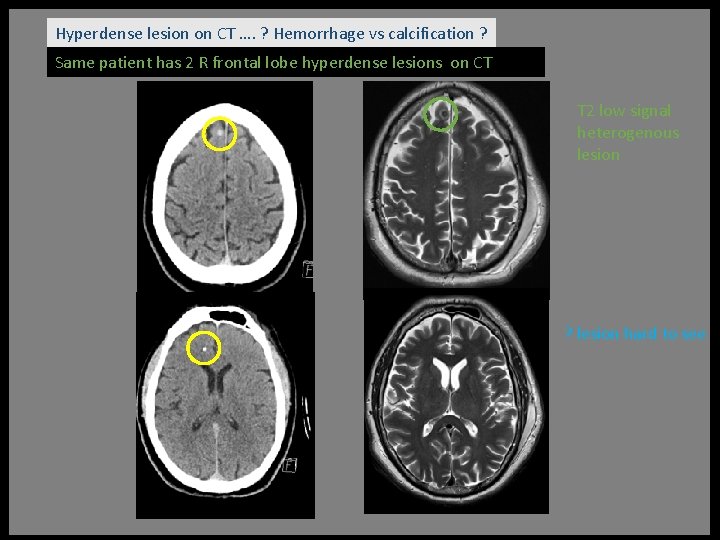
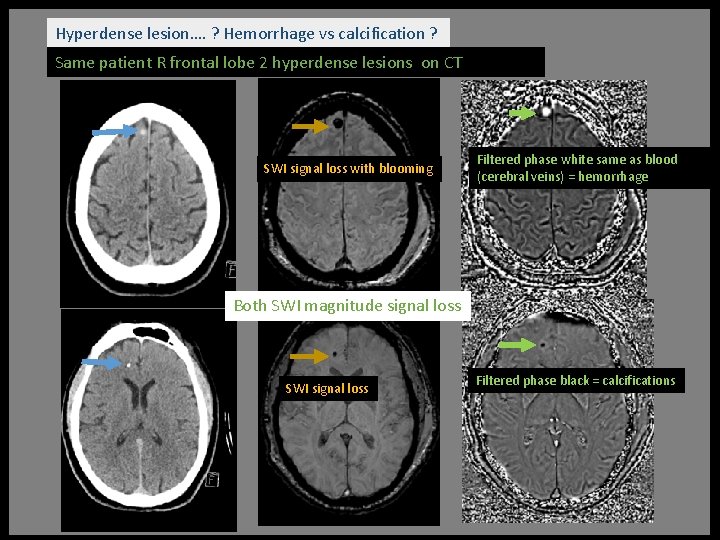
Hyperdense lesion on CT …. ? Hemorrhage vs calcification ? Same patient has 2 R frontal lobe hyperdense lesions on CT T 2 low signal heterogenous lesion ? lesion hard to see

Hyperdense lesion…. ? Hemorrhage vs calcification ? Same patient R frontal lobe 2 hyperdense lesions on CT SWI signal loss with blooming Filtered phase white same as blood (cerebral veins) = hemorrhage Both SWI magnitude signal loss SWI signal loss Filtered phase black = calcifications

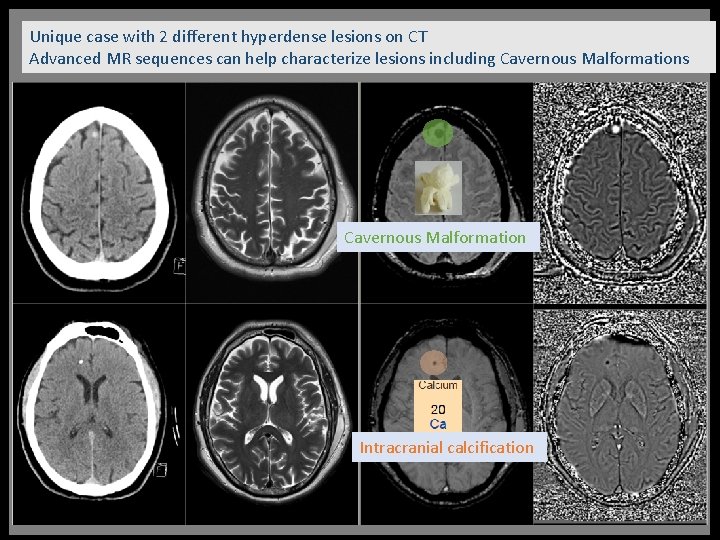
Unique case with 2 different hyperdense lesions on CT Advanced MR sequences can help characterize lesions including Cavernous Malformations Cavernous Malformation Intracranial calcification

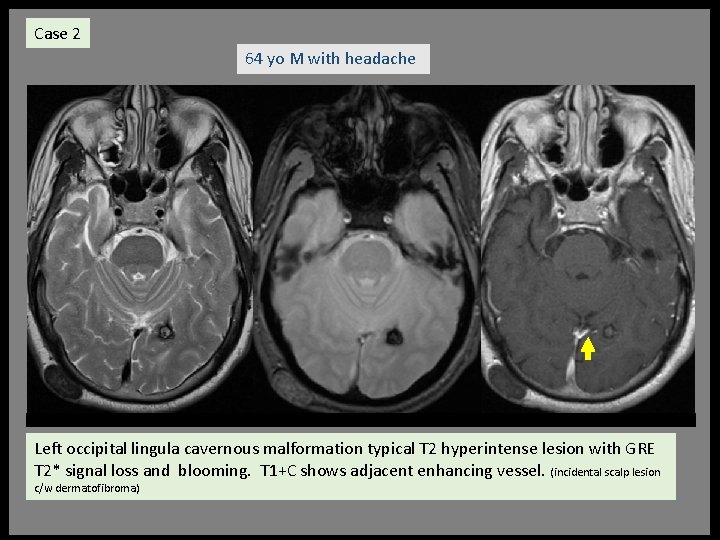
Case 2 64 yo M with headache Left occipital lingula cavernous malformation typical T 2 hyperintense lesion with GRE T 2* signal loss and blooming. T 1+C shows adjacent enhancing vessel. (incidental scalp lesion c/w dermatofibroma)

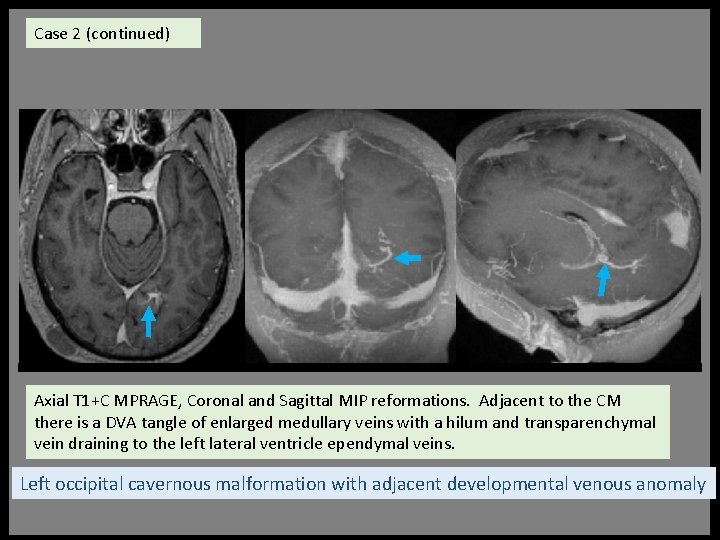
Case 2 (continued) Axial T 1+C MPRAGE, Coronal and Sagittal MIP reformations. Adjacent to the CM there is a DVA tangle of enlarged medullary veins with a hilum and transparenchymal vein draining to the left lateral ventricle ependymal veins. Left occipital cavernous malformation with adjacent developmental venous anomaly

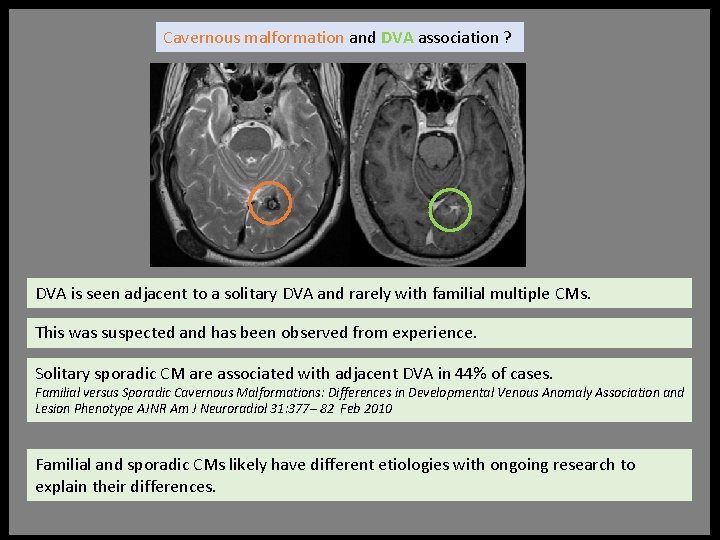
Cavernous malformation and DVA association ? DVA is seen adjacent to a solitary DVA and rarely with familial multiple CMs. This was suspected and has been observed from experience. Solitary sporadic CM are associated with adjacent DVA in 44% of cases. Familial versus Sporadic Cavernous Malformations: Differences in Developmental Venous Anomaly Association and Lesion Phenotype AJNR Am J Neuroradiol 31: 377– 82 Feb 2010 Familial and sporadic CMs likely have different etiologies with ongoing research to explain their differences.

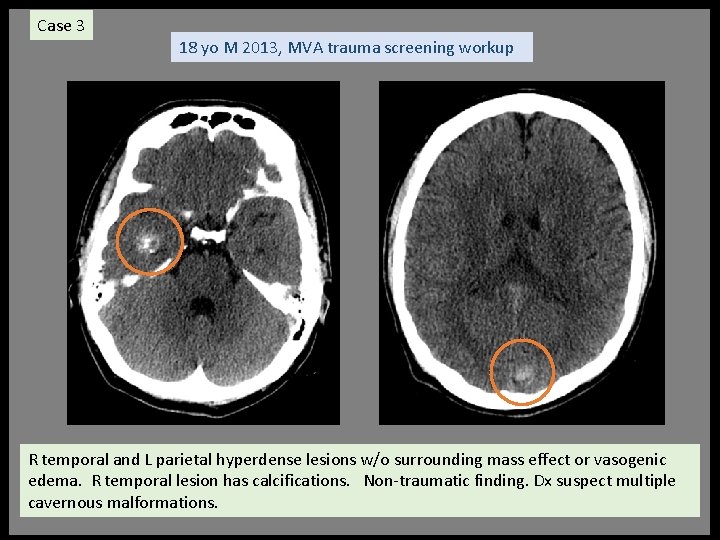
Case 3 18 yo M 2013, MVA trauma screening workup R temporal and L parietal hyperdense lesions w/o surrounding mass effect or vasogenic edema. R temporal lesion has calcifications. Non-traumatic finding. Dx suspect multiple cavernous malformations.

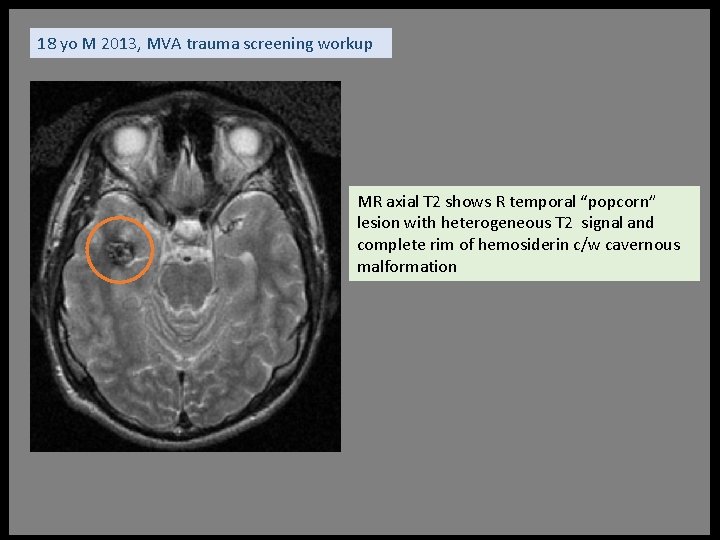
18 yo M 2013, MVA trauma screening workup MR axial T 2 shows R temporal “popcorn” lesion with heterogeneous T 2 signal and complete rim of hemosiderin c/w cavernous malformation

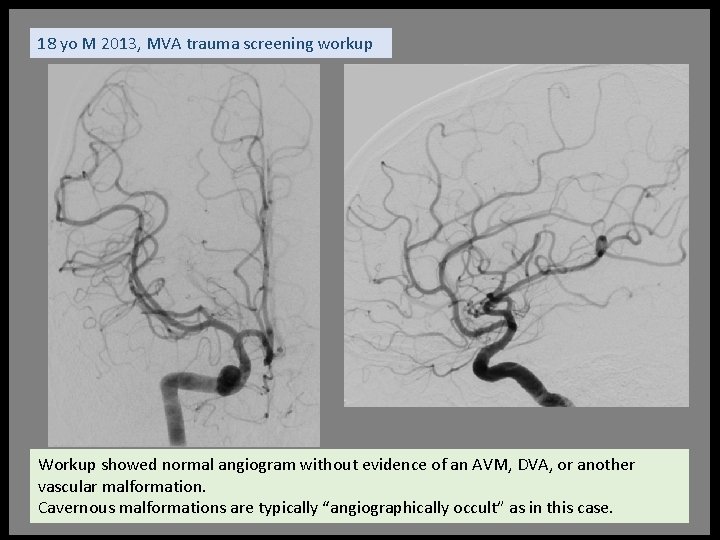
18 yo M 2013, MVA trauma screening workup Workup showed normal angiogram without evidence of an AVM, DVA, or another vascular malformation. Cavernous malformations are typically “angiographically occult” as in this case.

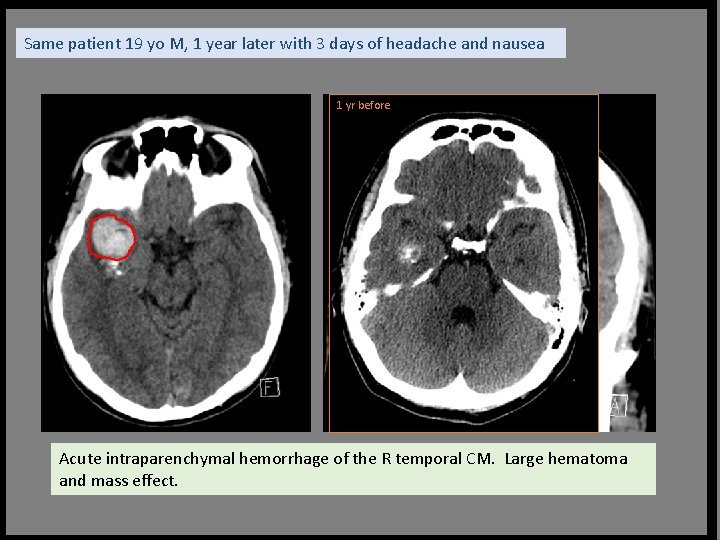
Same patient 19 yo M, 1 year later with 3 days of headache and nausea 1 yr before Acute intraparenchymal hemorrhage of the R temporal CM. Large hematoma and mass effect.

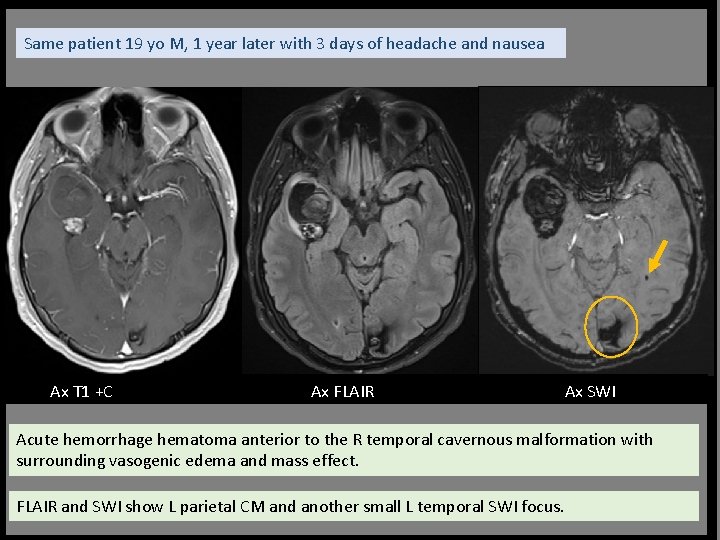
Same patient 19 yo M, 1 year later with 3 days of headache and nausea Ax T 1 +C Ax FLAIR Ax SWI Acute hemorrhage hematoma anterior to the R temporal cavernous malformation with surrounding vasogenic edema and mass effect. FLAIR and SWI show L parietal CM and another small L temporal SWI focus.

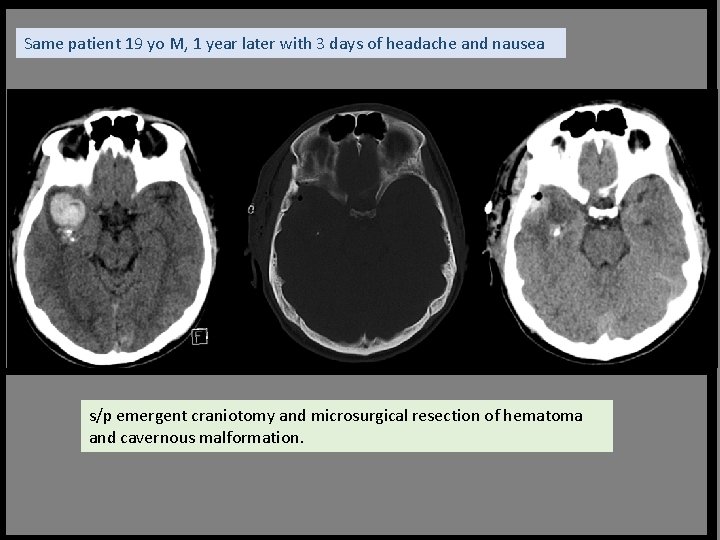
Same patient 19 yo M, 1 year later with 3 days of headache and nausea s/p emergent craniotomy and microsurgical resection of hematoma and cavernous malformation.

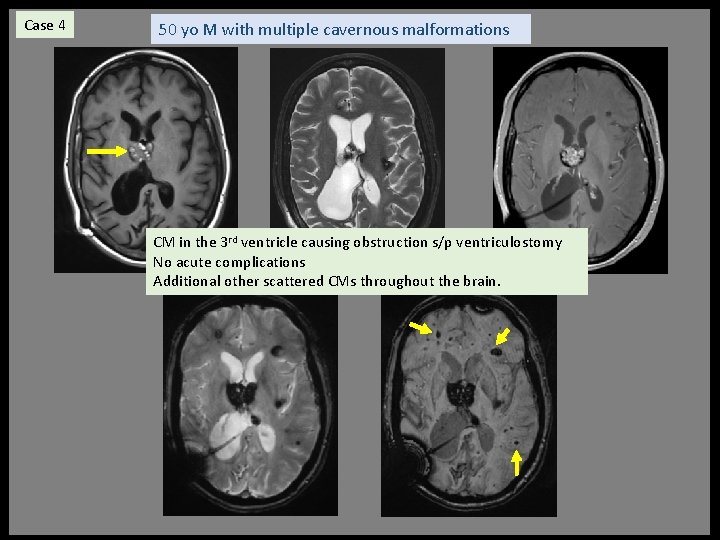
Case 4 50 yo M with multiple cavernous malformations CM in the 3 rd ventricle causing obstruction s/p ventriculostomy No acute complications Additional other scattered CMs throughout the brain.

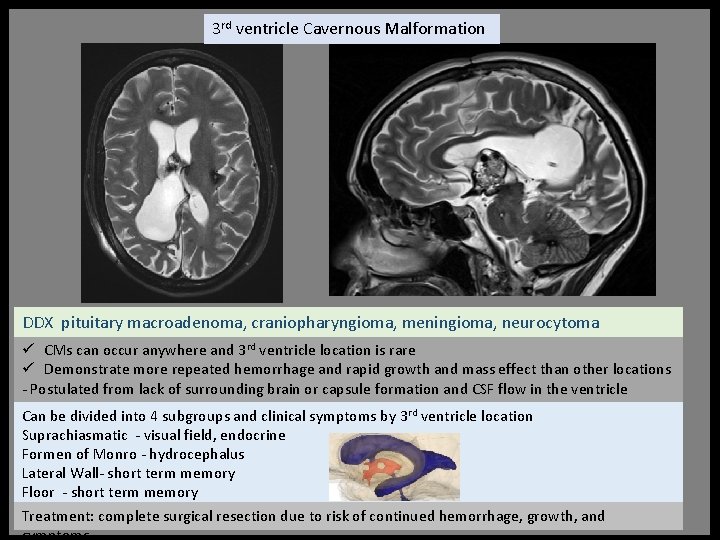
3 rd ventricle Cavernous Malformation DDX pituitary macroadenoma, craniopharyngioma, meningioma, neurocytoma ü CMs can occur anywhere and 3 rd ventricle location is rare ü Demonstrate more repeated hemorrhage and rapid growth and mass effect than other locations - Postulated from lack of surrounding brain or capsule formation and CSF flow in the ventricle Can be divided into 4 subgroups and clinical symptoms by 3 rd ventricle location Suprachiasmatic - visual field, endocrine Formen of Monro - hydrocephalus Lateral Wall- short term memory Floor - short term memory Treatment: complete surgical resection due to risk of continued hemorrhage, growth, and

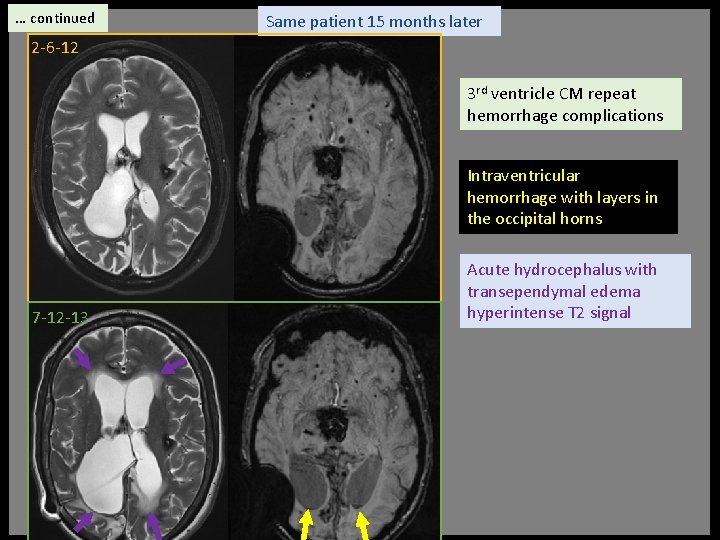
… continued Same patient 15 months later 2 -6 -12 3 rd ventricle CM repeat hemorrhage complications Intraventricular hemorrhage with layers in the occipital horns 7 -12 -13 Acute hydrocephalus with transependymal edema hyperintense T 2 signal

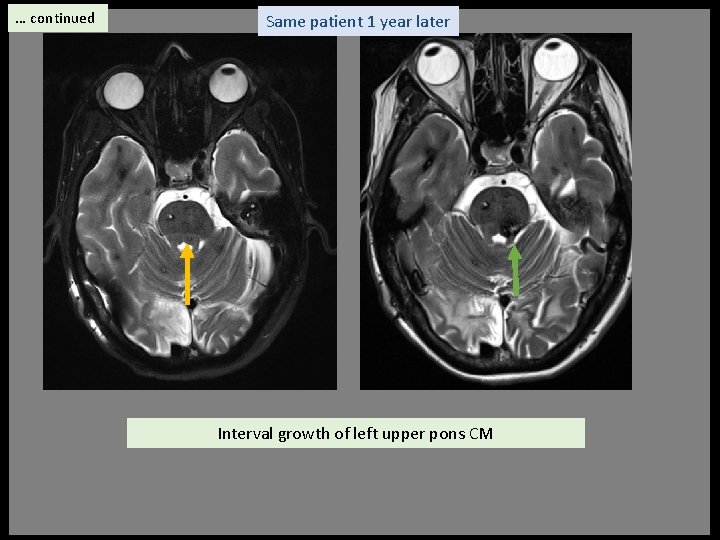
… continued Same patient 1 year later Interval growth of left upper pons CM

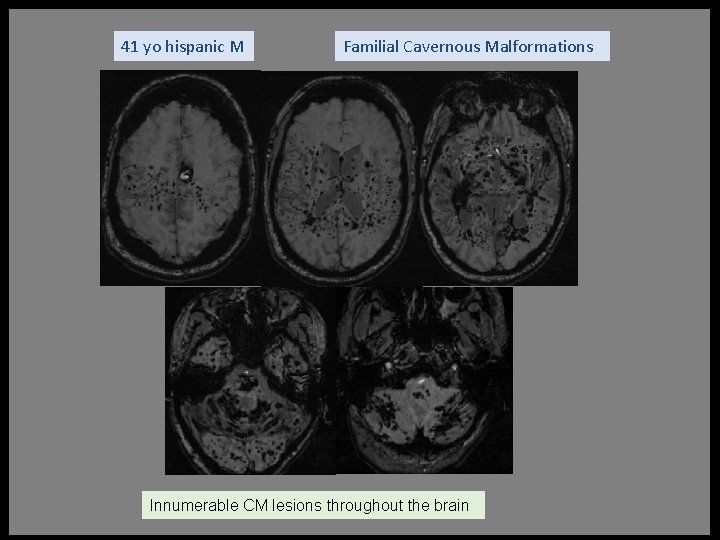
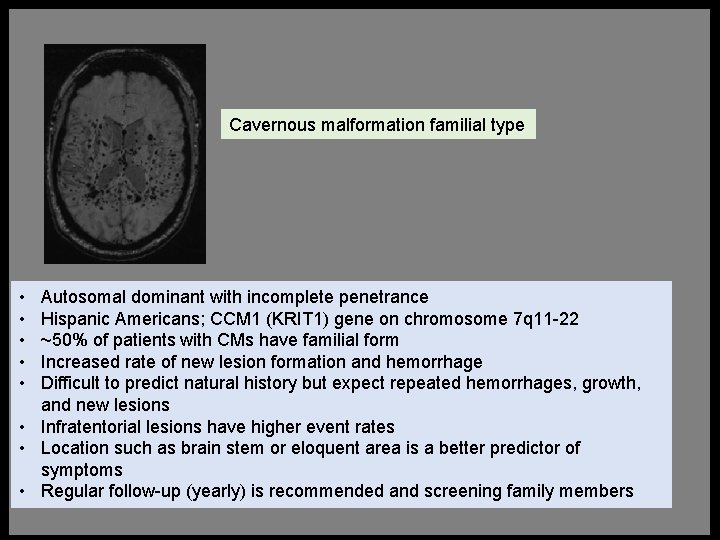
41 yo hispanic M Familial Cavernous Malformations Innumerable CM lesions throughout the brain

Cavernous malformation familial type • • • Autosomal dominant with incomplete penetrance Hispanic Americans; CCM 1 (KRIT 1) gene on chromosome 7 q 11 -22 ~50% of patients with CMs have familial form Increased rate of new lesion formation and hemorrhage Difficult to predict natural history but expect repeated hemorrhages, growth, and new lesions • Infratentorial lesions have higher event rates • Location such as brain stem or eloquent area is a better predictor of symptoms • Regular follow-up (yearly) is recommended and screening family members

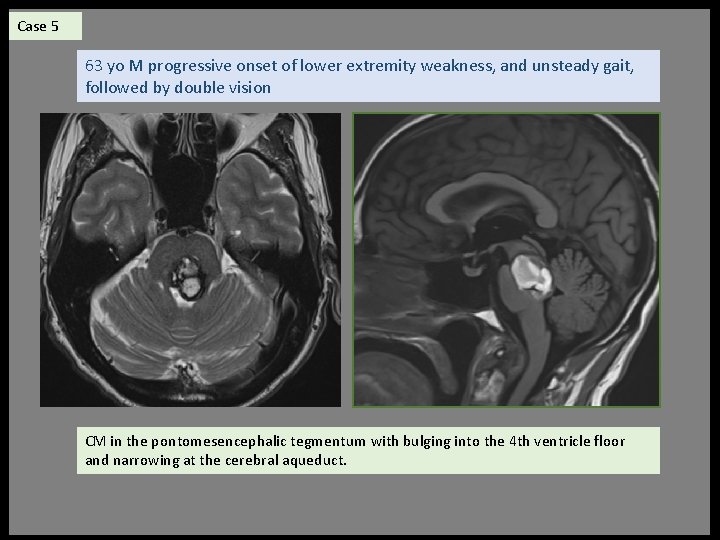
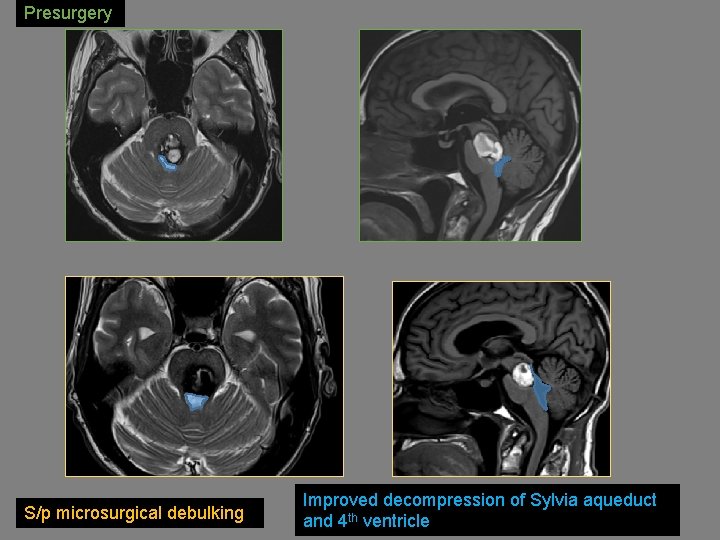
Case 5 63 yo M progressive onset of lower extremity weakness, and unsteady gait, followed by double vision CM in the pontomesencephalic tegmentum with bulging into the 4 th ventricle floor and narrowing at the cerebral aqueduct.

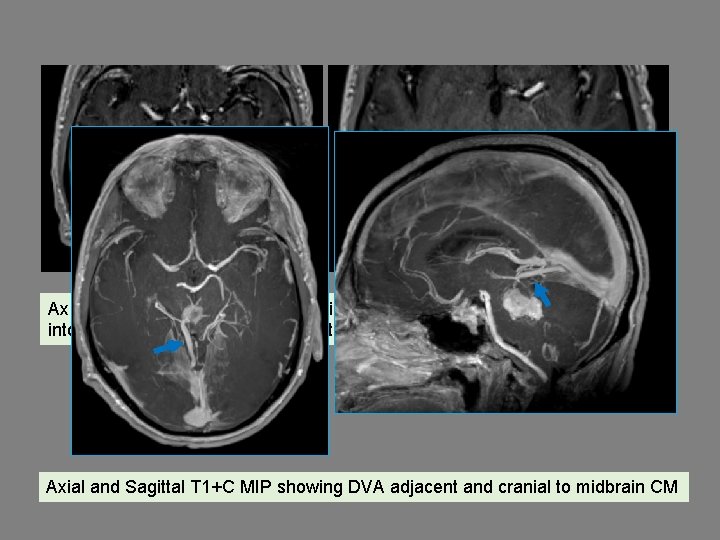
Ax T 1+C demonstrates a DVA cranial to the CM with draining collector veins into a dilated L basal vein of Rosenthal. Axial and Sagittal T 1+C MIP showing DVA adjacent and cranial to midbrain CM

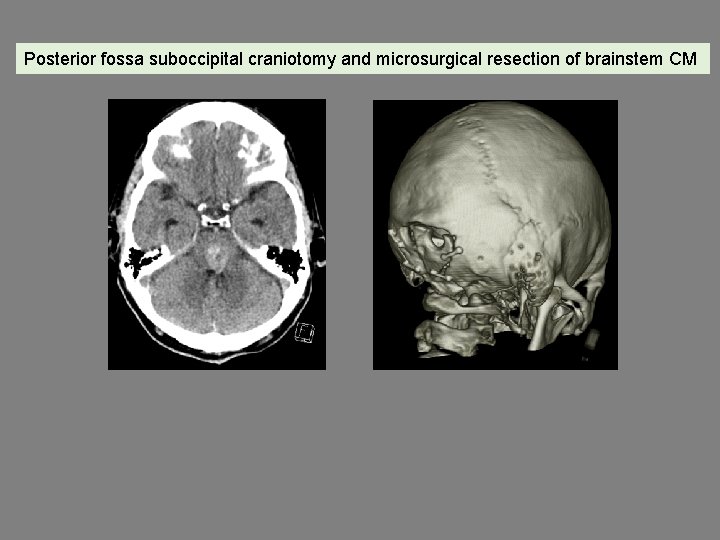
Posterior fossa suboccipital craniotomy and microsurgical resection of brainstem CM

Presurgery S/p microsurgical debulking Improved decompression of Sylvia aqueduct and 4 th ventricle

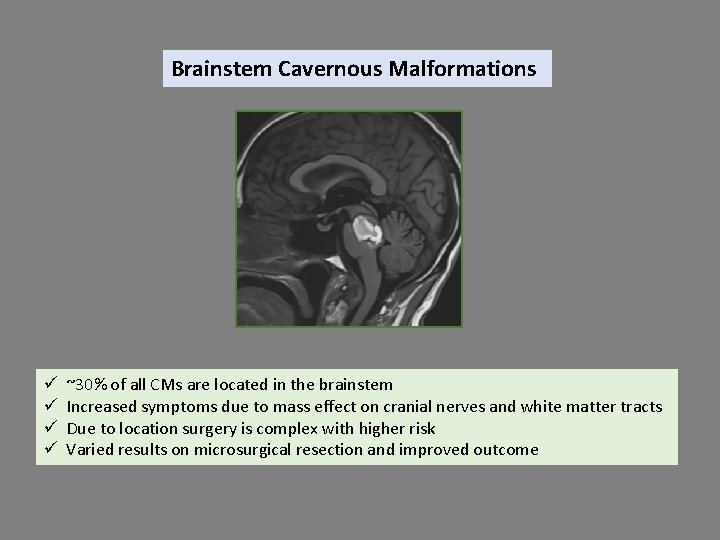
Brainstem Cavernous Malformations ü ü ~30% of all CMs are located in the brainstem Increased symptoms due to mass effect on cranial nerves and white matter tracts Due to location surgery is complex with higher risk Varied results on microsurgical resection and improved outcome

Cavernous Malformations Summary ü CMs can be encountered frequently during routine brain MR imaging. ü Knowledge of appearance, locations such as intraventricular and brainstem, and clinical course of repeated hemorrhage and growth are important for accurate diagnosis and follow-up imaging. ü Familial CMs have multiple lesions that increase over time in location and may change appearance with hemorrhages. ü SWI sequences can be helpful for problem solving, better lesion conspicuity, and follow-up. ü Associated DVAs and CMs occur more frequently with solitary lesions. ü Future research and knowledge is ongoing to better understand their etiology, natural history, and treatment options.

References 1. Rivera PP et al. Intracranial cavernous malformations. Neuroimag Clin N Am 13 (2003) 27– 40. 2. Tong KA, Ashwal S, Obenaus A, et al. Susceptibility-weighted MR imaging: a review of clinical applications in children. AJNR Am J Neuroradiol 2008; 29: 9– 17 3. Latchaw RE, Truwit CL, Heros, RC. Venous Angioma, Cavernous Angioma, and Hemorrhage, Commentary. AJNR 15: 12551257. 4. Sinson G, Zager E, Grossman R, et al. Cavernous malformations of the third ventricle. Neurosurgery 1995; 37: 37– 41. 5. Katayama, Y et al. Surgical management of cavernous malformations of the third ventricle. J Neurosurg. 80: 64 -72, 1994. 6. Rigamonti D, et al. Cerebral Cavernous Malformations Incidence and Familial Occurrence. NEJM 319: 6 (1998) 343 -347. Kattapong VJ et al. Familial cerebral cavernous angiomas: Clinical and radiologic studies Neurology. 1995; 45: 492 -497 8. Porter P, Willinsky R, Harper W, et al. Cerebral cavernous malformations: natural history and prognosis after clinical deterioration with or without hemorrhage. J Neurosurg 1997; 87: 190– 7. 9. Peterson TA, et al. Familial versus Sporadic Cavernous Malformations: Differences in Developmental Venous Anomaly Association and Lesion Phenotype. AJNR 31: 377 -82. 10. Dalyau RT, et al. Management of incidental cavernous malformations: a review. Neurosurgical Focus vol. 31, no. 6, article E 5, 2011. Frischer JM, et al. Microsurgery and radiosurgery for brainstem cavernomas: effective and complementary treatment options. World. Neurosurgery, vol. 81, no. 3 -4, pp. 520– 528, 2014.