Dyslipidemia in Children and Adolescents When and How
















































- Slides: 55

Dyslipidemia in Children and Adolescents: When and How to Diagnose and Treat NJ AAP Annual Conference June 9 th, 2021 Julie Brothers, MD Medical Director, Lipid Heart Clinic Medical Co-Director, Preventive Cardiovascular Program Associate Professor, Pediatrics, Division of Cardiology

Disclosures • None

Learning Objectives • Describe the NHLBI screening guidelines for dyslipidemia in children and adolescents • Understand diet and lifestyle treatment options for children and adolescents with dyslipidemia • Identify which patients would qualify for statin therapy and how to initiate statins • Discuss treatment strategies for patients with hypertriglyceridemia


Clinical Case I • 13 year old male • Screened because of family history of hypercholesterolemia and premature cardiovascular disease (CVD) • Father with hypercholesterolemia with myocardial infarction at 41 years, s/p CABG • Paternal grandfather with hypercholesterolemia and coronary stents x 2 at age 52 years • 15 yo brother with hypercholesterolemia, treated with statin

Clinical Case II • 10 year old female • Screened due to increasing BMI over the past 2 years • Father overweight • Mother with h/o obesity, now s/p gastric bypass surgery • Maternal uncle treated for hypertriglyceridemia • No early CVD

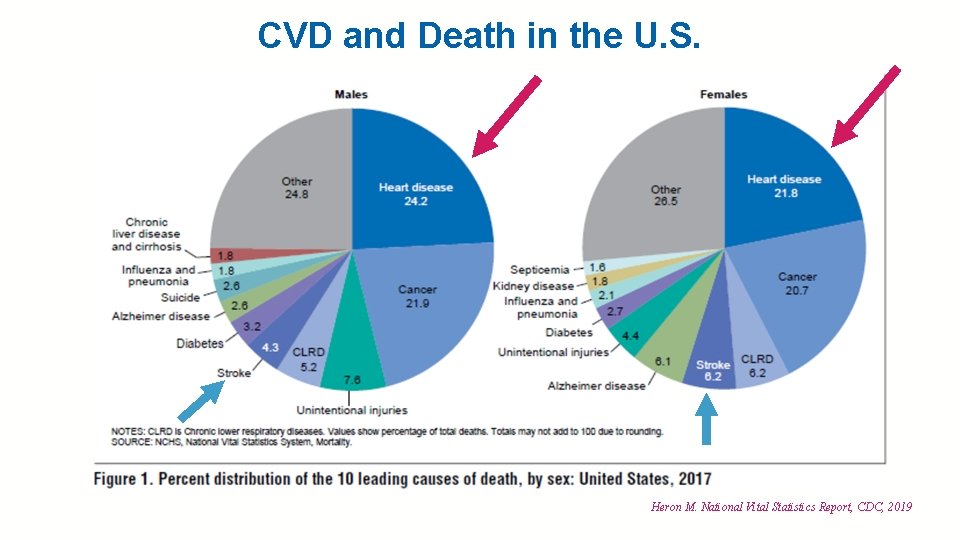
CVD and Death in the U. S. It begins in childhood Heron M. National Vital Statistics Report, CDC, 2019

Children with Hypercholesterolemia and CVD Risk • Cholesterol is the major component of advanced atherosclerotic plaques • There is a strong, positive correlation between serum cholesterol levels and CVD • As number of CV risk factors increase so does the severity of asymptomatic coronary and aortic atherosclerosis starting in childhood • Children with high cholesterol are likely to become adults with high cholesterol Lipid Research Clinics Program JAMA 1984; Kwiterovich Jr, et al J Clin Invest 1974; Slack, et al. , Lancet 1969, Benson et al N Eng J Med 1998

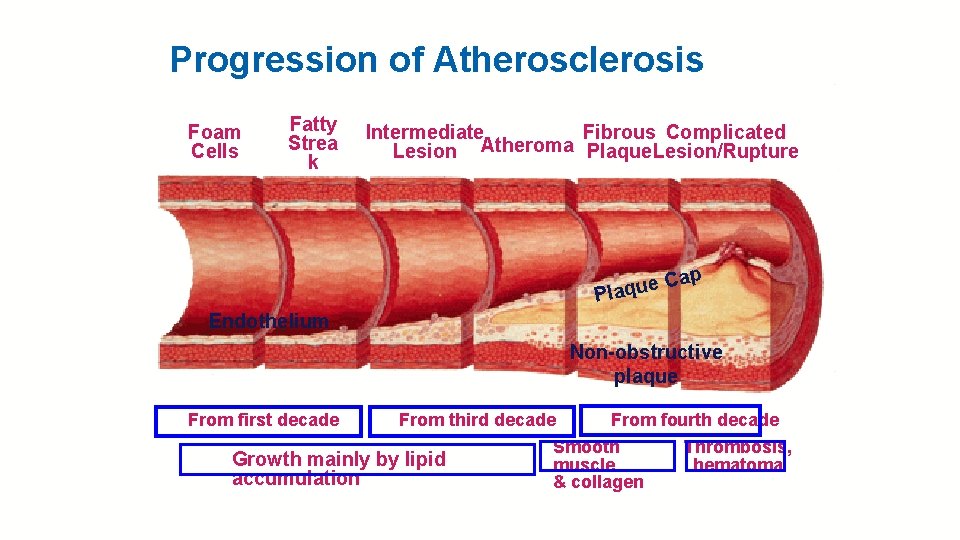
Progression of Atherosclerosis Foam Cells Fatty Strea k Intermediate Fibrous Complicated Lesion Atheroma Plaque. Lesion/Rupture p e Ca u q a l P Endothelium Non-obstructive plaque From first decade From third decade Growth mainly by lipid accumulation From fourth decade Smooth muscle & collagen Thrombosis, hematoma

2019 • Using National Health and Nutrition Examination Surveys (NHANES) from 1999 -2016, the authors examined trends in lipids and apolipoprotein B levels • Cross-sectional analysis

• Favorable temporal trends were noted in mean levels and in the distribution of ideal and adverse levels of HDL, non-HDL and TC • However, 19%-25% of all youths still had at least one abnormal lipid level at the end of the study period

Definitions • LDL-C (low density lipoprotein; “bad or L=lousy”) – Formed from VLDL or chylomicrons – Saturated, trans fats increase LDL-c – Major carrier of cholesterol into body tissues • HDL-C (high density lipoprotein; “good or H=heart healthy”) – Synthesized in liver and gut – Major carrier of cholesterol away from body tissues • Triglycerides (TG) – Major form of fat in body • Non-HDL-C* – Includes all atherogenic apolipoprotein B-containing lipoproteins: VLDL, intermediate-density lipoprotein (IDL), LDL, and lipoprotein(a)

NHLBI Screening Guidelines • Integrated age-specific cardiovascular risk reduction guidelines published 12/2011 • • Lipids and lipoproteins—Universal Screening Overweight/obesity Hypertension Diabetes mellitus and metabolic syndrome Nutrition/diet Physical activity Tobacco Kavey REW, Simons-Morton DG, de Jesus JM and the Expert Panel. Pediatrics 2011; 128: S 1 -44.

Rationale for Universal Screening • Early atherosclerosis exists in young patients with elevated cholesterol • Early treatment of CVD risk factors in youth is effective • Lipid disorders are common in children • Increasing with overweight and obesity • Screening with family history alone misses 30 -60% of children with dyslipidemia Kavey REW, Simons-Morton DG, de Jesus JM and the Expert Panel. . Pediatrics 2011; 128: S 1 -44.

Laboratory Testing • Non-fasting lipid profile (non-FLP) • Total-C, HDL-C –Calculate Non-HDL-C = Total cholesterol – HDL-C OR • 12 -hr fasting lipid profile (FLP) • Total-C, HDL-C, TG • If fasting TG < 400 mg/d. L: –Calculate LDL = (Total-C) – (HDL-C) – (TG/5) • If fasting TG ≥ 400 mg/d. L –Calculate Non-HDL-C = Total cholesterol – HDL-C

Why Use Non-HDL-C to Screen • Accurate in a non-fasting state • In adults: – Non-HDL-C = better predictor of CV events than LDL-C • In children: – Non-HDL-C and LDL-C are equally good predictors of adult lipid levels • In epidemiologic studies: – Non-HDL-C correlates with raised lesions and subclinical atherosclerosis on vascular imaging in childhood and at autopsy

When and How to Screen for Dyslipidemia

Lipid Screening < Age 2 years • No lipid screening

Lipid Screening: Ages 2 -8 years • No Routine Screening • Measure FLP twice & average results if child has: • Parent with total cholesterol ≥ 240 mg/dl • Premature CVD in 1 st or 2 nd degree relatives – < 55 years males and <65 years females • Diabetes (Type I or II) • Hypertension • BMI > 95 th percentile • Second hand smoke exposure • Chronic/end-stage kidney disease/post-renal transplant • Post-orthotopic heart transplantation • Kawasaki disease, with current or regressed aneurysm • Chronic inflammatory disease • HIV infection • Nephrotic syndrome Kavey REW et al. Pediatrics 2011; 128: S 1 -44

Lipid Screening: Ages 9 -11 years • Universal Screening • Measure once between 9 -11 years • If measured with Non-FLP: • Obtain FLP twice if • non-HDL ≥ 145 mg/d. L • HDL< 40 mg/d. L • If measured with FLP: OR • Repeat FLP if • LDL-C ≥ 130 mg/d. L • non-HDL-C ≥ 145 mg/d. L • HDL-C < 40 mg/d. L • TG ≥ 100 mg/d. L (< 10 yrs) or TG ≥ 130 mg/d. L (≥ 10 yrs)

Lipid Screening: Ages 12 -16 years • No routine screening • If new knowledge of CV risk (same as 2 -8 years), measure FLP twice and average results

Lipid Screening: 17 -21 years Universal Screening Measure once between 17 -21 years: Ages 17 -19 yrs • Non-FLP: • Obtain FLP twice if Ages 20 -21 yrs • Non-FLP: • Obtain FLP twice if • non-HDL ≥ 190 mg/d. L • HDL< 40 mg/d. L • non-HDL ≥ 145 mg/d. L • HDL< 40 mg/d. L • FLP: OR • Repeat if • LDL-C ≥ 130 mg/d. L • non-HDL-C ≥ 145 mg/d. L • HDL-C <40 mg/d. L • TG ≥ 130 mg/d. L • FLP: OR • Repeat if • LDL-C ≥ 160 mg/d. L • non-HDL-C ≥ 190 mg/d. L • HDL-C <40 mg/d. L • TG ≥ 150 mg/d. L

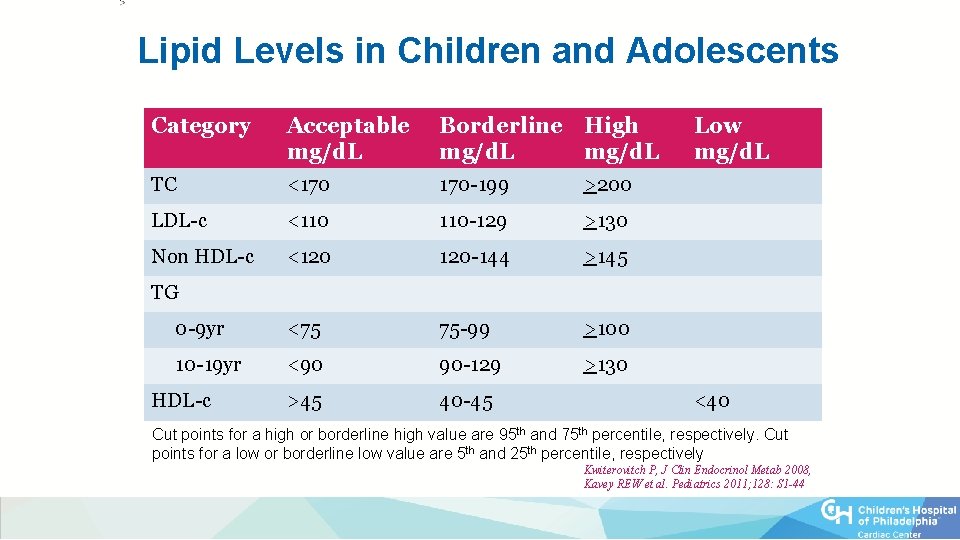
Lipid Levels in Children and Adolescents Category Acceptable mg/d. L Borderline High mg/d. L TC <170 170 -199 >200 LDL-c <110 110 -129 >130 Non HDL-c <120 120 -144 >145 0 -9 yr <75 75 -99 >100 10 -19 yr <90 90 -129 >130 >45 40 -45 Low mg/d. L TG HDL-c <40 Cut points for a high or borderline high value are 95 th and 75 th percentile, respectively. Cut points for a low or borderline low value are 5 th and 25 th percentile, respectively Kwiterovitch P, J Clin Endocrinol Metab 2008, Kavey REW et al. Pediatrics 2011; 128: S 1 -44

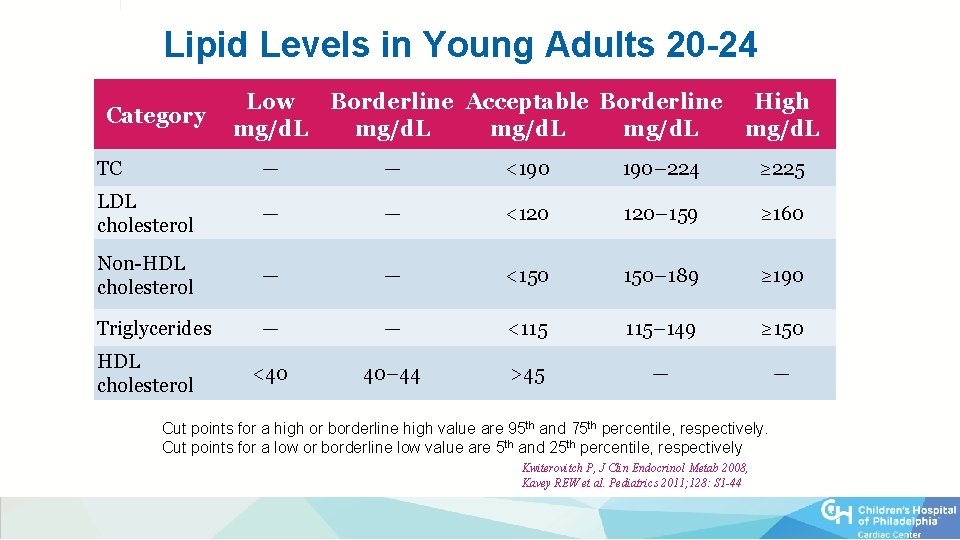
Lipid Levels in Young Adults 20 -24 Category Low mg/d. L Borderline Acceptable Borderline High mg/d. L TC — — <190 190– 224 ≥ 225 LDL cholesterol — — <120 120– 159 ≥ 160 Non-HDL cholesterol — — <150 150– 189 ≥ 190 Triglycerides — — <115 115– 149 ≥ 150 <40 40– 44 >45 — — HDL cholesterol Cut points for a high or borderline high value are 95 th and 75 th percentile, respectively. Cut points for a low or borderline low value are 5 th and 25 th percentile, respectively Kwiterovitch P, J Clin Endocrinol Metab 2008, Kavey REW et al. Pediatrics 2011; 128: S 1 -44

Clinical Case I (continued) • Physical Exam: • Vitals: • BMI 19. 4 (50 th %) • Blood pressure 120/74 (86 th %) • Pulse 72 bpm • PE: benign, no xanthomas, Tanner Stage II • Labs, mg/d. L (average of 2) • TC 444, HDL-c 64, LDL-c 366, TG 69, Non-HDL-c 380 mg/d. L, ALT/AST, CK: normal • Thyroid functions, UA, Glucose, Insulin: normal

Familial Hypercholesterolemia (FH) • Autosomal codominant inheritance – ~1: 200 -250 incidence (heterozygous), 1: 160, 000 worldwide (homozygous) • Mutations may be found in many genes: LDLR, apo. B, PCSK 9, or LDLRAP 1 • Genetic testing is available (We use Invitae) • Heterozygous FH – Usually TC > 270 mg/d. L, LDL-c > 160 mg/d. L – If untreated, risk of CVD – Men: 80% by 60 years old; Women: 45% by 60 years old • Homozygous FH – TC > 700 -1200 mg/d. L, LDL-C > 400 mg/d. L – Death from MI < age 30 years if untreated – Usually requires LDL apheresis + statins + injectable medications

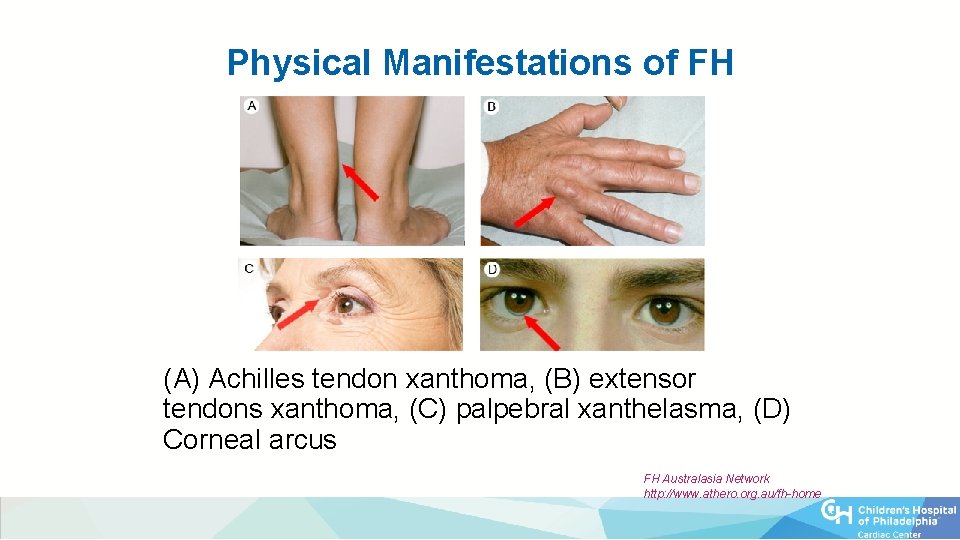
Physical Manifestations of FH (A) Achilles tendon xanthoma, (B) extensor tendons xanthoma, (C) palpebral xanthelasma, (D) Corneal arcus FH Australasia Network http: //www. athero. org. au/fh-home

The Three D’s: Diet, “Doing”, and Drugs • Diet


Children with Dyslipidemia, Overweight, or at Risk for CVD – Total fat 25%-30% daily kcals – Saturated fat <10 % daily kcals – Mono- and poly-unsaturated fats up to 20% daily calories – Avoid trans fats – Limit sweetened beverages – > 5 servings fruits & vegetables daily – Fiber: Age + 5 g/day (2 -10 yrs) 14 g/1000 kcal (11 -21 yr) NCEP expert panel of blood cholesterol levels in children and adolescents. Pediatrics 1992; 89: 495 -501.

Diet: High LDL-c • After 3 -6 months of low-saturated fat diet and LDL-c remains >130 mg/d. L • Reduce saturated fat intake to < 7% of total calories • Meet with registered dietitian • Soluble fiber • Psyllium (e. g. , Metamucil) • Up to 6 g/day for children 2– 12 years • Up to 12 g/day for those ≥ 12 years • Start at 3 g/day, increase in 3 gram increments, advise to drink plenty of water • Certain foods, such as: oat bran, barley, nuts, seeds, beans, lentils, peas, and some fruits and vegetables Daniels SR, Pediatrics 2008

Plant Stanols/Sterols • Phytochemicals that are found naturally in wide variety of foods, such as grains, vegetables, fruits, beans, nuts, and seeds • Added to some milk, cheese, juice and margarine spreads • Up to 2 g free plant stanols/sterols per day in children > 2 years with suspected FH • Lowers LDL by 5 -15% • Examples: Benecol & Smart Balance Heart Right Light margarine, Corowise plant sterol products, Nature-Made Cholest-Off, Vibrant Health Vanilla chews • Possible decrease in beta-carotene with long-term use • Eat one beta-carotene containing food daily

Clinical Case II • Physical exam: • Vitals: • BMI: 27. 0 kg/m 2 (122% of the 95 th BMI percentile ) • Blood pressure 114/70 (<90%) • Pulse: 75 bpm • PE: innocent murmur • Labs, mg/d. L: • TC: 213, HDL-c: 27, LDL-c: 140, TG: 229, non-HDL-c 186 • Thyroid functions, ALT/AST, glucose, insulin, UA: normal

Familial Combined Hyperlipidemia • Common lipid disorder • 1: 200 -300 • Autosomal dominant • TC 250 -350 mg/d. L, TG 200 -400 mg/d. L, low HDL • No unique clinical features • 10% of all patients with MI < 60 years

Combined Dyslipidemia of Obesity • Can be difficult to differentiate from familial combined hyperlipidemia • Becoming more common with obesity epidemic • Characterized by: • High TG, low HDL, normal to mildly increased LDL • Improves with diet, weight loss/stabilization, exercise • Focus on reducing simple carbohydrates and saturated fat, increasing complex carbohydrates • Physical activity is very important • Pharmacotherapy may be needed if diet/lifestyle is not implemented

Diet: High Triglycerides • Limit simple sugars and carbohydrates • Increase fiber and complex carbohydrates • Weight loss or stabilization • Omega-3 fatty acids • Foods such as: wild salmon, ground flaxseed, walnuts, winter squash • EPA + DHA, 2 -4 grams/day • Hard to get through diet alone • OTC or prescription (Lovaza, Vascepa), generally need TG > 500 mg/d. L for insurance approval • Weight loss or stabilization Kris-Etherton PM et al, Circulation 2002,

The Three D’s: Diet, “Doing”, and Drugs • “Doing”


Activity Recommendations • All children ≥ 2 years should participate in 1 hour of enjoyable, moderate-vigorous intensity activities daily • Limit sedentary activity (computer, television, texting, etc) to < 2 hr/day www. cdc. gov

The Three D’s: Diet, “Doing”, and Drugs • Drugs

When to consider medications (LDL-c)? • After intensive diet and lifestyle changes for up to 6 months, depending on risk level, in children > 10 years, > 8 years • Statin is first-line therapy Mc. Crindle et al, Circulation 2007, De. Ferranti et al. Circulation 2019

42 2019

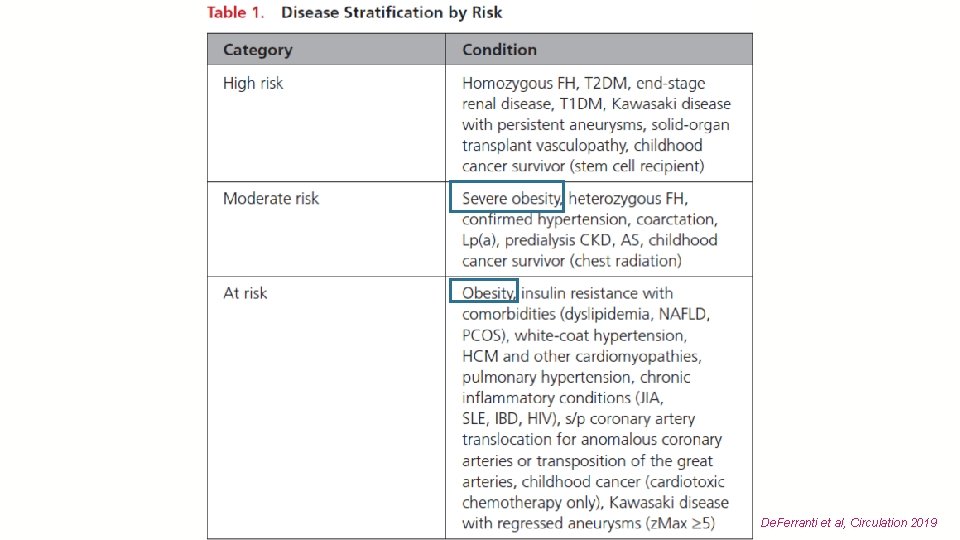
43 De. Ferranti et al, Circulation 2019

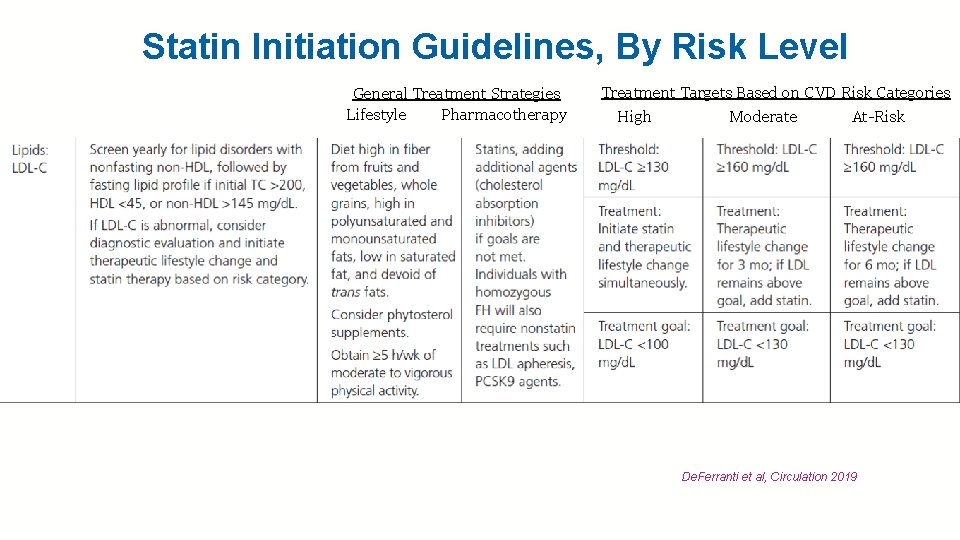
Statin Initiation Guidelines, By Risk Level General Treatment Strategies Lifestyle Pharmacotherapy Treatment Targets Based on CVD Risk Categories High Moderate At-Risk De. Ferranti et al, Circulation 2019

Statins Approved for Children Atorvastatin (Lipitor) 10 -20 mg/day (10 -17 yrs) 10 -80 mg/day (≥ 18 yrs) • Always start with the lowest dose Lovastatin • (Mevacor) mg/day Check CK, ALT/AST, 10 -40 Glu prior to(10 -17 yrs) starting; if obese, also check a Hgba 1 c Pravastatin (Pravachol) 10 -20 mg/day (8 -13 yrs) 10 -40 mg/day (14 -18 yrs) 20 -80 mg/day (>18 yrs) Rosuvastatin (Crestor) 5 -20 mg/day (10 -17 yrs) Simvastatin (Zocor) 10 -40 mg/day (10 -17 yrs)

Possible Statin Side Effects • Myalgia, myositis, rhabdomyolysis – Obtain baseline CK, and follow symptoms • Elevation of LFTs – Obtain baseline LFT’s, after medication initiation, and any change in medication – Once on stable dose and normal, I check annually • Increased fasting glucose and Hgb. A 1 c • Obtain a baseline fasting glucose. Monitor glucose and Hgb. A 1 c if child has risk factors for developing diabetes • Teratogenic – Consider birth control for girls/abstinence Pasternak RC et al, Circulation 2002; Thompson ED et al, JAMA 2003.

Further Management for Hyper. TG General Treatment Strategies Lifestyle Pharmacotherapy High Moderate At Risk De. Ferranti Circulation 2019

Clinical Case I • Severe heterozygous FH: LDL goal < 130 mg/d. L • Invitae testing results showed a pathogenic variant in the LDLR gene [c. 798 T>A (p. Asp 266 Glu)] • Labs I (in mg/d. L): • TC 444, HDL-c 64, LDL-c 366, TG 69, Non-HDL-c 380 mg/d. L, ALT/AST, CK: normal • Atorvastatin 10 mg nightly • Labs II, 2 months later: • TC 275, HDL-c 63, LDL-c 202, TG 51 (5 -50), non-HDL-c 213

Clinical Case I • Atorvastatin 20 mg nightly • Labs III, 2 months later • TC 244, HDL-c 66, LDL-c 165 , TG 67 (50 -75), non-HDL-c 178 • Atorvastatin 40 mg nightly • Labs IV, 3 months later • TC 221, HDL-c 73, LDL-c 138, TG 51, non-HDL-c 148

Clinical Case II dyslipidemia • • 3 Familial months combined later, lab IIvs (in. Obesity-related mg/d. L): TCI: 208, HDL 31, LDL 126, TG: 205, non-HDL-C 177 • • Lab • Started 2000 mg of 27, omega FATG: to goal TG < 150 mg/d. L • TC: 213, HDL-c: LDL-c: 3140, 229, non-HDL-c 186 • Encourage physical activity, increase to 45 minutes daily • • Lab III, 4 months later: Increase physical activity to 30 minutes daily, no • soda TC: in 172, LDL-c: 125, TG: 73, non-HDL-c the. HDL-c: house, 32, weight stabilization 140

Summary: Screening • Universal screening once age 9 -11 yrs and 17 -21 yrs – Fasting lipid profile or a non-fasting lipid profile • At-risk 2 -8 yr and 12 -16 yr olds – Fasting lipid profile

Summary: Acceptable Lipid Levels • LDL-C: <130 mg/d. L • TG: <100 mg/d. L if <10 yrs old TG: <130 mg/d. L if ≥ 10 yrs old • HDL-C: ≥ 45 mg/d. L • Non-HDL-C: < 145 mg/d. L

Summary: Medication Therapy • Consider statin therapy • If despite lifestyle changes and age > 8 -10 years and • LDL-c > 160 or > 130 based on risk category • Consider fish oil or additional pharmacotherapy • • TGs > 1000 (need to start along with diet/lifestyle) TGs 400 -999 mg/d. L OR TGs 130 -400 mg/d. L and non. HDL-c > 145 mg/d. L, depending on risk category

How to Refer to Lipid Heart Clinic • Families can call 215 -590 -4040 for an appointment • We offer telemedicine and in person appointments • Please have labs faxed to us at 267 -426 -9800 or emailed to: lipidheart@chop. edu • Any ? , please call 215 -590 -1804 • My email: brothersj@chop. edu

Thank you for your attention! 55